Module 22: Nodular Melanoma
Source: Dermoscopy Educational Course Authors: Natalia Jaimes and Scott W. Menzies (Chapter 8b); Cristian Navarrete-Dechent, Konstantinos Liopyris, Natalia Jaimes, and Ashfaq A. Marghoob (Chapter 8e)
1. Learning Objectives
After completing this module, the learner should be able to:
- Define nodular melanoma (NM) histopathologically as an invasive melanoma lacking a radial growth phase and explain why this distinction drives its unique dermoscopic morphology.
- List and identify the key dermoscopic features that positively correlate with pigmented NM, including blue-white veil, homogeneous blue pigmentation, blue-black structures, atypical vessels, and shiny white structures.
- Describe the dermoscopic approach to amelanotic and hypomelanotic NM, recognizing polymorphous vascular patterns and shiny white structures as the primary diagnostic clues.
- Apply the "blue-black rule" (blue and black pigmented areas involving at least 10% of the lesion surface) and state its reported sensitivity and specificity for melanoma.
- Apply the "EFG rule" (Elevated, Firm, Growing for more than one month) to clinically suspect NM when classic ABCD features are absent.
- Explain why NM is the most commonly missed melanoma subtype and identify the clinical and dermoscopic factors contributing to delayed diagnosis.
- Differentiate NM from its key clinical mimics -- blue nevus, thrombosed hemangioma, pigmented basal cell carcinoma, Spitz nevus, and pyogenic granuloma -- using dermoscopic criteria.
- Recognize that the majority of thick melanomas (greater than 3 mm Breslow thickness) are NMs and understand the prognostic implications of this association.
2. Prerequisites
- Module 01: Introduction and Principles of Dermoscopy -- Equipment operation, polarized vs. nonpolarized dermoscopy, and image capture.
- Module 02: Histopathologic Correlations of Dermoscopic Structures -- Understanding of how melanin depth, collagen alteration, and neoangiogenesis produce dermoscopic features (colors, blue-whitish veil, shiny white structures, vascular patterns).
- Module 03: Pattern Analysis Revised -- Mastery of basic geometric elements, pattern assessment, chaos and clues framework, and the nine clues to malignancy.
- Module 21: Superficial Spreading Melanoma -- Familiarity with SSM dermoscopic criteria (atypical network, irregular dots/globules, regression, blue-whitish veil, irregular streaks) to understand how NM differs from SSM.
3. Key Concepts
NM as De Novo Vertical Growth
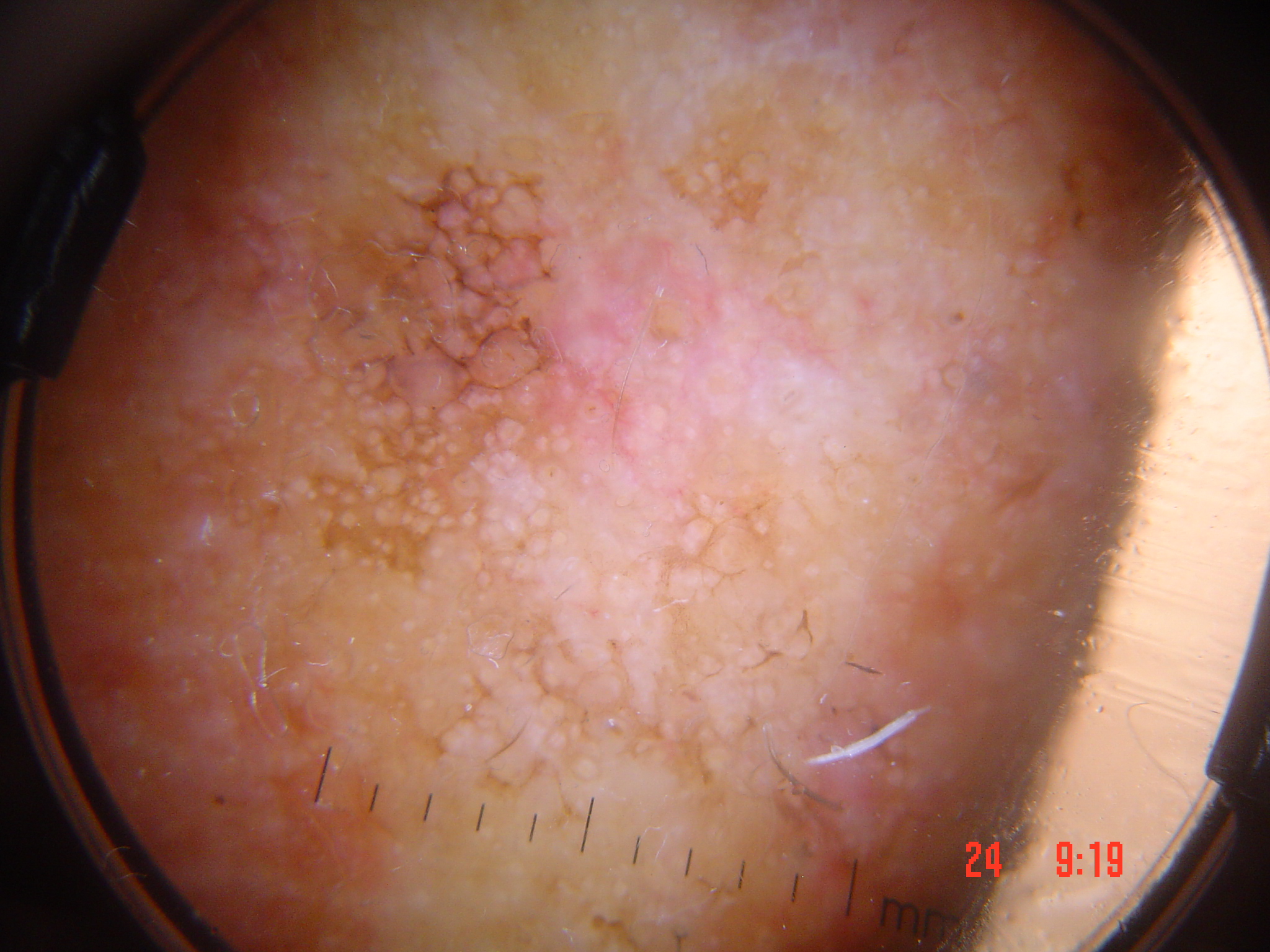
Nodular melanomas are defined as invasive melanomas without a radial growth phase. Specifically, they lack an in situ component beyond three rete ridges of the invasive vertical growth phase. Unlike SSM, which spreads laterally through the epidermis before invading vertically, NM grows directly downward into the dermis from the outset. This fundamental growth pattern explains:
- Why network, streaks, and regression structures are absent -- these features correlate with radial/pagetoid spread, which NM lacks.
