Module 07: TADA and Other Triage Algorithms
Source: Dermoscopy Educational Course
Authors cited: Natalia Jaimes, Ashfaq Marghoob (Ch 5b); Natalia Jaimes (Ch 5c, Ch 9b); Ralph Braun, Susana Puig, Josep Malvehy (Ch 8d)
1. Learning Objectives
After completing this module, the learner should be able to:
- Describe the three-step architecture of the Triage Amalgamated Dermoscopy Algorithm (TADA) and apply it to lesions on non-glabrous skin.
- List the two patterns, two structures, and four colors evaluated in TADA Step 3, and explain why each is suspicious.
- Apply the three-point checklist to pigmented lesions and calculate whether a lesion meets the biopsy threshold.
- Explain the AC rule and its intended use in layperson and community screening for melanoma.
- Define the blue-black rule, including the 10% surface area criterion, and state when it should and should not be applied.
- Calculate a total dermoscopy score (TDS) using the ABCD rule of dermoscopy, including the weighted multiplication factors, and interpret the score against diagnostic thresholds.
- Apply the Menzies method by evaluating negative and positive features to determine melanoma suspicion.
- Score a lesion using both the classic and revised seven-point checklist, and compare their sensitivity/specificity trade-offs.
- Calculate a CASH algorithm score and identify the threshold for melanoma suspicion.
- Apply the BRAAFF checklist to volar (acral) lesions and interpret the score for melanoma risk.
- Compare the diagnostic performance (sensitivity, specificity, diagnostic accuracy) of all major dermoscopic algorithms and select the most appropriate algorithm for a given clinical scenario.
2. Prerequisites
- Module 01: Introduction and Principles of Dermoscopy (equipment, polarized vs. non-polarized light)
- Module 02: Histopathologic Correlations of Dermoscopic Structures (structural terminology)
- Module 03: Pattern Analysis Revised (basic elements, patterns, and colors)
- Module 06: Chaos and Clues Triage Algorithm (chaos assessment, nine clues to malignancy)
3. Key Concepts
Triage vs. Diagnosis
Triage refers to the sorting and classification of lesions to determine which require biopsy or referral. The primary goal is to avoid missing skin cancer (maximize sensitivity). Making a specific histological diagnosis (e.g., distinguishing BCC from SCC from melanoma) is a secondary objective during triage.
Multiple Algorithms Exist for Good Reason
Different algorithms serve different purposes, populations, and settings:
- Triage algorithms (TADA, three-point checklist, AC rule, blue-black rule, Chaos and Clues) prioritize high sensitivity to avoid missing cancers.
- Differentiation algorithms (ABCD rule, Menzies method, seven-point checklist, CASH) use semi-quantitative scoring to distinguish benign from malignant among lesions already flagged as suspicious.
- Site-specific algorithms (BRAAFF) address unique anatomic locations such as volar skin.
The Asymmetry Principle
Virtually every dermoscopic algorithm includes asymmetry (of color, structure, or both) as a core criterion. Asymmetry in the distribution of dermoscopic colors and structures is the single most reproducible and powerful predictor of malignancy across all algorithms.
No Single Algorithm Is Perfect
All algorithms have trade-offs between sensitivity and specificity. Newer structures (shiny white lines, negative network, angulated lines) identified since the original publication of many algorithms have not yet been formally incorporated, and clinicians should not ignore these features when using any algorithm.
4. Core Content
PART A: TADA Algorithm (Chapter 5b)
Architecture and Philosophy
The Triage Amalgamated Dermoscopic Algorithm (TADA) is a three-step algorithm created by Jaimes, Marghoob, and colleagues to provide a simple method for guiding management decisions about whether a lesion should undergo biopsy or be referred to an expert clinician. TADA is specifically a triage algorithm that incorporates key criteria for malignancy derived from multiple existing algorithms.
Key design principles:
- TADA amalgamates criteria from established algorithms (ABCD rule, three-point checklist, Chaos and Clues, blue-black rule, AC rule) into a single streamlined workflow.
- It was designed and tested on lesions located on non-glabrous skin only. It cannot be used on lesions on volar surfaces, nails, or mucosae.
- It requires polarized light dermoscopy for Steps 2 and 3.
Performance Data
TADA has been tested in reader studies with clinicians and nurse practitioners:
| Metric | Range |
|---|---|
| Sensitivity | 88.1% -- 94.8% |
| Specificity | 72.3% -- 87.8% |
(Rogers et al., 2016; Seiverling et al., 2019)
TADA Algorithm Flowchart
flowchart TD
A[Lesion Identified] --> B{Step 1: Unequivocal<br/>SK, Angioma, or DF?}
B -->|Yes| C[Benign -- Reassure<br/>Patient]
B -->|No| D{Step 2: Pattern<br/>Organized or<br/>Disorganized?}
D -->|Disorganized| E[Suspicious --<br/>Biopsy]
D -->|Organized| F{Step 3: Any of<br/>2 Patterns, 2 Structures,<br/>or 4 Colors?}
F -->|Starburst or<br/>Negative Network| G[Biopsy<br/>Recommended]
F -->|Vessels or<br/>Ulceration| G
F -->|Blue, Black,<br/>Gray, or White| G
F -->|None Present| H{Lesion<br/>Palpable?}
H -->|No| I[Monitor with<br/>Digital Dermoscopy]
H -->|Yes / Raised| J[Consider Excision]
Three-Point Checklist Flowchart
flowchart TD
A[Pigmented Lesion] --> B{1. Asymmetry of<br/>color/structures?}
B -->|+1 point| C{2. Blue-white<br/>structures?}
B -->|0 points| C
C -->|+1 point| D{3. Atypical<br/>network?}
C -->|0 points| D
D -->|+1 point| E[Calculate Total<br/>Score]
D -->|0 points| E
E -->|Score >= 2| F[Biopsy or Referral<br/>Recommended]
E -->|Score 0-1| G[Low Suspicion --<br/>Monitor]
Step-by-Step TADA Application
TADA Step 1: Is the Lesion an Unequivocal Seborrheic Keratosis, Angioma, or Dermatofibroma?
