Module 25: Other Melanoma Subtypes
1. Learning Objectives
After completing this module, the learner should be able to:
- Recognize the concept of "difficult to diagnose" melanomas and explain why melanomas that lack classical ABCD criteria, mimic benign lesions, or present as featureless/structureless tumors pose a diagnostic challenge.
- Describe the dermoscopic features of desmoplastic melanoma, including the distinction between pure desmoplastic melanoma and mixed desmoplastic melanoma associated with lentigo maligna, and the paucity of melanocytic-specific structures.
- Identify the three dermoscopic patterns of nevoid melanoma (nevus-like, amelanotic, and multicomponent) and explain the clinical clues that help distinguish nevoid melanoma from a benign intradermal or compound nevus.
- Compare and contrast the dermoscopic features of spitzoid melanoma with those of benign Spitz and Reed nevi, identifying the two described dermoscopic patterns (amelanotic/Spitz nevus-like and pigmented/Reed nevus-like) and the clinical scenarios warranting biopsy.
- Explain the dermoscopic pitfalls associated with verrucous (seborrheic keratosis-like) melanoma, including anchoring bias, search satisfaction error, the blue-black sign, and methods to differentiate blue-white veil in melanoma from that in seborrheic keratoses.
- Describe the dermoscopic features of rare melanoma subtypes, including balloon cell melanoma, polypoid melanoma, primary dermal melanoma, follicular melanoma, pigmented epithelioid melanocytoma (animal-type melanoma), and nested melanoma of the elderly.
- Classify the five dermoscopic patterns of cutaneous melanoma metastases (blue nevus-like, nevus-like, angioma-like, vascular, and nonspecific) and explain how clinical context aids their recognition.
- Define featureless/structureless melanoma and articulate the management approach (biopsy or short-term digital monitoring) for isolated structureless lesions lacking specific dermoscopic criteria.
2. Prerequisites
- Module 01: Introduction and Principles of Dermoscopy -- understanding of dermoscopic equipment, polarized vs. nonpolarized modalities, and foundational terminology.
- Module 02: Dermoscopic Structures and Colors -- recognition of global patterns, local features (network, globules, dots, streaks, blotch, blue-white veil, regression structures, shiny white structures, vessels).
- Module 03: Pattern Analysis -- systematic approach to dermoscopic evaluation, two-step algorithm, and melanoma-specific structures.
- Module 21: Superficial Spreading Melanoma -- baseline knowledge of SSM-specific dermoscopic features (atypical network, streaks, pseudopods, blue-white veil, negative network, regression, multiple colors).
- Module 22: Nodular Melanoma -- understanding of pigmented NM (blue-black color, shiny white structures) and amelanotic/hypomelanotic NM (polymorphous vessels, shiny white structures).
- Module 23: Lentigo Maligna/Lentigo Maligna Melanoma -- features of melanoma on chronically sun-damaged skin and the significance of associated desmoplastic components.
- Module 24: Acral Lentiginous Melanoma -- dermoscopic approach to acral melanoma and the parallel ridge pattern.
3. Key Concepts
3.1 Difficult to Diagnose Melanomas -- Overview
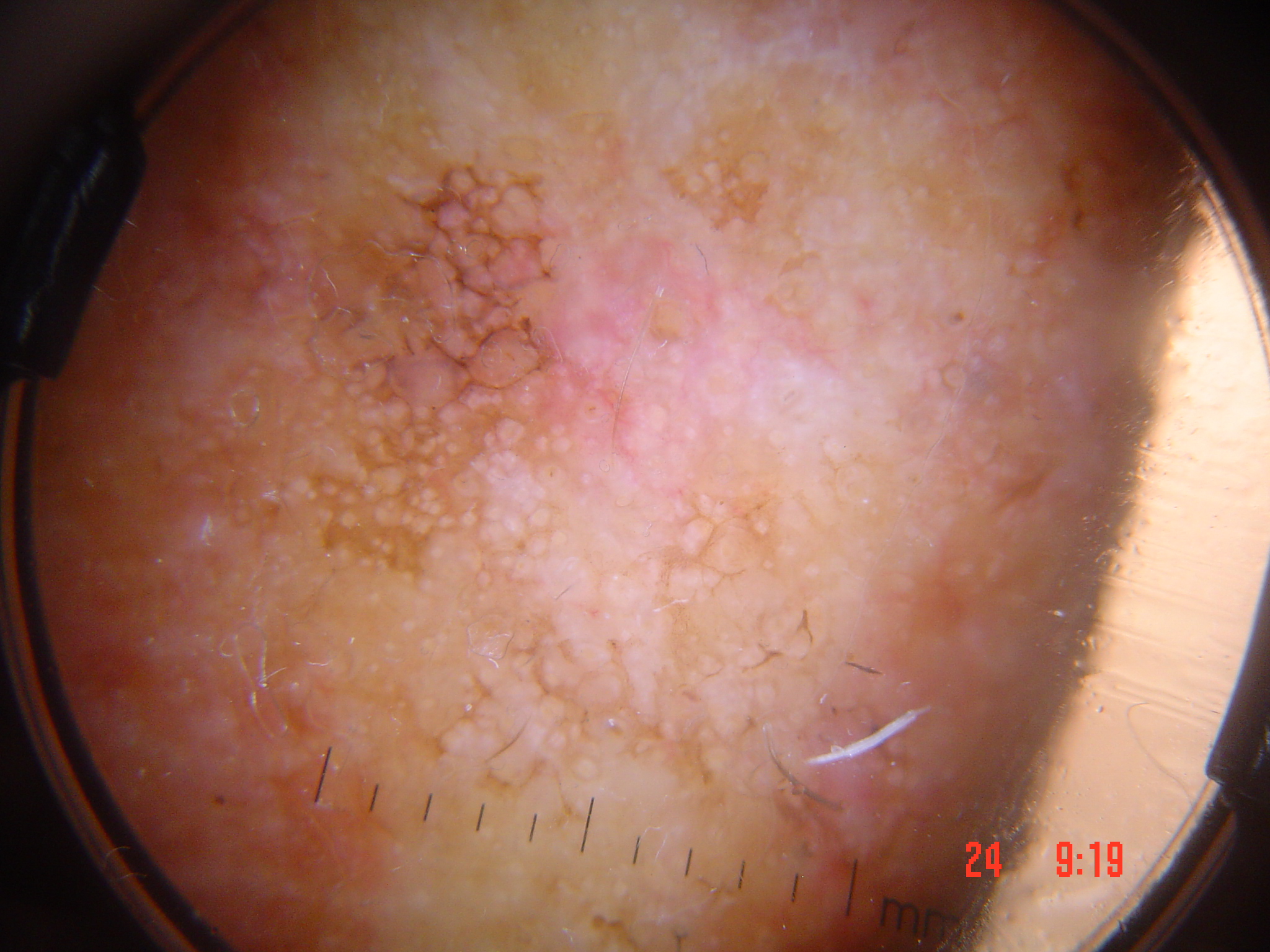
This category encompasses melanomas that escape detection because they:
- Lack the classical clinical ABCD features (Asymmetry, Border irregularity, Color variegation, Diameter >6 mm)
- Display an organized dermoscopic pattern mimicking a benign lesion
- Lack recognizable melanoma-specific dermoscopic structures (so-called "feature-poor," "featureless," or "structureless" melanomas)
These melanomas are at highest risk for being miscategorized as nonconcerning lesions.
3.2 Diagnostic Anchoring and Cognitive Bias
A recurrent theme across rare melanoma subtypes is the role of cognitive biases:
