Module 04: Top-Down 2-Step Pattern Analysis Algorithm
Source: Dermoscopy Educational Course Authors: Ashfaq A. Marghoob, Natalia Jaimes, and Ralph P. Braun
1. Learning Objectives
After completing this module, the learner should be able to:
- Explain the rationale behind the top-down reasoning strategy and how it differs from the traditional bottom-up 2-step algorithm.
- Apply Step 1 of the algorithm by recognizing the dermoscopic patterns of common benign lesions across four diagnostic levels.
- Identify and differentiate the 12 benign nevus patterns (Level 1) based on network, globules, homogeneous structures, and streaks.
- Distinguish intradermal nevi from basal cell carcinoma using clinical and dermoscopic clues (Level 2).
- Recognize the dermoscopic features of seborrheic keratoses and solar lentigines, including their involuting forms (Level 3).
- Identify other benign lesions (angiomas, angiokeratomas, lymphangiomas, sebaceous hyperplasias, and clear cell acanthomas) by their characteristic dermoscopic patterns (Level 4).
- Apply Step 2 by determining whether an equivocal lesion is disorganized (Step 2a) or organized (Step 2b) and selecting the appropriate evaluation pathway.
- List the melanoma-specific structures, BCC features, and SCC features used in Step 2a, and the five warning features (two patterns, two structures, four colors) that trigger biopsy in Step 2b.
2. Prerequisites
- Module 01: Introduction and Principles of Dermoscopy -- familiarity with polarized vs. nonpolarized dermoscopy and image acquisition.
- Module 02: Histopathologic Correlations of Dermoscopic Structures -- understanding how dermoscopic structures correlate with histologic findings.
- Module 03: Pattern Analysis Revised -- knowledge of basic dermoscopic elements (lines, dots, clods, circles, pseudopods, structureless areas), patterns, colors, and the Chaos and Clues short algorithm.
3. Key Concepts
The Top-Down Reasoning Strategy
Traditional dermoscopy algorithms follow a bottom-up approach: the observer first identifies individual dermoscopic structures, then assembles them into a pattern, and finally arrives at a diagnosis. The top-down approach reverses this sequence:
- The clinician begins by hypothesizing the most probable diagnosis (or differential diagnosis) for the lesion under investigation.
- Dermoscopy is then used to determine which specific features are present or absent to confirm or refute the hypothesis.
- This narrows the differential to the most likely diagnosis.
Key Innovation: Eliminating the Melanocytic/Nonmelanocytic Split
The traditional 2-step algorithm required the clinician to first classify a lesion as melanocytic or nonmelanocytic before proceeding. The top-down 2-step approach eliminates this requirement. Instead:
- Step 1 asks the clinician to recognize specific benign diagnoses (nevi, lentigines, SK, angiomas, etc.).
- Step 2 evaluates any lesion that cannot be confidently diagnosed in Step 1, regardless of whether it is melanocytic or nonmelanocytic.
Organized vs. Disorganized: The Central Dichotomy
The algorithm's second step hinges on one critical assessment -- the degree of entropy (disorder) in the distribution of colors and structures:
- Disorganized (asymmetric, chaotic) lesions have a high probability of malignancy and proceed to Step 2a.
- Organized (symmetric, orderly) lesions are likely benign but must still be screened for specific warning signs in Step 2b.
4. Core Content
4.1 Introduction to the 2-Step Algorithm
The top-down 2-step pattern analysis approach builds upon the previous 2-step approach and combines it with concepts derived from the Triage Amalgamated Dermoscopy Algorithm (TADA), using a top-down strategy of information processing.
Step 1: The observer attempts to make a specific diagnosis by recognizing the patterns associated with common benign skin lesions (e.g., nevi, lentigines, seborrheic keratoses, angiomas). If an unequivocal diagnosis of one of the benign lesions cannot be made with confidence, the lesion proceeds to Step 2.
Step 2: The observer determines whether the overall pattern of the lesion is organized or disorganized (based on the distribution of colors and structures):
- Step 2a (Disorganized): Lesions with a chaotic or asymmetric pattern are evaluated for specific features of BCC, SCC, or melanoma.
