Module 06: Chaos and Clues Triage Algorithm
A Decision Algorithm for Pigmented Lesions Based on Revised Pattern Analysis
Source: Dermoscopy Educational Course Authors: Cliff Rosendahl and Aksana Marozava
1. Learning Objectives
After completing this module, the learner should be able to:
- Define "chaos" in dermatoscopic terms as asymmetry of pattern, color, and/or border abruptness, and distinguish it from irregularity of lesion shape.
- Identify and apply the five red flags that warrant formal algorithmic assessment of a pigmented lesion (patient concern, clinical pattern-breaker, dermatoscopic chaos, dermatoscopic clues to change, and dermatoscopic uniqueness).
- Execute the Chaos and Clues decision algorithm in a stepwise fashion, from initial red flag identification through to biopsy/monitoring decision.
- Recognize and describe each of the nine clues to malignancy (gray or blue structures, eccentric structureless area, thick reticular lines, peripheral black dots/clods, segmental radial lines/pseudopods, white lines, parallel ridge lines on acral skin, polymorphous vessels, and angulated lines) and their histopathologic correlations.
- Differentiate the clues that apply to melanoma specifically from those that apply to pigmented basal cell carcinoma (pBCC) and pigmented squamous cell carcinoma (pSCC) in situ.
- Apply the four exceptions to the chaos requirement (changing lesion in adults, nodular/small lesions with clues, head/neck lesions with gray or circles, acral lesions with parallel ridge pattern).
- Interpret the published sensitivity and specificity data for the Chaos and Clues algorithm and understand its intended role in routine practice.
- Integrate the concept of biological symmetry and pattern recognition of common benign lesions into an efficient workflow for high-volume clinical practice.
2. Prerequisites
- Module 01: Introduction and Principles of Dermoscopy -- understanding of polarized vs. nonpolarized dermoscopy and equipment.
- Module 02: Histopathologic Correlations of Dermoscopic Structures -- knowledge of how dermoscopic structures correlate with histologic features.
- Module 03: Pattern Analysis Revised -- familiarity with the basic elements (lines, dots, clods, circles, pseudopods, structureless areas), patterns, colors, and the foundational concepts of revised pattern analysis.
3. Key Concepts
3.1 Triage Philosophy
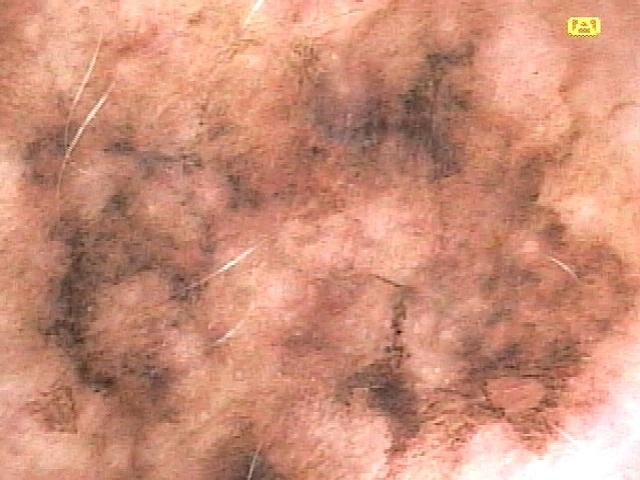
The Chaos and Clues algorithm is not a diagnostic method for identifying specific lesion types; it is a triage tool designed to guide the clinician to a single critical decision: Is excision biopsy indicated?
In the daily routine of clinical practice, a detailed algorithmic analysis of every lesion is neither realistic nor necessary. The vast majority of skin lesions are benign and can be diagnosed dermoscopically by pattern recognition. The five groups of common benign lesions encountered daily are:
- Nevus
- Benign keratinocytic lesions (seborrheic keratosis, solar lentigo)
- Hemangioma
- Dermatofibroma
- Sebaceous gland hyperplasia
Because these lesions are ubiquitous, the clinician can very rapidly become an expert at recognizing them by deliberately examining thousands of them with a dermatoscope to understand their characteristic protean variations.
Chaos and Clues is engaged only when a lesion is flagged as suspicious -- that is, when it cannot be immediately recognized as one of these common benign entities.
3.2 Chaos -- Definition
Chaos is defined as the presence of dermatoscopic asymmetry of any or all of:
- Pattern (asymmetric distribution of dermoscopic structures)
- Color (asymmetric distribution of colors)
- Border abruptness (asymmetric variation in how abruptly the lesion border is demarcated)
Key distinction: Irregularity of the shape (silhouette) of a lesion is NOT relevant. Chaos refers exclusively to the internal organization of structures, colors, and border characteristics.
3.3 Biological Symmetry
Benign lesions tend to have biological symmetry, which manifests as recognizable patterns -- analogous to how animal faces of different species have recognizable patterns. A dog's face is recognizable by pattern recognition even though there are many morphological varieties. Biological symmetry does not mean perfect mathematical symmetry; it means the pattern is recognizable and organized.
When a lesion lacks biological symmetry, it is chaotic and therefore unrecognizable as any specific benign entity. Pattern analysis must then be applied to weigh clues to determine what the lesion represents.
4. Core Content
4.1 Red Flags for Pigmented Lesions
Red flags are the features that flag a lesion as suspicious and therefore warrant formal algorithmic assessment. These features will either be known (patient concern), obvious (clinical pattern-breaker), or recognized during scanning dermatoscopic evaluation (chaos of pattern/color/border abruptness, dermatoscopic clues to change, dermatoscopic uniqueness).
Red Flag 1: Patient Concern or Clinical Evidence of Change
No lesion of patient concern should ever be dismissed without targeted examination including dermoscopy. Patients may be concerned because:
- A seborrheic keratosis is large and black
- A hemangioma has suddenly appeared
- A mole is perceived to have changed
Patient concern should automatically flag a lesion as suspicious and lead to an analytical assessment. Similarly, documented evidence of change at mature age -- including deliberately monitored change -- flags a lesion as suspicious and requiring focused dermatoscopic assessment.
Red Flag 2: Clinical Pattern-Breaker
The same disorganized and uncontrolled behavior of malignant tissue that causes dermatoscopic chaos often causes malignant lesions to clinically break the pattern of the surrounding skin. Malignant lesions may:
- Arise randomly
- Have an irregular, unexpected shape or color
- Eventually, through unrestrained growth, become larger than surrounding benign lesions
A lesion that breaks the pattern clinically should be flagged as suspicious and dermoscopically analyzed.
Red Flag 3: Dermatoscopic Chaos
Chaos of pattern, color, or border abruptness, as defined in Section 3.2 above. This is the central feature of the algorithm.
