Module 27: Differentiation -- Pattern Analysis and Melanoma-Specific Criteria; Rules and Algorithms
Source: Dermoscopy Educational Course Authors: Konstantinos Liopyris, Cristian Navarrete-Dechent, Natalia Jaimes, and Ashfaq A. Marghoob (Ch. 9a); Natalia Jaimes (Ch. 9b)
1. Learning Objectives
After completing this module, the learner should be able to:
- Describe the pattern analysis approach to differentiating benign melanocytic nevi from melanoma, including the concepts of "organized" versus "disorganized" patterns.
- Recognize and describe each of the 10 benign nevus patterns and explain why deviation from these patterns raises suspicion for malignancy.
- Identify all melanoma-specific dermoscopic criteria (atypical pigment network, negative pigment network, angulated lines, irregular globules/clods, irregular dots, streaks, irregular blotch, regression structures, shiny white structures, blue-whitish veil, polymorphous vessels) and correlate them with their histopathologic substrates.
- Calculate a Total Dermoscopy Score (TDS) using the ABCD rule of dermoscopy, applying the correct weighted factors, and interpret the result using established thresholds.
- Apply the Menzies method by evaluating negative and positive features and state the decision rule for melanoma diagnosis.
- Score a lesion using the classic and revised seven-point checklists, explain the difference in thresholds (3 points vs. 1 point), and discuss the sensitivity-specificity tradeoff of each version.
- Calculate a CASH score (Color, Architecture, Symmetry, Homogeneity) and apply the threshold of 8 or more for melanoma suspicion.
- Compare the diagnostic performance (sensitivity, specificity, diagnostic accuracy) of all four algorithms and pattern analysis, and explain why pattern analysis yields superior specificity in experienced hands.
2. Prerequisites
- Module 03: Pattern Analysis Revised -- Geometric terminology, basic elements, Chaos and Clues framework
- Module 04: Top-Down 2-Step Algorithm -- Step 1 benign lesion recognition, Step 2 equivocal lesion analysis
- Module 05: Prediction without Pigment -- Decision algorithm for nonpigmented lesions, vessel analysis
- Module 06: Chaos and Clues Triage Algorithm -- Nine clues to malignancy, application workflow
- Module 07: TADA and Other Triage Algorithms -- Overview of TADA, 3-point checklist, introductory ABCD/Menzies/7-point/CASH concepts
- Modules 15-20: Benign Melanocytic Lesions -- Congenital nevi, acquired nevi, intradermal nevi, blue nevi, Spitz/Reed nevi, other nevus variants
- Modules 21-26: Melanoma -- SSM, nodular melanoma, lentigo maligna, acrolentiginous melanoma, other subtypes, amelanotic melanoma
3. Key Concepts
The Systematic Differentiation Approach
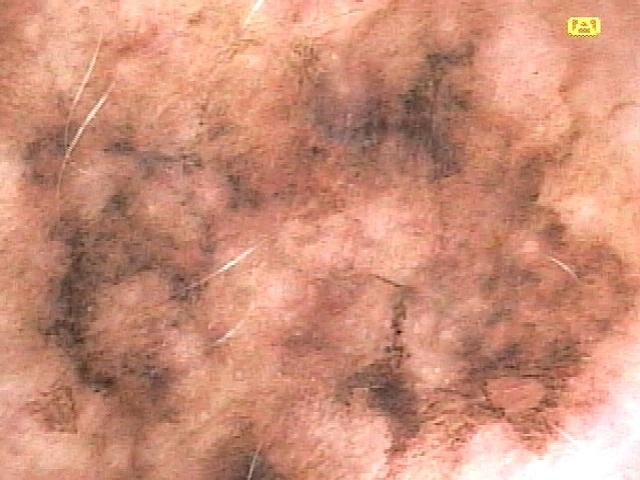
The clinical challenge in dermoscopy is not merely identifying individual structures but integrating them into a coherent diagnostic framework. Two complementary cognitive strategies are employed:
Heuristic (pattern recognition) -- Rapid, experience-driven evaluation based on matching the overall gestalt of a lesion to stored mental templates. Pattern analysis is the primary heuristic method. It requires significant experience to master but, once mastered, allows rapid and highly accurate evaluation.
Analytic (algorithmic) -- Structured, semi-quantitative scoring systems (ABCD rule, Menzies method, 7-point checklist, CASH) that guide the observer step-by-step through feature identification and scoring. These methods do not require significant experience and are best suited for novice dermoscopists.
As experience is gained, a natural shift occurs from predominantly analytic approaches to predominantly heuristic approaches. Importantly, studies show that both teaching methods improve diagnostic accuracy by approximately 20% in novices, but pattern analysis ultimately yields slightly better diagnostic accuracy and faster evaluation times than algorithmic methods.
In clinical practice, experienced dermoscopists use both approaches interactively -- pattern recognition for routine lesions and deliberate analytic reasoning when a case is complex, ill-defined, or unfamiliar.
The Core Principle
Benign melanocytic lesions tend to manifest organized, symmetric patterns. Melanomas tend to manifest disorganized, asymmetric patterns with at least one melanoma-specific structure. However, there are important exceptions: some melanomas (amelanotic melanoma, nodular melanoma) can display organized/symmetric patterns, and some benign nevi (multicomponent pattern) can appear complex. Thus, the recognition of melanoma-specific structures is essential regardless of overall pattern assessment.
4. Core Content
Chapter 9a -- Pattern Analysis for Differentiation
4.1 The Pattern Analysis Approach
Pattern analysis for differentiating benign from suspect melanocytic lesions begins with a fundamental acknowledgment: the "critical element of becoming an expert is accruing the vast experience that enables experts to recognize patterns effortlessly, most of the time -- and to recognize, as well, when the signs and symptoms do not fit a pattern at all."
The recommended approach proceeds in two phases:
Phase 1 -- Build a mental library of benign patterns: Since benign lesions constitute the vast majority of lesions encountered in daily practice, the learner first builds extensive experience recognizing the 10 benign patterns of nevi (see Section 4.2 below). Nevi tend to exhibit symmetry of pattern, structure, and color -- they manifest an "organized pattern."
