Module 26: Amelanotic and Hypomelanotic Melanoma
Dermoscopic Evaluation of Nonpigmented Melanoma
Source: Dermoscopy Educational Course
1. Learning Objectives
After completing this module, you should be able to:
- Define the distinction between amelanotic and hypomelanotic melanoma, including the role of eumelanin production in determining classification (pure amelanotic = no discernible eumelanin; hypomelanotic = low levels of eumelanin at least focally).
- Describe the frequency (2--8% of all melanomas), clinical presentation, and diagnostic challenge of amelanotic melanoma, explaining why these lesions frequently lack the classic ABCD criteria and may appear as symmetric pink lesions.
- Identify and classify the key dermoscopic vascular structures seen in amelanotic melanoma -- including dotted vessels, serpentine (linear irregular) vessels, hairpin vessels, milky-red areas/globules, and polymorphous patterns -- and explain how vessel morphology varies with tumor thickness and growth phase.
- Recognize shiny white structures (chrysalis/white lines), white network, and peripheral tan structureless areas as additional dermoscopic clues in amelanotic and hypomelanotic melanoma, particularly under polarized dermoscopy.
- Differentiate the vascular patterns of amelanotic superficial spreading melanoma (dotted vessels, orderly arrangement, thin tumors) from amelanotic nodular melanoma (polymorphous vessels, chaotic arrangement, thicker tumors).
- Distinguish amelanotic melanoma from its principal clinical mimics -- including pyogenic granuloma, basal cell carcinoma, squamous cell carcinoma, dermatofibroma, hemangioma, and amelanotic Spitz nevus -- using vessel morphology, arrangement, and associated dermoscopic clues.
- Apply the Prediction without Pigment algorithm framework (ulceration, white clues, vessel patterns) to the evaluation of suspected amelanotic melanoma, integrating clinical red flags and dermoscopic findings into a biopsy decision.
- Explain the optimal dermoscopic technique for evaluating amelanotic lesions, including minimal pressure application, use of ultrasound or octenidin gel as contact fluid, and the advantage of noncontact polarized dermoscopy for vessel and white structure visualization.
2. Prerequisites
- Module 01: Introduction and Principles of Dermoscopy -- understanding of polarized vs. nonpolarized dermoscopy is critical, as shiny white structures (chrysalis lines) are visible only under polarized light.
- Module 02: Histopathologic Correlations -- understanding of how vascular structures, dermal matrix alterations, and melanocyte distribution correspond to dermoscopic findings.
- Module 03: Pattern Analysis Revised -- foundational vocabulary of vessel structures (eight types), vessel arrangements (eight types), and the concepts of monomorphous vs. polymorphous patterns.
- Module 05: Prediction without Pigment -- the decision algorithm for nonpigmented lesions (ulceration --> white clues --> vessel patterns) provides the framework for evaluating amelanotic melanoma.
3. Key Concepts
The Challenge of Nonpigmented Melanoma
Amelanotic melanoma represents one of the most significant diagnostic challenges in clinical and dermoscopic dermatology. When melanin-based pigmentation is absent or minimal, the clinician loses the pigmented structures -- network, globules, streaks, blotches, blue-white veil -- that power most dermoscopic algorithms for melanoma detection. These lesions frequently lack the classic ABCD criteria (asymmetry, border irregularity, color variegation, diameter) that alert clinicians to pigmented melanoma, and they can convincingly mimic a wide range of benign and malignant entities, from inflammatory conditions to vascular tumors.
The dermoscopic evaluation of amelanotic melanoma therefore depends on an entirely different set of clues:
- Vascular patterns: The shape, arrangement, and context of blood vessels become the primary diagnostic information source.
- Shiny white structures: Chrysalis lines, white lines, and related structures visible under polarized dermoscopy reflect matrix remodeling by the tumor.
- Remnant pigmentation: In hypomelanotic variants, subtle focal pigmentation provides a valuable diagnostic anchor.
- Clinical context: Patient age, anatomic site, lesion history (growth, change), and the "ugly duckling" / clinical pattern-breaker concept become especially important.
The overarching principle is that although amelanotic melanomas lack pigment, they still induce neoangiogenesis and matrix remodeling. These biological processes produce visible dermoscopic clues that, when correctly identified and integrated, allow detection of many amelanotic melanomas that would otherwise be missed.
4. Core Content
4.1 Definition: Amelanotic vs. Hypomelanotic Melanoma
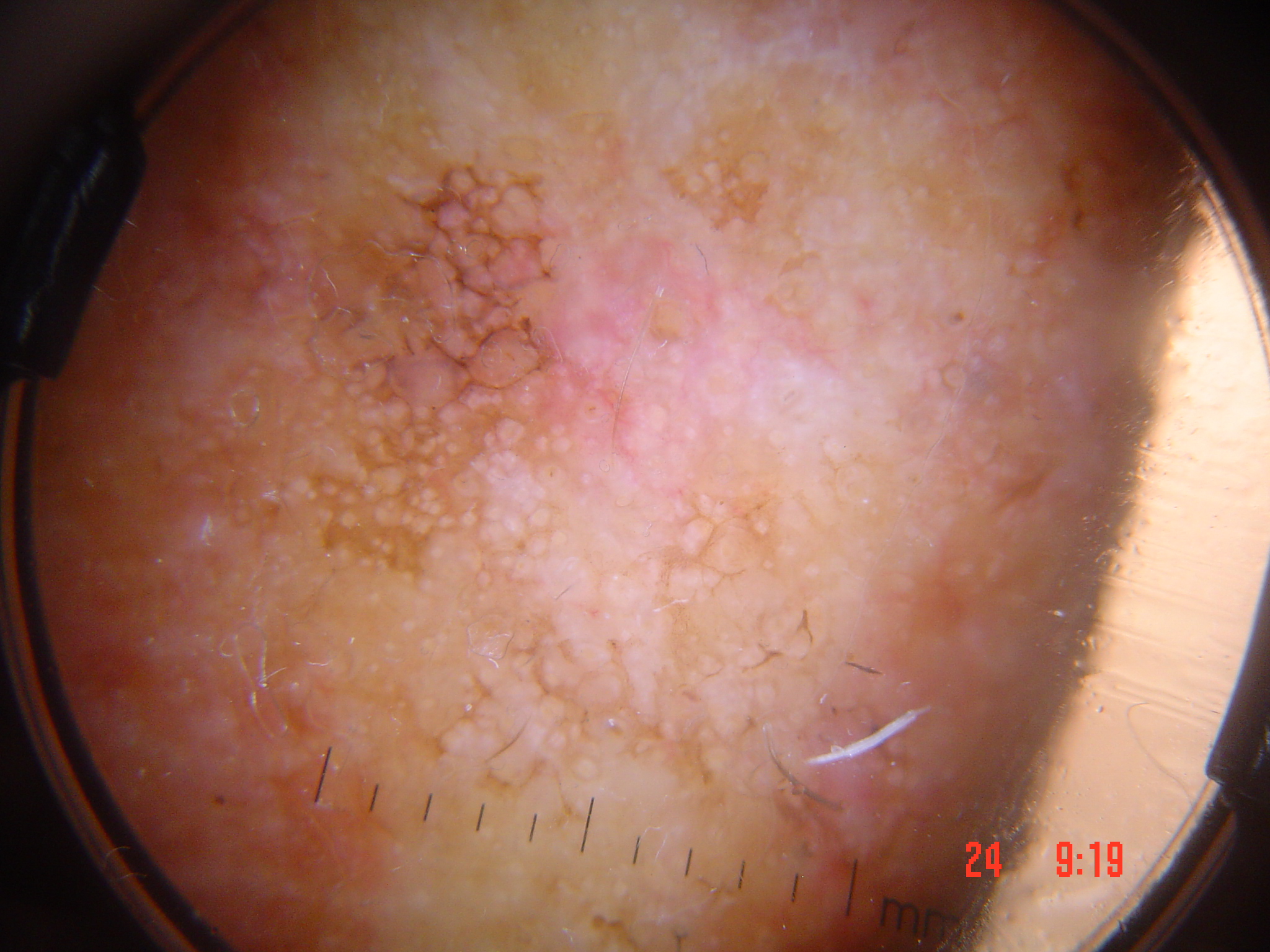
The term "amelanotic melanoma" is frequently employed as a clinical description for any melanoma lacking melanin pigmentation. However, a more precise classification distinguishes two categories:
- Pure amelanotic melanoma: Does not produce any discernible eumelanin. The lesion appears entirely pink/red/skin-colored both clinically and dermoscopically. No brown or gray pigmentation is visible at any magnification.