Red Flag 4: Dermatoscopic Clues to Change
Peripheral clods, radial lines, and pseudopods are all dermatoscopic clues to change. Key considerations by age:
- Circumferential peripheral clods may not cause concern in adolescence (consistent with a growing nevus)
- At mature age, any clues to change should flag a lesion as suspicious
- At intermediate age, assess in the context of other lesions on the patient
- Segmental radial lines or pseudopods should be recognized as a red flag at any age
Example: Two lesions with peripheral clods -- (a) a growing nevus on the back of an adolescent (not excised), and (b) a lesion on the back of a 60-year-old woman excised as nodular melanoma (3 mm diameter, Breslow thickness 0.9 mm). The melanoma, although arguably symmetrical, had disorganized structure consistent with malignant tissue.
Red Flag 5: Dermatoscopic Uniqueness (Ugly Duckling Sign)
Any lesion that has a dermatoscopic pattern different from all other lesions on the patient should be flagged as suspicious. This has been described as the dermatoscopic ugly duckling sign and is particularly relevant for a clod pattern nevus at mature age, which is usually not expected at that stage of life.
Example: Four lesions on the anterior thigh of a 50-year-old woman. Three were consistent with the patient's signature nevi (structureless, with reasonable biological symmetry). The fourth was also reasonably symmetrical but was the only clod pattern lesion, making it dermatoscopically unique -- excised as melanoma in situ.
4.2 What Chaos Really Means
There are two steps in the decision-making process:
- First step: Decide if a lesion is suspicious
- Second step: Decide if it is likely to be malignant
Dermatoscopic chaos is the most compelling factor in deciding whether a pigmented lesion is suspicious. While natural laws (gravity, electrical and magnetic fields, surface tension, feedback mechanisms) favor symmetry, malignant tissue defies natural laws -- this is the basis for both dermatopathological and dermatoscopic chaos. This chaotic behavior also produces all the other red flag characteristics and the clues to malignancy.
Practical tip: If a dermatoscopist is equivocating about the presence of chaos, the situation is usually resolved by considering whether the dermatoscopic pattern is consistent with the chaotic behavior of malignant tissue.
4.2.1 Chaos of Pattern
Requires the presence of more than one pattern (each covering at least approximately 20% of the lesion), with the patterns being asymmetrically combined.
Exception to the 20% rule: If any of the highly specific defined clues (peripheral black clods/dots, lines radial segmental/pseudopods) is asymmetrically present, even if the structure does not cover sufficient area to produce a pattern, it is considered chaotic.
4.2.2 Chaos of Color
Requires the presence of more than one color (light and dark brown are regarded as different colors if the transition between them is abrupt), with those colors being asymmetrically combined.
If the variation is obvious and abruptly demarcated, there is no lower limit of the area required to be covered by a color to create asymmetry.
4.2.3 Chaos of Border Abruptness
Defined as definite and asymmetric variability in the abruptness of demarcation of the border of a lesion.
This is distinct from the ABCD method's assessment of border abruptness. The ABCD method gives the highest score when the total border is abrupt (as in an ink-spot lentigo or solar lentigo). However, in the Chaos and Clues framework:
- Total border abruptness is a feature of benignancy (no asymmetry in border demarcation)
- Chaos of border abruptness (some portions abrupt, others gradual) is more likely in malignant lesions
Example: An invasive melanoma demonstrating chaos of pattern, color, and border abruptness -- with an abrupt border at the lower right extremity and a gradual border elsewhere.
Historical Note: Chaos of border abruptness was first recognized and described by Francis Drugge, the 12-year-old son of dermatologist Rhett Drugge (Stanford, Connecticut, USA).
Check Your Understanding
What does 'Chaos' mean in the Chaos and Clues algorithm, and how is it assessed?
Chaos refers to asymmetry of structure or pattern within a lesion. It is assessed by mentally dividing the lesion and comparing opposite halves. If the pattern in one half cannot be 'copied and pasted' to mirror the other half, the lesion exhibits chaos. Chaos alone is not sufficient for excision -- clues must also be present.
Key Takeaways
- Chaos in dermoscopy means asymmetry of structure and pattern, not simply clinical asymmetry of shape or color.
- A lesion with chaos has different dermoscopic patterns in different areas when comparing any two quadrants or halves.
- Chaos alone is not sufficient for biopsy; at least one clue to malignancy must also be present.
4.3 The Chaos and Clues Decision Algorithm Step-by-Step
The algorithm operates as follows:
Step 1 -- Assess for Chaos Examine the pigmented lesion for the presence of dermatoscopic asymmetry of pattern, color, and/or border abruptness.
- If chaos is absent and no exceptions apply --> the lesion is likely benign; no biopsy needed.
- If chaos is present --> proceed to Step 2.
Step 2 -- Search for Clues Examine the chaotic lesion for any one or more of nine clues to malignancy.
- If no clues are found --> monitor or dismiss (the chaos may reflect a benign but atypical lesion).
- If one or more clues are found --> excisional biopsy is considered, unless an unequivocal diagnosis of seborrheic keratosis can be made by pattern analysis.
Step 3 -- Check Exceptions Even for nonchaotic lesions, excisional biopsy is considered in four exceptional circumstances (see Section 4.5).
Check Your Understanding
Name at least four of the 'Clues to Malignancy' used in the Chaos and Clues algorithm.
The clues to malignancy include: thick reticular lines (thick network), gray or blue structures, black dots or clods in the periphery, radial lines or pseudopods (segmental), white lines (only seen with polarized dermoscopy), polymorphous vessels, and lines reticular or branched (for flat nonpigmented lesions). Any single clue plus chaos warrants excision.
4.4 The Nine Clues to Malignancy
Each clue is described below with its histopathologic correlation, which malignancies it applies to, and distinguishing features.
Clue 1: Gray or Blue Structures (Including Gray or Blue Structureless)
Appearance: Gray color contrasting with the brown background of a pigmented melanocytic lesion; blue color contrasting with other colors.
Histopathologic correlations:
- Gray color correlates with melanin in the superficial dermis, either in melanocytes, in keratinocytes, or as melanin incontinence in melanophages (frequently resulting from an immune attack, even on lesions confined to the epidermis).
- Blue color correlates with pigment in the deep dermis, most commonly in nested melanocytes or nests of BCC.
Clinical significance:
- Gray color is the most sensitive clue to malignancy.
- It is seen in most in situ melanomas, and in many pigmented BCCs and pigmented SCCs.
- In a study on flat pigmented facial lesions, the presence of gray color had a sensitivity of 95.8% and specificity of 30.6% for the diagnosis of melanoma.