The observer first determines whether the lesion fulfills the clinical and dermoscopic criteria for an unequivocal benign lesion from one of the three most commonly encountered categories:
- Seborrheic keratosis (SK) -- gyri and sulci (ridges and fissures), milia cysts, comedo-like openings, cerebriform pattern, well-demarcated borders
- Angioma -- red or blue-black lacunae separated by septae
- Dermatofibroma (DF) -- peripheral network with a central scar-like area, ring-like structures
If unequivocally benign: Reassure the patient. No further evaluation required.
If not unequivocally benign: Proceed to Step 2.
Clinical Note: Less common benign lesions (clear cell acanthoma, molluscum, xanthogranuloma, etc.) are not formally included in TADA Step 1. However, experienced clinicians who can confidently identify other benign entities may add them to the Step 1 list.
TADA Step 2: Does the Lesion Manifest a Disorganized Pattern?
Only lesions that are not unequivocally benign proceed to Step 2, which requires polarized light.
The observer assesses whether the lesion demonstrates an organized or disorganized pattern. Dermoscopic patterns take into account the distribution of colors and structures within the lesion.
- Disorganized pattern (chaotic distribution of colors and structures): Lesion is considered suspicious -- perform skin biopsy.
- Organized pattern: Proceed to Step 3.
Asymmetry (chaos or disorganized pattern) is the most important characteristic to help differentiate benign from malignant tumors. It is reproducible and demonstrates the highest inter-observer agreement.
TADA Step 3: Does the Organized-Appearing Lesion Manifest One of Two Patterns, Two Structures, or Four Colors?
Only equivocal lesions demonstrating an organized pattern proceed to Step 3, which also requires polarized light.
The observer evaluates for the presence of any of the following features:
1. Any one of two patterns:
| Pattern | Description | Significance |
|---|---|---|
| Starburst pattern | Streaks or globules forming a starburst (radial) arrangement | Can be seen in Spitz/Reed nevi but also in melanoma. Suspicious especially in individuals over age 12 years. Biopsy recommended. |
| Negative network pattern | Serpiginous negative (lighter) network throughout the lesion | Both Spitz nevi and melanomas can display this pattern. Biopsy recommended. |
2. Any one of two structures:
| Structure | Description | Significance |
|---|---|---|
| Vessels | Any vascular structure of any morphology | Lesions revealing any vascular structures should be biopsied. |
| Ulceration | Ulceration or erosions | Suspect lesion; biopsy recommended. |
3. Any one of four colors:
| Color | Clinical Significance |
|---|---|
| Blue | Blue-black color has high sensitivity for nodular melanoma. |
| Black | Concerning when present in an organized lesion not clearly a benign entity. |
| Gray | Important clue for skin cancer, particularly melanomas on sun-damaged skin. Blue-gray granularity has strong association with melanoma. |
| White | Includes shiny white structures (polarizing-specific) and white circles. Shiny white lines/streaks are melanoma-specific; shiny white blotches and strands are BCC-specific; white circles are associated with well-differentiated SCC. Although some benign lesions (DF, LPLK, Spitz nevi) may show white structures, for triage purposes any white color should be viewed with suspicion. |
Decision after Step 3:
- If any of the above features are present: Malignancy should be considered -- biopsy recommended.
- Additional considerations (outside the three-step flow):
- Lesions on volar skin (palms/soles) displaying a parallel ridge pattern should be considered suspicious.
- Any changing lesion in an adult should be considered suspicious for malignancy.
- If none of the above features are present and the lesion is nonpalpable: The lesion can be monitored (see digital monitoring approaches, Module 37).
Check Your Understanding
What does TADA stand for, and what is the key principle behind this algorithm?
TADA stands for Triage Amalgamated Dermoscopic Algorithm. Its key principle is simplification: rather than requiring identification of specific structures, TADA asks whether the lesion has any architectural disorder or is a 'gray, blue, or white' lesion. If the answer to either is yes, the lesion warrants biopsy or referral.