- Hypomelanotic melanoma: Produces low levels of eumelanin, at least in certain sections of the tumor. The lesion appears mainly amelanotic to the naked eye but reveals subtle melanin pigmentation when viewed with dermoscopy, often focally present as peripheral light brown structureless areas.
For clinical and dermoscopic purposes, both types present similar diagnostic challenges and are evaluated using the same approach. The presence of even subtle pigmentation in hypomelanotic variants, however, provides an additional diagnostic clue with a reported 93.8% positive predictive value for thin melanoma when peripheral tan structureless areas are identified.
Important distinction -- regressing melanoma: Melanomas in advanced stages of regression can appear hypopigmented or focally depigmented. However, this represents degradation of melanin rather than reduced production. These regressing melanomas are reliably distinguished by their dermoscopic features of scarlike depigmentation and peppering granularity (melanophages) and represent a separate diagnostic entity.
4.2 Frequency and Clinical Context
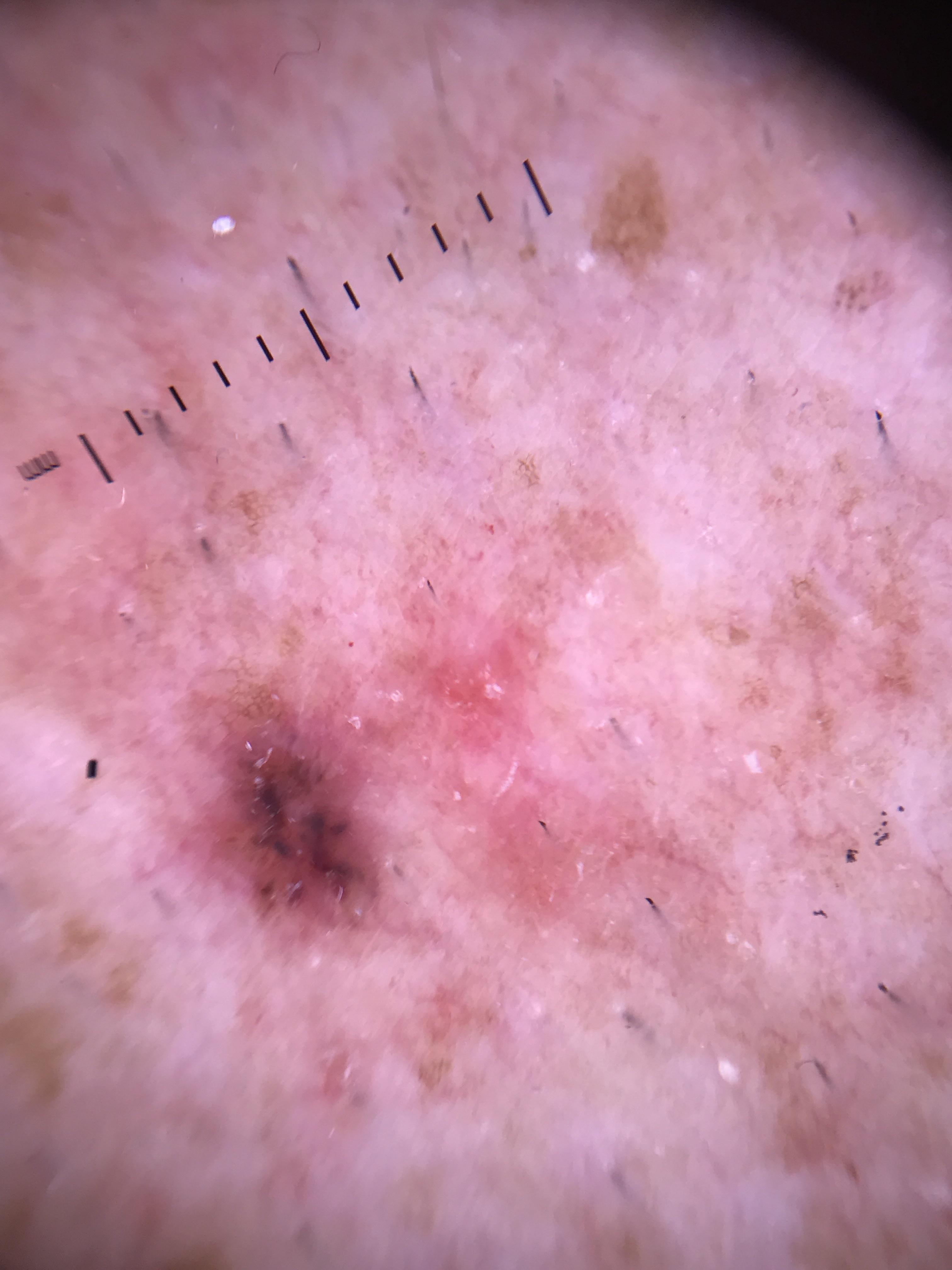
- Amelanotic melanoma accounts for at least 2--8% of all melanomas.
- Among nodular melanomas (NM), 30--40% are amelanotic or hypomelanotic.
- Amelanotic melanomas can present as either flat (superficial spreading) or nodular tumors.
Clinical presentation of flat (superficial spreading) amelanotic melanoma:
- Erythematous macules and plaques
- In most cases with well-defined borders and variable border irregularity
- With or without ulceration or light brown color at the periphery
- Not infrequently display a relatively symmetric silhouette -- this symmetry is due to the inability to visualize the irregular horizontal borders of the melanoma due to lack of pigment
- May reveal epidermal changes such as scale and/or disruption of skin markings
- Early amelanotic melanomas tend to display a symmetric shape both clinically and with the dermatoscope ("pink patch")
Clinical presentation of nodular amelanotic melanoma:
- Pink, elevated, firm, fast-growing tumors
- Tend to lack the classic ABCD criteria
- Better described by the EFG rule: Elevated, Firm, Growing
- May present as enlarging or changing amelanotic papules or nodules
Check Your Understanding
What are the primary dermoscopic features that help identify amelanotic melanoma?
The primary features include polymorphous vessels (combination of dotted, linear-irregular, and hairpin vessels), milky-red areas or globules, white shiny structures (visible only with PD), and absence of the typical dermoscopic criteria for benign lesions. The presence of multiple vessel types (polymorphous pattern) in a pink lesion is the single most important clue.
Key Takeaways
- Amelanotic melanoma is defined by the absence of classic pigmented dermoscopic features, making vascular patterns and white structures the primary diagnostic clues.
- The milky-red globular pattern (diffuse pink-red structureless areas with a milky quality) is characteristic of amelanotic melanoma and corresponds to neovascularization with thin, partially transparent epidermis.