Phase 2 -- Identify deviations from benign patterns: Once familiarized with normal nevus patterns, suspicious lesions that deviate from those benign patterns are readily identified. Malignant lesions, including melanomas, usually deviate from benign patterns and display some degree of asymmetry of pattern, color, and structure -- they manifest a "disorganized pattern."
4.2 The 10 Benign Nevus Patterns
The following global patterns are characteristic of benign nevi. Any melanocytic neoplasm that deviates from these patterns should be viewed with caution.
| # | Global Pattern | Definition | Clinical Association |
|---|---|---|---|
| 1 | Reticular diffuse | Diffuse homogeneous network with relatively uniform thickness and color of network lines; holes of relatively uniform size; network tends to fade at the periphery | Acquired nevi and small congenital nevi on the extremities |
| 2 | Reticular patchy | Homogeneous network in focal patches distributed in an organized manner, separated by homogeneous structureless areas lighter than the network lines; structureless areas are same color as background skin or slightly darker | Acquired nevi on the torso; superficial congenital nevi, especially lower extremity |
| 3 | Peripheral reticular with central hypopigmentation | Relatively uniform network at the periphery with a central homogeneous and hypopigmented structureless area (same color as background skin or slightly darker, but lighter than network lines) | Acquired nevi, more common in fair-skinned individuals |
| 4 | Peripheral reticular with central hyperpigmentation | Relatively uniform network at the periphery with a central homogeneous hyperpigmented structureless area or blotch (darker than network lines) | Acquired nevi, more common in darker-skinned individuals |
| 5 | Homogeneous tan, brown, or blue pigmentation (sometimes pink) | Primarily diffuse homogeneous structureless pattern; occasional globules and/or small focal network fragments may be evident | Tan = acquired nevi in fair skin; dark brown = congenital nevi; blue = blue nevi; pink = nevi in very fair-skinned/redheads (NB: amelanotic/hypomelanotic melanomas can appear similar but usually also reveal atypical vessels and/or shiny white structures) |
| 6 | Peripheral reticular with central globules | Relatively uniform network at the periphery with central globules | Often congenital nevi histopathologically |
| 7 | Peripheral globules with central network or homogeneous area and the starburst pattern | Central reticular or homogeneous component with peripheral globules; one row of uniform brown globules = Clark nevus in active radial growth; tiered (>1 row) globules = spitzoid morphology; classic starburst = streaks around entire perimeter | Clark nevi (growing), Spitz/Reed nevi in active radial growth |
| 8 | Globular (includes cobblestone) | Globules of similar shape, size, and color distributed symmetrically; globules usually round to oval; sometimes large and angulated (cobblestone appearance) | Congenital nevi (most commonly) |
| 9 | Two-component | Two different patterns present (reticular-globular, reticular-homogeneous, or globular-homogeneous); one half manifests one pattern, the other half manifests a different pattern | Benign nevi with dual pattern |
| 10 | Multicomponent | Definition 1 (benign): Organized and/or symmetrically distributed typical dots/globules, typical network, and homogeneous areas; axis of symmetry need only be in one axis. Definition 2 (caution): Symmetrically distributed globules, network, blotches, dots, veil, regression structures, and/or structureless areas with 3 or more structures required. A multicomponent pattern other than Definition 1 should be evaluated in context with the patient's other nevi (comparative approach). If it is the patient's signature pattern, it can be followed. If it is an outlier, biopsy should be considered. | Benign nevi (Definition 1); requires comparative approach (Definition 2) |
4.3 Global Pattern Assessment
The first step in differentiating nevi from melanoma is evaluating the global pattern:
Step 1: Evaluate global pattern
|
+----+----+
| |
v v
ORGANIZED DISORGANIZED
(Symmetric) (Asymmetric)
| |
v v
Matches one Step 2: Evaluate for
of 10 benign melanoma-specific
nevus structures
patterns?
| |
Yes No
| |
v v
Likely Any melanoma-
benign specific structure
present?
|
+----+----+
| |
Yes No
| |
v v
Consider Feature-poor/
melanoma featureless -->
until consider digital
proven monitoring
otherwise
Critical exceptions to the organized = benign rule:
- Some melanomas display an organized pattern (e.g., amelanotic melanoma, nodular melanoma). Even in these cases, the recognition of at least one melanoma-specific structure or blue-black/gray color under dermoscopy will raise suspicion.
- Dermoscopic asymmetry by itself is NOT a prerequisite for the diagnosis of melanoma.
- A subset of flat, feature-poor or featureless/structureless melanomas may prove challenging to diagnose; however, dermoscopy provides useful information by identifying changes over time through digital monitoring.
Clinical Scenario
A 38-year-old woman presents with an 8 mm flat brown lesion on her left thigh. Dermoscopy shows a diffuse reticular pattern with relatively uniform network lines that fade at the periphery, with no atypical features, asymmetry, or additional structures. The pattern is organized and symmetric across both axes.
What benign pattern does this lesion display, and what would change your assessment?
Reticular Diffuse Pattern (Benign Nevus Pattern #1)
This is one of the 10 recognized benign nevus patterns: diffuse homogeneous network with uniform line thickness and color, holes of uniform size, fading at the periphery. It corresponds to a junctional or superficial compound acquired nevus. Features that would raise suspicion include: focal thickening or gray discoloration of network lines (atypical network), eccentric blotch, asymmetric streaks, blue-white veil, negative network, or any melanoma-specific structure. Any deviation from the organized pattern should prompt closer evaluation.