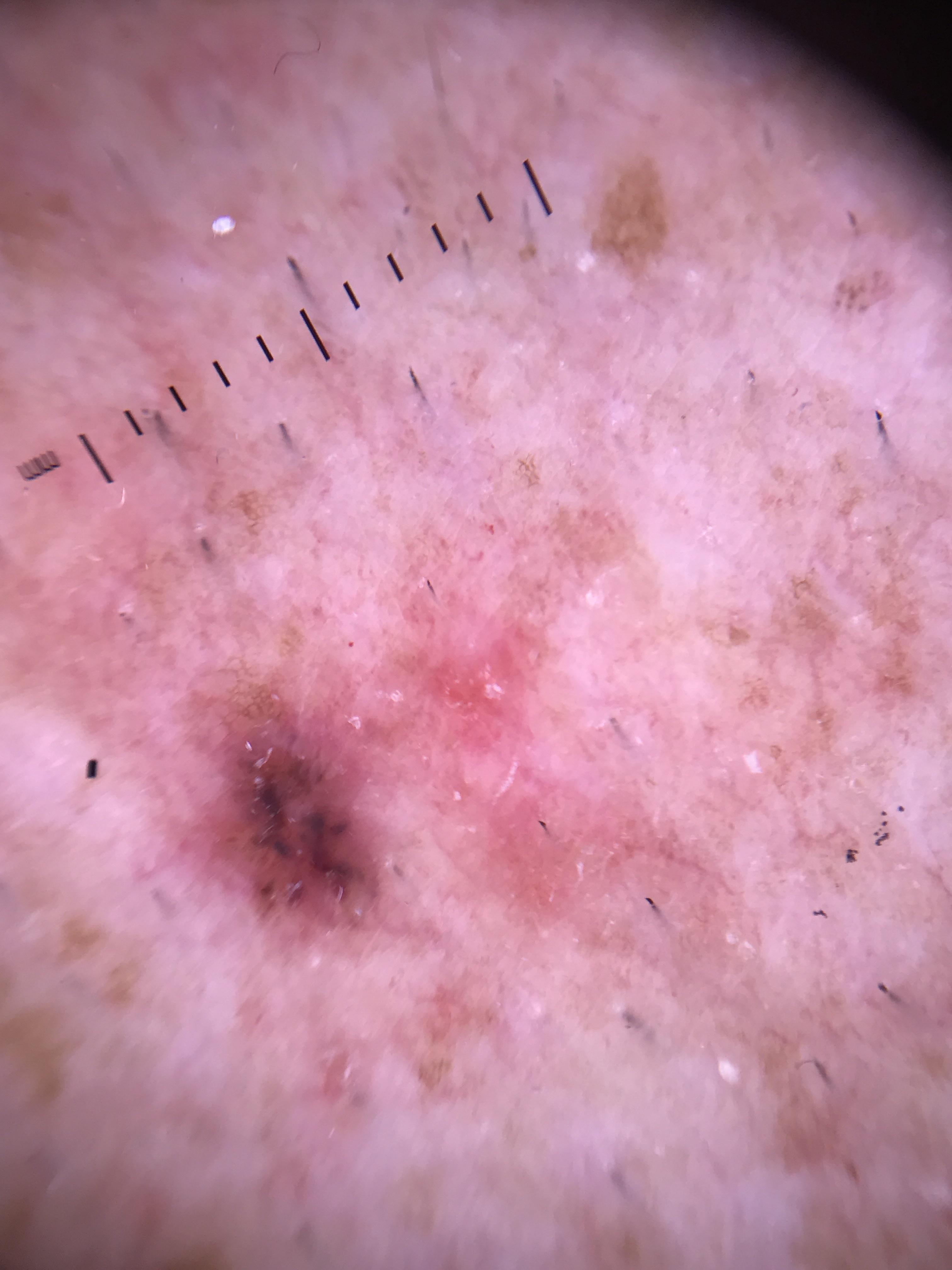
Clinical Scenario
A 56-year-old woman presents with a 7 mm pigmented papule on the right forearm that she noticed changing over 3 months. You apply the TADA algorithm. Step 1: the lesion is not an unequivocal SK, angioma, or dermatofibroma. Step 2: the overall pattern appears organized -- colors and structures are relatively symmetrically distributed. Step 3: you examine for the 2-2-4 criteria and find shiny white lines visible under polarized dermoscopy.
What is your diagnosis and key dermoscopic findings?
Suspicious lesion requiring biopsy (TADA Step 3 positive)
Despite the organized appearance (Step 2 negative), TADA Step 3 detects white structures (shiny white lines under polarized light), which is one of the four suspicious colors. Any one of the 2 patterns, 2 structures, or 4 colors in Step 3 is sufficient to recommend biopsy. White structures are a critical finding because shiny white lines can indicate melanoma (dermal invasion with stromal alteration) or BCC (shiny white blotches and strands from mucin and BCC matrix). This case demonstrates why Step 3 is essential -- organized-appearing malignancies would be missed without screening for these specific features.
Key Takeaways
- TADA (Triage Amalgamated Dermoscopic Algorithm) is designed for non-expert users and uses simple architectural disorder plus any specific feature to flag lesions for referral.
- The 3-point checklist (asymmetry, atypical network, blue-white structures) achieves high sensitivity and is suitable for primary care screening.
- The ABCD rule provides a quantitative total dermoscopy score (TDS) where scores above 5.45 indicate high melanoma probability.
- Menzies method requires both a negative feature (absence of symmetry and single color) and at least one of nine positive features for melanoma diagnosis.
PART B: Other Dermoscopic Algorithms in Skin Cancer Triage (Chapter 5c)
Overview
Chapter 5c organizes triage algorithms into three categories based on lesion pigmentation:
| Category | Algorithms |
|---|---|
| Pigmented lesions | Three-point checklist, AC rule, Blue-black rule, Chaos and Clues |
| Non-pigmented lesions | Prediction without Pigment (see Module 05) |
| Pigmented and non-pigmented | TADA |
Overall, algorithms for pigmented lesions have a sensitivity of 78.2%--92.9% and a specificity of 64%--92.3% for the diagnosis of pigmented skin cancers including melanoma and BCC.
Limitation: Algorithms designed for pigmented lesions will not help detect amelanotic or hypomelanotic skin cancers. Since the main purpose of these algorithms is to avoid missing pigmented skin cancer, some benign pigmented lesions (thrombosed hemangiomas, angiokeratomas, pigmented SK) may be misclassified as suspicious and subjected to biopsy.
Three-Point Checklist
Purpose: Initially developed for non-experts as a skin cancer screening tool.
Criteria (one point each):
| # | Criterion | Definition |
|---|---|---|
| 1 | Asymmetry | Asymmetry in the distribution of dermoscopic color and/or structures in one or two perpendicular axes. The contour or silhouette of the lesion does not factor into symmetry assessment. |
| 2 | Blue-white structures | Blue-white veil, and/or white scar-like depigmentation, and/or blue pepper-like granules. |
| 3 | Atypical network | Pigment network with thick lines and irregular-sized holes. |
Scoring: One point per criterion present. A score of 2 or 3 = positive (biopsy or referral recommended).
Hierarchy of predictive value: Asymmetry in the distribution of colors and structures is the best predictor of malignancy, followed by blue-white structures, then atypical network.
Performance:
| Metric | Range |
|---|---|
| Sensitivity (melanoma and BCC) | 79% -- 91% |
| Specificity (melanoma and BCC) | 71% -- 72% |
Limitation: The three-point checklist was not developed to identify pigmented SCC. It is therefore recommended that any pigmented lesion with focal adherent keratin or a rough texture revealing an asymmetric dermoscopic pattern be considered suspicious to avoid missing pigmented SCC.