- Anchoring bias: Fixing on the first diagnostic impression (e.g., "this looks like a seborrheic keratosis") and interpreting subsequent features to confirm that impression.
- Search satisfaction error: Stopping the examination once features supporting the initial impression are found, without thoroughly evaluating the entire lesion.
3.3 The Blue-Black Sign
The presence of blue and black areas together within a pigmented lesion is an important clue to melanoma, particularly in verrucous melanomas that clinically resemble seborrheic keratoses.
3.4 Shiny White Structures as a Universal Clue
Shiny white structures (shiny white lines, blotches, and strands -- visible only under polarized dermoscopy) are a recurring finding across multiple rare melanoma subtypes (nodular, desmoplastic, nevoid, spitzoid, flat amelanotic). They correlate with altered stromal matrix and are suggestive of dermal invasion.
3.5 Polymorphous Vessels
The combination of two or more vessel morphologies (most commonly dotted and serpentine vessels) within a single lesion is highly suggestive of melanoma. This pattern is seen in amelanotic nodular melanoma, desmoplastic melanoma, and cutaneous melanoma metastases.
3.6 The Wobble Sign and Ink Test
- Wobble sign: Placing a dermatoscope on a lesion in contact mode and applying horizontal back-and-forth pressure. Seborrheic keratoses slide en bloc, whereas melanomas do not (they "wobble"). Also used to expose the undersurface of polypoid lesions.
- Ink test: Painting the lesion with gentian violet surgical marker ink and wiping with alcohol. Ink is retained in sulci, crypts, and comedo-like openings (seborrheic keratosis) but is completely removed from areas overlying a negative network (melanoma).
3.7 Key Terminology
| Term | Definition |
|---|---|
| Desmoplastic melanoma (DM) | Melanoma characterized by invasive spindle-shaped melanoma cells within a prominent fibrotic stroma |
| Nevoid melanoma | Melanoma with melanocytes displaying a nevoid (benign-appearing) morphology on histopathology |
| Spitzoid melanoma | Histopathologically malignant tumor containing large epithelioid melanocytes resembling Spitz nevi |
| Verrucous melanoma (VM) | Melanoma clinically and dermoscopically resembling pigmented verrucous nevi or seborrheic keratoses |
| Polypoid melanoma | Rare melanoma with prominent vertical growth phase and polypoid or cauliflower-like shape |
| Balloon cell melanoma | Melanoma defined by large polygonal foamy cells with abundant cytoplasm on histopathology |
| Follicular melanoma | Primary melanoma originating from the hair follicle without associated lentigo maligna |
| PEM | Pigmented epithelioid melanocytoma (animal-type melanoma) -- dermal proliferation of heavily pigmented melanocytes |
| Nested melanoma | Histopathologic variant of SSM with large intraepidermal nests, typically in elderly patients |
| Epidermotropic metastasis | Cutaneous metastasis of melanoma to the skin, the most common site of melanoma metastasis |
| Featureless/structureless melanoma | Melanoma presenting with pigment but without definable dermoscopic structures |
| Blue-black sign | Simultaneous presence of blue and black areas in a lesion, strongly suggestive of melanoma |
| BWV (Blue-white veil) | Blue-white hue over a raised portion of a lesion, corresponding to dermal melanocytes and compact orthokeratosis |
4. Core Content
4.1 Introduction: The Challenge of Rare Melanoma Subtypes
Melanomas that manifest the classical clinical ABCDs or display a disorganized dermoscopic pattern are relatively straightforward to recognize. The diagnostic challenge lies with melanomas that lack these features -- those with an organized dermoscopic pattern, those that mimic benign entities such as seborrheic keratoses, and those that are feature-poor or structureless. Studying the dermoscopic morphology of these "difficult to diagnose melanomas" has revealed clues that can assist in their identification.