- Step 2b (Organized): Lesions with an organized pattern are screened for a specific set of warning features that, if present, should prompt biopsy.
Check Your Understanding
What is the first decision point in the 2-Step Algorithm, and what determines the answer?
The first step asks: Can you make a specific benign diagnosis? The observer attempts to recognize the patterns of common benign skin lesions (nevi, lentigines, seborrheic keratoses, angiomas, etc.) across four diagnostic levels. If an unequivocal diagnosis of one of the benign lesions cannot be made with confidence, the lesion proceeds to Step 2. The top-down approach eliminates the traditional melanocytic/nonmelanocytic classification requirement.
4.2 Step 1: Benign Lesion Recognition
Step 1 is built upon four diagnostic levels that guide the observer through a structured assessment of common benign lesions. Within each diagnostic category, individual dermoscopic structures must be placed within the context of other features present in the lesion -- the global pattern defining a given diagnosis is contingent on the presence of specific structures that carry high predictive value.
Level 1: Patterns in Acquired and Small Congenital Nevi
These nevi include junctional, compound, Spitz, Reed, and Clark's nevi. They display organized patterns, but each requires interpretation in context of:
- Patient history
- Lesion size
- Patient age
- Skin phenotype
- Anatomical location
- Whether the lesion is an outlier (does not adhere to the signature nevus pattern of the patient's other nevi)
There are three fundamental structures (network, globules, homogeneous) whose combinations produce 12 recognized benign patterns:
Network-Based Patterns
a. Diffuse reticular pattern
- Definition: An organized network with minimal variation in thickness and color (regular/typical network). The holes of the network are relatively uniform in appearance.
- Key contextual feature: Sun-damaged skin. Melanoma on sun-damaged skin can sometimes appear as isolated large lentiginous lesions with a network or patchy network pattern.
- Clues to melanoma: Older patient age, relatively large lesion size, presence as an isolated lesion on sun-damaged skin, and a network that is usually not distributed in an organized fashion.
b. Patchy reticular pattern
- Definition: Islands of typical network distributed in an organized manner. The network patches all have the same type of network with minimal variability in thickness and color.
- Key contextual feature: Same as diffuse reticular -- beware of isolated large lentiginous lesions on sun-damaged skin in older patients.
c. Peripheral network with central hypopigmentation
- Definition: Typical/regular network at the periphery with a central portion that is hypopigmented (lighter than the network but darker than the surrounding skin).
- Key contextual feature: Skin phenotype/color. Nevi with central hypopigmentation are usually seen in patients with lighter skin.
- Clues to melanoma: Central hypopigmentation in dark skin phenotypes should raise the possibility of melanoma.
d. Peripheral network with central hyperpigmentation
- Definition: Typical/regular network at the periphery with a central hyperpigmented area (blotch). This blotch is often due to accumulation of melanin-laden corneocytes in the stratum corneum (lamella), which can usually be tape-stripped off to reveal an underlying typical network.
- Key contextual feature: Nevi with central hyperpigmentation are seen in patients with darker skin phenotypes.
- Clues to melanoma: Central hyperpigmentation in light skin phenotypes should raise the possibility of melanoma.
Globular Patterns (+/- Network)
e. Globular pattern
- Definition: Round to oval globules with minimal variability in size and color (regular/typical), distributed in an organized manner within the lesion.
- Key contextual feature: Age and location. These nevi are usually congenital and found on the head/neck or torso.
- Clues to melanoma: Newly acquired lesions with globular morphology in an older individual, especially on an extremity. Black and blue globules (while occasionally seen in congenital nevi) should raise suspicion for melanoma.
f. Cobblestone globular pattern
- Definition: Large brown angulated globules creating a pattern reminiscent of cobblestones. This is a pattern associated with congenital nevi.
- Key contextual feature: Same as globular pattern -- congenital nevi of head/neck and torso.
g. Peripheral network with central brown globules
- Definition: Typical/regular network at the periphery with central brown globules that are regular with minimal variation in size and color. On rare occasions, the globules can be white, as seen in balloon cell nevi.