- Why blue-white veil and deep pigmentation dominate -- vertical growth drives melanocytes deep into the dermis, producing blue and gray colors.
- Why shiny white structures (crystalline structures) are common -- vertical invasion causes collagen matrix alteration visible under polarized light.
- Why dermoscopic vessels are often obscured in pigmented NM -- abundant eumelanin in dermis and epidermis blocks visualization of neoangiogenic vessels.
Diagnostic Urgency
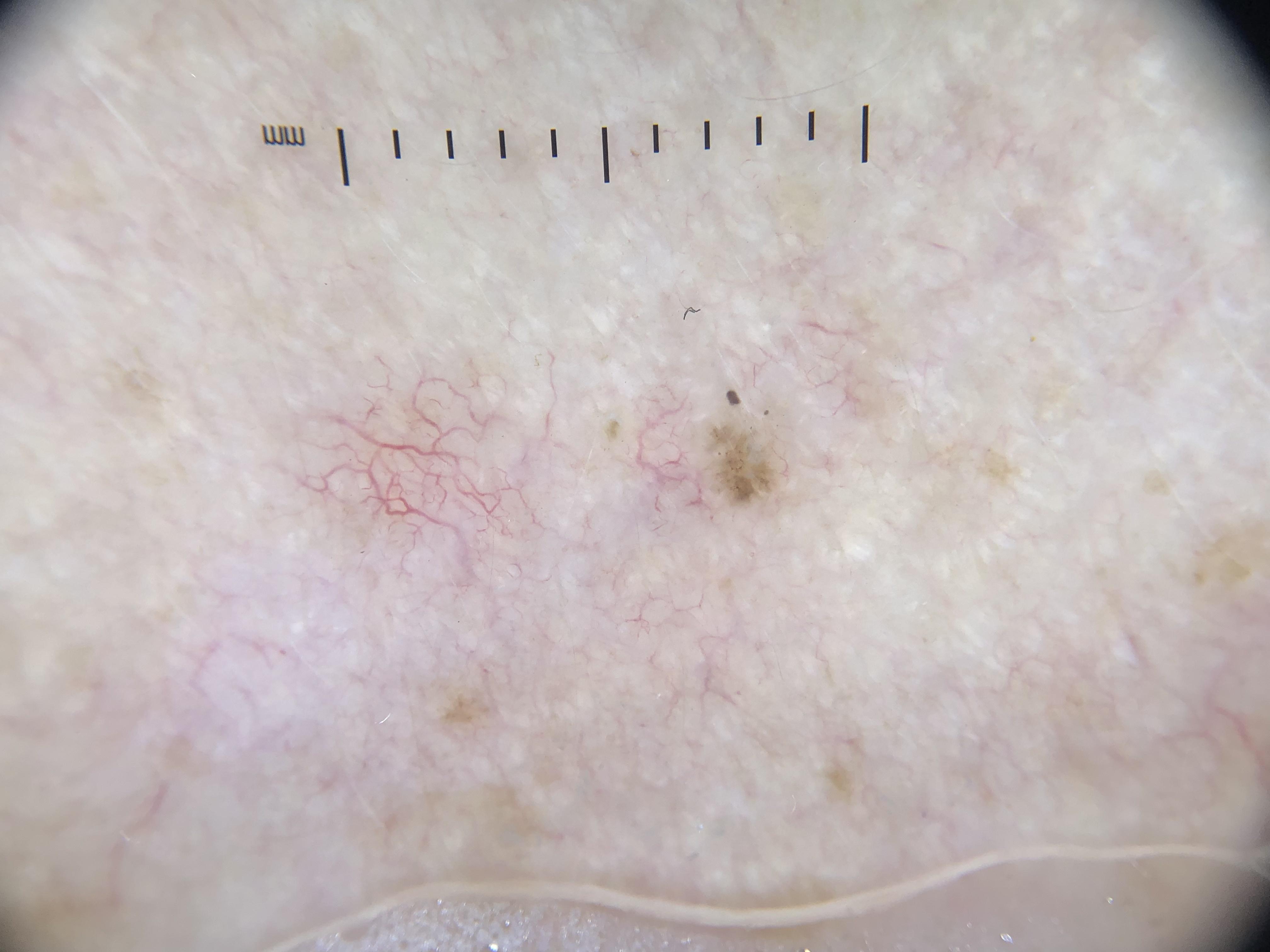
- NMs represent only 14% of invasive melanomas but are the predominant contributor to melanoma-related deaths.