This chapter covers the clinical and dermoscopic features of multiple challenging melanoma subtypes and highlights the clues to correctly identifying them.
4.2 Desmoplastic Melanoma
4.2.1 Clinical Overview
Desmoplastic melanoma (DM) is characterized by the association of invasive spindle-shaped melanoma cells within a prominent fibrotic stroma. DM comprises fewer than 4% of all cutaneous melanomas, with most cases presenting in patients older than 60 years on chronically sun-exposed skin.
DM can present as:
- An isolated sub-epidermal neoplasm (pure DM)
- In association with a non-DM melanoma, most frequently lentigo maligna (mixed DM)
Since most DMs are amelanotic and often lack epidermal involvement, early diagnosis remains challenging.
Clinical clues to suspect DM:
- A firm, subcutaneous, new, or changing scar-like lesion
- Located on sun-damaged skin of an elderly individual
- May be mistaken for a scar, cyst, or lipoma
4.2.2 Dermoscopic Features
Pure desmoplastic melanoma (desmoplasia throughout >=90% of the tumor):
- The lesion may show no structures or features visible with dermoscopy when the DM is not associated with an overlying LM or SSM
- Occasionally, one may see:
- Shiny white structures
- Vessels (serpentine, polymorphous)
- Granularity (especially if DM involves the papillary dermis)
- Milky-red areas
- Regression structures
Mixed desmoplastic melanoma (cellular foci without prominent stromal fibrosis, 10-90%):
- Atypical network
- Homogeneous areas
- Hyperpigmented areas
- Any lentigo maligna-specific criteria (when associated with LM)
4.2.3 Key Diagnostic Strategy
DMs associated with LM may be easier to detect because the LM acts as a "beacon" for the detection of DM. The critical clinical step is to routinely palpate any suspect LM before performing a biopsy. If the suspect LM has a focal firm area, one should entertain the possibility of an associated DM and perform an adequately deep biopsy that includes the area of firmness.
Check Your Understanding
What are the dermoscopic features of desmoplastic melanoma?
Desmoplastic melanoma often presents as an amelanotic or hypomelanotic lesion with subtle dermoscopic findings. Features may include white scar-like areas (reflecting dermal fibrosis), crystalline structures visible only under polarized dermoscopy, and atypical vascular patterns. Its bland dermoscopic appearance frequently leads to delayed diagnosis.
Key Takeaways
- Desmoplastic melanoma often appears amelanotic with prominent stromal fibrosis, showing subtle features such as shiny white lines (polarized), scar-like white areas, and polymorphous vessels.
- Mucosal melanoma shows a multicomponent pattern of blue, gray, and white structureless areas with irregular dots and globules on a background lacking standard skin dermoscopic patterns.
- Nevoid melanoma mimics a benign nevus with cobblestone or globular patterns and may be detected only by identifying subtle asymmetry, focal blue-white veil, or vessel irregularity.
Clinical Scenario
A 64-year-old woman presents with a firm, 8 mm skin-colored nodule on her upper back. She reports it has been growing for 3 months. Dermoscopy reveals a paucity of melanocytic structures, with scar-like white areas, shiny white lines under polarized light, and polymorphous vessels (dotted and serpentine).
What is the most likely diagnosis, and why is this melanoma subtype easily missed?
Desmoplastic Melanoma
Desmoplastic melanoma lacks typical melanocytic-specific dermoscopic structures because the tumor consists of spindle-shaped melanoma cells within prominent fibrotic stroma. The shiny white lines reflect stromal fibrosis, and polymorphous vessels indicate neoangiogenesis. This subtype is frequently misdiagnosed as a scar, dermatofibroma, or BCC because it often appears amelanotic. Palpation is important -- firm, indurated lesions on sun-damaged skin should raise suspicion, even without pigmented features.
4.3 Nevoid Melanoma
4.3.1 Clinical Overview
Nevoid melanoma accounts for fewer than 1% of all melanomas and is associated with a high mortality rate (15--37.5%), attributed to delays in detection. The reported mean Breslow thickness at diagnosis is 2.9 mm (range 0.4--12.0 mm).
On histopathology, nevoid melanomas display malignant melanocytes with a nevoid (benign-appearing) appearance. Clinically, they may present as pigmented or nonpigmented tumors. Although some are indistinguishable from SSM (manifesting the ABCDs), others resemble an intradermal and/or compound melanocytic nevus, displaying a dome-shaped to sessile symmetric morphology and mammillated surface.
4.3.2 Dermoscopic Features
Nevoid melanomas will not display the benign patterns seen in intradermal nevi. Instead, they frequently reveal:
- Milia-like cysts
- Irregular or eccentric globules
- Blue-white veil
- Shiny white structures
- Irregular or eccentric hyperpigmented blotches
- Atypical vessels
4.3.3 Three Dermoscopic Patterns
- Nevus-like pattern (48% of cases):
- Dome-shaped to sessile mammillated/papillomatous lesions resembling dermal nevi
- Dermoscopy reveals: atypical vessels, irregular dots/globules, and/or shiny white structures
- Amelanotic pattern (30% of cases):
- Atypical vessels with or without shiny white structures
- Multicomponent pattern (15% of cases):
- At least one of the classic melanoma-specific structures associated with SSM (atypical network, streaks, pseudopods, blue-white veil, etc.)