Check Your Understanding
What are the three criteria in the 3-Point Checklist, and how many must be present to warrant excision?
The three criteria are: (1) asymmetry of pattern, (2) atypical network (thick lines, irregular holes), and (3) blue-white structures. The presence of any two out of three criteria warrants excision or biopsy. This algorithm was designed for simplicity and is useful for less experienced dermoscopists.
AC Rule
Purpose: Developed as a simple rule to identify lesions suspicious for melanoma, suitable for the wider community including laypersons.
Criteria:
| Letter | Criterion | Definition |
|---|---|---|
| A | Asymmetry | Asymmetry in the distribution of structures and colors. |
| C | Color variation | Multiple colors within the lesion, with black or blue-gray color being most suggestive of melanoma. |
Scoring: Both criteria present = suspicious for melanoma.
Performance (tested in laypersons):
| Metric | Value |
|---|---|
| Sensitivity (melanoma) | 94% |
| Specificity (melanoma) | 62% |
Blue-Black Rule
Purpose: Proposed specifically to identify pigmented nodular melanomas, which often appear as symmetric papules or nodules and may be missed by algorithms relying heavily on asymmetry.
Definition: The blue-black feature is defined as the presence of a combination of blue and black areas involving at least 10% of the lesion surface area.
Exclusions: The blue-black feature is NOT counted when:
- Unequivocal comedo-like openings (as found in seborrheic keratosis) are present with the blue-black background.
- Dark lacunae (as seen in angiokeratomas) occur with the blue-black background.
Performance:
| Metric | Value |
|---|---|
| Sensitivity (melanoma) -- blue-black rule alone | 78.2% |
| Sensitivity (melanoma) -- blue-black rule + melanoma-specific structures | 84.6% |
| Specificity (melanoma) -- blue-black rule alone | 80.5% |
| Specificity (melanoma) -- melanoma-specific structures only | 97.6% |
| Specificity (melanoma) -- both criteria combined | 80.5% |
Additional melanoma-specific structures evaluated alongside the blue-black rule include: atypical network, negative network, irregular streaks, regression structures, and irregular brown structureless areas.
Note: In addition to detecting nodular melanoma, the presence of blue-black color can also aid in detection of other heavily pigmented skin malignancies, including pigmented nodular BCCs.
ABCD Rule of Dermoscopy
Purpose: A semi-quantitative scoring system created by Stolz and colleagues (1994) for the evaluation of pigmented lesions. This is a differentiation algorithm (not purely a triage tool).
Criteria and Scoring:
| Criterion | Assessment | Points | Multiplication Factor | Score Range |
|---|---|---|---|---|
| A -- Asymmetry | Contour AND content (color/structure distribution) in two perpendicular axes | 0 (none), 1 (mono-axial), 2 (bi-axial) | x 1.3 | 0 -- 2.6 |
| B -- Border | Abrupt cutoff of pigmentation at perimeter; lesion divided into 8 pie-shaped sections; score 1 for each segment with abrupt cutoff | 0 -- 8 | x 0.1 | 0 -- 0.8 |
| C -- Colors | Presence of: white, red, light brown, dark brown, blue-gray, black (1 point each) | 1 -- 6 | x 0.5 | 0.5 -- 3.0 |
| D -- Dermoscopic structures | Presence of: pigment network, branched streaks, dots, globules, homogeneous/structureless areas (1 point each). Homogeneous areas include hyperpigmented blotches, hypopigmented areas, depigmented or scar-like areas involving >10% of the lesion surface. | 1 -- 5 | x 0.5 | 0.5 -- 2.5 |
Total Dermoscopy Score (TDS): Sum of all four weighted scores.
| TDS | Interpretation |
|---|---|
| < 4.75 | Benign |
| 4.75 -- 5.45 | Suspicious |
| > 5.45 | Highly suggestive of malignancy (melanoma) |
TDS range: 1.0 -- 8.9 (theoretical: 0.5 -- 8.5 per some sources)
Important note: In contrast to most other algorithms, the ABCD rule of dermoscopy and the CASH algorithm are the only methods that take into account both the contour (shape) and the content (color/structure distribution) of the lesion during asymmetry evaluation.
Performance:
| Metric | Range |
|---|---|
| Sensitivity (pigmented melanoma) | 78% -- 98% |
| Specificity (experts) | 45% -- 80% |
| Specificity (non-experts) | 56% -- 78% |
ABCDE Modification
The ABCDE method is a clinical (not dermoscopic) modification that adds E for Evolution to the original clinical ABCD criteria (Asymmetry, Border irregularity, Color variation, Diameter >6 mm). The E criterion acknowledges that change over time (evolution) is an important indicator of melanoma.
While the delineation of dermoscopic algorithms has certainly improved diagnostic accuracy, the ABCDE method for clinical examination remains a useful adjunct, though it is limited in cases where nevi and melanoma are difficult to distinguish clinically.
Reference: Rigel DS, Friedman RJ, Kopf AW, Polsky D. ABCDE -- an evolving concept in the early detection of melanoma. Arch Dermatol. 2005;141:1032-4.
Check Your Understanding
In the ABCD rule of dermoscopy, what four features are scored and what is the threshold for suspicion?
The ABCD rule scores Asymmetry (0-2), Border irregularity (0-8), Color diversity (1-6 colors), and Dermoscopic structures (1-5 types). Each is multiplied by a weighting factor. A total dermoscopy score (TDS) above 5.45 suggests melanoma, while scores below 4.75 suggest a benign lesion.
Menzies Method
Purpose: Developed to differentiate invasive melanomas from other pigmented lesions.
Structure: Evaluates 11 dermoscopic criteria classified into negative features (low sensitivity for melanoma when absent) and positive features (high specificity for melanoma, >85%).