Applies to: Melanoma, pBCC, pSCC (all three pigmented malignancies).
Clue 2: Eccentric Structureless Area
Appearance: A structureless area that:
- Covers a sufficient area of the lesion to form a pattern
- Is eccentrically located (contrasted to a structured pattern or a structureless pattern of significantly different color)
- Has a color other than skin-colored
Histopathologic correlations:
- Different colors of melanin may be produced by the chaotic behavior of malignant melanocytes
- If pink is present, it may be caused by increased blood flow from the high metabolic demand of tumor tissue
- If white is present, it may correlate with fibrosis after regression
Applies to: Melanoma, pBCC, pSCC (all three pigmented malignancies).
Example: An eccentric light brown structureless area extending to the left of a structured (lines reticular) area in an in situ melanoma.
Clue 3: Thick Reticular Lines
Appearance: Lines reticular where the lines are at least as thick as the holes they surround. In a chaotic lesion, they will be focally distributed rather than evenly widespread.
Histopathologic correlation: Correlates with rete ridges widened by pigment-laden malignant melanocytes.
Applies to: Melanoma specifically -- the presence of reticular lines effectively rules out the diagnosis of BCC or SCC.
Differential considerations: Thick reticular lines frequently occur in seborrheic keratoses due to acanthotic rete ridges (proliferation of pigmented keratinocytes), but in SK they will be widespread and other clues to seborrheic keratosis are expected.
Example: An in situ melanoma with lines reticular on the right and an eccentric structureless area on the left. Inferiorly, the reticular lines are focally thicker than the holes they surround -- unequivocal but focal, consistent with the chaotic behavior of malignant tissue.
Clue 4: Black Dots and Clods, Peripheral
Appearance: Black dots and/or clods located at the periphery of the lesion.
Histopathologic correlation: Correlates with pigmented pagetoid melanocytes and nests of melanocytes in melanomas.
Applies to: Melanoma specifically (though because dots are common in both pBCC and pSCC in situ, and gray may be perceived as black, this clue can also be seen in those tumors in practice).
Why peripheral?: Black dots can be seen centrally in nevi that have been traumatized, correlating with pigment in ascending keratinocytes. Pagetoid spread can occur anywhere in a melanoma, so when black dots or clods are seen peripherally, they are regarded as a clue to malignancy.
Example: A small (4 mm diameter) young melanoma in situ where the feature of peripheral black clods at the upper right border gives the lesion both chaos and a clue.
Clue 5: Lines Radial or Pseudopods, Segmental
Appearance: Radial lines or pseudopods distributed segmentally (asymmetrically) around the lesion periphery.
Histopathologic correlation: In melanocytic lesions, these structures correlate with fascicles of pigmented melanocytes extending from the periphery of a lesion, signifying growth.
Applies to:
- Segmental pseudopods are specific to melanoma
- Lines radial segmental are found in all three pigmented malignancies
Key distinguishing features:
- In melanomas: Radial lines extend from reticular lines, clods, or structureless areas of equivalently dense or darker pigmentation.
- In BCCs: Radial lines invariably converge and may project from hypopigmented structureless areas (though not always).
- In pSCC in situ: Lines radial segmental are usually created by dots in a linear arrangement.
Examples:
- Radial lines/pseudopods segmental in a melanoma in situ extending from pigmented structures as dark as, or darker than, the radial lines/pseudopods.
- In a pBCC, radial lines converge and extend from a nonpigmented area.
- In pSCC in situ, radial lines segmental composed of dots in a linear arrangement; surface keratin is an additional diagnostic clue.
Clue 6: White Lines
Appearance: Lines that are whiter than normal surrounding skin. Two types:
- Polarizing-specific white lines (also called crystalline structures or chrysalis): Straight, shiny white lines oriented perpendicularly to each other but not crossing. Only seen with polarized dermoscopy. Polarizing-specific blue lines have the same significance.
- White lines seen with both modalities: May sometimes correlate with reticular white lines seen with nonpolarized dermoscopy.
Applies to: BCC (pigmented or nonpigmented) -- commonly; melanoma (pigmented or nonpigmented) -- not unusual; pSCC in situ -- rarely.
Also seen in benign lesions: Dermatofibroma and Spitz nevus commonly show white lines. However, white lines are not expected in any other type of nevus (unless traumatized) or in seborrheic keratosis.
Examples:
- Polarized dermoscopy of a melanoma in situ displaying white lines in a perpendicularly oriented arrangement.
- Nonpolarized dermoscopy of an invasive melanoma demonstrating white lines in a reticular arrangement.
Clue 7: Lines Parallel on the Ridges (Acral) / Lines Parallel Chaotic on Nails
Appearance:
- On acral skin (palms/soles): A pattern of parallel lines where pigment follows the dermatoglyphic ridges rather than the furrows
- On nails: Lines parallel that are chaotic (varying in width, interval, and color) in the nail matrix
Applies to: Melanoma specifically on acral skin or nail matrix.
Site specificity: This is the only clue to malignancy that is specific to a particular anatomical site.
Important considerations:
- The longer an acral or nail matrix melanoma remains untreated, the more likely it is to develop any of the other clues to melanoma
- Melanoma may arise in an acral nevus, in which case any of the other eight clues will override a benign parallel furrow pattern that may be present
- An acral melanoma may be arguably symmetrical but still qualifies for excision as an "exception" (see Section 4.5)
Examples:
- Melanoma in situ on the sole with a parallel ridge pattern. Pigmented circles marking the center of ridges correlate with pigmented malignant melanocytes in eccrine ducts.
- Lines parallel chaotic in a nail matrix melanoma -- varying in width, interval, and color.
- Radial lines segmental overriding a benign furrow pattern in a melanoma arising in an acral nevus. In the benign furrow pattern, pigment is over the ridges but the lines (assessed at edges) lie in the furrows.
Clue 8: Polymorphous Vessels
Appearance: More than one morphologic type of vessel present in the lesion.
Applies to:
- Melanoma: Polymorphous vessels including various types of linear vessels in raised portions, dot vessels over macular areas, and any pattern of linear vessel. Generally, other clues (pigment clues and/or white lines) are also expected.
- pBCC: Often has monomorphous serpentine/serpentine branched vessels but may show polymorphous linear vessels, especially on the lower limb. Ulceration (common in BCC) and associated keratinization may produce polymorphous vessels including looped vessels in radial arrangement and even dotted vessels.
- NOT pSCC in situ: Expected to have a monomorphous pattern of coiled vessels (may appear as dots depending on visual acuity and magnification).