- Allows an easier diagnosis
4.3.4 Key Diagnostic Strategy
Remain suspicious of any "banal" mammillated intradermal nevus-like appearing lesion that is:
- New or changing in an older individual
- Lacks a benign pattern under dermoscopy (i.e., does not match patterns of intradermal or congenital nevi)
- Reveals atypical vessels, shiny white structures, atypical dots/globules, or any melanoma-specific structures
4.4 Spitzoid Melanoma
4.4.1 Clinical Overview
The term spitzoid melanoma refers to histopathologically malignant tumors containing large epithelioid melanocytes resembling those seen in Spitz nevi. Clinically, spitzoid melanomas typically present as enlarging or changing amelanotic or pigmented palpable lesions (papule, nodule, or plaque). Spitzoid melanomas can have a symmetric appearance, lacking the ABCDs.
4.4.2 Dermoscopic Features
The following dermoscopic structures are seen in spitzoid melanomas:
- Atypical broadened network
- Negative network
- Reticular depigmentation
- Shiny white lines
- Homogeneous pinkish background
- Atypical vessels, including dotted and polymorphous vessels
4.4.3 Two Dermoscopic Patterns
- Amelanotic pattern (Spitz nevus-like):
- Dotted or polymorphous vessels
- Shiny white lines
- Negative network
- Reticular depigmentation
- Multicomponent pattern possible
- These lesions can be morphologically indistinguishable from benign Spitz nevi
- Pigmented pattern (Reed nevus-like):
- Starburst, globular, homogeneous, negative network, or reticular pattern
- These melanomas can be indistinguishable from Reed nevi
4.4.4 Key Diagnostic Strategy
Since the morphology of spitzoid melanoma can mimic Spitz and Reed nevi, one needs to rely on other clues to decide when a biopsy is warranted:
- Spitzoid lesions developing in older individuals should always raise suspicion for melanoma
- Lesions that are asymmetrically or rapidly growing should always raise suspicion for melanoma
Check Your Understanding
How does nevoid melanoma differ dermoscopically from a benign dermal nevus?
Nevoid melanoma closely mimics benign nevi and may show a relatively symmetric, globular or cobblestone pattern. Subtle clues include irregular peripheral globules of varying sizes, blue-white veil in focal areas, and irregular vascular blush. These differences may be extremely subtle, which is why nevoid melanoma is one of the most challenging subtypes to detect.
Clinical Scenario
A 71-year-old man presents with a 6 mm dome-shaped papule on his back that resembles a dermal nevus. Dermoscopy shows a cobblestone pattern with comma vessels, but close inspection reveals subtle focal asymmetry, a small area of blue-white veil at one edge, and irregular dark dots not present in his other nevi.
What is the most likely diagnosis, and why is this subtype dangerous?
Nevoid Melanoma
Nevoid melanoma mimics a benign intradermal or compound nevus with cobblestone or globular patterns. It accounts for <1% of melanomas but has a high mortality (15-37.5%) due to diagnostic delay, with a mean Breslow thickness of 2.9 mm at diagnosis. The clues in this case are subtle: focal asymmetry, a small area of blue-white veil, and irregular dots not consistent with benign globules. These would be missed without careful dermoscopic examination. The "ugly duckling" concept may help -- if this lesion differs from the patient's other dermal nevi, suspicion should be raised.
4.5 Verrucous Melanoma (Seborrheic Keratosis-Like Melanoma)
4.5.1 Clinical Overview
Verrucous melanoma (VM) accounts for fewer than 3% of all melanomas. Approximately 50% of VMs are misdiagnosed clinically as benign lesions. VMs can resemble seborrheic keratoses (SK), displaying sharply demarcated borders and a keratotic surface with or without invaginated crypts and comedo-like openings.
4.5.2 Cognitive Biases in Diagnosis
Because VMs clinically resemble SKs, the clinician may fall into the trap of:
- Search "satisfaction": Searching for dermoscopic features that support the clinical impression of SK, anchoring on those features
- Anchoring bias: Turning a blind eye to melanoma-suggestive features
- Misinterpretation of structures: Globules in a VM can be misinterpreted as comedo-like openings; a negative network can be misinterpreted as gyri and sulci
4.5.3 Dermoscopic Features
Key dermoscopic findings in verrucous melanoma include:
- Blue-black areas (the "blue-black sign") -- an important clue
- Atypical dots and globules
- Streaks
- Bluish-white veil
- Regression structures (granularity/peppering and scar-like depigmentation) -- present focally
- Comedo-like openings, gyri and sulci, and milia-like cysts -- features overlapping with SK
4.5.4 Differentiating VM from Seborrheic Keratosis
Three clues differentiate blue-white veil (BWV) in SK from BWV in melanoma:
SKs with BWV will not display any other melanoma-specific structures (streaks, atypical network, angulated lines, negative network, shiny white lines, atypical dots/globules). In melanoma, BWV may coexist with these structures or reveal shiny white lines within the BWV area.
SKs will almost always display multiple comedo-like openings and/or milia cysts within the BWV area, whereas in melanoma, the BWV will not reveal other structures or will reveal shiny white lines.
The wobble sign: SKs slide en bloc under horizontal pressure from a dermatoscope, whereas melanomas do not slide en bloc and instead "wobble."