- Thick melanomas (greater than 3 mm Breslow thickness) are predominantly NMs (56%).
- Between 30% and 40% of NMs are amelanotic or hypomelanotic, making them especially prone to diagnostic delay.
- A proportion of early NMs escape detection because they lack the classic ABCD clinical features of SSM.
- NM is widely regarded as the most commonly missed melanoma subtype.
4. Core Content
4.1 Epidemiology and Clinical Significance
NMs account for approximately 14% of invasive melanomas but carry the worst prognosis of any melanoma subtype due to their rapid vertical growth and the frequent delay in diagnosis. They are the largest contributor to melanoma-related deaths. Thick melanomas (greater than 3 mm Breslow thickness) are predominantly NMs (56%), underscoring the clinical urgency of early detection.
Clinically, NMs may lack the "ABCD" features more typical of SSMs. The classic dermoscopy features of SSMs (see Module 21) -- including features correlating with radial growth and pagetoid spread (streaks, pseudopods, radial streaming) and those features found in thin melanomas (atypical network, regression features including multiple blue-gray fine dots/peppering, and scarlike areas) -- are often lacking in NMs.
4.2 Dermoscopic Features of Pigmented NM
The histopathology and growth dynamics of pigmented NMs explain their dermoscopic morphology. NMs are characterized by prominent vertical growth with a relative lack of radial growth. Thus, dermoscopic features associated with radial growth (network structures, streaks) are not often seen. In contrast, dermoscopic features associated with vertical growth -- including matrix alterations (shiny white lines) and tumor cell aggregates (globules) -- are commonly present.
It is uncommon for NMs to spontaneously regress or involute; therefore, regression structures (scarlike depigmentation and granularity/peppering) are not a prominent feature. Although these tumors have neoangiogenic vessels in the dermis, the vessels are virtually invisible with dermoscopy due to the abundant eumelanin pigment present in the dermis and epidermis, which obscures the observer's ability to see the dermal vessels. The pigment is often so extensive that no dermoscopic structures can be appreciated, and the lesion simply appears as a blue-black nodule with an intermix of different hues of blue, red, and gray color.
NMs can display a clinically symmetric shape with an asymmetric pigmentation pattern under dermoscopy. However, the asymmetry of pattern may be less marked compared with SSM, and a small percentage of pigmented NMs (5.8%) can show symmetry of pigmentation pattern across all axes. Nevertheless, the majority of pigmented NMs can be diagnosed using standard dermoscopy criteria.
Dermoscopic structures that positively correlate with NM include:
Areas of homogeneous blue pigmentation -- Reflecting deep dermal melanin deposition from vertical growth. Unlike blue nevi, which display a relatively "homogeneous blue" hue, pigmented NMs typically show an intermix of different hues of blue, red, and gray.
Asymmetrical pigmentation pattern -- Though less marked than in SSM, present in the vast majority of pigmented NMs (approximately 94%).
Atypical peripheral black dots/globules with irregular size and distribution -- Representing tumor cell aggregates in the epidermis. Irregular brown dots/globules are predictive of NM less than 2 mm in thickness.
Blue-white veil -- The defining feature of the nodular component in many NMs. It reflects acanthosis with compact orthokeratosis overlying confluent nests of heavily pigmented melanocytes and melanophages in the dermis.
Pink, blue, or black color -- Multiple (five to six) colors are frequently present, scored from tan, dark brown, black, blue, gray, and red. The multicolored appearance reflects varied melanin depth and vascularity.
Atypical vascular structures -- Including polymorphous vessels, milky-red globules/areas, and homogeneous red areas. Vessel types include hairpin (looped) vessels, dotted vessels (indicative of melanocytic origin), and linear irregular vessels.
Blue-black structures -- Defined as the presence of a combination of blue and black pigmented areas involving at least 10% of the lesion surface. This is the basis of the "blue-black rule" (see Section 4.5).
Shiny white structures (shiny white streaks or lines) -- Visible only with polarized dermoscopy. These result from collagen matrix alteration caused by the invasive vertical growth component. Also known as crystalline structures.
Ulceration/erosion -- Indicating epidermal destruction overlying the vertically expanding tumor mass.
Check Your Understanding
Why is nodular melanoma particularly challenging to diagnose with dermoscopy?
Nodular melanoma often lacks the classic dermoscopic features of superficial spreading melanoma (atypical network, irregular streaks) because it grows vertically from the outset, bypassing the radial growth phase. It may appear as a symmetric, structureless nodule with blue-white veil or may be amelanotic, making recognition with pattern-analysis algorithms difficult.
Key Takeaways
- Nodular melanoma (NM) frequently presents with blue-black color corresponding to dense dermal melanin, and this blue-black homogeneous pattern may be the only dermoscopic clue.
- Atypical vessels in NM include irregular linear, dotted, and hairpin vessels, often in a polymorphous pattern reflecting the chaotic tumor vasculature.
- Ulceration in NM corresponds to epidermal disruption overlying the tumor and is associated with thicker, more aggressive tumors with worse prognosis.