4.4 Melanoma-Specific Criteria Checklist
Any lesion that deviates from the benign patterns listed above and manifests at least one of the following melanoma-specific structures should be considered a melanoma until proven otherwise.
| Dermoscopic Feature | Definition | Histopathologic Correlate |
|---|---|---|
| Atypical pigment network | Network with increased variability in color, thickness, and spacing of lines; asymmetrically distributed | Lines = pigmented keratinocytes or melanocytes along DEJ; holes = suprapapillary plate |
| Negative pigment network | Serpiginous interconnecting broadened hypopigmented lines surrounding elongated and curvilinear globules. Seen in de novo melanomas and melanomas arising in pre-existing nevi | Distorted/attenuated rete ridges with confluent nested melanocytes along DEJ (brown elongated globular structures) flanked by elongated/widened rete ridges (hypopigmented areas) |
| Angulated lines | Gray to brown lines meeting at acute angles creating a zig-zag pattern; can coalesce to form polygons (rhomboids); may appear as solid lines or lines composed of gray dots (pointillism). Mainly seen in melanoma on sun-damaged skin (lentigo maligna) | Flattening of DEJ, confluent melanocytes along DEJ, melanophages in papillary dermis |
| Irregular globules/clods | Clods, round or oval, with heterogeneity in size, shape, and/or color | Nests of nevomelanocytes at DEJ or dermis |
| Irregular dots | Dots, black or brown with heterogeneity in color and off-center distribution; often found with atypical network or toward the periphery of melanoma | Aggregates of melanocytes or melanin granules; if black = stratum corneum; if brown = epidermis below stratum corneum |
| Streaks (always at periphery): radial streaming, pseudopods | Radial streaming: radial and segmental lines. Pseudopods: radial and segmental lines with bulbous projections at tips | Confluent junctional nests of melanocytes at lesion periphery |
| Irregular blotch | Structureless zone with so much brown-black-blue pigment that it obscures other structures; classified as irregular if off-center or if multiple blotches present | Aggregates of melanin in stratum corneum or throughout all layers of epidermis with or without dermal involvement |
| Regression structures: peppering/granularity | Dots with gray color | Free melanin or melanophages in papillary dermis |
| Regression structures: scarlike depigmentation | White structureless zone lighter than surrounding normal skin; usually seen with peppering | Fibrotic papillary dermis |
| Shiny white structures (polarized dermoscopy only) | Shiny white lines oriented parallel and orthogonal to each other; may coalesce into grid of square-shaped white-lined structures. NOT to be confused with negative network (visible in both polarized and nonpolarized) | Altered matrix collagen and dermal fibroplasia |
| Blue-whitish veil | Structureless zone, blue with white "ground glass" haze found over a raised area; does NOT occupy the entire lesion | Heavily pigmented dermal melanocytes combined with compact orthokeratosis |
| Polymorphous vessels | Vessels with more than one morphology, usually consisting of dotted and linear serpentine vessels plus any other vessel morphology | Tumoral neo-angiogenesis in the dermis |
4.5 Feature-by-Feature Comparison: Nevus vs. Melanoma
| Feature | Nevus Version | Melanoma Version |
|---|---|---|
| Pigment network | Typical: uniform thickness, color, and spacing of lines; fades at periphery | Atypical: variable thickness, color, and spacing; asymmetric distribution |
| Negative network | Not typically present | Serpiginous hypopigmented lines surrounding elongated curvilinear globules |
| Dots | Regular: uniform in size and color, evenly distributed | Irregular: heterogeneous color, off-center distribution |
| Globules/clods | Regular: similar shape, size, and color; symmetrically distributed | Irregular: heterogeneous in size, shape, and/or color |
| Streaks | Circumferential (entire perimeter); seen in Spitz/Reed nevi in growth phase | Segmental (focal at periphery); asymmetric radial streaming or pseudopods |
| Blotch | Regular: central, symmetric (regular blotch) | Irregular: off-center or multiple blotches obscuring structures |
| Structureless areas | Homogeneous, symmetric; same color tone or slightly darker than background | Eccentric, asymmetric; variable colors; regression, blue-whitish veil |
| Vessels | Regular pattern: comma vessels (intradermal nevi) | Polymorphous: multiple vessel morphologies in a single lesion |
| Overall pattern | Organized, symmetric; one of 10 benign patterns | Disorganized, asymmetric; chaotic distribution of colors and structures |
4.6 Important Diagnostic Nuances
Agreement on melanoma-specific structures is imperfect even among experts: Preliminary data suggest that agreement on the presence and spatial localization of melanoma-specific structures is poor even among experienced dermoscopists. Nevertheless, their presence increases the possibility of malignancy.
The heterogeneity principle: Irregular dots may be confused with irregular globules; however, the heterogeneity in size, shape, and color of the structure, and their chaotic distribution, will raise suspicion for melanoma irrespective of whether the observer classifies the structure as a dot or as a globule.
Both approaches are used interactively: Dermoscopic evaluation utilizes both heuristic and analytic approaches in an interactive fashion. Nonanalytic reasoning (pattern recognition) is essential to diagnostic expertise and is developed through practice and clinical experience. Deliberative analytic reasoning is the primary strategy when a case is complex, ill-defined, unusual, or when the physician has limited experience with the particular disease entity.
Check Your Understanding
How does the concept of 'dermoscopic symmetry' differ from clinical symmetry?
Dermoscopic symmetry evaluates the distribution and arrangement of colors and structures within the lesion, not just its overall shape. A lesion may appear clinically symmetric (round shape) but be dermoscopically asymmetric if the internal structures, colors, or patterns are unevenly distributed. Dermoscopic asymmetry is a more sensitive indicator of malignancy than clinical asymmetry.
Key Takeaways
- Specific dermoscopic features (e.g., arborizing vessels for BCC, comedo-like openings for SK) provide high positive predictive value for particular diagnoses.
- Sensitive features (e.g., any atypical pattern, any vessel irregularity) cast a wide net and are useful for screening but produce more false positives.
- The tension between sensitivity and specificity means that no single feature or algorithm is optimal for all clinical scenarios; the approach must be adapted to the pretest probability.
Clinical Scenario
A 48-year-old man presents with a 10 mm pigmented lesion on his upper back. Dermoscopy reveals an atypical pigment network (broadened, irregular lines with gray coloration), an eccentric irregular blotch, regression structures (blue-gray peppering) in one quadrant, and shiny white lines under polarized light. Using the ABCD rule, you score: Asymmetry = 2, Border = 4, Color = 4, Dermoscopic structures = 4, yielding TDS = 7.45.
What does this TDS indicate, and which melanoma-specific structures are present?