4.5.5 Negative Network vs. Gyri and Sulci
These two structures can appear very similar on a two-dimensional dermoscopic image, but they differ in three-dimensional topography:
- Negative network: Associated with changes at the level of the rete ridges and dermis; the surface of the lesion is relatively smooth without clinically visible invaginations.
- Gyri and sulci: Due to raised epidermal ridges alternating with invaginations; visible on the surface, especially with side lighting.
- The ink test: Painting with gentian violet and wiping with alcohol -- ink is retained in sulci/crypts/comedo-like openings (SK) but is completely removed from areas overlying a negative network (melanoma).
4.5.6 Melanomas Arising in Association with SK (Collision Tumors)
Melanomas can be found in up to 3.7% of collision tumors. Diagnosing these melanomas is challenging due to the same anchoring bias described above.
Regarding peppering/granularity in SK-like lesions:
- A solar lentigo or SK can involute and reveal regression structures (granularity/peppering), as seen in lichen planus-like keratosis (LPLK)
- Distinguishing involuting lentigo/SK from melanoma:
- Direction of involution: Lentigo/SK involution occurs centripetally (from the outer edge to center). Peppering expanding centrifugally should raise concern for melanoma.
- Remnant SK features: A partially involuted lentigo/SK will show remnants of classic lentigo/SK features at the edge opposite the area of peppering.
- Granularity quality: Involuting lentigo/SK tends to show "coarser" clumped granules; in melanoma, the granularity tends to be "fine" with tiny granular specks.
Key Takeaways
- Spitzoid melanoma shows features overlapping with Spitz nevus (starburst, globular) but displays asymmetry, irregular streaks, blue-white veil, or atypical vessels that favor malignancy.
- Balloon cell melanoma may appear as a light-colored lesion with white globules corresponding to balloon cells and should be considered when a light melanocytic lesion shows subtle asymmetry.
- Metastatic melanoma to the skin shows blue-gray nodules or structureless areas, often lacking epidermal changes; dermoscopy may reveal a pattern similar to blue nevus.
4.6 Flat Amelanotic Melanoma
Although nodular amelanotic melanoma and amelanotic DM are covered in their respective sections, flat (superficial spreading) amelanotic melanoma has distinct characteristics.
Early amelanotic melanomas lack the ABCD features and tend to display a symmetric shape both clinically and dermoscopically ("pink patch"). This symmetry is due to the inability to visualize the irregular horizontal borders of the melanoma because of the absence of melanin pigment.
Dermoscopic findings:
- Pink hue
- Dotted to serpentine to polymorphous vessels
- With or without shiny white structures
Although lacking pigment, amelanotic melanomas induce neoangiogenesis and matrix remodeling, making vessel and stromal changes the primary diagnostic clues.
4.7 Other Rare Melanoma Subtypes
4.7.1 Primary Dermal Melanoma
Primary dermal melanomas account for fewer than 1% of all melanomas. They usually present as solitary, smooth-surfaced nodular lesions in elderly patients. The primary focus of the melanoma is confined to the dermis; the epidermis and superficial papillary dermis are usually not involved.
Dermoscopic features:
- Often no specific or discernible dermoscopic finding (because the epidermis is not involved)
- Some may reveal atypical vessels and shiny white structures
- May present as bluish nodules on dermoscopy (similar to NM or epidermotropic metastatic melanoma)
4.7.2 Polypoid Melanoma
Polypoid melanoma is a rare tumor characterized by a prominent vertical growth phase. Clinically, polypoid melanomas display a polypoid or "cauliflower-like" shape.
Dermoscopic features:
- Poorly characterized, but can reveal structures similar to those seen in nevoid melanomas
- Ulceration frequently impedes visualization of underlying structures
- Key examination technique: Inspect the surface of the lesion near the base, which is often hidden by the overhanging polypoid/sessile portion
- Use the wobble test to expose the undersurface of pedunculated lesions by placing the dermatoscope on the lesion and applying horizontal back-and-forth pressure, causing the lesion to roll
4.7.3 Follicular Melanoma
Follicular melanoma is an extremely rare variant of primary melanoma that can mimic a comedo or pigmented cyst. It should be distinguished from lentigo maligna with secondary follicular invasion. In follicular melanoma, the melanoma originates from the hair follicle without an associated LM; in the latter, a LM invades the follicle.
Dermoscopic features (from limited case reports):
- Irregular or eccentric globules
- Homogeneous blue-gray or pinkish-red areas
- Shiny white structures
- Central ulcerations
- Atypical vessels
- Frequently seen on the nose
4.7.4 Balloon Cell Melanoma
This rare variant is diagnosed histopathologically by the presence of large, polygonal foamy cells with abundant cytoplasm, in addition to classic melanoma features (nuclear pleomorphism, atypia, mitoses, lack of maturation with descent into the dermis).
Dermoscopic features:
- Clinically, balloon cell melanomas fulfill the ABCDs criteria and are relatively easy to detect as probable melanomas
- On dermoscopy: disorganized pattern displaying any of the conventional melanoma-specific structures
- No specific dermoscopic structures have been identified to predict this subtype
- Key distinguishing observation: While white globules are a hallmark of balloon cell nevi, they are not seen in balloon cell melanomas
4.7.5 Pigmented Epithelioid Melanocytoma (PEM / "Animal-Type Melanoma")
PEM encompasses different atypical melanocytic lesions, including animal-type melanoma. PEM frequently involves lymph nodes but tends to have an indolent clinical course. Histopathologically, PEM corresponds to a dermal proliferation of heavily pigmented dendritic and epithelioid melanocytes, admixed with slightly larger and less pigmented epithelioid cells.