- Dotted vessels combined with linear-irregular vessels (polymorphous vascular pattern) are the most common vascular finding in amelanotic melanoma.
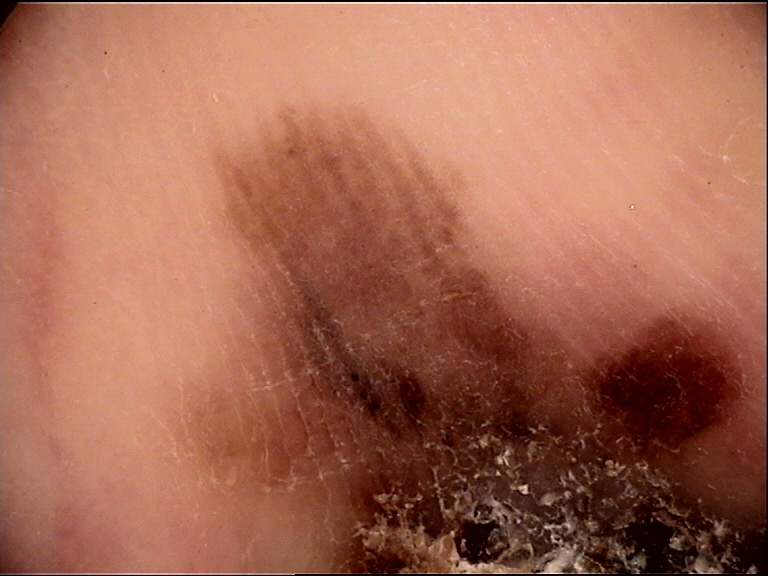
Clinical Scenario
A 59-year-old man presents with a 6 mm erythematous macule on his left forearm. Clinically it appears symmetric with well-defined borders. Dermoscopy reveals orderly arranged dotted vessels with subtle peripheral light brown structureless areas and shiny white lines under polarized light. No pigment network, globules, or blue-white veil are visible.
What is the most likely diagnosis, and what is the significance of the peripheral tan areas?
Hypomelanotic Superficial Spreading Melanoma
The orderly dotted vessels suggest a flat (superficial spreading) melanoma rather than nodular. The peripheral light brown structureless areas are a critical clue -- they represent focal residual melanin production and have a 93.8% positive predictive value for thin melanoma. The shiny white lines (visible only under polarized dermoscopy) indicate dermal matrix remodeling by the tumor. Despite the symmetric clinical appearance (a common trap in amelanotic melanoma), the combination of these features warrants biopsy.
4.3 Dermoscopic Features

The dermoscopic criteria for amelanotic melanomas rely on the analysis of vascular patterns and shiny white structures, which are only seen with polarized dermoscopy.
4.3.1 Polymorphous/Atypical Vessels
The single most important dermoscopic finding in amelanotic melanoma is the presence of polymorphous vessels -- a combination of two or more vessel morphologies within the same lesion. The most common combination is dotted and serpentine vessels.
Polymorphous vessels:
- Combination of 2 or more vessel morphologies in the same lesion
- Most common combination: dotted + serpentine (linear irregular) vessels
- PPV for melanoma: 52.6%
- Associated with amelanotic melanoma, desmoplastic melanoma, and cutaneous melanoma metastases
Specific vessel types seen in amelanotic melanoma:
| Vessel Type | Morphology | Association in Amelanotic Melanoma |
|---|---|---|
| Dotted | Red dots (0.01--0.02 mm), too small for discernible shape | Early/thin melanomas; 90% PPV for melanocytic lesion; also seen in Spitz nevi and Clark nevi |
| Serpentine (linear irregular) | Undulating short vessels with irregular course | Intermediate to thick melanomas; 67.6% PPV for melanoma; highly predictive of thicker (>2 mm) NM |
| Hairpin | U-shaped loop-like vessels, may be twisted on their axis | Thick melanomas and nodular melanomas; among the most important single vascular structures in NM |
| Corkscrew | Coiled and tortuous vessels | Cutaneous melanoma metastases, nodular melanoma, desmoplastic melanoma |
Predominantly central vessels are among the most predictive vascular features in melanoma.
4.3.2 Milky-Red Areas and Globules
Milky-red areas/globules are ill-defined areas or globules of milky-red color, representing diffuse neoangiogenesis within the tumor dermis. They are among the most diagnostically significant features of amelanotic melanoma.
- PPV for melanoma: 77.8%
- Ill-defined globules of milky-red color and/or ill-defined areas of milky-red color
- The milky-red background represents a diffuse vascular blush from neoangiogenesis
- Vessels surrounded by a milky-red background are associated with melanoma, whereas vessels surrounded by a white halo are associated with keratinizing tumors
- Milky-red areas are a key feature of amelanotic melanoma, desmoplastic melanoma, and nodular melanoma
4.3.3 Shiny White Structures (Chrysalis, Rosettes)
Shiny white structures are visible only with polarized dermoscopy and represent stromal matrix remodeling by the tumor. In amelanotic melanoma, where pigmented structures are absent, shiny white structures may be the only clue to malignancy alongside vascular patterns.
- Shiny white lines (chrysalis structures): Orthogonal white lines visible under polarized light; correspond to altered dermal collagen (fibrosis, desmoplasia)
- Shiny white streaks: Linear bright-white structures under polarized light
- In amelanotic NM: shiny white structures are almost always present along with polymorphous vessels
- Polarizing-specific white lines can also be seen in BCC, SCC in situ, LPLK, dermatofibroma, and Spitz nevus -- correlation with vessel morphology is needed to distinguish these
4.3.4 White Network (Inverse/Negative Network)
The negative network (also called inverse or white network) consists of serpiginous interconnected white lines surrounding darker globular structures. In melanoma, it represents elongated rete ridges with bridging connections.