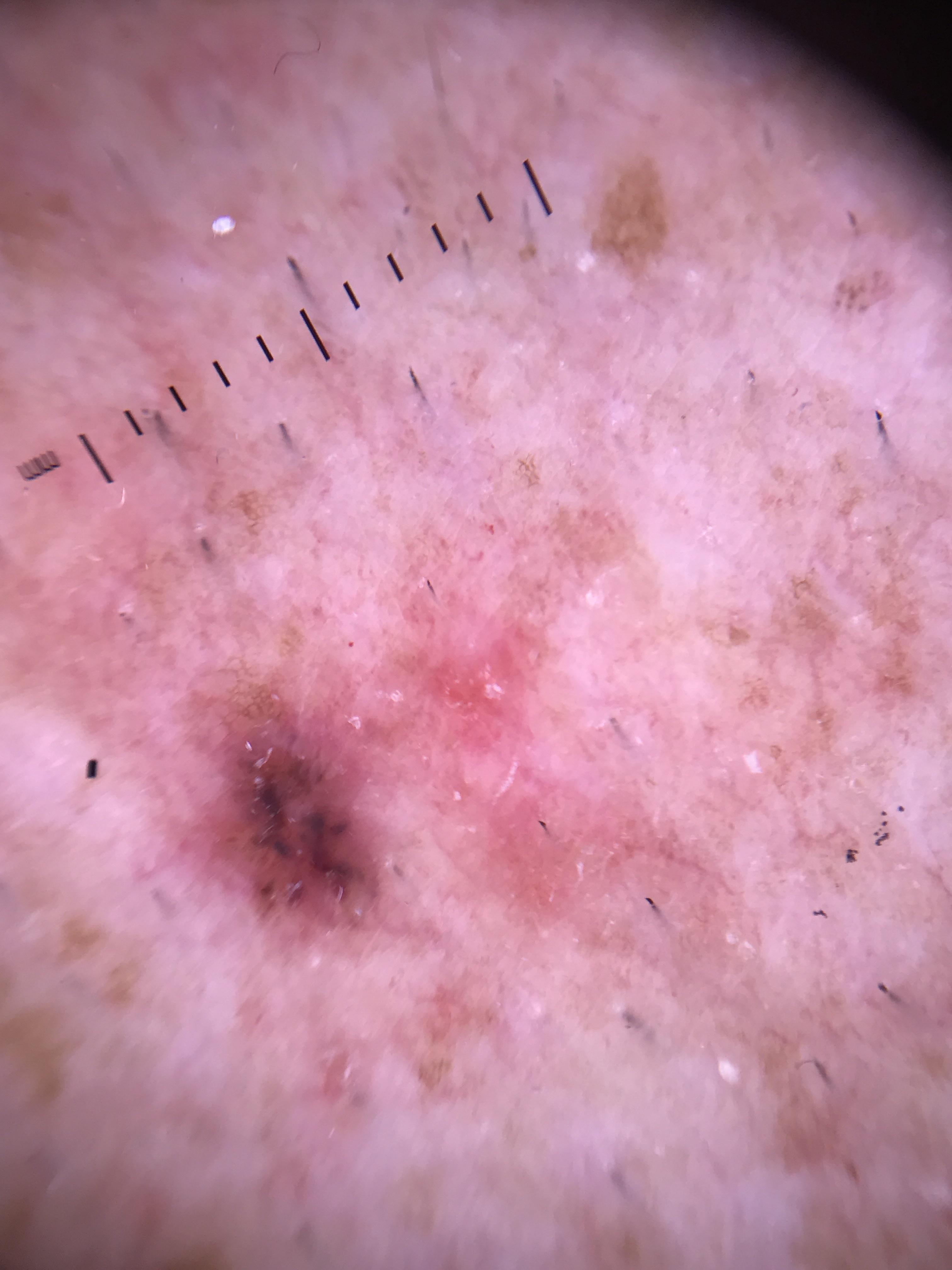
Clinical Scenario
A 62-year-old man presents with a rapidly growing 12 mm blue-black nodule on his left calf that appeared 3 months ago. Dermoscopy reveals homogeneous blue pigmentation with intermixed areas of black, gray, and red, a blue-white veil covering most of the lesion, and shiny white lines visible under polarized light. No network or streaks are visible.
What is the most likely diagnosis, and why are network and streaks absent?
Nodular Melanoma (NM)
The blue-black nodule with blue-white veil, shiny white lines, and absent network/streaks is classic for NM. Network and streaks are absent because NM grows vertically from the outset, lacking the radial growth phase that produces these features. The blue-white veil reflects acanthosis overlying deep dermal melanocytes, and shiny white lines indicate collagen matrix alteration from vertical invasion. The blue-black rule (blue and black areas involving >10% of the lesion) further supports melanoma. Urgent excision is required given the rapid growth (EFG rule: Elevated, Firm, Growing).
4.3 Amelanotic and Hypomelanotic NM
A diagnostically significant proportion of NMs are hypomelanotic or amelanotic compared with invasive non-NM (37.3% vs. 7.5%). This is the single most important factor contributing to diagnostic delay.
Nonpigmented NMs can be classified as:
- Pure amelanotic NM (ANM): No discernable eumelanin production.
- Hypomelanotic NM: Appears mainly amelanotic to the naked eye but reveals subtle melanin pigmentation under dermoscopy.
Since there is minimal to no eumelanin pigment to block dermoscopic light, amelanotic NMs almost always display:
- Polymorphous vascular pattern -- The polymorphous vessels usually consist of dotted and serpentine vessels. Rarely will there be vessels with a comma shape (as seen in intradermal nevi) or an arborizing configuration (as seen in BCC). The presence of serpentine vessels is highly predictive of thicker NMs (greater than 2 mm).