Melanoma (TDS > 5.45)
A TDS above 5.45 indicates high suspicion for melanoma. This lesion manifests four melanoma-specific structures: (1) atypical pigment network, (2) irregular blotch, (3) regression structures, and (4) shiny white lines. The Menzies method would also be positive (no symmetry of pattern, no single color, plus at least one positive feature). The seven-point checklist scores at least 5 points (atypical network = 2, regression = 1, irregular blotch = 1, shiny white structures = 1). All four algorithms agree -- excisional biopsy is indicated.
Chapter 9b -- Rules and Algorithms
4.7 Overview of Dermoscopic Algorithms
Several algorithms and scoring systems have been created to guide the observer in the dermoscopic decision-making process. This chapter covers four major systems:
- ABCD rule of dermoscopy
- Menzies method
- Seven-point checklist (classic and revised)
- CASH algorithm
All are relatively simple, accurate, and reproducible methods for dermoscopic evaluation. Although all have similar sensitivity, methods that rely on pattern analysis demonstrate superior specificity, making them the preferred methods utilized by experienced clinicians.
Important caveat: None of these algorithms has been updated since original publication. Many new melanoma-specific structures have been identified since (shiny white lines, negative network, angulated lines). These more newly identified structures should not be ignored by clinicians electing to use one of these algorithms.
4.8 ABCD Rule of Dermoscopy
The ABCD rule of dermoscopy is a semi-quantitative scoring system created by Stolz and colleagues in 1994 for the evaluation of pigmented lesions. It analyzes four criteria, each multiplied by a weighted factor. The four individual weighted scores are summed to produce the Final Dermoscopy Score (FDS), also called the Total Dermoscopy Score (TDS).
Criteria:
A -- Asymmetry (weighted factor: x1.3; range 0-2.6):
- Refers to the contour AND distribution of colors and structures within the lesion in none, one, or two perpendicular axes.
- Score 0 = no asymmetry (symmetric in both axes)
- Score 1 = mono-axial asymmetry (asymmetric in one axis)
- Score 2 = bi-axial asymmetry (asymmetric in both axes)
- Note: The ABCD rule and the CASH algorithm are the only methods that take into account both contour and content of the lesion during asymmetry evaluation.
B -- Border sharpness (weighted factor: x0.1; range 0-0.8):
- Refers to the abrupt cutoff of pigmentation at the perimeter.
- Evaluated by tracing four imaginary lines that divide the lesion into eight pie-shaped sections.
- A score of 1 is given to each segment presenting with an abrupt cutoff of pigment.
- Score range: 0-8
C -- Colors (weighted factor: x0.5; range 0.5-3.0):
- The lesion is evaluated for the presence of each of six colors:
- White
- Red
- Light brown
- Dark brown
- Blue-gray
- Black
- A score of 1 is given to each color present.
- Score range: 1-6
D -- Dermoscopic structures (weighted factor: x0.5; range 0.5-2.5):
- The lesion is evaluated for the presence of five structures:
- Pigment network
- Branched streaks
- Dots
- Globules (aggregated globules)
- Homogeneous/structureless areas (including hyperpigmented blotches, hypopigmented areas, depigmented or scarlike areas involving >10% of surface area)
- A score of 1 is given to each structure present.
- Score range: 1-5
Calculation:
TDS = (Asymmetry score x 1.3) + (Border score x 0.1) + (Color score x 0.5) + (Structure score x 0.5)
Interpretation thresholds:
| TDS Range | Interpretation |
|---|---|
| < 4.75 | Benign |
| 4.75 - 5.45 | Suspicious -- close follow-up or biopsy recommended |
| > 5.45 | Highly suggestive of malignancy -- biopsy/excision indicated |
Total possible range: 1.0 to 8.9
Performance: Sensitivity 78-98%; Specificity 45-90% (varies with examiner experience).
4.9 Menzies Method
The Menzies method was developed to differentiate invasive melanomas from other pigmented lesions. It evaluates 11 dermoscopic criteria classified into negative features (2) and positive features (9).
Decision rule: For the diagnosis of melanoma, BOTH negative features must be ABSENT and at least ONE positive feature must be PRESENT.
Negative Features (neither can be present in melanoma):
| # | Negative Feature | Description |
|---|---|---|
| 1 | Symmetrical pigmentation pattern | Symmetric pigment pattern across all axes |
| 2 | Presence of only one color | Only one of the following colors: tan, dark brown, black, gray, blue, or red |
The two negative features have demonstrated a low sensitivity for melanoma (i.e., most melanomas will lack these features, making them good at ruling melanoma in when absent). Their presence essentially excludes the diagnosis of melanoma.
Positive Features (at least one must be present to consider melanoma):
| # | Positive Feature | Description |
|---|---|---|
| 1 | Multiple colors | Presence of five or more colors (from: tan, dark brown, black, gray, blue, red) |
| 2 | Blue-white veil | Irregular and confluent blue pigmentation with an overlying white "ground glass" film, not associated with red-blue lacunae |
| 3 | Multiple brown dots | Aggregations of dark brown dots, usually within the body of the lesion |
| 4 | Multiple blue/gray dots | Diffuse, partly aggregated dots, "pepper-like" in appearance |
| 5 | Peripheral black dots or globules | Black dots or globules at or near the edge of the lesion |
| 6 | Broadened network | Pigment network with areas of thick grids |
| 7 | Pseudopods | Finger-like projections with small knobs at their tips, directly connected to the tumor body or the pigment network |
| 8 | Radial streaming | Radial and asymmetric linear extensions at the edge of the lesion |
| 9 | Scarlike depigmentation | White, irregular area of depigmentation |
The nine positive features have a high specificity for melanoma (>85%).
Application logic:
Step 1: Are BOTH negative features present?
|
+----+----+
| |
Yes No (at least one negative feature is absent)
| |
v v
Melanoma Step 2: Is at least ONE positive feature present?
EXCLUDED |
+----+----+
| |
Yes No
| |
v v
Suspect Melanoma
MELANOMA less likely
Performance: Sensitivity 85-92% (for pigmented melanoma 86-95%; for amelanotic melanoma 54%); Specificity 38-78%; Diagnostic accuracy 83%.