- Negative network has an OR of 9.9 for nevus-associated melanomas
- Can be present in hypomelanotic melanomas as a subtle finding
- Visible under polarized light
4.3.5 Remnant Pigmentation
In hypomelanotic melanomas, subtle remnant pigmentation visible under dermoscopy provides critical diagnostic clues:
- Peripheral light brown structureless areas: The most significant feature of hypomelanotic melanoma; these tan structureless areas at the lesion periphery have a 93.8% positive predictive value for thin melanomas
- Peripheral dots/globules: Foci of brown dots and globules indicate melanocytic origin and can be the only evidence of the melanocytic nature of an otherwise amelanotic lesion
- Focal network remnants: Remnants of pigment network at the lesion periphery, sometimes as broadened atypical network
- Blue-white veil (focal): Even small foci of blue-white veil indicate melanin in the dermis with an overlying epidermal component
4.3.6 Ulceration
Ulceration may be present in amelanotic melanoma, particularly in nodular variants:
- True amelanotic, ulcerated nodular melanoma can present with linear irregular and dotted vessels over a milky-red background
- Ulceration impedes visualization of underlying structures
- In the Prediction without Pigment algorithm, ulceration is the first step assessed (highest priority)
- Ulceration promotes neoangiogenesis, producing additional polymorphous vessels
4.3.7 Blue-White Structures (Subtle)
While amelanotic melanomas by definition lack significant pigmentation, some hypomelanotic variants may display subtle blue-white structures:
- Blue-white veil: When present even focally, highly suggestive of melanoma (corresponds to orthokeratosis overlying melanin-containing cells in the dermis)
- Scarlike depigmentation: If present, suggests regression rather than true amelanosis
- Peppering/granularity: Fine blue-gray dots representing melanophages -- again suggests regression rather than primary amelanosis
- These features, when present, are often subtle and require careful examination
4.4 Vascular Patterns in Detail

Assessment Technique
To achieve optimal visualization of blood vessels in amelanotic lesions:
- Apply minimal pressure to avoid blanching the vessels
- Use ultrasound gel or octenidin gel as the contact fluid -- the high viscosity prevents flow, maintaining optical contact between the glass plate and the skin surface without pressure
- Control compression by raising and lowering the pressure of the glass plate and observing the disappearance and refilling of the vessels
- Consider noncontact polarized dermoscopy as an alternative -- this makes vessels more conspicuous and allows simultaneous visualization of shiny white streaks
Three-Component Vascular Assessment
Assessment of vascular structures in amelanotic melanoma comprises evaluation of three characteristics:
1. Shape (Morphology) of Blood Vessels:
- Dotted, serpentine, hairpin, corkscrew, comma, arborizing, glomerular
- See Tables 8F.1 and 8F.2 for comprehensive listings
2. Arrangement of Vessels:
- Random, clustered, serpiginous, linear, centered, radial, reticular, branched
- Predominantly central distribution is predictive of melanoma
- In early melanomas, vessels tend to be more orderly; in advanced melanomas, more chaotic
3. Additional Features:
- Vessels surrounded by a milky-red background --> associated with melanoma
- Vessels surrounded by a white halo --> associated with keratinizing tumors (SCC, SK)
- The presence of these contextual features significantly impacts diagnostic specificity
Vessel Morphology Related to Tumor Thickness
The morphology and arrangement of vessels in amelanotic melanoma evolve with tumor stage and thickness:
| Stage | Thickness | Typical Vessel Pattern | Arrangement |
|---|---|---|---|
| Early / thin | < 0.5 mm | Predominantly dotted vessels (homogeneous shape) | Orderly, relatively regular |
| Intermediate | 0.5--2 mm | Hairpin + serpentine vessels appear; dotted vessels may persist | Mixed; increasing irregularity |
| Thick / advanced | > 2 mm | Polymorphous: dotted + serpentine + hairpin + corkscrew | Chaotic, highly irregular |
- Early and thin amelanotic melanomas: vessels appear more orderly and homogeneous in shape with a predominant dotted pattern (note: dotted vessels alone are not predictive of melanoma)
- Intermediate thickness melanomas: hairpin and serpentine vessels appear; these vessel types are observed only in tumors with intermediate thickness (0.5--2 mm)
- Thick amelanotic melanomas: can present with highly irregular and often chaotic vascular structures
Check Your Understanding
Why are amelanotic melanomas frequently misdiagnosed, and how can dermoscopy improve detection?
Amelanotic melanomas lack the pigmented features (network, globules, streaks) that most diagnostic algorithms rely upon, so they are often clinically misdiagnosed as benign inflammatory or vascular lesions. Dermoscopy improves detection by revealing subtle vascular patterns (polymorphous vessels), milky-red globules, and white structures (under PD) that are invisible to the naked eye.
Clinical Scenario
A 66-year-old woman presents with a 9 mm pink, firm, elevated nodule on her right forearm that has been growing for 5 weeks. Dermoscopy reveals a chaotic arrangement of polymorphous vessels (dotted, serpentine, and hairpin), milky-red globules, a small central ulceration, and no pigmentation whatsoever.
What is the differential diagnosis, and which features favor melanoma over pyogenic granuloma?
Amelanotic Nodular Melanoma vs. Pyogenic Granuloma
Both amelanotic NM and pyogenic granuloma can present as rapidly growing pink/red nodules with ulceration. Key differentiating features: polymorphous vessels (multiple vessel types) strongly favor melanoma, whereas pyogenic granuloma typically shows a homogeneous pattern of dotted and looped vessels with a white collarette. The milky-red globules are characteristic of melanoma neoangiogenesis. The shiny white lines (if present under polarized light) would further support melanoma. The EFG criteria (Elevated, Firm, Growing >1 month) apply. In practice, any growing amelanotic nodule warrants excisional biopsy.
4.5 Amelanotic SSM vs. Amelanotic NM Features
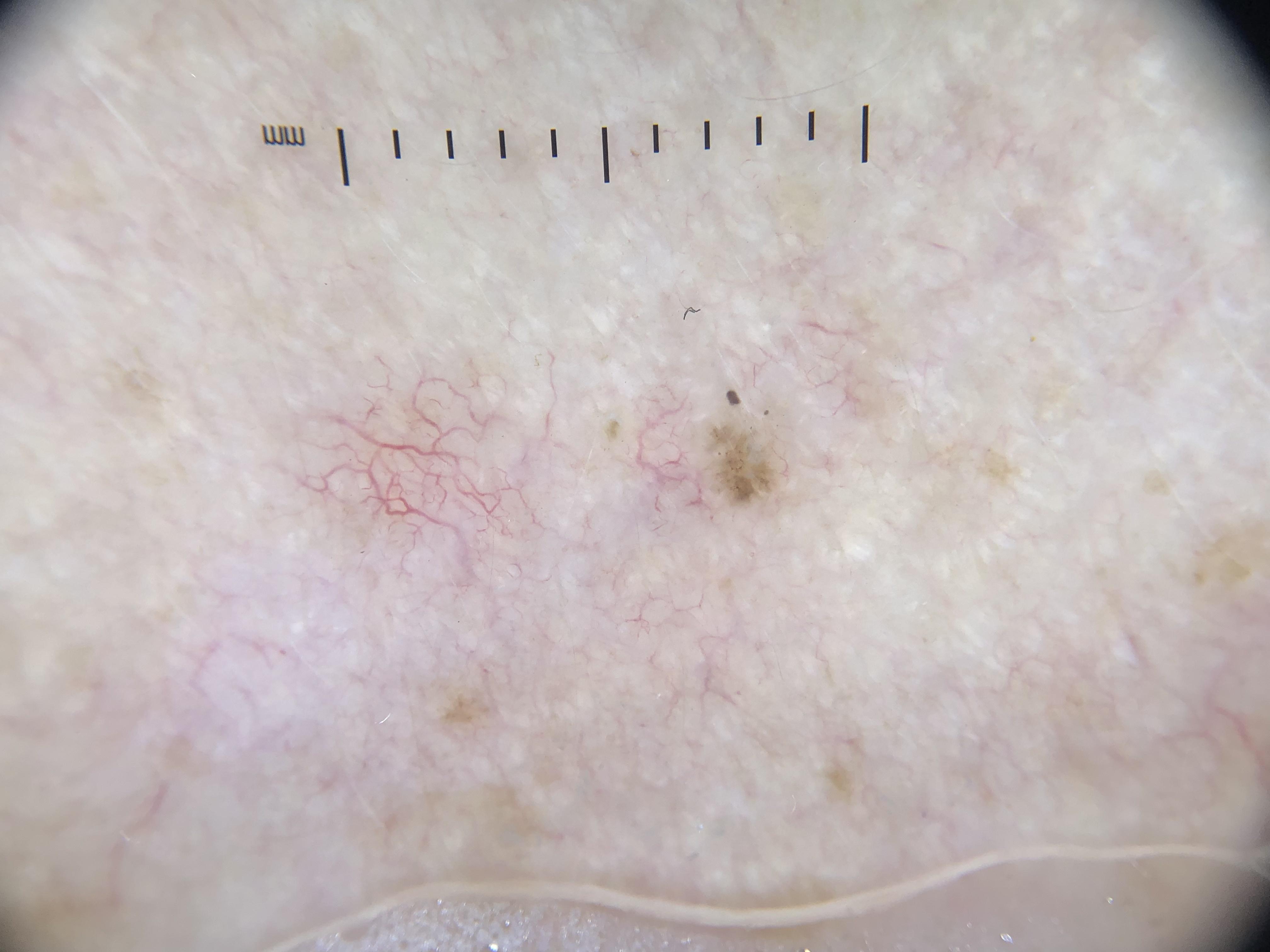
Amelanotic Superficial Spreading Melanoma (Flat)
- Presents as a "pink patch" -- erythematous macule or plaque
- Often displays a relatively symmetric silhouette clinically and dermoscopically
- Dermoscopic features: pink hue with dotted to serpentine to polymorphous vessels, with or without shiny white structures
- Vessels tend to be more orderly and uniform in early stages
- Hypomelanotic variants reveal peripheral light brown structureless areas (93.8% PPV for thin melanoma)
- Remnant pigment structures (focal network, dots, globules) may be visible
- Scale and disruption of skin markings can be present