- Key contextual feature: Age and location (congenital, head/neck or torso).
h. Reticular pattern with peripheral globules
- Definition: Typical network with a peripheral rim of regular brown globules. Associated with the radial growth phase of Clark's/dysplastic nevi.
- Histopathologic correlation: One rim of peripheral globules corresponds to dysplastic nevi with mild to moderate atypia. A multi-tiered peripheral globular pattern corresponds to dysplastic nevi with at least some degree of spitzoid morphology.
- Key contextual feature: Age and location. Most common on the torso of younger to middle-aged patients, often in patients with atypical mole syndrome.
- Clues to melanoma: Newly acquired lesions with peripheral globules in older individuals, especially on an extremity or with melanoma-specific structures.
Streak-Based Pattern
i. Starburst pattern
- Definition: Darkly pigmented nevus with a symmetric distribution of streaks around its perimeter. Associated with Reed's nevi in their radial growth phase.
- Key contextual feature: Age. Streaks can also be encountered in superficial spreading melanoma, but such melanomas are extremely rare in pre-adolescent individuals.
- Clues to melanoma: In children, starburst pattern has an extremely high pretest probability for Reed's nevi. In older individuals, starburst pattern has a heightened pretest probability for melanoma.
Homogeneous Patterns
j. Homogeneous blue
- Definition: Homogeneous blue color with a whitish veil that encompasses the entire lesion's surface -- the hallmark of a blue nevus. The blue color and white veil display minimal variation in hues.
- Key contextual feature: History. Epidermotropic metastasis can mimic blue nevi; a previous history of invasive melanoma is the key contextual feature.
- Clues to melanoma: Multiple hues (heterogeneous blue color or nonhomogeneous veil) should prompt consideration of melanoma.
k. Homogeneous brown
- Definition: Homogeneous brown color with minimal to no variation in hues. Usually devoid of other structures, though rare regular dots/globules and network fragments may be present. Associated with small to medium congenital nevi.
- Key contextual feature: Age. These nevi are present at birth or develop within the first few years of life and are stable.
- Clues to melanoma: Newly acquired homogeneous brown lesions in adults should be viewed with caution. If nonpalpable, digital monitoring is appropriate; biopsy if change is detected.
l. Homogeneous tan/pink
- Definition: Featureless tan to pink color; some may also display vessels.
- Key contextual feature: Skin phenotype/color. These nevi are seen predominantly in individuals with skin types I-II.
- Clues to melanoma: Newly acquired tan to pink nevi in darker-skinned individuals should raise concern for amelanotic or hypomelanotic melanoma. However, amelanotic melanomas are also common in skin types I-II. Outlier lesions should always raise suspicion. Nonpalpable lesions can be digitally monitored; raised lesions or those showing change should be viewed with extreme suspicion.
Level 2: Patterns Seen in IDN and Dermatofibroma (Raised Lesions/Papules)
a. Intradermal Nevi (IDN)
Key contextual features: IDN are defined first and foremost by clinical morphology:
- Miescher's nevi: Raised dome-shaped lesions on the face
- Unna's nevi: Sessile mamillated lesions on the torso
Both types have preserved skin markings and may have hair emanating from their surface.
Dermoscopic features of IDN:
- Predominantly comma-shaped vessels or a polymorphous vascular pattern with at least some comma-shaped vessels
- Brown halo
- Globules (including cobblestone-type globules)
- Small foci of tan to brown structureless pigment and/or hypopigmented areas
Differentiating IDN from BCC (Miescher's type can be challenging):
| Feature | IDN | BCC |
|---|---|---|
| History | Present for many years, no change, no spontaneous bleeding | Recent onset or change |
| Skin markings | Preserved | Lost (shiny surface) |
| Hair | May be present (highly suggestive of IDN) | Absent |
| Wobble sign | IDN wobble on dermoscopy | BCC tend not to wobble |
| Arborizing vessels | Limited arborization, often only one point creating a "Y"-shaped vessel | Extensive arborization |
| Vessel quality | Less sharp focus, less bright color | Sharper focus, brighter red |
| Shiny white blotches/strands | Absent | Present on polarized dermoscopy |
b. Dermatofibromas (DF)
Key contextual features: DFs are firm papules that dimple on lateral pressure.