Dermoscopic features (from a study of nine PEMs):
- All lesions presented with homogeneous blue pigmentation
- Some cases had blue-black color and shiny white structures
- A characteristic feature was the presence of blue pigmentation in lymphatic vessels
4.7.6 Nested Melanoma (Nested Melanoma of the Elderly)
Nested melanoma is a histopathologic variant of melanoma characterized by the presence of a nested pattern with nests scattered along the dermo-epidermal junction. Usually presents in adults older than 60 years as relatively large outlier lentiginous macules on chronically sun-damaged skin on the lower extremities and trunk.
Dermoscopic features:
- Disorganized pattern with atypical dots/globules
- Homogeneous or structureless areas (brown or red)
- Wide skin markings
- Irregular or eccentric blotches (black or brown)
4.8 Epidermotropic (Skin) Metastasis
Cutaneous melanoma can metastasize to any organ, but metastasis to the skin remains the most common. Epidermotropic metastasis can clinically resemble blue nevi, dermal nevi, and angiomas.
4.8.1 Five Dermoscopic Patterns of Melanoma Metastasis
- Blue nevus-like pattern:
- Homogeneous and diffuse blue color with or without different hues of blue, black, and/or gray
- Can be indistinguishable from blue nevus or exogenous pigmentation (tattoo)
- Clinical context (history of prior invasive melanoma) is essential for detection
- Nevus-like pattern:
- Brown, black, or bluish aggregated globules
- Some lesions can also reveal reddish globules or atypical vessels
- Angioma-like pattern:
- Homogeneous milky-red area or milky-red globules
- Milky-red globules can resemble the lacunae seen in angiomas
- Differs from angiomas: Lacunae-like structures in epidermotropic metastasis are not separated from each other by septae, or are irregularly separated by ill-defined septae
- Atypical vessels can often be seen inside the lacunae-like structures
- Pink homogeneous papules or pyogenic granuloma-like metastasis also fall under this subtype
- Vascular pattern:
- Atypical vessels as the predominant structure
- Vessel morphology can vary: dotted, serpentine, corkscrew, or polymorphous
- Nonspecific pattern:
- Does not manifest any of the above patterns
- Recognized by the presence of pigment and a disorganized dermoscopic morphology
Key Takeaways
- Melanoma in children is rare but not negligible; atypical spitzoid lesions in children require careful evaluation as they may represent spitzoid melanoma.
- Melanoma in dark skin types often presents on acral or mucosal sites and may show unique features including broad irregular bands (nails), diffuse pigmentation (soles), and blue-gray mucosal patterns.
- Regression as the predominant feature (extensive white scar-like and blue-gray areas) can indicate a regressed melanoma where the primary tumor is no longer identifiable but the diagnosis remains important for staging.
4.9 Featureless/Structureless Melanoma
Melanomas presenting with pigment but without definable structures are classified as featureless or structureless melanomas. Due to the feature-poor morphology, they tend to be easily overlooked.
Management approach:
- Whenever an isolated nonspecific lesion (e.g., structureless pink or brown lesion) is encountered, melanoma should always enter the differential diagnosis
- These lesions should either undergo biopsy for definitive diagnosis or be subjected to sequential monitoring via the short-term monitoring protocol
- Critical rule: Digital dermoscopic monitoring is reserved only for flat, nonpalpable lesions; palpable or raised lesions should not be subjected to monitoring, as they may represent melanomas in their vertical growth phase
4.10 Conclusion and Overarching Detection Strategy
Difficult to diagnose melanomas refer to those melanomas that are challenging to detect without dermoscopy due to the lack of clinical ABCD criteria. Overall, these melanomas tend to display a disorganized pattern under dermoscopy. If they appear organized, they can still be detected based on correctly identifying any of the following:
- Starburst or negative network pattern
- Vessels or ulceration
- Any of the following colors: blue-black, gray, or white (including shiny white structures seen under polarized light)
Those that are truly featureless remain the most difficult to detect, and besides monitoring nonpalpable lesions with digital dermoscopy for change, there is no reliable way to diagnose them by dermoscopy alone.
Key Takeaways
- Rare melanoma subtypes often lack the classic ABCD features and dermoscopic patterns taught for SSM, making pattern recognition insufficient as the sole diagnostic tool.
- The presence of any dermoscopic feature that cannot be explained by a benign diagnosis should lower the threshold for biopsy, especially in lesions with a discordant clinical-dermoscopic picture.
- Clinicopathologic correlation is essential for rare melanoma subtypes because dermoscopy alone cannot reliably distinguish them from their benign mimics.