- Lacks the ABCD features of pigmented SSM -- the symmetry is due to the inability to see irregular horizontal melanoma borders without pigment
Key dermoscopic features of hypomelanotic/amelanotic SSM (from the largest published series, >80% SSMs):
Most predictive non-regressing features (in order):
- Blue-white veil (when present)
- Irregularly shaped depigmentation
- Irregularly distributed and shaped brown dots/globules
- Five to six colors (in partially pigmented lesions)
- Predominantly central vessels
- Peripheral light brown structureless areas
- Asymmetrical pigmentation pattern
- Milky-red pink areas
- Greater than one shade of pink
- Asymmetrical shape
- Dotted and linear irregular vessels in combination
- Linear irregular vessels as the predominant vessel type
Features that were uncommon in amelanotic/hypomelanotic SSM:
- Multiple (>3) milia-like cysts (1%)
- Regularly distributed comma vessels (1%) or comma vessels as predominant type (2.9%)
- Blue-gray globules of irregular size or distribution (1.9%)
- Arborizing small-diameter vessels (6.7%) or arborizing as predominant type (8.6%)
- Symmetrical pigmentation pattern (7.6%)
Amelanotic Nodular Melanoma (ANM)
- Presents as a pink, elevated, firm, fast-growing nodule (EFG rule)
- 30--40% of all nodular melanomas are amelanotic or hypomelanotic
- Since there is minimal to no eumelanin to block dermoscopy light, ANMs almost always display:
- Polymorphous vascular pattern (the polymorphous vessels usually consist of dotted and serpentine vessels)
- Shiny white structures
- Rarely will there be comma-shaped vessels (as in IDN) or arborizing configuration (as in BCC)
- Serpentine vessels are highly predictive of thicker (>2 mm) NMs
- Irregular brown dots/globules are predictive of NM less than 2 mm in thickness
- Ulceration may impede visualization of underlying structures
- May display milky-red areas/globules as a prominent feature
Summary table from Chapter 8e:
| Feature | Amelanotic NM |
|---|---|
| Key dermoscopic findings | Shiny white structures + atypical vessels (polymorphous pattern) |
| Clinical characteristics | Many lack classic ABCD; palpable; elevated, firm, growing |
| Histopathological basis | Vertical growth of malignant melanocytes into dermis with matrix alteration; lack of radial growth phase |
Key Takeaways
- Polymorphous vessels (two or more vessel morphologies in a single lesion) are the strongest vascular clue to amelanotic melanoma, reflecting the chaotic angiogenesis of the tumor.
- Amelanotic melanoma can retain trace pigment visible only under dermoscopy as subtle tan-brown areas, irregular dots, or faint regression; these residual clues can be diagnostic.
- White shiny lines under polarized dermoscopy are frequently present in amelanotic melanoma and reflect the dermal stromal response to tumor invasion.
4.6 Clinical Mimics: Differential Diagnosis
Amelanotic melanoma can mimic a wide range of pink, nonpigmented lesions. Distinguishing it from these mimics is one of the central challenges in dermoscopy.
Amelanotic Spitz Nevus
- Can present with a vascular pattern of dotted vessels similar to amelanotic melanoma
- Dotted vessels in regular arrangement highly predictive of melanocytic lesion (90% PPV)
- Cannot always be reliably distinguished from early amelanotic melanoma by dermoscopy
- Rule: Excision is recommended for any pink solitary lesion with this vascular pattern, as amelanotic Spitz nevi and amelanotic melanoma can be indistinguishable dermoscopically
Basal Cell Carcinoma (BCC)
- Characterized by arborizing (branched serpentine) vessels with a translucent stroma that casts vessels into sharp relief
- 94% PPV for BCC when arborizing vessels are present
- Arborizing vessels are uncommon in melanoma (seen in only 6.7--8.6% of amelanotic/hypomelanotic melanomas)
- Polarizing-specific white lines are the most frequent white clue in BCC
- Key distinction: BCC shows monomorphous branched serpentine vessels; melanoma shows polymorphous vessels including dotted vessels
- Some overlap exists -- biopsy prior to any nonsurgical treatment of amelanotic lesions is essential
Squamous Cell Carcinoma (SCC) / Bowen Disease
- Bowen disease (SCC in situ): May present with glomerular (coiled) vessels mimicking the glomerular apparatus of the kidney (61.9% PPV for Bowen disease)
- SCC/KA: White circles (87% specific), surface keratin, white structureless areas
- Vessels surrounded by a white halo are associated with keratinizing tumors (SCC, SK) -- this contrasts with the milky-red background of melanoma
- Key distinction: Glomerular/coiled vessels and keratin clues favor SCC; polymorphous vessels with dotted + linear irregular over milky-red background favor melanoma
Dermatofibroma (DF)
- Amelanotic dermatofibroma can present with vascular patterns that overlap with early melanoma
- May show polarizing-specific white lines (similar to BCC and melanoma)
- Central white scar-like area with peripheral pigment network (when pigmented)
- Key distinction: In nonpigmented variants, early DF may be difficult to distinguish; clinical context (firm papule, dimple sign) is important
Hemangioma / Angioma
- Characterized by clods-only pattern (red, purple, blue well-circumscribed structures)
- In angiomas, lacunae are separated by well-defined septae
- Key distinction from melanoma metastases: Melanoma metastases with angioma-like pattern show milky-red globules that are not separated by septae or have irregularly defined septae; atypical vessels may be seen within the lacunae-like structures
Pyogenic Granuloma
- May present as a rapidly growing pink-red nodule with ulceration
- Can mimic amelanotic nodular melanoma clinically
- Key distinction: Pyogenic granulomas typically show homogeneous red coloring, white collarette, and homogeneous vascular pattern without the polymorphous vessels characteristic of melanoma
Melanocytic Nevi with Fibrotic Modification
- Pink, nonpigmented variants can mimic early amelanotic melanoma
- Comma vessels in regular arrangement have 94% PPV for intradermal/congenital nevus
- Key distinction: Comma vessels and regular arrangement favor benign nevus; polymorphous vessels and milky-red background favor melanoma
Check Your Understanding
What benign lesions most commonly mimic amelanotic melanoma on dermoscopy?
The most common mimics include pyogenic granuloma (homogeneous red structureless area with a collarette), dermatofibroma (central white patch with peripheral network), inflamed seborrheic keratosis, and clear cell acanthoma (string-of-pearls vascular pattern). Hemangioma with thrombosis can also mimic amelanotic melanoma. Polymorphous vessels and lack of benign-specific features favor melanoma.
4.7 Prediction without Pigment Algorithm Application
The Prediction without Pigment algorithm (Module 05, Chapter 4c) provides the systematic framework for evaluating amelanotic melanoma. When confronting a nonpigmented lesion of concern:
Step 1: Is there ulceration?