Key points for melanoma vessels:
- Dot vessels correlate with vessels ascending in dermal papillae and are not expected in the raised portion of a melanoma (where regular dermal papillae morphology is not expected)
- Vessel clues are useful for differentiating melanoma from pBCC and pSCC in situ
Examples:
- BCC displaying linear polymorphic vessels -- branched serpentine centrally and looped peripherally.
- Totally ulcerated BCC resulting in a polymorphous pattern including almost every vessel type.
- Gray color (clue to malignancy) with serpentine vessels centrally + dot vessels = melanoma (focally invasive).
- Lightly pigmented SCC in situ with monomorphic coiled vessels appearing as dots on one side; a few linear serpentine dermal plexus vessels at the edge do NOT make this a polymorphous pattern.
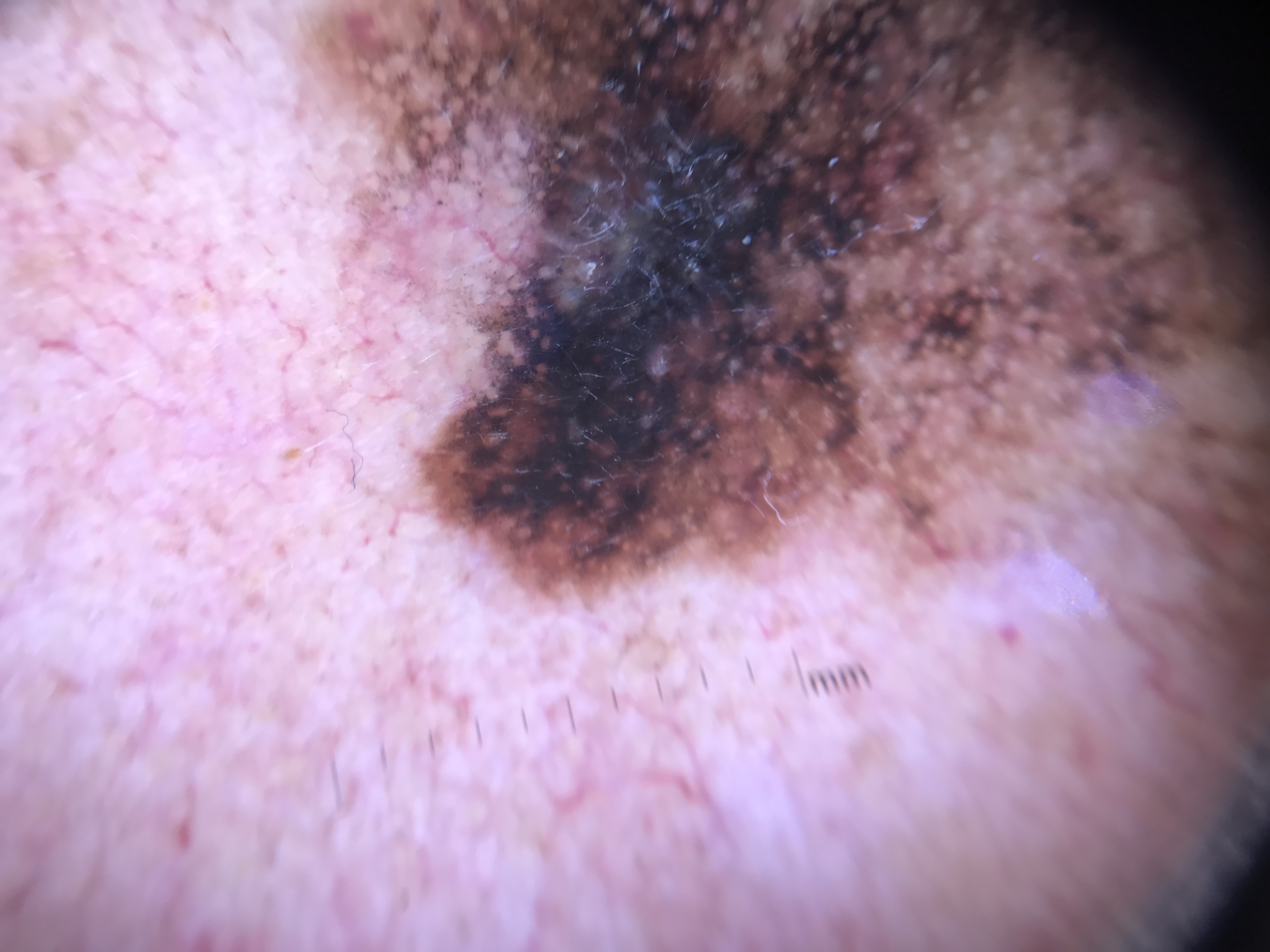
Clinical Scenario
A 47-year-old woman presents with a 9 mm pigmented lesion on the right upper arm that she has been watching for a year. Dermoscopy reveals asymmetry of pattern: a reticular pattern in the upper half and a structureless brown-to-blue area in the lower half. Colors include light brown, dark brown, and gray. You identify the following clues: gray dots scattered in the structureless area (Clue 1 -- gray structures), thick reticular lines in the upper portion where the lines are thicker than the holes they surround (Clue 5 -- thick reticular lines), and segmental radial lines at the 5 o'clock position (Clue 4).
What is your diagnosis and key dermoscopic findings?
Melanoma (superficial spreading type)
Step 1 of Chaos and Clues identifies chaos: the lesion shows more than one pattern (reticular + structureless) combined asymmetrically, more than one color (brown, dark brown, gray) arranged asymmetrically, and variability in border abruptness. Step 2 reveals three clues: gray structures (corresponding to melanophages in the papillary dermis), thick reticular lines (indicating melanoma cell proliferation in the rete ridges -- not seen in pigmented BCC or Bowen disease), and segmental radial lines (highly specific for melanoma, unlike circumferential radial lines seen in Reed nevus). One clue in the presence of chaos would be sufficient for biopsy; three clues make the diagnosis of melanoma highly likely.
Clue 9: Angulated Lines
Appearance: Straight lines (not reticular or branched) meeting at angles of 90 degrees or more but not crossing. These lines may join to enclose a polygon. Straight pigment interfaces have the same significance as straight lines.
Applies to: Primarily melanoma (valuable clue), but may also rarely be seen in pBCC, pSCC in situ, and pigmented actinic keratosis.
Examples:
- Angulated lines forming both complete and incomplete polygons in a melanoma in situ.
- Angulated lines in a pigmented BCC.
Key Takeaways
- The nine clues include: eccentric structureless area, thick lines (reticular/branched), gray or blue structures, black dots/clods at periphery, radial lines or pseudopods (segmental), white lines, polymorphous vessels, parallel ridge pattern (acral), and angulated lines.
- Each clue has a specific histopathologic correlate that explains why it indicates malignancy.