Dermoscopic features:
- A symmetric lesion with a peripheral network and a central white scarlike area
- In the region between the network and the central scarlike area: ring-like globules and vessels
- With polarized light: the central scarlike area displays a pink hue and often reveals shiny white lines
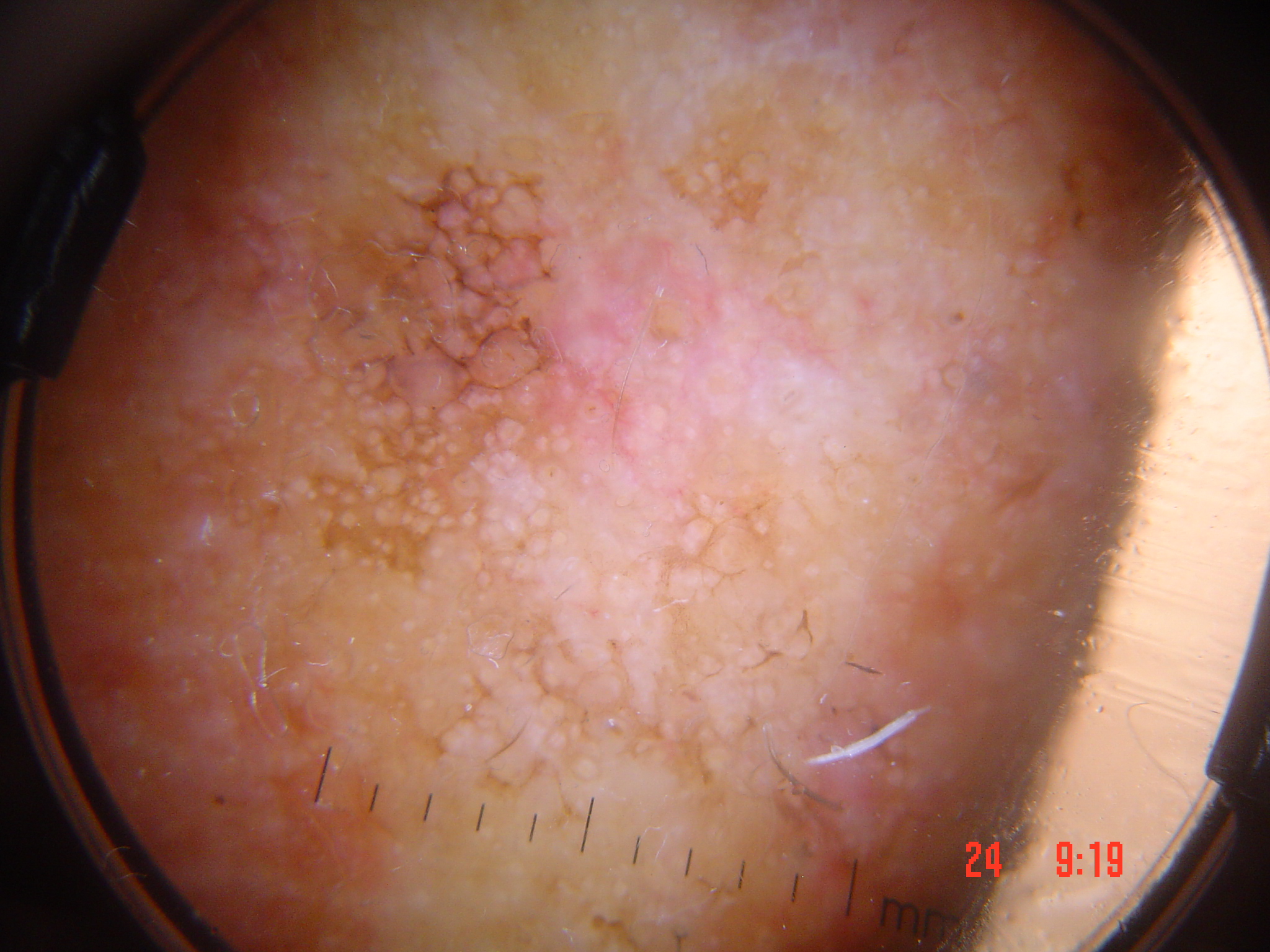
Clinical Scenario
A 42-year-old woman presents with a dome-shaped, flesh-colored papule on the nose that has been present for over 10 years with no change in size. Dermoscopy reveals comma-shaped vessels, a few cobblestone-type globules, a brown halo, and preserved skin markings. A single hair is seen emanating from the surface.