4.10 The Seven-Point Checklist
The seven-point checklist evaluates seven dermoscopic features frequently associated with melanoma, categorized into major and minor criteria with differential weighting.
Classic Seven-Point Checklist:
Major Criteria (2 points each):
| Criterion | Definition | Classic Score | Revised Score |
|---|---|---|---|
| Atypical pigment network | Prominent (hyperpigmented or thick) and irregular network | 2 | 1 |
| Blue-whitish veil (white-blue areas) | Irregular, structureless white-blue area with an overlying "ground glass" film; cannot occupy the entire lesion | 2 | 1 |
| Atypical vascular pattern | Linear irregular or dotted vessels, irregularly distributed outside areas of regression | 2 | 1 |
Minor Criteria (1 point each):
| Criterion | Definition | Classic Score | Revised Score |
|---|---|---|---|
| Radial streaming (streaks) | Radial and asymmetric linear or bulbous projections at the edge of the lesion | 1 | 1 |
| Irregular blotches | Black, brown, and/or gray structureless areas with irregular shape or distribution | 1 | 1 |
| Irregular dots and globules | Black or brown round structures irregularly distributed | 1 | 1 |
| Regression structures | White scarlike depigmentation and/or "peppering" | 1 | 1 |
Scoring:
- Major criteria score range: 0-6 (3 criteria x 2 points each)
- Minor criteria score range: 0-4 (4 criteria x 1 point each)
- Total score range: 0-10
Classic threshold: Total score of 3 or more = suggestive of melanoma.
Revised Seven-Point Checklist:
The revised version proposes that the presence of ANY criterion (major or minor) is sufficient to consider a lesion suspicious for melanoma. The threshold for biopsy is lowered to a total score of 1 (instead of 3). Each criterion receives a score of 1 (no differential weighting). This achieves higher sensitivity at the cost of lower specificity.
The authors acknowledge that a sensitive and specific method to diagnose melanoma requires that additional factors and context be taken into account during examination, including:
- Clinical characteristics of the lesion
- Age and skin type of patient
- Location of lesion
- Whether the lesion is an outlier lesion (comparative approach)
- Whether the lesion has changed during follow-up
Performance (Classic): Sensitivity 62-95% (amelanotic melanoma 41%); Specificity 35-97%. Performance (Revised): Sensitivity 88%; Specificity 75%.
Key Takeaways
- Pattern-based differentiation uses global assessment (overall architecture) followed by local feature analysis (specific structures) to reach a diagnosis.
- Criteria-based rules (checklists, scoring systems) standardize the diagnostic process and are particularly valuable for less experienced dermoscopists.
- Expert dermoscopists integrate pattern recognition, probabilistic reasoning, and clinical context simultaneously, achieving diagnostic accuracy that exceeds any single algorithm.
4.11 CASH Algorithm
The CASH (Color, Architecture, Symmetry, and Homogeneity) algorithm was developed by Henning and colleagues in 2007 as a comprehensive scoring system. Total score range is 2-17.
C -- Color (score range 1-6): The lesion is evaluated for the presence of each of six colors. One point is given for each color present:
| Color | Score |
|---|---|
| Light brown | 1 |
| Dark brown | 1 |
| Brown | 1 |
| Red | 1 |
| White | 1 |
| Blue | 1 |
A -- Architectural disorder (score range 0-2): Refers to order versus disorder in the distribution of dermoscopic structures:
| Degree | Description | Score |
|---|---|---|
| None/mild | Colors and dermoscopic structures distributed in an organized or slightly disordered manner | 0 |
| Moderate | Dermoscopic structures lose their uniformity and are distributed in an irregular manner | 1 |
| Marked | Arrangement of colors and dermoscopic structures is completely disorganized (chaotic) | 2 |
S -- Symmetry (score range 0-2): Takes into account shape AND dermoscopic structures:
| Symmetry | Score |
|---|---|
| Bi-axial symmetry | 0 |
| Mono-axial symmetry | 1 |
| Bi-axial asymmetry | 2 |
H -- Homogeneity/Heterogeneity of dermoscopic structures (score range 1-7): The lesion is evaluated for the number of distinct dermoscopic structures present. One point per structure:
| Structure | Score |
|---|---|
| Network | 1 |
| Dots/globules | 1 |
| Streaks/pseudopods | 1 |
| Blue-white veil | 1 |
| Regression structures | 1 |
| Blotches | 1 |
| Polymorphous vessels | 1 |
Calculation:
CASH score = Color score + Architectural disorder score + Symmetry score + Homogeneity score
Interpretation threshold:
| CASH Score | Interpretation |
|---|---|
| < 8 | Likely benign |
| >= 8 | Suspicious for melanoma |
Performance: Sensitivity 87-98%; Specificity 67-68%.
4.12 Comparative Analysis of Algorithms
All four algorithms share common principles:
- They assess for asymmetry/symmetry in some form
- They evaluate the number and diversity of colors
- They identify the presence of specific dermoscopic structures
- They produce a numeric score compared against a threshold
Key differences:
| Feature | ABCD Rule | Menzies | 7-Point Checklist | CASH |
|---|---|---|---|---|
| Scoring type | Weighted semi-quantitative | Binary (negative/positive) | Weighted (classic) or unweighted (revised) | Unweighted additive |
| Number of criteria | 4 composite criteria | 11 (2 negative + 9 positive) | 7 (3 major + 4 minor) | 4 composite criteria |
| Asymmetry assessment | Contour + content | Pattern only | Not directly scored | Shape + structures |
| Border evaluation | Yes (8 segments) | No | No | No |
| Color scoring | 6 colors, weighted | Binary (1 vs. 5+ colors) | Not directly scored | 6 colors, unweighted |
| Threshold | 4.75 (suspicious), 5.45 (malignant) | Binary rule | 3 (classic), 1 (revised) | 8 |
| Best for | General screening | Invasive melanoma vs. pigmented lesions | Structured teaching, sequential monitoring | Comprehensive scoring |
| Original publication | Stolz et al. 1994 | Menzies et al. 1996 | Argenziano et al. 1998 | Henning et al. 2007 |
4.13 When to Use Which Algorithm
For novice dermoscopists:
- Start with the seven-point checklist -- it focuses on a limited number of well-defined structures and provides a clear scoring system for learning.