- Only one clue is needed in a chaotic lesion to warrant biopsy; more clues increase specificity but are not required.
4.5 Exceptions: When to Biopsy Even Without Chaos
Chaos and Clues was tested on a consecutive series of pigmented lesions (majority of melanomas being in situ) and found to have a sensitivity of 90.6% (BCC 98.5%, SCC 86.5%, melanoma 79.3%) and a specificity of 62.7% for the diagnosis of malignancy of any type.
To move the sensitivity closer to 100%, the following four exceptions are included:
Exception 1: Any Changing Lesion on an Adult
This includes:
- A lesion with a history of change
- Lesions with monitored change (e.g., documented structural change over 6 months)
- Lesions with dermatoscopic clues to change such as peripheral clods or radial lines/pseudopods
Age-dependent interpretation of peripheral clods:
- Under age 30: Peripheral clods in an otherwise unremarkable nevus are consistent with a growing nevus
- Over age 50: Peripheral clods should raise suspicion
- Between ages 30-50: Weigh the clues, exercise discretion; if doubt remains, excision biopsy is prudent
Examples:
- A lesion monitored for 6 months showing structural change with a small cluster of peripheral black dots at the upper extremity -- excised as melanoma in situ.
- A large symmetrical lesion on the abdomen of a 70-year-old man with peripheral clods/dots -- excised as invasive melanoma.
- A 3 mm diameter raised lesion on the flank of a 60-year-old woman. Despite structural symmetry, it had peripheral clods (clue to change) and gray structures (clue to malignancy) -- nodular melanoma, Breslow thickness 0.8 mm.
Exception 2: A Nodular or Small (<6 mm) Lesion with Any Clue to Malignancy
Small is arbitrarily defined as less than 6 mm in diameter (the size cited in the clinical ABCD method). A nodular or small lesion lacking the morphology of a known benign lesion that has any clue to malignancy should be considered for biopsy.
Important caveats:
- This exception should only be applied if there is an additional significant cause for concern
- Many nevi have gray color or patterns that could be interpreted as angulated lines, but if they are nonchaotic, have a gradual border supporting a diagnosis of nevus, and have no concerning history, biopsy is not indicated
- Dermatofibroma is a small nodular lesion that frequently has central polarizing-specific white lines; if DF can be diagnosed confidently by clinical and dermatoscopic criteria (including historical stability), excision biopsy is not necessary
Exception 3: Any Lesion on the Head or Neck with Pigmented Circles and/or Dermatoscopic Gray
Young melanomas on the head and neck may be symmetrical, possibly related to a physical barrier effect of numerous follicles.
Performance data from a study on flat pigmented facial lesions:
- Gray structures: sensitivity 95.8%, specificity 30.5% for melanoma
- Gray circles: sensitivity 54.2%, specificity 83.3% for melanoma
- Pigmented circles (any color): sensitivity 70.83%, specificity 76.9% for melanoma
Example: A pigmented lesion on the ear lobe of a 42-year-old man that was arguably symmetrical but lacked a uniform border. Pigmented circles related to adnexal openings were a compelling clue to melanoma -- excised as melanoma in situ.
Caveat: A 4 mm lesion on the ear of an adult male with dermatoscopic gray -- technically a small lesion with a clue AND a head/neck lesion with gray. However, the lesion had the unequivocal morphology of a nevus (symmetry, gradual border over total periphery) and historical stability, so excision was not indicated.
Clinical Scenario
A 71-year-old man presents with a 5 mm dome-shaped dark nodule on the scalp that his barber noticed 2 months ago. The lesion is firm, elevated, and reportedly growing. Dermoscopy reveals a relatively organized pattern with homogeneous dark blue-black color. No chaos of pattern or color is immediately apparent. However, you note gray structureless areas at the base and the lesion lacks the morphology of any known benign lesion.
What is your diagnosis and key dermoscopic findings?
Nodular melanoma (suspected -- biopsy via Exception 2)
Although the lesion appears relatively organized (no clear chaos of pattern), Exception 2 of the Chaos and Clues algorithm applies: a nodular or small (<6 mm) lesion with any clue to malignancy and additional cause for concern should be considered for biopsy. The gray structures (Clue 1) are present. The additional causes for concern include: it is an elevated, firm, and continuously growing (EFG) lesion; it is newly detected in an older adult; and it cannot be confidently diagnosed as any benign lesion. Exception 3 also applies (head/neck lesion with gray). Nodular melanomas are a critical pitfall because they may appear organized due to their rapid vertical growth without the asymmetric peripheral features of superficial spreading melanoma.
Exception 4: Any Lesion on Acral Skin with a Parallel Ridge Pattern
Young melanomas on acral skin may be symmetrical, possibly related to a physical barrier effect of numerous eccrine ducts. Any acral lesion with a parallel ridge pattern pigmented by melanin should be considered for excision.
Check Your Understanding
If a lesion shows chaos but no clues, what is the recommended management?
If a lesion shows chaos but no clues to malignancy, it should be monitored rather than immediately excised. The algorithm recommends short-term digital monitoring (3-month follow-up) to detect any emerging clues. The absence of clues significantly reduces the probability of malignancy despite the asymmetric pattern.
4.6 How to Assess for Chaos
A practical approach to assessing chaos:
- View the lesion dermoscopically and ask: "Is this pattern recognizable as any of the common benign lesions (nevus, SK, hemangioma, dermatofibroma, sebaceous hyperplasia)?"
- If yes: The lesion has biological symmetry; move on.
- If no: Assess systematically for:
- Pattern asymmetry: Are there two or more patterns covering significant area (approximately 20% each), arranged asymmetrically?
- Color asymmetry: Are there two or more colors with abrupt transitions, arranged asymmetrically?
- Border abruptness asymmetry: Is there definite, asymmetric variability in how sharply the border is demarcated?
- If equivocating: Ask whether the dermatoscopic pattern is consistent with the chaotic behavior of malignant tissue.
Remember: Shape irregularity is NOT relevant. Only internal organization matters.
4.7 When to Biopsy vs. Monitor
Biopsy is indicated when:
- Chaos is present AND one or more clues to malignancy are found (unless the lesion is unequivocally a seborrheic keratosis)
- Any of the four exceptions apply
Monitoring may be appropriate when:
- The lesion is nonchaotic, recognizable as benign, with no exceptions
- The lesion is chaotic but no clues to malignancy are present (consider short-term monitoring)
- An exception technically applies but the lesion has unequivocal morphology of a specific benign entity with historical stability
Seborrheic keratosis exception: Even if a lesion is chaotic and has clues, if an unequivocal diagnosis of seborrheic keratosis can be made by pattern analysis, excisional biopsy may not be required. This requires confident recognition of SK-specific features.