What is your diagnosis and key dermoscopic findings?
Intradermal nevus (Miescher's type)
In Step 1, Level 2 of the 2-Step Algorithm, intradermal nevi on the face (Miescher's nevi) are recognized by their dome-shaped morphology, preserved skin markings, comma-shaped vessels, brown halo, and globules. The presence of hair is highly suggestive of IDN over BCC. Key differentiators from BCC include long history without change, preserved skin markings (BCC has a shiny surface with lost markings), limited vessel arborization (BCC shows extensive branching), and absence of shiny white blotches and strands.
Level 3: Seborrheic Keratosis and Solar Lentigo
Key contextual features and clues:
| Feature | Description |
|---|---|
| Borders | Well-demarcated, sharp borders (both lentigo and SK). Lentigo borders often display a moth-eaten morphology. |
| Gyri/ridges and sulci/fissures | Sulci are often filled with keratin with a brownish color. Short keratin-filled sulci = crypts. Numerous gyri and sulci create a cerebriform to coral fan-like pattern. |
| Fingerprint-like structures | Seen in lentigines; correspond with early gyri formation. On rare occasions, short slightly curved "U"-shaped structures tend to be oriented in the same vectoral direction -- the "jelly sign" (resembling jelly spread with a knife across bread). |
| Milia-like cysts | Multiple (multi) milia-like cysts. |
| Comedo-like openings | Multiple comedo-like openings. |
| Hairpin (looped/twisted looped) vessels | With a white halo. Correspond to capillary loops in the dermal papilla. The white halo corresponds to keratinocytes in rete ridges surrounding the dermal papilla. Some capillaries may become thrombosed, appearing as small black dots or loops. |
Important differential considerations:
Heavily pigmented SK (melanoacanthoma):
- Can display a blue-white veil. Differentiating from melanoma:
- An SK will not display other melanoma-specific structures (streaks, atypical network, angulated lines, negative network, shiny white lines, atypical dots/globules).
- Within the blue-white veil of an SK, one will almost always see multiple comedo-like openings.
- The wobble test: SK slides en bloc, whereas melanoma wobbles.
Lichen planus-like keratosis (LPLK) / involuting lentigo or SK:
- During involution, regression structures (granularity/peppering) may appear, making differentiation from melanoma difficult. Clues:
- Involution of lentigo/SK usually occurs from the edge, moving centripetally. Peppering expanding centrifugally from the center should raise concern for melanoma or melanoma arising in SK.
- In lesions not yet fully involuted, classic lentigo/SK features can usually still be seen at the edge opposite the area of peppering.
- The granularity in involuting lentigo/SK tends to be coarser, and the granules often appear clumped.
Level 4: Other Benign Lesions
a. Angioma and Hemangiomas (Chapter 6g)
- Lacunae with red to maroon to bluish colors, separated from each other with intervening stroma.
b. Angiokeratomas (Chapter 6g)
- Lacunae with varying shades of red, maroon, and blue.
- Thrombosed lacunae may have a black color.
- The center of the lesion often has a blue-whitish veil, and the surrounding skin has an erythematous halo.
c. Lymphangioma (Chapter 6g)
- Lacunae with a clear to slightly yellowish tinge of color.
- Blood may be present; when so, it settles to the bottom of the lacunae due to gravity, creating two-toned lacunae with the hypopyon sign.
d. Sebaceous Hyperplasia (Chapter 6h)
- Whitish/yellowish polylobular globular structures resembling popcorn.
- Crown vessels: present at the periphery, radiating toward the center but not crossing its midline. (Molluscum contagiosum manifests a similar pattern.)
e. Clear Cell Acanthoma (Chapter 6h)
- Dotted or glomerular vessels arranged in a string of pearls pattern.
Note: As expertise is accumulated, Step 1 can be expanded by adding other benign lesions such as poroma and xanthogranuloma, among others.