- The ABCD rule provides a systematic framework that reinforces attention to asymmetry, border, color, and structures.
- The Menzies method is useful for its binary decision logic -- first check for the two exclusion criteria, then look for positive features.
For experienced clinicians:
- Pattern analysis is the preferred method as it demonstrates superior specificity and faster evaluation times.
- Algorithms serve as a structured backup when encountering complex or unfamiliar lesions.
For screening in primary care/non-specialist settings:
- The revised seven-point checklist (threshold of 1) maximizes sensitivity, which is appropriate when the primary goal is not to miss melanoma, accepting a higher false-positive rate.
- The CASH algorithm provides a comprehensive assessment that is relatively straightforward to apply.
For research and education:
- Any algorithm can be used as a standardized framework for teaching and comparison.
- The ABCD rule is widely studied and has extensive validation data across different populations.
4.14 Algorithm Limitations and Pitfalls
No algorithm has been updated since its original publication -- newly identified melanoma-specific structures (shiny white lines, negative network, angulated lines) are not incorporated into any scoring system.
All algorithms require pre-classification as melanocytic: For all analytically based scoring algorithms, a given pigmented lesion must first be classified as melanocytic (nevus vs. melanoma) rather than non-melanocytic. Only after ruling out a non-melanocytic diagnosis can the algorithms be applied.
Amelanotic melanoma is poorly detected: All algorithms have significantly lower sensitivity for amelanotic and hypomelanotic melanomas compared to pigmented melanomas.
Nodular melanoma challenges: Many classic dermoscopic criteria are based on features observed in superficial spreading melanoma with melanin/melanocytes in the epidermis or at the DEJ. Nodular melanomas may lack these criteria.
Context matters: None of the algorithms incorporate patient age, skin type, lesion location, personal/family history, or change over time -- all of which are important contextual factors for clinical decision-making.
Sensitivity vs. specificity tradeoff: Lowering the scoring threshold (e.g., revised 7-point checklist) increases sensitivity but decreases specificity, leading to more unnecessary biopsies.
Inter-observer variability: Agreement on the presence of specific dermoscopic structures is imperfect even among experts, which affects the reproducibility of all scoring systems.
Check Your Understanding
What are the 'specific patterns' that allow confident benign diagnosis without further algorithmic analysis?
Specific benign patterns include: the comma vessel pattern (dermal nevus), the strawberry pattern (actinic keratosis), the lacunar pattern (hemangioma), the starburst pattern in a young patient (Spitz/Reed nevus), the parallel furrow pattern (acral nevus), the cerebriform/fissure pattern (seborrheic keratosis), and the central white patch with peripheral network (dermatofibroma). These patterns have high positive predictive values for their respective diagnoses.
Key Takeaways
- Combining specific features (high PPV) with sensitive screening criteria (high NPV) in a sequential approach optimizes both melanoma detection and biopsy efficiency.
- The number needed to biopsy (NNB) is a clinically meaningful metric: expert dermoscopists achieve NNB of 3-5 for melanoma, while naked-eye examination has NNB of 15-30.
- Continuous learning and feedback (correlating dermoscopic impressions with histologic outcomes) is the most effective way to improve individual diagnostic performance.
5. Algorithm Scoring Reference Tables
Table A: ABCD Rule of Dermoscopy -- Complete Scoring
| Criterion | Score Options | Raw Score Range | Weighted Factor | Final Score Range |
|---|---|---|---|---|
| A -- Asymmetry | 0 = no asymmetry; 1 = mono-axial; 2 = bi-axial | 0-2 | x 1.3 | 0 - 2.6 |
| B -- Border | 0-8 segments with sharp cutoff | 0-8 | x 0.1 | 0 - 0.8 |
| C -- Colors | 1 point per color (white, red, light brown, dark brown, blue-gray, black) | 1-6 | x 0.5 | 0.5 - 3.0 |
| D -- Structures | 1 point per structure (network, branched streaks, dots, globules, structureless areas) | 1-5 | x 0.5 | 0.5 - 2.5 |
| Total Dermoscopy Score | 1.0 - 8.9 |
Thresholds: < 4.75 = benign | 4.75-5.45 = suspicious | > 5.45 = malignant
Table B: Menzies Method -- Complete Criteria
| Category | Feature | Description | Rule |
|---|---|---|---|
| Negative Feature 1 | Symmetrical pattern | Symmetric pigment pattern across all axes | BOTH negative features must be ABSENT to consider melanoma |
| Negative Feature 2 | Only one color | Only 1 of 6 colors (tan, dark brown, black, gray, blue, red) | |
| Positive Feature 1 | Multiple colors | 5 or more colors present | At least ONE positive feature must be PRESENT to consider melanoma |
| Positive Feature 2 | Blue-white veil | Irregular confluent blue pigmentation + white "ground glass" film | |
| Positive Feature 3 | Multiple brown dots | Aggregations of dark brown dots within lesion body | |
| Positive Feature 4 | Multiple blue/gray dots | Diffuse, "pepper-like" partly aggregated dots | |
| Positive Feature 5 | Peripheral black dots/globules | Black dots or globules at/near lesion edge | |
| Positive Feature 6 | Broadened network | Pigment network with areas of thick grids | |
| Positive Feature 7 | Pseudopods | Finger-like projections with knobs at tips, connected to tumor body | |
| Positive Feature 8 | Radial streaming | Radial, asymmetric linear extensions at lesion edge | |
| Positive Feature 9 | Scarlike depigmentation | White, irregular area of depigmentation |
Decision: Melanoma = BOTH negative features ABSENT + at least 1 positive feature PRESENT.