Key Takeaways
- Biopsy is indicated when chaos plus at least one clue is present; monitoring is appropriate for chaotic lesions without clues.
- Exceptions exist: nodular lesions with blue-black color should be biopsied even without classic chaos, and patient history of change can override the algorithm.
- The algorithm achieves high sensitivity (>90%) for melanoma detection while maintaining reasonable specificity to avoid excessive biopsies.
4.8 Worked Examples from the Text
Example 1: Biological Symmetry vs. Chaos
Five lesions diagnosed by pattern recognition as biologically symmetrical (no chaos): (a) nevus, (b) seborrheic keratosis, (c) hemangioma, (d) dermatofibroma, (e) sebaceous hyperplasia. A sixth lesion (f) was asymmetrical, could not be recognized as any common benign lesion -- pattern analysis revealed disorganization with clues to malignancy; excised as invasive melanoma.
Example 2: Chaos of Border Abruptness
Four lesions from the same patient. Three benign (compound congenital-type nevi) confirmed by stability over time: (a) central clod pattern with peripheral structureless and lines -- concentric symmetry; (b) central skin-colored clods with peripheral lines -- concentric symmetry; (c) structureless pattern with central gray -- symmetry. Shape was irrelevant. The fourth lesion (d) had unequivocal asymmetry of both pattern and color, consistent with chaotic behavior of malignant tissue, and was the only one with chaos of border abruptness -- excised as melanoma in situ.
Example 3: Dermatoscopic Uniqueness
Four lesions on the anterior thigh of a 50-year-old woman. Three were consistent with signature nevi (structureless, biologically symmetrical). The fourth was reasonably symmetrical but was the only clod pattern lesion -- dermatoscopically unique. Excised as melanoma in situ.
Example 4: Nodular Melanoma Caught by Exception
A 3 mm lesion on the flank of a 60-year-old. Only 3 mm diameter and raised. Had structural symmetry, but: (1) peripheral clods as a dermatoscopic clue to change, and (2) it was both small and nodular with the clue of gray structures. Nodular melanoma, Breslow thickness 0.8 mm.
Example 5: Progressive Chaos and Histological Disorganization
Dermatoscopic chaos can be seen to increase along with histological disorganization moving from perilesional skin to melanoma in situ to invasive melanoma -- all encountered on the same patient on the same day.
4.9 Sensitivity and Specificity Data
Overall Chaos and Clues Performance
Tested on a consecutive series of pigmented lesions (majority of melanomas being in situ):
| Metric | Overall | BCC | SCC | Melanoma |
|---|---|---|---|---|
| Sensitivity | 90.6% | 98.5% | 86.5% | 79.3% |
| Specificity | 62.7% | -- | -- | -- |
Reference: Rosendahl C, Tschandl P, Cameron A, Kittler H. Diagnostic accuracy of dermatoscopy for melanocytic and nonmelanocytic pigmented lesions. J Am Acad Dermatol. 2011 Jun; 64(6):1068-73.
Gray Color Performance (Flat Pigmented Facial Lesions)
| Feature | Sensitivity | Specificity |
|---|---|---|
| Any gray structures | 95.8% | 30.6% |
| Gray circles | 54.2% | 83.3% |
| Pigmented circles (any color) | 70.83% | 76.9% |
Reference: Tschandl P, Rosendahl C, Kittler H. Dermatoscopy of flat pigmented facial lesions. J Eur Acad Dermatol Venereol. 2014 Mar 24.
The exceptions were added to address the gap between the 79.3% sensitivity for melanoma and the target of near-100% sensitivity.
Key Takeaways
- Chaos and Clues is designed as a screening algorithm prioritizing sensitivity over specificity to minimize missed melanomas.
- The algorithm performs best when applied systematically to every lesion rather than selectively to suspicious-appearing ones.
- Combining Chaos and Clues with clinical context (patient age, lesion history, ugly duckling sign) further improves diagnostic accuracy.
5. Decision Algorithm Flowchart
flowchart TD
A[Pigmented Lesion] --> B{Red Flag<br/>Present?}
B -->|No| C[Likely Benign<br/>Pattern Recognition]
B -->|Yes| D{Assess for<br/>CHAOS}
D -->|No Chaos| E{Check 4<br/>Exceptions}
D -->|Chaos Present| F{Search for<br/>9 Clues}
E -->|No Exception| C
E -->|Exception Applies| G[Consider Biopsy]
F -->|No Clues Found| H[Monitor /<br/>Reassess]
F -->|1+ Clues Found| I{Unequivocal<br/>SK?}
I -->|Yes| J[Reassure]
I -->|No| K[Consider<br/>Excision Biopsy]
Text version of algorithm
PIGMENTED LESION
|
[Red Flag Present?]
/ \
NO YES
| |
LIKELY BENIGN [Assess for CHAOS]
(pattern recognition) |
/ \
NO CHAOS CHAOS PRESENT
| |
[Check Exceptions] [Search for CLUES]
/ \ / \
NO YES NO CLUES >= 1 CLUE
| | | |
LIKELY CONSIDER MONITOR/ [Unequivocal SK?]