- Shiny white structures -- Visible under polarized light, representing dermal matrix alteration.
- Milky-red/pink areas -- An important feature reflecting neoangiogenesis and altered dermal stroma.
- Linear irregular vessels and hairpin vessels -- The most important single vascular structures in amelanotic/hypomelanotic NM.
In amelanotic NMs, atypical vascular structures may be the only clues for diagnosis and are indicative of angiogenesis. Thicker melanomas tend to show more peripheral vessels than thin melanomas.
Key distinguishing point: If blue-gray globules or vessels are visualized in a heavily pigmented nodule, it is more likely that the lesion will prove to be a pigmented nodular BCC than a NM. This is because in pigmented nodular BCC, the epidermis is not heavily melanized -- only the dermal BCC tumor islands are. Therefore, dermoscopic light can still reach the superficial dermis, allowing the observer to see vessels and blue-gray BCC tumor islands.
4.4 The Pattern of NM: Homogeneous Disorganized or Featureless
The dermoscopic pattern of NM is often characterized as:
- Homogeneous disorganized -- dermoscopically asymmetric despite sometimes appearing clinically symmetric.
- Featureless with atypical vessels -- structureless pink or blue-black background with scattered vascular structures.
This reflects the fundamental nature of NM: vertical growth without the structured patterns (network, streaks) that characterize radial growth melanomas.
Check Your Understanding
What are the dermoscopic clues that help identify nodular melanoma?
Key clues include blue-white veil over a raised portion, atypical vascular pattern (dotted and/or linear-irregular vessels), peripheral black dots or globules, milky-red or pink globules/areas, and ulceration. The combination of blue-white structures with polymorphous vessels in a nodular lesion should raise suspicion even without a pigment network.
4.5 The Blue-Black Rule
The "blue-black rule" is a simplified dermoscopic clue specifically developed for recognizing pigmented nodular melanoma.
Definition: The presence of a combination of blue and black pigmented areas involving at least 10% of the lesion surface.
Performance:
- Sensitivity for the diagnosis of melanoma: 78.2%
- Specificity for the diagnosis of melanoma: 80.5%
Application: When encountering a pigmented nodule with combined blue and black areas covering at least 10% of its surface, melanoma must be strongly considered and biopsy is generally indicated. This rule is particularly useful for less experienced dermoscopists as it provides a simple, binary criterion for raising suspicion.
Key Takeaways
- The EFG criteria (Elevated, Firm, Growing) were developed specifically for NM because nodular melanoma frequently lacks the ABCD clinical features used for flat melanomas.
- Amelanotic NM may show only milky-red or pink structureless areas with polymorphous vessels and is one of the most commonly missed melanoma subtypes.
- Symmetric pigmented nodules (blue-black) still require the blue-black rule: any nodule with blue and black color and no other definitive benign features should be excised.
Clinical Scenario
A 70-year-old woman presents with a 10 mm pink, dome-shaped, firm nodule on her right shin that has been growing for 6 weeks. Dermoscopy reveals a milky-red structureless background with polymorphous vessels (dotted, hairpin, and linear irregular) and shiny white lines under polarized light. There is no pigment visible.
What is the most likely diagnosis, and what clinical rule applies?
Amelanotic Nodular Melanoma
Approximately 37% of NMs are amelanotic or hypomelanotic. The polymorphous vascular pattern (multiple vessel types in one lesion) combined with shiny white lines is highly suspicious for amelanotic melanoma. The EFG rule applies: Elevated, Firm, and Growing for more than one month -- all three criteria are met. Amelanotic NM is the most commonly missed melanoma subtype because it lacks pigment-based dermoscopic criteria. Key mimics include pyogenic granuloma and BCC, but the polymorphous vessels with shiny white lines favor melanoma.
4.6 The EFG Rule: Detecting NM Without Classic ABCD Criteria
Because a proportion of early NMs escape detection due to their lack of classic ABCD features, the "EFG" criteria were proposed to supplement the ABCD rule:
- E -- Elevated: The lesion is raised above the skin surface.
- F -- Firm: The lesion feels firm to palpation (not soft or compressible).
- G -- Growing: The lesion has been continuously growing for more than one month.
Any elevated, firm, and continuously growing lesion that does not match the pattern recognition morphology of a common benign lesion warrants biopsy. This rule underscores the importance of growth as a key feature of NM, as evolution ("E" for evolution) was also added to the ABCD rule to improve early detection. Amelanotic NMs in particular present as pink, elevated, firm, fast-growing tumors that fit the EFG criteria.
4.7 Why NM Is the Most Commonly Missed Melanoma
Multiple factors contribute to NM being the melanoma subtype most prone to diagnostic delay:
- Absence of classic ABCD features: NMs may lack asymmetry, border irregularity, color variegation, and the larger diameter typical of SSM.
- High rate of amelanosis/hypomelanos: 30-40% of NMs are amelanotic or hypomelanotic, compared with only 7.5% of non-nodular invasive melanomas.
- Relatively symmetric shape: NMs can present as symmetric nodules, failing to trigger the "ugly duckling" alarm.
- Symmetric dermoscopic pigmentation: 5.8% of pigmented NMs show symmetry across all axes under dermoscopy.
- Lack of radial growth features: Network, streaks, and regression structures -- the features most clinicians look for -- are absent.
- Mimicry of benign lesions: Pigmented NM can mimic blue nevus; amelanotic NM can mimic pyogenic granuloma, dermal nevus, or cyst.