Negative Features (2) -- Neither can be present in melanoma:
| Feature | Definition |
|---|---|
| Symmetrical pigmentation pattern | Symmetric pigment pattern across all axes |
| Presence of only one color | Only one of: tan, dark brown, black, gray, blue, red |
If both negative features are present: the diagnosis of melanoma is excluded.
Positive Features (9) -- At least one must be present to consider melanoma:
| # | Feature | Description |
|---|---|---|
| 1 | Blue-white veil | Irregular and confluent blue pigmentation with an overlying white "ground glass" film, not associated with red-blue lacunae |
| 2 | Multiple brown dots | Aggregations of dark brown dots, usually within the body of the lesion |
| 3 | Pseudopods | Finger-like projections with small knobs at their tips, directly connected to the tumor body or pigment network |
| 4 | Radial streaming | Radial and asymmetric linear extensions at the edge of the lesion |
| 5 | Scar-like depigmentation | White, irregular area of depigmentation |
| 6 | Peripheral black dots/globules | Black dots or globules at or near the edge of the lesion |
| 7 | Broadened network | Pigment network with areas of thick grids |
| 8 | Multiple blue/gray dots | Diffuse, partly aggregated dots, "pepper-like" in appearance |
| 9 | Multiple colors | Presence of five or more colors (of the six: tan, dark brown, black, gray, blue, red) |
Decision logic: If both negative features are present AND no positive feature is present, melanoma is excluded. If any positive feature is present, melanoma should be suspected.
Performance:
| Metric | Range |
|---|---|
| Sensitivity (pigmented melanoma) | 86% -- 95% |
| Sensitivity (amelanotic melanoma) | 54% |
| Specificity (experts) | 71% -- 78% |
| Specificity (non-experts) | 38% -- 76% |
| Diagnostic accuracy | 83% |
Seven-Point Checklist
The seven-point checklist evaluates seven dermoscopic features frequently associated with melanoma, categorized into major and minor criteria.
Classic Version (Argenziano et al., 1998)
Major Criteria (2 points each):
| Criterion | Definition | Score |
|---|---|---|
| Atypical pigment network | Prominent (hyperpigmented or thick) and irregular network | 2 |
| Blue-whitish veil | Irregular, structureless white-blue area with an overlying "ground glass" film; cannot occupy the entire lesion | 2 |
| Atypical vascular pattern | Linear irregular or dotted vessels, irregularly distributed outside areas of regression | 2 |
Minor Criteria (1 point each):
| Criterion | Definition | Score |
|---|---|---|
| Irregular streaks | Radial and asymmetric linear or bulbous projections at the edge of the lesion | 1 |
| Irregular blotches | Black, brown, and/or gray structureless areas with irregular shape or distribution | 1 |
| Irregular dots and globules | Black or brown round structures irregularly distributed | 1 |
| Regression structures | White scar-like depigmentation and/or "peppering" | 1 |
Scoring:
- Major criteria range: 0 -- 6 points
- Minor criteria range: 0 -- 4 points
- Total score range: 0 -- 10 points
- Threshold for melanoma: Total score of 3 or more
flowchart TD
A[Pigmented Lesion] --> B{Major Criteria}
B --> C[Atypical pigment<br/>network? +2]
B --> D[Blue-whitish<br/>veil? +2]
B --> E[Atypical vascular<br/>pattern? +2]
A --> F{Minor Criteria}
F --> G[Irregular<br/>streaks? +1]
F --> H[Irregular<br/>blotches? +1]
F --> I[Irregular dots<br/>& globules? +1]
F --> J[Regression<br/>structures? +1]
C & D & E & G & H & I & J --> K[Total Score<br/>0-10 points]
K -->|Score >= 3| L[Suspicious for<br/>melanoma -- Biopsy]
K -->|Score < 3| M[Low suspicion --<br/>Monitor or reassure]
Revised Version (Argenziano et al., 2010)
The revised seven-point checklist lowered the threshold for biopsy:
- Each criterion (major or minor) scores 1 point (all criteria weighted equally)
- Threshold for excision: Total score of 1 or more (i.e., the presence of any single criterion is sufficient to consider a lesion suspicious)
- Result: Higher sensitivity but lower specificity compared to the classic version
The authors acknowledge that a sensitive and specific method requires consideration of additional context: clinical characteristics, age and skin type, lesion location, whether the lesion is an outlier (comparative approach), and whether it has changed during follow-up.
Performance:
| Version | Sensitivity | Specificity |
|---|---|---|
| Classic (score >= 3) | 62% -- 95% | 35% -- 97% |
| Revised (score >= 1) | 88% | 75% |
| Amelanotic melanoma (classic) | 41% | -- |
Note on Terminology: The seven-point checklist described here is sometimes referred to as the Italian version (Argenziano et al., 1998). The term "Glasgow 7-point checklist" refers to a clinical (not dermoscopic) scoring system using different criteria (change in size, shape, color; inflammation; crusting/bleeding; sensory change; diameter >=7 mm). This module focuses on the dermoscopic seven-point checklist.
CASH Algorithm
Purpose: The CASH (Color, Architecture, Symmetry, Homogeneity) algorithm provides a semi-quantitative scoring system for the dermoscopic evaluation of pigmented lesions.
Criteria and Scoring:
| Criterion | Assessment | Score Range |
|---|---|---|
| Color | Presence of each: light brown, dark brown, brown, red, white, blue (1 point each) | 0 -- 6 |
| Architectural disorder | None/mild (0): colors and structures distributed in an organized or slightly disordered manner; Moderate (1): structures lose uniformity and are distributed irregularly; Marked (2): completely disorganized (chaotic) arrangement | 0 -- 2 |
| Symmetry | Taking into account shape AND dermoscopic structures: Bi-axial symmetry (0); Mono-axial symmetry (1); Bi-axial asymmetry (2) | 0 -- 2 |
| Homogeneity/Heterogeneity | Number of dermoscopic structures present (1 point each): network, dots/globules, streaks/pseudopods, blue-white veil, regression structures, blotches, polymorphous vessels | 0 -- 7 |
Total CASH score range: 2 -- 17
Threshold: A total score of 8 or more is considered suspicious for melanoma.