BENIGN BIOPSY REASSESS / \
YES NO
| |
REASSURE CONSIDER
EXCISION BIOPSY
EXCEPTIONS (biopsy even without chaos):
1. Any changing lesion on an adult
2. Nodular or small (<6 mm) lesion with any clue (lacking benign morphology)
3. Head/neck lesion with pigmented circles or gray (lacking benign morphology)
4. Acral lesion with parallel ridge pattern
CLUES TO MALIGNANCY (9 total):
1. Gray or blue structures
2. Eccentric structureless area (any color)
3. Thick reticular lines (focal)
4. Black dots/clods -- peripheral
5. Lines radial or pseudopods -- segmental
6. White lines (polarizing-specific or both modalities)
7. Lines parallel on ridges (acral) / lines parallel chaotic (nails)
8. Polymorphous vessels
9. Angulated lines (>=90 degrees, not crossing)
6. Clue-by-Clue Reference Table
| # | Clue | Dermoscopic Appearance | Histopathologic Correlation | Applies to | Key Differentiator |
|---|---|---|---|---|---|
| 1 | Gray or blue structures | Gray contrasting with brown; blue contrasting with other colors | Gray = melanin in superficial dermis (melanocytes, keratinocytes, melanophages); Blue = pigment in deep dermis (nested melanocytes or BCC nests) | Melanoma, pBCC, pSCC | Most sensitive clue; present in most in situ melanomas |
| 2 | Eccentric structureless area | Structureless area covering significant area, eccentrically placed, non-skin-colored, contrasting with structured pattern or different-colored structureless area | Chaotic melanin production; pink = increased blood flow; white = fibrosis/regression | Melanoma, pBCC, pSCC | Must be eccentric and cover enough area to form a pattern |
| 3 | Thick reticular lines | Lines reticular at least as thick as the holes they surround; focally distributed | Rete ridges widened by pigment-laden malignant melanocytes | Melanoma only | Rules out BCC/SCC; in SK they are widespread, not focal |
| 4 | Black dots/clods, peripheral | Black dots and/or clods at the lesion periphery | Pigmented pagetoid melanocytes and melanocyte nests | Melanoma primarily | Central black dots may be seen in traumatized nevi (benign) |
| 5 | Lines radial/pseudopods, segmental | Radial lines or pseudopods asymmetrically distributed at periphery | Fascicles of pigmented melanocytes extending peripherally | Pseudopods = melanoma only; radial segmental = all three | In melanoma: extend from equally/more pigmented areas; in BCC: converge from hypopigmented areas |
| 6 | White lines | Whiter than surrounding skin; polarizing-specific (perpendicular, non-crossing) or visible with both modalities | Fibrosis, altered collagen | BCC (common), melanoma (not unusual), pSCC (rare) | Also seen in DF and Spitz nevus (benign); NOT expected in other nevi or SK |
| 7 | Lines parallel on ridges / chaotic on nails | Acral: pigment on dermatoglyphic ridges; Nails: lines varying in width, interval, color | Malignant melanocytes in eccrine ducts (acral) or nail matrix | Melanoma only (site-specific) | Only site-specific clue; other clues may override benign furrow pattern |
| 8 | Polymorphous vessels | Two or more vessel morphologies (serpentine, branched, dotted, looped, linear) | Multiple vascular patterns from chaotic angiogenesis | Melanoma, pBCC (may have if ulcerated); NOT pSCC in situ | pSCC in situ = monomorphous coiled; dot vessels not expected in raised melanoma |
| 9 | Angulated lines | Straight lines meeting at >=90 degrees, not crossing; may form polygons; straight pigment interfaces equivalent | Irregular tumor borders at dermis level | Melanoma (primary), rare in pBCC, pSCC, pigmented AK | Distinct from reticular lines (not branched, not forming network holes) |
7. Clinical Pearls
Chaos is not about shape. The silhouette or contour of a lesion is irrelevant. Chaos refers exclusively to the internal asymmetry of pattern, color, and border abruptness. A lesion can be round and symmetric in shape but chaotic internally.
Gray is the most sensitive clue. In a chaotic lesion, gray color should always be searched for first. Its sensitivity for melanoma in flat pigmented facial lesions is 95.8%.
When in doubt about chaos, think about malignancy. If you are equivocating about whether a lesion is chaotic, ask yourself: "Is this pattern consistent with the chaotic behavior of malignant tissue?" This reframing often resolves the question.
Peripheral vs. central black dots matter. Black dots centrally may simply be trauma-related pigment in ascending keratinocytes. Peripheral black dots/clods suggest pagetoid spread and are a clue to melanoma.
Total border abruptness is benign; asymmetric border abruptness is suspicious. An ink-spot lentigo with an abrupt border around 100% of its perimeter would score highly on the ABCD method but shows no chaos of border abruptness. A melanoma with abrupt borders on one side and gradual on the other shows chaotic border abruptness.
Age matters for peripheral clods. Peripheral clods in a teenager are likely a growing nevus. The same finding in a 60-year-old is a red flag for melanoma. Between 30 and 50, exercise clinical judgment.
The dermatoscopic ugly duckling is a powerful red flag. A lesion that looks different from all other lesions on the patient -- even if it appears internally symmetrical -- warrants careful algorithmic assessment.
Seborrheic keratosis is the "escape clause." Even if a lesion is chaotic with clues, an unequivocal SK diagnosis can override the recommendation for biopsy. But the key word is "unequivocal."
Thick reticular lines must be focal to be a clue. In melanoma, thick reticular lines are focally distributed. In seborrheic keratosis, they are widespread. Context is everything.
Head, neck, and acral melanomas can be symmetrical. The exceptions for these sites exist because melanomas in these locations may be constrained by surrounding structures (follicles, eccrine ducts) and present with deceptive symmetry.
Chaos and Clues is a framework, not a straitjacket. The authors explicitly encourage clinicians to use it as a framework on which to organize their accumulated experience and to individualize the method for their own style and practice.
Become an expert at recognizing benign lesions first. The algorithm is only engaged when a lesion cannot be recognized as benign. Rapid, confident pattern recognition of the five common benign groups (nevus, SK, hemangioma, DF, sebaceous hyperplasia) is the foundation of efficient practice.
Clinical Scenario
A 38-year-old woman presents with a 7 mm pigmented lesion on her right calf that she has noticed for approximately one year. Dermoscopy reveals two patterns combined asymmetrically: a reticular pattern on one side and a structureless dark brown area on the other. The border is abrupt inferiorly but gradually fades superiorly. You identify gray structureless areas centrally and a single focus of peripheral black dots at the 3 o'clock position.
What is your diagnosis?
Melanoma (early superficial spreading type)
The lesion demonstrates chaos of pattern (reticular plus structureless areas, asymmetrically combined), chaos of color (dark brown and gray, asymmetrically distributed), and chaos of border abruptness (abrupt inferiorly, gradual superiorly). Two clues to malignancy are present: gray structures (Clue 1, the most sensitive clue, correlating with melanin in the superficial dermis) and peripheral black dots (Clue 4, correlating with pagetoid melanocytes). One clue in the setting of chaos is sufficient to recommend excision biopsy.
Clinical Scenario
A 62-year-old man presents with a 12 mm pigmented lesion on the upper back. He reports no change, but it is the only lesion on his body with a clod pattern -- all of his other moles have a structureless pattern. Dermoscopy shows a reasonably symmetric clod pattern with uniform brown color and a gradual border. No gray structures, no thick reticular lines, and no peripheral black dots are identified.
What is your diagnosis?
Suspicious lesion requiring biopsy (Red Flag 5 -- dermatoscopic ugly duckling)
Although the lesion itself appears biologically symmetrical (no chaos) and no clues to malignancy are identified, Red Flag 5 applies: this is the only clod-pattern lesion among structureless signature nevi, making it dermatoscopically unique. At age 62, a clod pattern nevus is generally not expected. The literature illustrates a similar scenario where a symmetrical but unique lesion was excised as melanoma in situ. Dermatoscopic uniqueness warrants formal algorithmic assessment and consideration of excision biopsy.