- If yes --> biopsy recommended. Amelanotic melanoma (especially nodular) can present with ulceration. Ulceration is also common in BCC and SCC.
- Additional dermoscopic clues can then predict the specific diagnosis.
Step 2: Are white clues present?
- Polarizing-specific white lines can be seen in amelanotic melanoma (as well as BCC, SCC in situ, DF, Spitz nevus)
- If white lines are present --> biopsy recommended
- Use vessel patterns as supplementary evidence: polymorphous vessels including dotted vessels favor melanoma over BCC
Step 3: Vessel pattern analysis (when no ulceration or white clues)
- If the pattern is one of the four benign monomorphous patterns (clods-only, centered, serpiginous, reticular) --> likely benign (with caveats)
- If polymorphous vessels are present, especially dotted + serpentine/linear irregular --> suspect melanoma
- If dotted vessels over a milky-red background --> suspect melanoma
- All other vessel patterns (not fitting benign monomorphous patterns) --> assess for biopsy
Application to amelanotic melanoma specifically:
- Amelanotic melanoma typically reaches the algorithm at Step 2 (if white lines are present) or Step 3 (vessel pattern analysis)
- The combination of dotted + linear vessels is a frequent pattern in amelanotic melanoma and is not seen in BCC
- Milky-red areas are a strong clue that the nonpigmented lesion is melanoma rather than another malignancy
Key Takeaways
- The principal differentials for amelanotic melanoma include pyogenic granuloma (collarette, homogeneous red), BCC (arborizing vessels), SCC (glomerular/hairpin vessels with keratin), and Merkel cell carcinoma (linear-irregular vessels).
- A pink or red lesion that is growing and cannot be confidently diagnosed as benign by dermoscopy should be biopsied; the clinical maxim is that amelanotic melanoma is a diagnosis often made by histology after biopsy of an uncertain lesion.
- Applying the nonpigmented lesion algorithm (Prediction without Pigment) to any pink-red growing lesion increases the detection rate of amelanotic melanoma.
4.8 When to Suspect Amelanotic Melanoma
The following clinical and dermoscopic scenarios should raise suspicion for amelanotic melanoma:
- Isolated, pink outlier lesion -- even if the lesion does not manifest any of the classic ABCD criteria for melanoma. The "ugly duckling" concept applies to nonpigmented lesions as well.
- Erythematous symmetric lesion -- amelanotic melanomas not infrequently present as symmetric pink patches or plaques.
- EFG lesion -- any elevated, firm, growing pink nodule should be suspected for amelanotic NM.
- Polymorphous vessels (especially dotted + serpentine) over a milky-red background -- this combination is highly suggestive of melanoma.
- Shiny white structures without other specific features -- in a nonpigmented lesion, shiny white structures with atypical vessels should raise concern for melanoma.
- Peripheral tan structureless areas -- subtle brown pigmentation at the lesion periphery in an otherwise pink lesion strongly suggests hypomelanotic melanoma.
- Any pink lesion that cannot be confidently identified as one of the common benign entities (nevus, SK, hemangioma, DF, sebaceous hyperplasia, cyst) or as BCC/SCC.
Check Your Understanding
What is the significance of the 'milky-red' color in dermoscopy?
Milky-red areas or globules represent areas of neoangiogenesis and increased vascularity within a lesion. This color is strongly associated with melanoma (both pigmented and amelanotic) and represents one of the key features detected by polarized dermoscopy. It reflects increased and disorganized blood vessel proliferation within the tumor stroma.
4.9 Index of Suspicion Criteria
The following findings, individually or in combination, increase the index of suspicion for amelanotic melanoma:
High suspicion (strongly favor melanoma):
- Milky-red areas/globules (PPV 77.8%)
- Serpentine (linear irregular) vessels as predominant type (PPV 67.6%)
- Polymorphous vessels: dotted + serpentine combination (PPV 52.6%)
- Peripheral light brown structureless areas (PPV 93.8% for thin melanoma)
- Predominantly central vessels
Moderate suspicion (require biopsy for clarification):
- Shiny white structures (chrysalis lines) in a nonpigmented lesion
- Dotted vessels over a pink background (90% PPV for melanocytic lesion, but not specific for melanoma)
- Any polymorphous vessel pattern in a lesion that is not clearly benign
- Hairpin vessels in a pink nodule
Supporting clinical features:
- Clinical pattern-breaker / ugly duckling
- Patient concern or documented evidence of change
- EFG criteria (elevated, firm, growing)
- Location on chronically sun-exposed skin in an elderly patient
- Solitary pink lesion that defies confident diagnosis
Important caveat: Although the presence of the aforementioned vessel morphologies is not 100% specific for amelanotic melanoma, their presence in the correct clinical context can be suggestive of melanoma. As a rule, excision is recommended for any pink solitary lesion displaying these vascular patterns when it cannot be confidently classified as benign.
Key Takeaways
- Amelanotic melanoma is the most commonly missed melanoma subtype in both clinical and dermoscopic practice because it lacks the pattern features that most algorithms rely on.
- Polarized dermoscopy is essential for evaluating amelanotic lesions because shiny white structures, vascular details, and subtle residual pigment are best appreciated under cross-polarized light.
- Any persistent pink papule or nodule that does not respond to empiric treatment (antibiotics, steroids) within 4-6 weeks should be biopsied to exclude amelanotic melanoma.
5. Amelanotic Melanoma Features Reference Table
Table A: Vascular Structures in Melanocytic Tumors
| Dermoscopic Structure | Morphology | Diagnostic Associations | Comment |
|---|---|---|---|
| Comma vessels | Slightly curved vessels | Dermal nevi, congenital melanocytic nevi | 94% PPV for intradermal nevus/congenital nevus |
| Hairpin vessels | U-shaped loop-like vessels; may be twisted on axis; pink halo common in irritated SK but can be seen in melanoma | Thick melanomas | Most important single vascular structures in NM are linear irregular vessels and hairpin vessels |
| Dotted vessels | Red dots (0.01--0.02 mm) | Spitz nevi and early melanoma (dotted over milky-red background); Clark nevi (dotted over tan background) | 90% PPV for melanocytic skin lesion |
| Serpentine (linear irregular) | Undulating short vessels | Melanoma, congenital nevi | 67.6% PPV for melanoma |
| Milky-red globules / vascular blush | Ill-defined globules of milky-red color and ill-defined areas of milky-red color | Melanoma (including amelanotic, desmoplastic, nodular melanoma) | 77.8% PPV for melanoma |
| Polymorphous | Combination of 2+ vessel morphologies; most common: dotted + serpentine | Melanoma (including amelanotic, desmoplastic), cutaneous melanoma metastases | 52.6% PPV for melanoma |
| Corkscrew | Coiled and tortuous vessels | Cutaneous melanoma metastases, nodular melanoma, desmoplastic melanoma | -- |
Table B: Vascular Structures in Nonmelanocytic Tumors
| Dermoscopic Structure | Morphology | Diagnostic Association | Comment |
|---|---|---|---|
| Glomerular vessels | Coiled vessels mimicking kidney glomerular apparatus | Bowenoid AK, Bowen disease / SCC in situ, clear cell acanthoma | 61.9% PPV for Bowen disease |
| Hairpin vessels | U-shaped vessels; may be twisted; white halo common in keratinocytic tumors | Keratinizing tumors (keratoacanthoma, SK); rarely BCC (2.6%) | 70% PPV for SK |
| Arborizing vessels | Large diameter vessels branching irregularly into fine capillaries | BCC; also cysts, furuncles, adnexal tumors | 94% PPV for BCC |