Important note: Like the ABCD rule, CASH evaluates both the contour (shape) and the content (structure distribution) for asymmetry assessment.
Performance:
| Metric | Range |
|---|---|
| Sensitivity | 87% -- 98% |
| Specificity | 67% -- 68% |
BRAAFF Rule
Purpose: Created by Lallas et al. (2015) specifically for the evaluation of volar (acral) skin lesions.
Structure: The algorithm uses both positive (associated with melanoma) and negative (associated with benign nevi) criteria, with each criterion having a different score weight based on the strength of its association.
Scoring:
| Type | Letter | Criterion | Score |
|---|---|---|---|
| Positive | B | Irregular blotch | +1 |
| Positive | R | Parallel ridge pattern | +3 |
| Positive | A | Asymmetry of structures | +1 |
| Positive | A | Asymmetry of colors | +1 |
| Negative | F | Parallel furrow pattern | -1 |
| Negative | F | Fibrillar pattern | -1 |
Interpretation: A total score of >= 1 is required for the diagnosis of acral melanoma (i.e., the lesion should be considered suspicious).
Note: The parallel ridge pattern carries the highest positive weight (+3), reflecting its strong association with acral melanoma. The negative criteria (parallel furrow pattern, fibrillar pattern) are characteristic benign acral patterns that reduce suspicion.
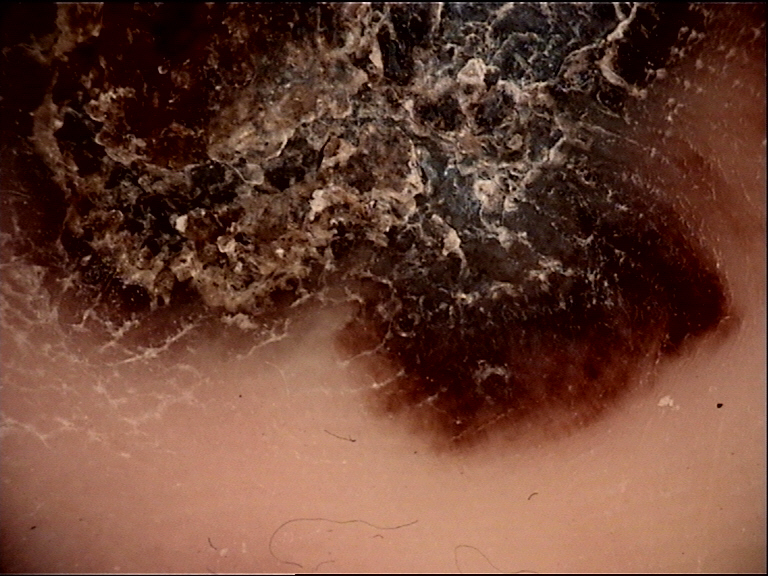
Clinical Scenario
A 65-year-old man presents for a routine skin check. You evaluate a 10 mm pigmented macule on the left forearm using the Three-Point Checklist. You note: (1) Asymmetry of structures -- the lesion has an irregular reticular pattern on one side and a structureless area on the other (1 point). (2) Blue-white structures -- a faint blue-whitish haze is present centrally (1 point). (3) Atypical network -- thick brown lines with variation in color and spacing are present in the reticular area (1 point). Total score: 3.
What is your diagnosis and key dermoscopic findings?
Melanoma (suspected -- Three-Point Checklist score 3, threshold is 2)
The Three-Point Checklist requires only a score of 2 or more to recommend biopsy or referral. This lesion scores 3/3, indicating high suspicion. The asymmetry of structures reflects a disorganized growth pattern. The blue-white structures suggest either melanin deep in the dermis with overlying orthokeratosis (blue-white veil) or regression. The atypical network indicates irregularly thickened rete ridges with disarranged melanocyte proliferation. This case also illustrates cross-algorithm concordance: applying TADA would flag the disorganized pattern (Step 2), and the ABCD rule would generate a high TDS from asymmetry, border, color, and dermoscopic structure scores.
Prediction without Pigment
This algorithm was created for the evaluation of amelanotic (non-pigmented) lesions and is discussed in detail in Module 05. It is referenced here for completeness as the counterpart to pigmented lesion algorithms.
Chaos and Clues
This algorithm is discussed in detail in Module 06. It was developed for the evaluation of pigmented skin lesions with a sensitivity of 90.6% (BCC 98.5%, SCC 86.5%, melanoma 79.3%) and a specificity of 62.7% for malignancy of any type.
Key Takeaways
- The 7-point checklist assigns weighted scores to major criteria (atypical network, blue-white veil, atypical vascular pattern) and minor criteria, with a threshold of 3 points.
- No single algorithm is definitively superior; choice depends on clinical setting, user experience, and whether sensitivity or specificity is prioritized.
- All algorithms share common features that predict malignancy: asymmetry, irregular vasculature, blue-white structures, and atypical pigment patterns.
Summary Table: Criteria Used Across Triage Algorithms
| Criterion | 3-Point | AC Rule | Blue-Black Rule | Chaos & Clues | Prediction w/o Pigment | TADA |
|---|---|---|---|---|---|---|
| Asymmetry | x | x | x | x | ||
| Color variation | x | x | x | x | x | |
| Atypical network | x | x | ||||
| Blue-white structures | x | x | x | |||
| Blue-black colors (>10%) | x | x | ||||
| Ulceration | x | x | ||||
| Shiny white structures | x | x | ||||
| Keratin clues | x | x | ||||
| Vascular pattern | x | x |
Key Takeaways
- Algorithm comparison shows that simpler algorithms (3-point, TADA) favor sensitivity while more detailed ones (ABCD, pattern analysis) can achieve higher specificity.