Check Your Understanding
In Step 2 of the algorithm, what distinguishes the pathway for evaluating equivocal lesions?
Step 2 distinguishes lesions based on whether their overall pattern is organized or disorganized (based on the distribution of colors and structures). Disorganized (chaotic, asymmetric) lesions proceed to Step 2a for evaluation of specific BCC, SCC, or melanoma features. Organized (symmetric, orderly) lesions proceed to Step 2b and are screened for specific warning features that, if present, should prompt biopsy.
Key Takeaways
- The 2-step algorithm first asks whether a lesion can be confidently recognized as benign before proceeding to detailed analysis.
- Nine benign recognition levels provide rapid pattern-based diagnosis: dermatofibroma, seborrheic keratosis, hemangioma, solar lentigo, clear cell acanthoma, and others.
- Failing to recognize a lesion as benign at Step 1 does not mean it is malignant -- it means further analysis in Step 2 is required.
4.3 Step 2: Equivocal Lesion Analysis
Lesions that cannot be unequivocally diagnosed as one of the benign lesions in Step 1 proceed to Step 2. The observer determines whether the overall pattern is organized or disorganized, based on a gestalt impression of the degree of entropy (distribution of colors and structures).
Step 2a: Disorganized Lesions
This step is reserved for lesions manifesting a disorganized or chaotic appearance. In general, these lesions will prove to be cancer or cancer mimickers.
Most common diagnosable cancers: BCC, SCC, and melanoma.
Other malignancies (often also disorganized): Merkel cell carcinoma, sebaceous carcinoma, porocarcinoma. Clues such as color, location, and specific structures (e.g., polylobular structures in sebaceous carcinoma, looped vessels with rounded endings in porocarcinoma) may suggest a specific rare cancer, but no structure or combination can definitively diagnose these rare cancers via dermoscopy. Since these lesions display disorganized patterns overlapping with BCC/SCC/melanoma features, they will get biopsied.
Benign mimickers: A subset of dysplastic nevi, spitzoid nevi, and BAPomas can manifest a disorganized pattern and will likely be biopsied or closely monitored, since dermoscopy alone cannot discriminate them from melanoma. Additional technologies (short-term digital dermoscopy monitoring, confocal microscopy, electrical impedance spectroscopy, gene expression profiling via tape-stripping) may help manage these lesions.
1. Basal Cell Carcinoma (BCC)
Pigmented structures:
- a. Leaf-like structures
- b. Spoke wheel-like structures
- c. Concentric globules
- d. Blue-gray dots in a bird-shot scatter distribution
- e. Blue-gray nonaggregated globules
- f. Blue-gray ovoid nest
Nonpigmented structures:
- a. Arborizing vessels
- b. Ulceration or multiple erosions
- c. Shiny white blotches and strands (seen with polarized dermoscopy)
- d. Multiple aggregated yellowish-whitish globules (MAY globules)
Special subtype -- Fibroepithelioma of Pinkus (BCC subtype):
- Clinically: dry-scaly surface (not shiny), often slightly sessile
- Dermoscopically: features associated with melanoma, including nonarborizing polymorphous vessels, shiny white lines, and reticular depigmentation (hypopigmented to pink lines intersecting at acute angles = HPLA lines), which is a subtype of negative network
2. Squamous Cell Carcinoma (SCC)
- a. Adherent scale (rough texture) -- present in almost all lesions
- b. Glomerular (coiled) vessels:
- Focally distributed towards the periphery
- Diffusely present throughout the lesion
- Aligned linearly within the lesion
- c. White circles
- d. Brown circles
- e. Rosettes (seen with polarized light)
- f. Brown dots aligned in a linear fashion
Special subtypes:
2.1 Keratoacanthoma (KA):
- Characteristic dome-shaped appearance with central scale/keratin
- Dermoscopically: white circles, shiny white blotches, and looped to twisted looped (hairpin) vessels with a whitish halo at the periphery
- Most now agree these represent a form of well-differentiated SCC with potential for spontaneous involution
2.2 Actinic Keratosis (AK):
- Contains cells similar to SCC but not encompassing the entire epidermal thickness
- Rough texture on palpation; considered by some as early SCC
- Nonpigmented AK: Prominent white follicular openings with or without rosettes and perifollicular erythema -- the "strawberry pattern". Some AKs display large areas of adherent scale-crust (hypertrophic AK) with dotted or glomerular vessels.