- Featureless morphology: Some NMs appear as feature-poor or structureless lesions under dermoscopy, making them difficult to categorize as concerning.
- Rapid growth: The very speed of NM progression means the window for early detection is inherently shorter than for SSM.
4.8 Differential Diagnosis of NM
Pigmented NM vs. Blue Nevus
The critical differential for a heavily pigmented blue-black nodule. Blue nevi display a relatively "homogeneous blue" hue, while pigmented NMs typically show an intermix of different hues (blue, red, gray) and are more likely to exhibit multicolored areas, blue-white veil, and atypical vessels when present.
Pigmented NM vs. Pigmented Basal Cell Carcinoma (BCC)
A hypomelanotic nodule with features resembling pigmented BCC (large blue-gray ovoid nests, ulceration) but lacking arborizing vessels typical of BCC -- and instead showing brown globules and dotted vessels (indicative of melanocytic origin) along with milky-red globules (specific for melanoma) -- should raise concern for NM. If blue-gray globules or vessels are visible in a heavily pigmented nodule, pigmented nodular BCC is more likely than NM, because the non-melanized epidermis in BCC allows dermoscopic light to reach dermal structures.
Amelanotic NM vs. Pyogenic Granuloma
Both present as rapidly growing pink-red vascular nodules. Amelanotic NM will show polymorphous vascular patterns with multiple vessel morphologies (dotted, serpentine, hairpin), shiny white structures under polarized light, and milky-red areas. Pyogenic granuloma typically shows a more homogeneous vascular pattern with red lacunae or a collarette of scale.
NM vs. Spitz Nevus
Both may present as pigmented or amelanotic papules/nodules. Spitz nevi typically show a symmetric starburst pattern with circumferential radial lines or pseudopods, a regular dotted vascular pattern, and organized globular patterns. NM shows asymmetric pattern, polymorphous vessels, and blue-white veil.
NM vs. Thrombosed Hemangioma/Angiokeratoma
Thrombosed hemangiomas display homogeneous dark-red to blue-black lacunae with clearly defined borders and septa. NM lacks lacunae and septae and instead shows multicolored areas, blue-white veil, and atypical vessels when present.
Key Takeaways
- NM must be differentiated from pigmented BCC (arborizing vessels present), blue nevus (stable and homogeneous), and thrombosed hemangioma (lacunae visible under dermoscopy).
- The combination of blue-white veil, irregular vessels, and any pigmented structureless areas in a nodule is highly specific for melanoma and should prompt immediate excision.
- Any rapidly growing nodule (weeks to months) should be biopsied regardless of dermoscopic findings, as NM can evolve faster than surveillance intervals.
5. NM Features Reference Table
| Feature | Pigmented NM | Amelanotic/Hypomelanotic NM | Clinical Significance |
|---|---|---|---|
| Blue-white veil | Frequently present; defining feature | Absent (insufficient pigment) | Reflects acanthotic epidermis over pigmented dermal melanocytes |
| Blue-black structures | Present (blue-black rule: at least 10% surface) | Absent | Sensitivity 78.2%, specificity 80.5% for melanoma |
| Homogeneous blue pigmentation | Present with intermixed hues of blue, red, gray | Absent | Distinguishes from blue nevus (uniform blue) |
| Multiple colors (5-6) | Frequently present (tan, dark brown, black, blue, gray, red) | Absent or minimal | Correlates with thick melanoma |
| Atypical vessels | Often obscured by dense pigment | Almost always present (polymorphous pattern) | Linear irregular and hairpin vessels are most important |
| Polymorphous vascular pattern | May be present peripherally | Present (dotted + serpentine) | Comma-shaped and arborizing morphologies argue against NM |
| Milky-red globules/areas | May be present | Important feature | Specific for melanoma; reflect neoangiogenesis |
| Shiny white structures | Present (polarized light only) | Present (polarized light only) | Matrix alteration from vertical invasion; also called crystalline structures |
| Dotted vessels | May be present | Commonly present | Indicative of melanocytic origin |
| Hairpin vessels | Present in some cases | Present in some cases | Correlate with thick melanoma |
| Ulceration/erosion | Frequently present | May be present | Indicates epidermal destruction by tumor mass |
| Atypical peripheral dots/globules | Present (irregular size and distribution) | Absent or rare | Irregular brown dots/globules predict NM less than 2 mm |
| Asymmetric pigmentation pattern | Present in approximately 94% | N/A (no significant pigment) | Less marked than in SSM |
| Network/streaks/regression | Absent | Absent | Features of radial growth phase, which NM lacks |
| Peripheral vessels | Less common | More common in thicker tumors | Thicker melanomas show more peripheral vessels |
| Serpentine vessels | May be obscured | Present | Highly predictive of NM thicker than 2 mm |
6. NM vs. Blue Nevus Differential Table
| Feature | Nodular Melanoma (Pigmented) | Blue Nevus |
|---|---|---|
| Color uniformity | Intermix of different hues (blue, red, gray, black) | Relatively homogeneous blue hue |
| Blue-white veil | Frequently present | Absent (structureless blue differs from blue-white veil) |
| Number of colors | Multiple (5-6 colors common) | Typically 1-2 colors (blue, blue-gray) |
| Pattern symmetry | Asymmetric in approximately 94% | Symmetric, uniform |
| Surface change | Ulceration common; surface disruption | Smooth, intact surface |
| Growth | Rapidly growing; elevated, firm | Stable; may be flat or slightly raised |
| Atypical vessels | Present (when visible through pigment) | Absent |
| Shiny white structures | Present under polarized light | Absent or inconspicuous |
| Blue-black rule | Positive (blue + black areas covering at least 10%) | Typically negative (lacks black component) |
| Dots/globules | Atypical, irregular distribution | Absent |
| Patient history | New or changing lesion; rapid evolution | Longstanding stable lesion |
| Borders | May be irregular or well-defined | Well-defined, regular |
| Clinical action | Biopsy mandatory | Observation acceptable if typical; biopsy if any atypical features |
7. Clinical Pearls
NM lacks the features you are trained to find. The dermoscopic hallmarks of SSM -- atypical network, irregular streaks, regression structures -- are characteristically absent in NM. Recognizing NM requires a different cognitive framework: look for what IS present (blue-white veil, blue-black color, shiny white structures, atypical vessels) rather than the usual melanoma checklist.