Table C: Seven-Point Checklist -- Classic and Revised Scoring
| Category | Criterion | Definition | Classic Score | Revised Score |
|---|---|---|---|---|
| Major | Atypical pigment network | Prominent, hyperpigmented/thick, irregular network | 2 | 1 |
| Major | Blue-whitish veil | Irregular structureless white-blue area with "ground glass" film; not occupying entire lesion | 2 | 1 |
| Major | Atypical vascular pattern | Linear irregular or dotted vessels, irregularly distributed outside regression areas | 2 | 1 |
| Minor | Radial streaming (streaks) | Radial, asymmetric linear or bulbous projections at lesion edge | 1 | 1 |
| Minor | Irregular blotches | Black, brown, and/or gray structureless areas with irregular shape/distribution | 1 | 1 |
| Minor | Irregular dots and globules | Black or brown round structures irregularly distributed | 1 | 1 |
| Minor | Regression structures | White scarlike depigmentation and/or "peppering" | 1 | 1 |
| Maximum possible score | 10 | 7 |
Classic threshold: Total >= 3 = suspicious for melanoma Revised threshold: Total >= 1 = suspicious for melanoma (any single criterion)
Table D: CASH Algorithm -- Complete Scoring
| Criterion | Sub-items | Score | Score Range |
|---|---|---|---|
| Color | Light brown (1), Dark brown (1), Brown (1), Red (1), White (1), Blue (1) | 1 per color present | 1-6 |
| Architectural disorder | None/mild (0), Moderate (1), Marked (2) | 0, 1, or 2 | 0-2 |
| Symmetry | Bi-axial symmetry (0), Mono-axial (1), Bi-axial asymmetry (2) | 0, 1, or 2 | 0-2 |
| Homogeneity | Network (1), Dots/globules (1), Streaks/pseudopods (1), Blue-white veil (1), Regression structures (1), Blotches (1), Polymorphous vessels (1) | 1 per structure present | 1-7 |
| Total CASH Score | 2-17 |
Threshold: Total >= 8 = suspicious for melanoma
6. Algorithm Performance Comparison Table
| Algorithm | Sensitivity (Pigmented Melanoma) | Sensitivity (Amelanotic Melanoma) | Specificity (Experts) | Specificity (Nonexperts) | Diagnostic Accuracy |
|---|---|---|---|---|---|
| ABCD Rule | 78-98% | -- | 45-80% | 56-78% | 70-90% |
| Menzies Method | 86-95% | 54% | 38-76% | -- | 83% |
| Seven-Point Checklist (Classic) | 62-95% | 41% | 35-97% | -- | 16-88% |
| Revised Seven-Point Checklist | 88% | -- | 75% | -- | -- |
| CASH Algorithm | 87-98% | -- | 67% | -- | 68% |
| Pattern Analysis | 82-85% | -- | 61-79% | -- | 79-88% |
Key takeaways from the performance data:
Sensitivity: The ABCD rule, CASH algorithm, and Menzies method all achieve high sensitivity (>85%) for pigmented melanoma. The classic seven-point checklist has the widest sensitivity range (62-95%), reflecting its performance variation across different studies and examiner experience levels.
Specificity: Pattern analysis achieves the highest specificity range among experts (79-88%), confirming its role as the preferred method for experienced clinicians. The seven-point checklist shows the widest specificity range (35-97%), largely dependent on whether the classic or revised version is used and the examiner's experience.
Amelanotic melanoma: All algorithms perform significantly worse for amelanotic melanoma. The Menzies method reports only 54% sensitivity, and the seven-point checklist only 41%. This underscores the need for additional criteria (polymorphous vessels, shiny white structures, milky-red areas) when evaluating nonpigmented lesions.
Expert vs. nonexpert: Where data are available, specificity is consistently lower for nonexperts, indicating that algorithmic approaches partially but incompletely compensate for lack of experience.
7. Clinical Pearls
Start with global pattern assessment: Before applying any scoring algorithm, evaluate the lesion globally. Ask: "Does this look organized or disorganized?" An organized pattern matching one of the 10 benign nevus patterns provides strong reassurance -- but always check for melanoma-specific structures as a safety net.
The heterogeneity principle supersedes precise structure naming: Do not get bogged down debating whether a structure is an "irregular dot" or an "irregular globule." What matters is the heterogeneity in size, shape, color, and the chaotic distribution -- these features raise suspicion regardless of the precise label.
Algorithms are training wheels, not the bicycle: All four algorithms were designed primarily as educational and standardization tools for less experienced dermoscopists. As you gain experience, you will naturally shift toward pattern analysis. The algorithms remain valuable as a structured backup for difficult cases.
Gray and blue colors demand attention: Across all algorithms, blue-whitish veil and blue/gray structures appear repeatedly as important criteria. Gray peppering and blue-white veil are among the most diagnostically useful features. Never dismiss blue or gray coloration in a melanocytic lesion.
Context is not captured by algorithms: Patient age, skin type, lesion location, personal/family history, and evolution over time are all important diagnostic inputs that no algorithm formally incorporates. Always use algorithms in conjunction with clinical context.
The Menzies method's elegance lies in its negative features: The two negative features (symmetric pattern AND only one color) provide a simple, rapid exclusion of melanoma. If a lesion is perfectly symmetric in pattern AND shows only one color, melanoma is essentially excluded -- a powerful and fast screening tool.
Watch for "featureless" melanomas: A subset of early melanomas are flat and feature-poor/featureless. These will score low on all algorithms. Digital monitoring with sequential imaging is the key to detecting these lesions through identification of change over time.
Nodular lesions are a special category: Classic melanoma criteria are based predominantly on superficial spreading melanoma. Nodular melanomas may lack these features. Key clues for nodular melanoma include blue-black color, polymorphous vessels, milky-red areas, and shiny white lines. When in doubt about a nodular lesion, excise it -- never subject nodular lesions to short-term monitoring.
The revised 7-point checklist prioritizes not missing melanoma: With a threshold of 1 (any single criterion), the revised version is intentionally sensitive. This is appropriate in clinical settings where missing a melanoma has greater consequences than performing additional biopsies.
Newly described melanoma-specific structures are not in the algorithms: Shiny white lines, negative pigment network, and angulated lines are important melanoma-specific structures identified after these algorithms were published. Clinicians must actively look for these features even when using a formal scoring algorithm.