- Pigmented AK (AK colliding with lentigo): Differentiation from lentigo maligna (LM):
| Feature | Pigmented AK | Lentigo Maligna |
|---|---|---|
| Surface | Rough texture | Smooth surface |
| Follicular openings | Large, whitish, uniformly distributed | Variable size, asymmetric pigment distribution (often grayish), surrounded by gray dots, not uniformly distributed |
| Rosettes | Many | Few to none |
| Angulated lines | Due to keratin -- brownish color, rough texture | Not rough, often grayish tones |
| Color clue | -- | Gray color on facial skin should always prompt consideration of LM |
Note: Collision lesions between pigmented AK and LM are not uncommon on actinically damaged skin.
3. Melanoma
Melanoma-specific structures:
- a) Atypical network
- b) Angulated lines
- c) Atypical streaks
- d) Negative network -- Two distinct subtypes:
- Type 1: Brown elongated to curvilinear globular structures on a lighter background. Associated with melanomas arising in nevi, Spitz nevi, and some small globular congenital-type nevi in children.
- Type 2 (Reticular depigmentation): Hypopigmented to pink lines meeting at acute angles (HPLA lines). Seen in melanoma, Spitz, and Fibroepithelioma of Pinkus.
- e) Shiny white lines -- Should NOT be classified as negative network; created by numerous shiny white lines oriented parallel and orthogonal to each other, resulting in box-shaped polygons.
- f) Atypical blotch(es) -- Including small hyperpigmented areas.
- g) Atypical dots and globules
- h) Blue-white veil -- Over palpable portion of the lesion.
- i) Regression structures -- Peppering/granularity and/or scarlike depigmentation. Key points:
- Granularity in melanoma usually encompasses more than 10% of the surface area.
- The scarlike depigmented area will be flat (nonpalpable) and devoid of vessels and shiny white lines.
- Extensive regression can mimic a blue-white veil; however, in regression, this blue-whitish area will be nonpalpable.
- j) Peripheral tan structureless areas
- k) Atypical vessels -- Except for vessels seen in IDN, any vessel in a melanocytic lesion should raise suspicion for melanoma. Contextual features (morphology of other patient lesions and lesion history) determine management.
Clinical Scenario
A 58-year-old man presents with an 8 mm pigmented lesion on the left shoulder that his wife noticed has become darker over the past 3 months. Step 1 of the 2-Step Algorithm fails to identify a recognizable benign pattern. In Step 2, you note a disorganized pattern with asymmetric distribution of colors and structures. Dermoscopy reveals an atypical network with variable line thickness, segmental streaks at the 3 o'clock position, an eccentric blue-white veil over a palpable area, and peppering occupying approximately 15% of the surface. Multiple colors are present: brown, black, blue-gray, and pink.
What is your diagnosis and key dermoscopic findings?
Melanoma (superficial spreading type)
This lesion proceeds to Step 2a (disorganized pattern). Multiple melanoma-specific structures are present: atypical network (variable line thickness indicates disarranged rete ridges), segmental atypical streaks (indicating radial growth phase melanoma -- unlike the circumferential distribution of Reed's nevus), blue-white veil over a palpable area (indicating acanthosis with orthokeratosis over dermal melanin), and regression structures (peppering over >10% of the surface area). The presence of four or more colors further supports the diagnosis. Immediate biopsy is warranted.
Additional notes on Step 2a:
- Some heavily pigmented nodular BCC may be difficult to differentiate from heavily pigmented nodular melanoma. While subtle clues (vessel morphology, pigment distribution) exist, biopsy should always be performed before definitive management.
- Some LPLK lesions are also difficult to differentiate from melanoma, and biopsy will be needed.