- In primary care or screening settings, high-sensitivity algorithms are preferred to minimize missed melanomas even at the cost of more referrals.
- Experienced dermoscopists may use pattern analysis as the primary method, reserving algorithmic checklists for equivocal cases or teaching.
5. Algorithm Comparison Table
Comprehensive Performance Comparison (Chapter 5b and Chapter 5c)
| Algorithm | Primary Purpose | Criteria Count | Scoring System | Threshold | Sensitivity (Pigmented Melanoma) | Sensitivity (Amelanotic Melanoma) | Specificity (Experts) | Specificity (Non-experts) | Diagnostic Accuracy |
|---|---|---|---|---|---|---|---|---|---|
| TADA | Triage (pigmented + non-pigmented) | 3 steps (2 patterns, 2 structures, 4 colors) | Stepwise decision tree | Any feature in Step 3 | 88.1% -- 94.8% | Included in design | 72.3% -- 87.8% | 72.3% -- 87.8% | -- |
| 3-Point Checklist | Triage (pigmented) | 3 criteria | Additive (1 pt each) | >= 2 points | 79% -- 91% | Not designed for | 71% -- 72% | 71% -- 72% | -- |
| AC Rule | Triage (pigmented, melanoma focus) | 2 criteria | Both must be present | Both present | 94% (laypersons) | Not designed for | 62% (laypersons) | 62% | -- |
| Blue-Black Rule | Triage (nodular melanoma) | 1 feature + optional structures | Present/absent (10% area) | Blue-black >= 10% | 78.2% -- 84.6% | Not designed for | 80.5% -- 97.6% | -- | -- |
| ABCD Rule | Differentiation (pigmented) | 4 criteria | Weighted semi-quantitative (TDS) | < 4.75 benign; 4.75--5.45 suspicious; > 5.45 malignant | 78% -- 98% | Not designed for | 45% -- 80% | 56% -- 78% | -- |
| Menzies Method | Differentiation (pigmented, invasive melanoma) | 11 criteria (2 negative, 9 positive) | Negative/positive logic | Both negatives absent + any positive present | 86% -- 95% | 54% | 71% -- 78% | 38% -- 76% | 83% |
| 7-Point Checklist (Classic) | Differentiation (pigmented) | 7 criteria (3 major, 4 minor) | Weighted additive (major=2, minor=1) | >= 3 points | 62% -- 95% | 41% | 71% -- 87% | 35% -- 97% | 16% -- 88% |
| 7-Point Checklist (Revised) | Differentiation (pigmented) | 7 criteria (equal weight) | Additive (1 pt each) | >= 1 point | 88% | -- | 75% | -- | -- |
| CASH | Differentiation (pigmented) | 4 criteria | Additive semi-quantitative | >= 8 points | 87% -- 98% | -- | 68% | 67% | -- |
| BRAAFF | Triage (volar/acral) | 6 criteria (4 positive, 2 negative) | Weighted additive (+3/+1/-1) | >= 1 point | Site-specific | -- | -- | -- | -- |
| Chaos & Clues | Triage (pigmented) | Chaos + 9 clues | Stepwise decision tree | Chaos + any clue | 90.6% overall (melanoma 79.3%) | Not designed for | 62.7% | -- | -- |
| Pattern Analysis | Differentiation (pigmented) | Global pattern assessment | Expert pattern recognition | Expert judgment | 82% -- 85% | -- | 79% -- 88% | 61% -- 79% | -- |
Key observation: Methods relying on pattern analysis demonstrate superior specificity and are preferred by experienced clinicians. Semi-quantitative scoring algorithms are more useful for non-experts and standardized screening programs.
6. Clinical Pearls
TADA is uniquely versatile: Unlike most algorithms that address only pigmented lesions, TADA can evaluate both pigmented and non-pigmented lesions on non-glabrous skin. This makes it particularly useful in general screening settings.
Start with Step 1 confidence: Before investing time in algorithmic analysis, become expert at recognizing unequivocal seborrheic keratoses, angiomas, and dermatofibromas. Examining thousands of these common benign lesions deliberately with a dermatoscope builds rapid pattern recognition.
Asymmetry is the common thread: Every major triage algorithm includes asymmetry as a criterion. When in doubt about a lesion, asymmetry in the distribution of colors and structures is the single most reliable indicator of concern.
The blue-black rule fills a gap: Nodular melanoma can be symmetric, making it invisible to algorithms that rely heavily on asymmetry. The blue-black rule specifically targets this diagnostic pitfall. Remember the 10% surface area threshold.
Know your thresholds: ABCD TDS < 4.75 (benign), 4.75--5.45 (suspicious), > 5.45 (malignant). Seven-point classic >= 3. Seven-point revised >= 1. CASH >= 8. BRAAFF >= 1.
The Menzies method has a unique logic structure: It is the only algorithm that uses exclusionary negative features. If both symmetry of pattern AND only one color are present, melanoma is excluded -- a powerful ruling-out tool for experienced practitioners.
BRAAFF is the only algorithm specifically designed for acral skin: Do not use general algorithms (TADA, three-point checklist, etc.) on volar surfaces without also considering acral-specific patterns. The parallel ridge pattern carries the highest weight (+3) for good reason.
No algorithm captures newly described structures: Shiny white lines, negative network, and angulated lines were described after most algorithms were published. Clinicians should not ignore these features regardless of which algorithm they use.
Context matters beyond the score: Age, skin type, location, history of change, and whether the lesion is an outlier (ugly duckling sign) should all be considered alongside any algorithm result. The revised seven-point checklist explicitly incorporates this principle.
Pigmented SCC is the blind spot: The three-point checklist, AC rule, and blue-black rule were not designed to detect pigmented SCC. Any pigmented lesion with focal adherent keratin or rough texture showing an asymmetric dermoscopic pattern should be flagged as suspicious regardless of algorithm output.