Clinical Vignettes
Clinical Scenario A 40-year-old woman presents with a 6 mm flat pigmented lesion on her upper back. On dermoscopy, you observe a relatively uniform brown pigment network at the periphery with a central homogeneous area. The network lines are of consistent width and spacing. Using the Menzies method, the lesion is symmetric in pattern and shows only two colors (light brown and dark brown). No positive features of melanoma are identified.
What is the most likely diagnosis?
Diagnosis: Benign compound nevus -- excluded from melanoma by the Menzies method.
This case illustrates Clinical Pearl 6: the Menzies method's two negative features -- symmetric pattern AND limited colors -- provide a simple, rapid exclusion of melanoma. However, always check for shiny white lines with polarized dermoscopy (Clinical Pearl 10), as these newly described melanoma-specific structures are not captured by the original algorithms.
Clinical Scenario A 55-year-old man presents with a 9 mm flat pigmented lesion on the left calf. Dermoscopy reveals an asymmetric lesion with broadened irregular network in one quadrant and a blue-white structure (regression) in another. ABCD score: Asymmetry 2.6, Border 0.3, Color 1.5, Dermoscopic structures 1.0. Total = 5.4.
What is the most likely diagnosis?
Diagnosis: Melanoma -- ABCD score of 5.4 falls in the suspicious range (4.75-5.45).
This demonstrates the utility of formal scoring algorithms for objective decision-making. However, Clinical Pearl 5 applies: context (age, history, location, evolution) is not captured by algorithms. The broadened atypical network and regression structures together are sufficient clinical indication for biopsy regardless of the algorithmic score.
Clinical Scenario A 62-year-old woman with many nevi presents with a 5 mm flat lesion on the right thigh that she feels has changed. Dermoscopy reveals a mostly featureless/structureless light brown pattern. The ABCD score is 2.1, the 7-point checklist scores 0, and the Menzies method identifies no positive features.
What is the appropriate management?
Management: Short-term digital dermoscopic monitoring -- a "featureless" lesion that algorithms cannot classify.
Clinical Pearl 7: a subset of early melanomas are flat and feature-poor. These score low on all algorithms. Digital monitoring with sequential imaging detects these lesions through change over time. However, per Clinical Pearl 8, this conservative approach is ONLY appropriate for flat lesions. If this lesion were raised or nodular, biopsy rather than monitoring would be mandatory.
9. Cross-References
| Topic | Reference |
|---|---|
| Pattern analysis for melanocytic lesions (full chapter) | Chapter 9a, pp. 216-219 |
| 10 benign nevus patterns (Figure + Table) | pp. 216-217 |
| Melanoma-specific criteria (Figure + Table) | pp. 217-218 |
| Key points for pattern analysis approach | p. 219 |
| ABCD rule of dermoscopy (Table) | Chapter 9b, pp. 220-221 |
| Menzies method (Table) | Chapter 9b, pp. 220-221 |
| Seven-point checklist -- classic and revised (Table) | Chapter 9b, pp. 222 |
| CASH algorithm (Table) | Chapter 9b, pp. 222 |
| Diagnostic accuracy comparison (Table) | Chapter 9b, pp. 223 |
| Summary of algorithm comparison | Chapter 9b, pp. 222-223 |
| Benign nevi patterns (detailed chapters) | Chapters 7a-7f, pp. 150-190 |
| Melanoma subtypes | Chapters 8a-8e, pp. 191-220 |
| Amelanotic/hypomelanotic melanoma | Chapter 8f, pp. 221-226 |
| Difficult to diagnose melanomas | Chapter 8e |
| Revised pattern analysis | Chapter 4a, pp. 42-49 |
| Chaos and Clues | Chapter 5a, pp. 81-91 |
| TADA and other triage algorithms | Chapters 5b-5c, pp. 92-100 |
| Rules to avoid missing melanoma | Chapter 9c, pp. 224-228 |
10. Related Modules
| Module | Title | Relationship |
|---|---|---|
| Module 03 | Pattern Analysis Revised | Foundation: geometric terminology and Chaos and Clues framework used in pattern analysis approach to differentiation |
| Module 04 | Top-Down 2-Step Algorithm | Alternative primary decision algorithm; Step 1 benign recognition complements the 10 benign nevus patterns |
| Module 05 | Prediction without Pigment | Essential complement for amelanotic/hypomelanotic lesions where all algorithms perform poorly |
| Module 06 | Chaos and Clues Triage Algorithm | Triage algorithm based on pattern analysis; uses chaos (asymmetry) and clues to guide biopsy decisions |
| Module 07 | TADA and Other Triage Algorithms | Introductory coverage of ABCD, Menzies, 7-point, CASH; this module provides the definitive detailed treatment |
| Module 15 | Congenital Melanocytic Nevi | Prerequisite: globular, reticular, and cobblestone patterns are among the 10 benign patterns |
| Module 16 | Acquired Melanocytic Nevi | Prerequisite: junctional, compound, and dermal nevi patterns form the basis of benign pattern recognition |
| Module 19 | Spitz and Reed Nevi | Prerequisite: starburst and peripheral globule patterns are among the 10 benign patterns; circumferential vs. segmental streaks is a critical distinction |
| Module 21 | Superficial Spreading Melanoma | Melanoma-specific criteria are most commonly seen in SSM; this module shows criteria in clinical context |
| Module 22 | Nodular Melanoma | Important limitation case: nodular melanomas may lack classic algorithmic criteria |
| Module 26 | Amelanotic and Hypomelanotic Melanoma | Important limitation case: all algorithms have significantly reduced sensitivity for amelanotic melanoma |
| Module 28 | Improving Sensitivity and Specificity | Direct continuation: 7 rules to avoid missing melanoma, comparative approach, digital monitoring |
Module 27 -- Version 1.0 Part of the Dermoscopy Educational Course.
Image Sources & Citations
- DERM12345 (Skin Lesion Dataset with 40 Subclasses): DERM12345: A Large-scale Skin Lesion Image Dataset with 40 Subclasses. Figshare. 2023. License: CC-BY-4.0.
- HIBA Dermoscopy Dataset: HIBA Dermoscopy Dataset. Hospital Italiano de Buenos Aires. License: CC-BY-4.0.