Apply the blue-black rule to every pigmented nodule. If combined blue and black pigmented areas involve at least 10% of the lesion surface, melanoma must be suspected. This simple rule has a sensitivity of 78.2% and specificity of 80.5%, making it a high-yield screening criterion for less experienced dermoscopists.
Use the EFG rule for amelanotic nodules. Any elevated, firm, and continuously growing lesion that does not match a known benign pattern should be biopsied. This rule catches the 30-40% of NMs that are amelanotic or hypomelanotic and would otherwise be missed by pigment-based criteria.
Polymorphous vessels in a pink nodule = melanoma until proven otherwise. In amelanotic NM, atypical vascular structures may be the ONLY diagnostic clue. The combination of dotted and serpentine vessels in a polymorphous arrangement is strongly suggestive. Importantly, comma-shaped vessels (intradermal nevus) and arborizing vessels (BCC) are rarely seen in NM, helping narrow the differential.
Serpentine vessels predict thickness. The presence of serpentine vessels in a nodular melanocytic lesion is highly predictive of NM thicker than 2 mm Breslow thickness, while irregular brown dots/globules predict NM less than 2 mm -- a finding with staging and management implications.
Always use polarized dermoscopy for nodules. Shiny white structures (crystalline structures, shiny white streaks, and lines) are visible ONLY with polarized light. In both pigmented and amelanotic NM, they represent collagen matrix alteration from vertical invasion and are an important diagnostic clue that is invisible under nonpolarized dermoscopy.
Blue-gray globules or vessels visible in a heavily pigmented nodule favor BCC over NM. In pigmented nodular BCC, the epidermis is not heavily melanized, so dermoscopic light can penetrate to the superficial dermis, making vessels and blue-gray tumor islands visible. In pigmented NM, the dense eumelanin throughout the epidermis and dermis obscures these structures. Use this counterintuitive finding to help distinguish the two entities.
A brown globule and dotted vessels in a multicolored nodule indicate melanocytic origin. Even when other features suggest pigmented BCC (blue-gray ovoid nests, ulceration), the presence of brown globules and dotted vessels shifts the diagnosis toward melanocytic origin -- and when combined with milky-red globules, is specific for melanoma.
Featureless NMs demand a low biopsy threshold. Some NMs present with feature-poor or structureless dermoscopic morphology. When an isolated nonspecific nodule (structureless pink or blue-black) is encountered and cannot be confidently classified as benign, it should be biopsied rather than monitored. Palpable or raised lesions should never be subjected to watchful-waiting monitoring protocols.
NM can arise within a pre-existing nevus. NM may present as a small papule with atypical vessels over a pink background within an otherwise banal nevus. Any new papular or nodular component arising within a flat nevus warrants high suspicion.
Clinical Vignettes
Clinical Scenario A 60-year-old man presents with a rapidly growing, 10 mm dark blue-black dome-shaped nodule on the upper back that appeared 3 months ago. Dermoscopy reveals extensive blue-white veil covering more than half the lesion, combined areas of blue and black pigment occupying approximately 30% of the surface, and shiny white structures visible with polarized dermoscopy. No pigment network, regression structures, or irregular streaks are identified.
What is the most likely diagnosis?
Diagnosis: Pigmented nodular melanoma.
This case illustrates the critical teaching points about NM diagnosis. First, NM lacks the features you are trained to find (Clinical Pearl 1): the classic SSM features -- atypical network, irregular streaks, regression structures -- are characteristically absent. Instead, look for what IS present: blue-white veil, blue-black color, and shiny white structures. The blue-black rule applies (Clinical Pearl 2): combined blue and black areas involving at least 10% of the lesion surface mandate suspicion for melanoma (sensitivity 78.2%, specificity 80.5%). Shiny white structures visible only with polarized dermoscopy represent collagen matrix alteration from vertical invasion (Clinical Pearl 6). Always use polarized dermoscopy for nodules.
Clinical Scenario A 55-year-old woman presents with a 7 mm firm, pink, dome-shaped nodule on the right lower leg that has been growing steadily for 6 weeks. Dermoscopy reveals a pink structureless background with polymorphous vessels: dotted vessels centrally and serpentine vessels peripherally. No pigmentation, blue-white veil, or ulceration is present. The lesion is elevated, firm, and continuously growing.
What is the most likely diagnosis?
Diagnosis: Amelanotic nodular melanoma -- the EFG rule applies.