Clinical Scenario
A 42-year-old man presents with an 8 mm pigmented papule on his left shoulder. The lesion is not an unequivocal SK, angioma, or dermatofibroma. On polarized dermoscopy, the pattern appears disorganized with asymmetric distribution of colors and structures, including irregular brown globules on one side and a structureless blue-gray area on the other. Using the TADA algorithm, what is your assessment?
What is your diagnosis?
Suspicious lesion -- biopsy recommended (TADA Step 2 positive)
After excluding the three unequivocal benign entities in Step 1, TADA Step 2 assesses for an organized versus disorganized pattern. This lesion demonstrates a disorganized pattern (asymmetric distribution of colors and structures), which is sufficient to classify it as suspicious and recommend biopsy. There is no need to proceed to Step 3. Asymmetry in the distribution of dermoscopic colors and structures is the single most reproducible and powerful predictor of malignancy across all algorithms.
Clinical Scenario
A 58-year-old woman presents with a symmetric, darkly pigmented 6 mm dome-shaped nodule on the trunk. Dermoscopy reveals an organized pattern with homogeneous blue-black color covering approximately 50% of the surface. No comedo-like openings or lacunae are seen. You apply the three-point checklist: the lesion is symmetric (0 points), blue-white structures are present (1 point), and no atypical network is seen (0 points). The score is 1. Should you rely on this result?
What is your diagnosis?
Suspected nodular melanoma -- biopsy recommended despite three-point checklist score of 1
While the three-point checklist score of 1 falls below the biopsy threshold of 2, this demonstrates a limitation of algorithms that rely heavily on asymmetry. The blue-black rule should also be applied: blue and black color involving at least 10% of the lesion surface has a sensitivity of 78.2% for melanoma. This combination covers approximately 50% of the surface, far exceeding the 10% threshold. No comedo-like openings or lacunae exclude SK and angiokeratoma. The TADA algorithm would also flag this lesion at Step 3 (blue and black colors present). No single algorithm is perfect, and clinicians should apply multiple algorithms when the initial result is discordant with clinical concern.
Clinical Scenario
A 70-year-old man has a pigmented lesion on his sole. Dermoscopy shows a parallel ridge pattern, an irregular blotch, and asymmetry of both structures and colors. No parallel furrow pattern or fibrillar pattern is present. You calculate the BRAAFF score. What is your assessment?
What is your diagnosis?
Acral melanoma -- biopsy recommended (BRAAFF score = +6)
The BRAAFF score is calculated as: parallel ridge pattern (+3) + irregular blotch (+1) + asymmetry of structures (+1) + asymmetry of colors (+1) = +6. No negative criteria are present (no parallel furrow pattern, no fibrillar pattern). A score of 1 or greater is sufficient to warrant biopsy. The parallel ridge pattern carries the highest weight (+3) because it is strongly associated with acral melanoma, corresponding to malignant melanocytes in eccrine ducts. This is also the only site-specific clue in the Chaos and Clues algorithm (Clue 7), and Exception 4 applies. BRAAFF is the only algorithm specifically designed for volar skin evaluation.
8. Cross-References
| Topic | Chapter/Section | Pages |
|---|---|---|
| TADA algorithm | Chapter 5b | 81--85 |
| Three-point checklist, AC rule, Blue-black rule, Chaos & Clues | Chapter 5c | 86--89 |
| Chaos and Clues (full algorithm) | Chapter 5a | 70--80 |
| ABCD rule of dermoscopy (scoring details) | Chapter 9b | 220--223 |
| Menzies method (criteria and scoring) | Chapter 9b | 220--223 |
| Seven-point checklist (classic and revised) | Chapter 9b | 220--223 |
| CASH algorithm (scoring details) | Chapter 9b | 221--223 |
| BRAAFF algorithm (acral lesions) | Chapter 8d | 197--201 |
| Comparative diagnostic accuracy table | Chapter 9b | 223 |
| Prediction without Pigment | Chapter 4c | 72--80 |
| Pattern analysis revised | Chapter 4a | 53--60 |
| Digital monitoring | Chapter 13 | 320--335 |
9. Related Modules
| Module | Relationship |
|---|---|
| Module 01: Introduction and Principles | Prerequisite -- equipment, polarized vs. non-polarized light required for TADA Steps 2-3 |
| Module 02: Histopathologic Correlations | Prerequisite -- understanding structural terminology used across all algorithms |
| Module 03: Pattern Analysis Revised | Prerequisite -- foundational pattern elements used in all algorithmic assessment |
| Module 04: Top-Down 2-Step Algorithm | Related -- alternative organizational framework for lesion evaluation |
| Module 05: Prediction without Pigment | Complementary -- algorithm for non-pigmented lesions referenced in Chapter 5c |
| Module 06: Chaos and Clues | Prerequisite -- detailed understanding of chaos and the nine clues to malignancy |
| Module 22: Nodular Melanoma | Follow-up -- the blue-black rule and TADA address symmetric nodular melanoma |
| Module 24: Acrolentiginous Melanoma | Follow-up -- BRAAFF algorithm applies specifically to volar lesions |
| Module 27: Differentiation Patterns and Rules | Advanced -- detailed scoring systems (ABCD, Menzies, 7-point, CASH) for differentiation |
| Module 28: Sensitivity and Specificity | Advanced -- evidence-based comparison of all algorithms, ugly duckling sign, monitoring strategies |
| Module 29: Collision Tumors and Exceptions | Advanced -- diagnostic pitfalls and atypical presentations that challenge all algorithms |
Image Sources & Citations
- HIBA Dermoscopy Dataset: HIBA Dermoscopy Dataset. Hospital Italiano de Buenos Aires. License: CC-BY-4.0.
- DERM12345 (Skin Lesion Dataset with 40 Subclasses): DERM12345: A Large-scale Skin Lesion Image Dataset with 40 Subclasses. Figshare. 2023. License: CC-BY-4.0.