Clinical Scenario
A 50-year-old woman presents with a 4 mm flat pigmented lesion on her left cheek. The lesion is smooth to palpation. Dermoscopy reveals a somewhat symmetric pattern with pigmented circles related to follicular openings and subtle gray color between the circles. No obvious chaos of pattern, color, or border abruptness is appreciated. She has extensive background photodamage.
What is your diagnosis?
Suspected melanoma (lentigo maligna) -- biopsy via Exception 3
Although the lesion lacks overt chaos, Exception 3 of the Chaos and Clues algorithm applies: any lesion on the head or neck with pigmented circles and/or dermatoscopic gray that lacks the unequivocal morphology of a known benign lesion should be considered for biopsy. Melanomas on the head and neck may be deceptively symmetrical due to the physical barrier effect of follicular structures. The smooth surface texture (distinguishing it from actinic keratosis, which is rough) and the gray color (sensitivity of 95.8% for melanoma in flat pigmented facial lesions) further support the need for biopsy.
9. Cross-References
| Topic | Source |
|---|---|
| Chaos and Clues algorithm and red flags | Chapter 5a, pp. 70-80 |
| Chaos and Clues flowchart | |
| Biological symmetry concept | 5a.2 |
| Red flags (clinical pattern-breaker, clues to change, uniqueness) | pp. 70-72 |
| Chaos definitions (pattern, color, border abruptness) | pp. 72-73 |
| Gray/blue structures | pp. 73-74 |
| Eccentric structureless area | p. 74 |
| Thick reticular lines | pp. 74-75 |
| Black dots/clods peripheral | p. 75 |
| Lines radial/pseudopods segmental | pp. 75-76 |
| White lines | p. 76 |
| Lines parallel (acral/nails) | pp. 76-77 |
| Polymorphous vessels | pp. 76-78 |
| Angulated lines | p. 78 |
| Exceptions (1-4) | pp. 78-80 |
| Validation study data | p. 78 (Ref. 8) |
| Flat pigmented facial lesion study | pp. 73-74 (Refs. 6, 7) |
| TADA algorithm (comparison) | Chapter 5b |
| Other triage algorithms (comparison) | Chapter 5c |
| Revised pattern analysis (foundation) | Chapter 4a |
| Prediction without Pigment (nonpigmented lesions) | Chapter 4c |
Key References from the Chapter
- Kittler H, Rosendahl C, Cameron A, Tschandl P. Dermatoscopy. 2nd ed. Austria: Facultas; 2016.
- Rosendahl C, Cameron A, McColl I, Wilkinson D. Dermatoscopy in routine practice: "Chaos and Clues." Aust Fam Physician. 2012 Jul; 41(7):482-7.
- Bourne P, Rosendahl C, Keir J, Cameron A. BLINCK: a diagnostic algorithm for skin cancer diagnosis combining clinical features with dermatoscopy findings. Dermatol Pract Conc. 2012;2(2):12.
- Rosendahl C, Hishon M, Cameron A, Barksdale S, Weedon D, Kittler H. Nodular melanoma: five consecutive cases in a general practice. Dermatol Pract Concept. 2014;4(2):15.
- Scope A, Marghoob AA. The "ugly duckling" sign: an early melanoma recognition tool for clinicians and the public. Melanoma Lett. 2007;25:1-2.
- Tschandl P, Rosendahl C, Kittler H. Dermatoscopy of flat pigmented facial lesions. J Eur Acad Dermatol Venereol. 2014 Mar 24.
- Rosendahl C, Cameron A, Wilkinson D, Belt P, Williamson R, Weedon D. Nail matrix melanoma: consecutive cases in a general practice. Dermatol Pract Conc. 2012;2(2):13.
- Rosendahl C, Tschandl P, Cameron A, Kittler H. Diagnostic accuracy of dermatoscopy for melanocytic and nonmelanocytic pigmented lesions. J Am Acad Dermatol. 2011 Jun; 64(6):1068-73.
10. Related Modules
| Module | Relationship |
|---|---|
| Module 01: Introduction and Principles | Prerequisite -- equipment, polarized vs. nonpolarized dermoscopy |
| Module 02: Histopathologic Correlations | Prerequisite -- understanding dermoscopic-histologic correlations for the clues |
| Module 03: Pattern Analysis Revised | Prerequisite -- foundational elements, patterns, and colors used in Chaos and Clues |
| Module 04: Top-Down 2-Step Algorithm | Parallel -- alternative algorithmic approach to lesion triage |
| Module 05: Prediction without Pigment | Companion -- decision algorithm for nonpigmented lesions (Chaos and Clues addresses pigmented lesions) |
| Module 07: TADA and Other Triage Algorithms | Companion -- comparison of Chaos and Clues with TADA, 3-point checklist, AC rule, blue-black rule |
| Module 09: Basal Cell Carcinoma | Extension -- detailed dermoscopic patterns of BCC (relevant to clues 1, 2, 5, 6, 8, 9) |
| Module 11: SCC Spectrum | Extension -- detailed dermoscopic patterns of SCC (relevant to clues 1, 2, 5, 8) |
| Module 12: SK, Solar Lentigo, LPLK | Extension -- SK as the "escape clause" in the algorithm |
| Module 21: Superficial Spreading Melanoma | Extension -- detailed melanoma features (all clues applicable) |
| Module 22: Nodular Melanoma | Extension -- Exception 2 (small/nodular lesions); blue-black rule |
| Module 23: Lentigo Maligna | Extension -- Exception 3 (head/neck); gray structures and circles |
| Module 24: Acrolentiginous Melanoma | Extension -- Clue 7 (parallel ridge pattern); Exception 4 (acral skin) |
| Module 30: Face | Extension -- facial lesion algorithms, annular-granular structures, Exception 3 |
| Module 31: Palms and Soles | Extension -- acral patterns, parallel ridge vs. furrow, Clue 7, Exception 4 |
| Module 33: Nails | Extension -- nail matrix melanoma, lines parallel chaotic (Clue 7) |
| Module 37: Digital Monitoring | Extension -- monitoring strategy for nonchaotic lesions or equivocal findings |
This module is part of the Dermoscopy Educational Course. It should be studied in conjunction with the referenced figures for complete visual understanding of the described dermoscopic features.
Image Sources & Citations
- DERM12345 (Skin Lesion Dataset with 40 Subclasses): DERM12345: A Large-scale Skin Lesion Image Dataset with 40 Subclasses. Figshare. 2023. License: CC-BY-4.0.
- HIBA Dermoscopy Dataset: HIBA Dermoscopy Dataset. Hospital Italiano de Buenos Aires. License: CC-BY-4.0.