5. Rare Melanoma Subtypes Reference Table
| Subtype | Key Dermoscopic Features | Common Mimics |
|---|---|---|
| Desmoplastic melanoma (pure) | Shiny white structures; milky-red areas; regression structures; atypical vessels (serpentine, polymorphous); often featureless | Scar, cyst, lipoma, dermal tumor |
| Desmoplastic melanoma (mixed) | Atypical network; homogeneous/hyperpigmented areas; any LM-specific criteria | Lentigo maligna, solar lentigo |
| Nevoid melanoma (nevus-like) | Atypical vessels; irregular dots/globules; shiny white structures; milia-like cysts | Intradermal nevus, compound nevus |
| Nevoid melanoma (amelanotic) | Atypical vessels with or without shiny white structures | Dermal nevus, amelanotic BCC |
| Nevoid melanoma (multicomponent) | Classic melanoma-specific structures (network, streaks, blue-white veil) | SSM |
| Spitzoid melanoma (amelanotic) | Dotted/polymorphous vessels; shiny white lines; negative network; reticular depigmentation | Spitz nevus |
| Spitzoid melanoma (pigmented) | Starburst, globular, homogeneous, negative network, or reticular pattern | Reed nevus |
| Verrucous melanoma | Blue-black areas; atypical dots/globules; streaks; bluish-white veil; comedo-like openings; gyri and sulci; milia-like cysts | Seborrheic keratosis, pigmented verrucous nevus |
| Flat amelanotic melanoma | Pink hue; dotted to serpentine to polymorphous vessels; shiny white structures | Inflammatory dermatoses, Bowen disease |
| Primary dermal melanoma | Often featureless; atypical vessels; shiny white structures; bluish nodule | Blue nevus, epidermotropic metastasis, cyst |
| Polypoid melanoma | Similar to nevoid melanoma; ulceration common; polypoid/cauliflower shape | Pyogenic granuloma, polypoid nevus |
| Follicular melanoma | Irregular/eccentric globules; homogeneous blue-gray or pinkish-red areas; shiny white structures; central ulcerations; atypical vessels | Pigmented cyst, comedo, LM with follicular invasion |
| Balloon cell melanoma | Disorganized pattern; conventional melanoma-specific structures; absence of white globules | Balloon cell nevus (has white globules) |
| PEM (animal-type melanoma) | Homogeneous blue pigmentation; blue-black color; shiny white structures; blue pigmentation in lymphatic vessels | Blue nevus, cellular blue nevus |
| Nested melanoma | Disorganized pattern; atypical dots/globules; homogeneous/structureless areas; wide skin markings; irregular/eccentric blotches | Large lentigo, solar lentigo, LM |
| Epidermotropic metastasis (blue nevus-like) | Homogeneous diffuse blue, with or without blue/black/gray hues | Blue nevus, tattoo |
| Epidermotropic metastasis (nevus-like) | Brown/black/bluish aggregated globules; reddish globules; atypical vessels | Dermal nevus |
| Epidermotropic metastasis (angioma-like) | Milky-red area/globules; lacunae-like structures without clear septae; atypical vessels within lacunae | Angioma, pyogenic granuloma |
| Epidermotropic metastasis (vascular) | Atypical vessels (dotted, serpentine, corkscrew, polymorphous) as predominant structure | Angioma, amelanotic melanoma |
| Epidermotropic metastasis (nonspecific) | Pigment with disorganized morphology, no specific pattern | Various pigmented lesions |
| Featureless/structureless melanoma | Pigment present but no definable structures; structureless pink or brown areas | Dermatosis, lentigo, pink patch |
6. Clinical Pearls
Always palpate suspect lentigo maligna before biopsy. A focal firm area within a suspect LM should raise concern for an associated desmoplastic melanoma component. Ensure the biopsy is deep enough to include the area of firmness.
Any new or changing dome-shaped lesion in an older individual that lacks a benign dermoscopic pattern should be biopsied. Nevoid melanomas have a 2.9 mm mean Breslow thickness at diagnosis because they mimic banal intradermal nevi.
Age matters for spitzoid lesions. The morphologic overlap between spitzoid melanoma and Spitz/Reed nevi is substantial. A spitzoid lesion developing in an older individual or one that is asymmetrically or rapidly growing should always raise suspicion for melanoma.
Before diagnosing a seborrheic keratosis, actively search for melanoma-specific structures. Approximately 50% of verrucous melanomas are misdiagnosed as benign. Do not deploy destructive techniques (e.g., cryosurgery) without thorough dermoscopic examination and exclusion of melanoma features.
The blue-black sign is a critical red flag. In any lesion clinically resembling a seborrheic keratosis, the simultaneous presence of blue and black areas should prompt biopsy.
Use the wobble sign and ink test when diagnostic uncertainty exists. The wobble sign differentiates SK (slides en bloc) from melanoma (wobbles). The ink test differentiates gyri and sulci (retains ink) from negative network (ink wiped clean).
White globules are present in balloon cell nevi but absent in balloon cell melanoma. This is a helpful distinguishing feature in the differential diagnosis of balloon cell lesions.
For polypoid lesions, always examine the base. The diagnostic surface may be hidden under the overhanging portion of the lesion. Use the wobble test to roll the lesion and expose hidden areas.
Clinical context is paramount for cutaneous melanoma metastases. A blue nodule, nevus-like lesion, or angioma-like lesion in a patient with a history of invasive melanoma should be evaluated with a high index of suspicion.
Featureless melanomas are the most difficult to diagnose. For flat, nonpalpable structureless lesions, short-term digital dermoscopic monitoring is acceptable. For palpable or raised lesions that are structureless, biopsy is mandatory -- do not monitor these, as they may be in the vertical growth phase.
Polymorphous vessels are a hallmark of melanoma. The combination of dotted and serpentine vessels (or any two or more vessel morphologies) within a single lesion is a strong indicator of melanoma across multiple subtypes.
Corkscrew vessels are strongly associated with cutaneous melanoma metastases and should prompt urgent evaluation, especially in patients with known melanoma history.
Clinical Vignettes
Clinical Scenario A 75-year-old man presents with a firm, scar-like, skin-colored plaque (15 mm) on the right temple that has been slowly enlarging for 18 months. He had a lentigo maligna excised from the same area 6 years ago. Dermoscopy reveals shiny white structures visible under polarized light, milky-red areas, and serpentine vessels. No pigmented structures are visible. Palpation reveals a firm, indurated area.
What is the most likely diagnosis?