| Crown vessels | Branching or nonbranching vessels radiating toward center of lesion but not crossing center; often with yellowish "popcorn" globules | Sebaceous hyperplasia, molluscum contagiosum | 83% PPV for sebaceous hyperplasia |
| Dotted/glomerular in serpiginous distribution | Vessels in a serpiginous pattern | Clear cell acanthoma | 100% PPV (pathognomonic) |
| Strawberry pattern | Pink to red pseudonetwork with white-yellow circles (adnexal openings) over erythematous background | Actinic keratosis | -- |
Table C: Non-Vascular Dermoscopic Features in Amelanotic/Hypomelanotic Melanoma
| Feature | Description | Significance |
|---|---|---|
| Shiny white structures | Orthogonal white lines, white streaks (polarized light only) | Matrix remodeling; present in amelanotic NM and SSM |
| Peripheral tan structureless areas | Subtle light brown structureless areas at lesion periphery | 93.8% PPV for thin melanoma; key feature of hypomelanotic melanoma |
| Milky-red background | Diffuse ill-defined pink-red background color | Neoangiogenesis; distinguishes melanoma from keratinizing tumors (which have white halos around vessels) |
| Remnant network | Focal areas of pigment network at periphery | Indicates melanocytic origin; often broadened/atypical |
| Brown dots/globules | Focal irregular brown dots or globules | Indicate melanocytic origin; irregularly distributed in melanoma |
| Scale/disruption of skin markings | Epidermal changes visible on surface | Can be present in flat amelanotic SSM |
| Negative network | White interconnecting lines forming inverse network | OR 9.9 for nevus-associated melanoma |
6. Amelanotic Melanoma vs. Clinical Mimics Differential Table
| Feature | Amelanotic Melanoma | BCC | SCC / Bowen | Hemangioma | Spitz Nevus (Amelanotic) | Dermatofibroma | Pyogenic Granuloma |
|---|---|---|---|---|---|---|---|
| Predominant vessel type | Polymorphous (dotted + serpentine) | Arborizing (branched serpentine) | Glomerular / coiled | Clods-only | Dotted (regular) | Variable; comma-like | Homogeneous red |
| Vessel arrangement | Random to chaotic; predominantly central | Branched | Linear or serpiginous | Clods-only pattern | Regular, orderly | Variable | Homogeneous |
| Milky-red areas | Present (77.8% PPV) | Absent | Absent | Absent | Absent or minimal | Absent | Absent |
| White halo around vessels | Absent | Absent | Present (keratinizing) | Absent | Absent | Absent | Absent |
| Shiny white structures | Often present (polarized light) | White lines common | Less common | Absent | May be present | May be present | Absent |
| Translucent stroma | Absent | Present (casts vessels into sharp focus) | Absent | Absent | Absent | Absent | Absent |
| Surface keratin / white circles | Absent | May be present if ulcerated | Characteristic (87% specific for SCC) | Absent | Absent | Absent | Absent |
| Ulceration | May be present (nodular) | Frequently present | May be present | Rare | Rare | Absent | Common |
| Pigment remnants | Possible (hypomelanotic) | Possible (pigmented BCC) | Absent | Absent | Absent | Peripheral network | Absent |
| Key distinguishing clue | Polymorphous vessels + milky-red background | Arborizing vessels + translucent stroma | Glomerular vessels + white circles | Clods without linear vessels within | Regular dotted vessels | Firm papule with dimple sign | White collarette; rapid growth |
| Clinical context | Solitary pink outlier; EFG | Ulcerated nodule; sun-damaged skin | Scaly plaque; sun-exposed | Stable red papule; typical morphology | Young patient; dome-shaped | Firm papule; lateral compression sign | Rapid growth; bleeding history |
7. Clinical Pearls
"Consider amelanotic melanoma for any isolated, pink outlier lesion." Even if the lesion does not manifest any classic ABCD criteria, an isolated pink lesion that does not match the surrounding lesion pattern (the "ugly duckling" sign applied to nonpigmented lesions) warrants careful dermoscopic evaluation and a low threshold for biopsy.
Symmetry can be deceptive. It is not uncommon for amelanotic melanomas to present as erythematous symmetric lesions. The apparent symmetry is an artifact of the lack of pigment -- the irregular horizontal borders of the melanoma are invisible without melanin. Do not use symmetric shape alone to dismiss a pink lesion.
Minimal pressure is essential for vascular assessment. Apply as little pressure as possible during dermoscopy of amelanotic lesions to avoid blanching the vessels. Use ultrasound gel or octenidin gel as the contact fluid for optimal visualization. Noncontact polarized dermoscopy is an excellent alternative.
Milky-red background is the vascular context that separates melanoma from keratinizing tumors. Vessels over a milky-red background suggest melanoma (PPV 77.8%), while vessels surrounded by a white halo suggest keratinizing tumors (SCC, SK). This contextual feature is as important as vessel morphology itself.
Vessel morphology reflects tumor thickness. Early melanomas show orderly dotted vessels; intermediate-thickness tumors develop hairpin and serpentine vessels; thick tumors display chaotic polymorphous vessels. Understanding this progression helps correlate dermoscopic findings with tumor stage.
Dotted vessels alone are not diagnostic of melanoma. While dotted vessels have 90% PPV for a melanocytic lesion, they are also seen in Spitz nevi, Clark nevi, and other conditions. It is the combination with linear irregular vessels (polymorphous pattern) that raises the strongest suspicion for melanoma.
The periphery holds the clue in hypomelanotic melanoma. Peripheral light brown structureless areas (93.8% PPV for thin melanoma) may be the most diagnostically valuable feature of hypomelanotic melanoma. Always examine the lesion periphery carefully for subtle brown pigmentation that may not be apparent clinically.
Biopsy before nonsurgical treatment of any amelanotic lesion. Because of the overlap between amelanotic melanoma and other malignant amelanotic lesions (particularly BCC), it is easier to distinguish all malignant amelanotic/hypomelanotic lesions from benign lesions than to discriminate melanoma from other malignancies. This underscores the importance of histopathologic confirmation before any nonsurgical treatment.
Shiny white structures and vessels can be the only dermoscopic clues. In true amelanotic melanoma with no pigmentation whatsoever, vascular structures and shiny white streaks (seen with polarized light only) may be the only available diagnostic information. This emphasizes the critical importance of using polarized dermoscopy for all nonpigmented lesion evaluations.
Apply the EFG rule to pink nodules. Any pink nodule that is elevated, firm, and growing should be considered for excision regardless of dermoscopic findings. The EFG rule was developed specifically to capture nodular melanomas -- including amelanotic variants -- that escape detection by the conventional ABCD criteria.
Clinical Vignettes
Clinical Scenario A 56-year-old woman presents with a 7 mm pink macule on her upper back that she noticed 4 months ago. Dermoscopy reveals dotted vessels in a relatively regular arrangement over a pink background. Subtle light brown structureless areas are present at the periphery, occupying approximately 15% of the lesion surface. No white structures, ulceration, or blue-white veil is visible.
What is the most likely diagnosis?
Diagnosis: Hypomelanotic melanoma.
The peripheral light brown structureless areas are the critical diagnostic clue. With a 93.8% PPV for thin melanoma, these subtle areas may be the most diagnostically valuable feature of hypomelanotic melanoma (Clinical Pearl 7). The dotted vessels alone have 90% PPV for a melanocytic lesion but are not melanoma-specific (Clinical Pearl 6). The combination of dotted vessels with peripheral light brown structureless areas in a new lesion should prompt biopsy.