This case demonstrates the 30-40% of NMs that are amelanotic or hypomelanotic. The EFG rule (Clinical Pearl 3) is the key: any Elevated, Firm, and continuously Growing lesion that does not match a known benign pattern should be biopsied. The polymorphous vessels (dotted + serpentine) in a pink nodule equal melanoma until proven otherwise (Clinical Pearl 4). Importantly, comma-shaped vessels (intradermal nevus) and arborizing vessels (BCC) are rarely seen in NM, and their absence helps narrow the differential. The serpentine vessels predict Breslow thickness >2 mm (Clinical Pearl 5), carrying staging and management implications. Featureless NMs demand a low biopsy threshold -- never subject palpable or raised lesions to watchful waiting (Clinical Pearl 9).
Clinical Scenario A 50-year-old man presents for evaluation of a flat brown nevus on the left chest that he has had for many years. On examination, a 4 mm pink papule is noted arising within the flat nevus. He confirms the papule appeared recently (approximately 2 months ago). Dermoscopy of the flat surrounding nevus shows a regular reticular pattern. Dermoscopy of the new pink papule shows atypical dotted vessels on a pink background with milky-red globules. No pigment structures are visible within the papule itself.
What is the most likely diagnosis?
Diagnosis: Nodular melanoma arising within a pre-existing nevus.
This case illustrates Clinical Pearl 10: NM may present as a small papule with atypical vessels over a pink background within an otherwise banal nevus. The flat surrounding component shows a regular reticular pattern consistent with a benign junctional nevus. However, the new papular component with atypical dotted vessels and milky-red globules is alarming. The milky-red globules combined with brown globules and dotted vessels are specific for melanoma (Clinical Pearl 8). Any new papular or nodular component arising within a flat nevus warrants high suspicion and immediate excisional biopsy. The deceptively benign appearance of the surrounding nevus should not delay action on the newly elevated component.
9. Cross-References
| Topic | Reference |
|---|---|
| Nodular melanoma full chapter | Chapter 8b, pp. 187-189 |
| NM definition and epidemiology | Chapter 8b, p. 187 |
| Dermoscopic features of pigmented NM | Chapter 8b, pp. 187-188 |
| Amelanotic/hypomelanotic NM features | Chapter 8b, p. 188 |
| Key points for NM | Chapter 8b, p. 189 |
| NM figure: blue-white veil, multiple colors, ulceration, hairpin vessel | Chapter 8b |
| NM figure: extensive blue-white veil, dotted vessels | Chapter 8b |
| NM figure: asymmetric pattern, blue-white veil | Chapter 8b |
| Hypomelanotic NM: brown globules, dotted vessels, blue-white veil | Chapter 8b |
| Hypomelanotic NM: milky-red globule, dotted vessels, BCC-like features | Chapter 8b |
| Amelanotic NM: dotted vessels, ulceration | Chapter 8b |
| NM arising on a nevus: atypical vessels on pink background | Chapter 8b |
| Amelanotic NM: hairpin vessels, shiny white structures (polarized) | Chapter 8b |
| Blue-black rule reference | Argenziano G, et al. Br J Dermatol. 2011;165(6):1251-5 |
| Difficult to diagnose melanomas: NM | Chapter 8e, pp. 202-203 |
| EFG rule for nodular melanoma | Chapter 8e, p. 202 |
| Pigmented NM figures: homogeneous blue, blue-white veil, irregular globules | |
| Table of dermoscopic findings in NM | Chapter 8e |
| Vascular structures in melanocytic tumors | Chapter 8f |
| Amelanotic melanoma chapter | Chapter 8f, pp. 210-214 |
| Superficial spreading melanoma for comparison | Chapter 8a |
10. Related Modules
| Module | Title | Relationship |
|---|---|---|
| Module 18 | Blue Nevi and Variants | Critical differential for pigmented NM; distinguishing homogeneous blue (blue nevus) from multicolored blue-black intermix (NM) |
| Module 21 | Superficial Spreading Melanoma | Understanding the radial growth features (atypical network, streaks, regression) that are characteristically ABSENT in NM |
| Module 26 | Amelanotic and Hypomelanotic Melanoma | Comprehensive coverage of vascular patterns and shiny white structures in amelanotic tumors, including the 30-40% of NMs that are amelanotic |
| Module 09 | Basal Cell Carcinoma | Differential diagnosis of pigmented nodular BCC vs. pigmented NM (arborizing vessels, blue-gray ovoid nests, visible vessels in heavily pigmented nodules) |
| Module 19 | Spitz and Reed Nevi | Differential diagnosis of Spitz nevus (symmetric starburst, organized globular pattern) vs. NM (asymmetric, polymorphous vessels, blue-white veil) |
| Module 13 | Vascular Lesions | Differential diagnosis of thrombosed hemangioma (lacunae with septa) and pyogenic granuloma vs. amelanotic NM |
| Module 25 | Other Melanoma Subtypes | Additional difficult-to-diagnose melanomas including desmoplastic, nevoid, and spitzoid subtypes |
| Module 07 | TADA and Other Triage Algorithms | Blue-black rule, EFG rule, and other triage algorithms applicable to NM detection |
Module 22 -- Version 1.0 Part of the Dermoscopy Educational Course.
Image Sources & Citations
- DERM12345 (Skin Lesion Dataset with 40 Subclasses): DERM12345: A Large-scale Skin Lesion Image Dataset with 40 Subclasses. Figshare. 2023. License: CC-BY-4.0.
- HIBA Dermoscopy Dataset: HIBA Dermoscopy Dataset. Hospital Italiano de Buenos Aires. License: CC-BY-4.0.