Diagnosis: Desmoplastic melanoma.
Desmoplastic melanoma characteristically presents as a firm, scar-like lesion that lacks melanocytic-specific structures on dermoscopy. The diagnostic triad is shiny white structures (reflecting dense stromal fibrosis), milky-red areas, and serpentine vessels. The history of prior LM at the same site is highly relevant: approximately 83% of desmoplastic melanomas are associated with overlying or adjacent lentigo maligna. This case underscores Clinical Pearl 10 from Module 25: featureless melanomas are the most difficult to diagnose. For flat, nonpalpable structureless lesions, monitoring is acceptable; but for palpable or raised lesions that are structureless, biopsy is mandatory.
Clinical Scenario A 62-year-old woman presents with a dome-shaped, symmetric, brown papule (7 mm) on the left forearm that has been present for years but recently began growing. Dermoscopy shows a homogeneous brown pattern with regular cobblestone-like globules, closely resembling an intradermal nevus. However, on careful inspection, subtle milky-red areas are visible at the periphery and irregular brown dots are present in one quadrant.
What is the most likely diagnosis?
Diagnosis: Nevoid melanoma -- melanoma masquerading as a benign nevus.
Nevoid melanoma is among the most diagnostically challenging melanoma subtypes because it dermoscopically mimics dermal nevi. The cobblestone-like globules and homogeneous brown pattern create a false sense of security. However, the subtle milky-red areas at the periphery and irregular dots in one quadrant are melanoma-specific features that should not be overlooked. Polymorphous vessels are a hallmark of melanoma (Clinical Pearl 11), and even subtle vascular changes in a "benign-appearing" lesion demand attention. The history of recent growth in a previously stable lesion is an important clinical clue. This case highlights why complete dermoscopic examination -- including the lesion base and periphery (Clinical Pearl 8) -- is essential for all raised lesions.
Clinical Scenario A 48-year-old man with a history of thick melanoma (Breslow 3.2 mm) excised from the left upper back 2 years ago presents with two new small (4 mm) blue-purple nodules on the left trunk, approximately 8 cm from the excision scar. The nodules appeared over the past 3 months. Dermoscopy of one nodule reveals a blue-black structureless pattern with scattered corkscrew vessels at the periphery. The other nodule shows a pink background with milky-red areas and irregular linear vessels.
What is the most likely diagnosis?
Diagnosis: Cutaneous melanoma metastases (in-transit metastases).
This case illustrates Clinical Pearl 9: clinical context is paramount for cutaneous melanoma metastases. Blue nodules or angioma-like lesions in a patient with a history of thick invasive melanoma should be evaluated with high suspicion. Corkscrew vessels are strongly associated with cutaneous melanoma metastases (Clinical Pearl 12) and should prompt urgent evaluation. The two nodules show different dermoscopic patterns (pigmented and amelanotic), which is consistent with the variable presentation of metastatic deposits. In-transit metastases occur in the lymphatic drainage pathway between the primary tumor site and the regional lymph node basin. Urgent biopsy and staging workup are mandatory.
8. Cross-References
| Topic | Chapter Reference |
|---|---|
| Superficial spreading melanoma (SSM) features | Chapter 8a |
| Nodular melanoma (NM) details | Chapter 8b |
| Amelanotic/hypomelanotic melanoma | Chapter 8f |
| Lentigo maligna / LM melanoma | Chapter 8c |
| Acral lentiginous melanoma | Chapter 8d |
| Intradermal nevus patterns | Chapter 7c |
| Congenital nevi patterns | Chapter 7a |
| Spitz nevus | Chapter 7d |
| Melanoma-specific structures (comprehensive) | Chapter 9a |
| Seborrheic keratosis features | Chapter 6a |
| Lichen planus-like keratosis (LPLK) | Chapter 6e |
| Short-term digital monitoring protocol | Chapter 13 |
| Dermoscopic findings in difficult to diagnose melanomas | Chapter 8e, p. 203 |
9. Related Modules
- Module 19: Spitz Nevus and Reed Nevus -- essential for understanding the morphologic overlap between benign spitzoid lesions and spitzoid melanoma, including the starburst pattern, negative network, and the clinical decision-making framework for biopsy of spitzoid lesions.
- Module 21: Superficial Spreading Melanoma -- baseline understanding of melanoma-specific structures (atypical network, blue-white veil, streaks, pseudopods, regression) that reappear in the multicomponent patterns of nevoid and verrucous melanomas.
- Module 22: Nodular Melanoma -- directly related content on pigmented NM (blue-black color, shiny white structures) and amelanotic NM (polymorphous vessels), which overlaps with desmoplastic melanoma and polypoid melanoma features.
- Module 23: Lentigo Maligna -- understanding of LM-specific dermoscopic criteria is essential for recognizing mixed desmoplastic melanomas, which often have an overlying LM component acting as a "beacon."
- Module 29: Collision Tumors -- covers the diagnostic challenges of melanomas arising within seborrheic keratoses and other benign neoplasms, directly relevant to verrucous melanoma and collision tumor scenarios discussed in this module.
- Module 05: Prediction Without Pigment -- provides the foundation for understanding vascular patterns (polymorphous, dotted, serpentine, corkscrew) and shiny white structures that are central to diagnosing amelanotic and desmoplastic melanoma subtypes.
Image Sources & Citations
- DERM12345 (Skin Lesion Dataset with 40 Subclasses): DERM12345: A Large-scale Skin Lesion Image Dataset with 40 Subclasses. Figshare. 2023. License: CC-BY-4.0.