Clinical Scenario A 64-year-old man presents with a 9 mm firm, pink, dome-shaped nodule on the left shoulder that has been growing over 8 weeks. Dermoscopy reveals polymorphous vessels: dotted, hairpin, and serpentine in a disorganized arrangement. Milky-red areas are present centrally. Shiny white structures are visible with polarized dermoscopy. No pigmentation whatsoever is seen.
What is the most likely diagnosis?
Diagnosis: True amelanotic nodular melanoma.
Shiny white structures and vessels can be the only dermoscopic clues (Clinical Pearl 9). The polymorphous vessels reflect tumor thickness (Clinical Pearl 5). The milky-red background separates melanoma from keratinizing tumors with PPV 77.8% (Clinical Pearl 4). The EFG rule applies (Clinical Pearl 10): elevated, firm, and growing mandates excision. Never treat an amelanotic lesion nonsurgically without biopsy first (Clinical Pearl 8).
Clinical Scenario A 71-year-old woman presents with a 5 mm pinkish papule on the right forearm. Dermoscopy reveals a milky-pink background with a few dotted vessels and faint serpentine vessels. No pigmentation, no white structures, no ulceration, and no specific pattern is identified. The lesion does not fit any recognizable benign category. She states it appeared about 3 months ago and has been slowly growing.
What is the most likely diagnosis?
Diagnosis: Possible amelanotic melanoma -- "featureless" pattern requiring biopsy.
The key reasoning is that the lesion does not match any specific benign entity. When a lesion cannot be confidently classified as benign, and it is new and growing, biopsy is the appropriate next step. The absence of features diagnostic of any specific benign entity is itself a red flag. Minimal pressure during dermoscopy is essential (Clinical Pearl 3) to avoid blanching vessels that may be the only diagnostic clue.
9. Cross-References
| Topic | Reference |
|---|---|
| Chapter 8f: Amelanotic and Hypomelanotic Melanoma (primary source) | Chapter 8f, pp. 210--215 |
| Vascular structures in melanocytic tumors -- comprehensive table | Chapter 8f |
| Vascular structures in nonmelanocytic tumors -- comprehensive table | Chapter 8f |
| Partially pigmented melanoma with milky-red nodule | Chapter 8f |
| Regressive melanoma with polymorphic vessels | Chapter 8f |
| True amelanotic ulcerated NM with linear irregular + dotted vessels | Chapter 8f |
| Amelanotic NM with polymorphic vessels and milky-red areas | Chapter 8f |
| Hypomelanotic melanoma with hairpin + serpentine vessels | Chapter 8f |
| Early melanomas with dotted vessels and variable brown color | --8F.11 |
| Amelanotic melanoma with atypical vessels and shiny white structures | Chapter 8f |
| Amelanotic SSM variants (hypomelanotic features, PPV data) | Chapter 8a, pp. 181--184 |
| Amelanotic SSM with arborizing vessels -- importance of biopsy before nonsurgical treatment | Chapter 8a |
| Hypomelanotic SSM with pin-point vessels and peripheral brown areas | Chapter 8a |
| Nodular melanoma -- amelanotic NM dermoscopic characteristics | Chapter 8b, pp. 188--189 |
| Amelanotic NM with dotted vessels and hairpin vessels | Chapter 8b |
| Amelanotic/hypomelanotic NM classification and features | Chapter 8e |
| Flat amelanotic melanoma: pink patch with polymorphous vessels | Chapter 8e |
| Prediction without Pigment algorithm and flowchart | Chapter 4c |
| Amelanotic melanoma with polarizing-specific white lines | Chapter 4c |
| Polymorphous vessels with dots favoring melanoma vs. BCC | Chapter 4c |
| Argenziano G et al. -- Vascular structures PPV data | Arch Dermatol. 2004;140(12):1485--9 |
| Menzies SW et al. -- Dermoscopic evaluation of amelanotic and hypomelanotic melanoma | Arch Dermatol. 2008;144(9):1120--7 |
| Jaimes N et al. -- Clinical and dermoscopic characteristics of amelanotic non-nodular melanomas | J Eur Acad Dermatol Venereol. 2012;26(5):591--6 |
| Pizzichetta MA et al. -- Amelanotic/hypomelanotic melanoma clinical and dermoscopic features | Br J Dermatol. 2004;150(6):1117--24 |
| Menzies SW et al. -- Dermoscopic evaluation of nodular melanoma | JAMA Dermatol. 2013;149(6):699--709 |
| Chamberlain AJ et al. -- EFG rule for nodular melanoma | J Am Acad Dermatol. 2003;48(5):694--701 |
| Balagula Y et al. -- Significance of crystalline/chrysalis structures | J Am Acad Dermatol. 2012;67(2):194.e1--8 |
| Zalaudek I et al. -- Vascular structures Part I (melanocytic tumors) | J Am Acad Dermatol. 2010;63(3):361--74 |
| Zalaudek I et al. -- Vascular structures Part II (nonmelanocytic tumors) | J Am Acad Dermatol. 2010;63(3):377--86 |
10. Related Modules
| Module | Relationship |
|---|---|
| Module 05: Prediction without Pigment | Essential prerequisite -- provides the systematic algorithm (ulceration --> white clues --> vessel patterns) used to evaluate amelanotic melanoma. The present module is the disease-specific deep dive that applies that algorithmic framework to melanoma. |
| Module 22: Nodular Melanoma | Companion module -- covers all NM including pigmented variants; 30--40% of NMs are amelanotic/hypomelanotic. The blue-black rule, EFG criteria, and dermoscopic patterns of pigmented NM complement the amelanotic NM content in this module. |
| Module 01: Introduction and Principles | Prerequisite -- polarized vs. nonpolarized dermoscopy understanding is critical, as shiny white structures (chrysalis lines) are visible only with polarized light and are a key diagnostic clue in amelanotic melanoma. |
| Module 03: Pattern Analysis Revised | Prerequisite -- vessel structure types, vessel arrangements, and the monomorphous/polymorphous distinction are foundational concepts applied throughout this module. |
| Module 08: Dermatofibroma | Differential diagnosis -- amelanotic DF can mimic early amelanotic melanoma; polarizing-specific white lines can be present in both entities. |
| Module 09: Basal Cell Carcinoma | Differential diagnosis -- arborizing vessels, translucent stroma, and ulceration overlap with BCC; distinguishing BCC from amelanotic melanoma by vessel morphology (monomorphous arborizing vs. polymorphous with dotted vessels) is a critical clinical skill. |
| Module 10: Actinic Keratosis | Differential diagnosis -- strawberry pattern and surface changes of AK contrast with the vascular patterns of amelanotic melanoma. |
| Module 11: SCC Spectrum | Differential diagnosis -- glomerular vessels, white circles (87% specific), and keratin clues of SCC/Bowen disease vs. the polymorphous dotted + serpentine pattern of melanoma. |
| Module 13: Vascular Lesions | Differential diagnosis -- hemangioma (clods-only pattern) and pyogenic granuloma are important clinical mimics of amelanotic melanoma. |
| Module 20: Spitz Nevus | Differential diagnosis -- amelanotic Spitz nevi can present with dotted vessels indistinguishable from early amelanotic melanoma; excision is recommended for both. |
This module is part of the Dermoscopy Educational Course. For the complete course outline and suggested study paths, see COURSE_OUTLINE.md.
Image Sources & Citations
- DERM12345 (Skin Lesion Dataset with 40 Subclasses): DERM12345: A Large-scale Skin Lesion Image Dataset with 40 Subclasses. Figshare. 2023. License: CC-BY-4.0.
- HIBA Dermoscopy Dataset: HIBA Dermoscopy Dataset. Hospital Italiano de Buenos Aires. License: CC-BY-4.0.