Step 2b: Organized Lesions
This step is reserved for lesions that are not unequivocally benign (from Step 1) but manifest an organized architectural morphology on dermoscopy. While organized lesions are likely benign, certain organized malignancies must not be missed:
- Rare tumors: Merkel cell carcinoma, leiomyosarcoma, and others
- Melanoma subtypes: nodular, nevoid, desmoplastic, spitzoid, amelanotic, epidermotropic metastasis, and featureless/structureless/feature-poor melanomas
The Step 2b Warning Feature Set:
A feature set consisting of any ONE of the following should prompt biopsy:
| Category | Warning Features |
|---|---|
| Patterns (2) | Starburst pattern, Negative network pattern |
| Structures (2) | Vessels, Ulceration |
| Colors (4) | Blue-black, Gray, Shiny white, (any of these) |
If none of these warning features are present: The lesion requires monitoring (e.g., short-term digital dermoscopy monitoring, total body photography) to determine whether it is benign or malignant. Additional technologies such as confocal microscopy, electrical impedance spectroscopy, and gene expression profiling via tape-stripping may assist in management.
Key Takeaways
- Step 2 applies structured algorithms (ABCD rule, 7-point checklist, Menzies method, pattern analysis, or TADA) to equivocal lesions that were not resolved in Step 1.
- The choice of algorithm matters less than consistent application; all validated algorithms achieve comparable sensitivity when used correctly.
- Lesions that remain equivocal after Step 2 should be biopsied or monitored with short-term digital dermoscopy.
4.4 Special Sites (Step 3)
The rules of the 2-step algorithm can be applied to any lesion on the skin. However, additional dermoscopic criteria exist for lesions located on special sites:
| Special Site | Chapter Reference |
|---|---|
| Face | Chapter 11a |
| Palms and soles (volar/glabrous skin) | Chapters 8d, 11b |
| Nail unit | Chapter 11d |
| Mucosal surfaces (lips, genitalia) | Chapter 11c |
These sites have separately different algorithms to assist in differentiating benign from malignant lesions.
Clinical Scenario
A 29-year-old woman presents with a 5 mm organized-appearing lesion on the right forearm that she first noticed 6 months ago. Step 1 does not confidently identify a benign pattern. In Step 2, you determine the lesion has an organized architecture. Dermoscopy reveals a homogeneous tan-pink color with no network, no globules, and no obvious structures. However, you notice faint dotted vessels and a subtle blue-gray hue at one edge.
What is your diagnosis and key dermoscopic findings?
Suspicious for amelanotic/hypomelanotic melanoma -- biopsy indicated
This lesion enters Step 2b (organized but not confidently benign). The Step 2b Warning Feature Set requires only ONE of the following to prompt biopsy: starburst pattern, negative network, vessels, ulceration, blue-black color, gray color, or shiny white structures. This lesion meets at least two warning criteria: vessels (dotted vessels) and gray color (blue-gray hue at one edge). Despite the organized appearance, even a single warning feature mandates biopsy or further workup. Feature-poor or amelanotic melanomas can appear deceptively organized.
Check Your Understanding
What should you do if a lesion cannot be confidently diagnosed as benign in Step 1?
If the lesion cannot be unequivocally diagnosed as one of the benign lesions in Step 1 (across all four diagnostic levels), it proceeds to Step 2 regardless of whether it is melanocytic or nonmelanocytic. In Step 2, you determine whether the overall pattern is organized or disorganized, then follow the appropriate evaluation pathway (Step 2a for disorganized lesions, Step 2b for organized lesions).
Key Takeaways
- Special anatomic sites (face, acral skin, nails, mucosa) require site-specific algorithms because standard pattern rules do not apply.
- Facial lesions lack a true pigment network; acral lesions follow parallel pattern rules; nail lesions require longitudinal band analysis.
- Applying trunk-and-extremity algorithms to special sites leads to both missed melanomas and unnecessary biopsies.
5. Algorithm Decision Tree
flowchart TD
A[Examine Lesion] --> B{Step 1: Specific<br/>Benign Diagnosis?}
B -->|Level 1: Nevus| C[12 Benign Nevus<br/>Patterns Recognized]
B -->|Level 2: IDN/DF| D[Raised Lesion:<br/>IDN or Dermatofibroma]
B -->|Level 3: SK/Lentigo| E[SK or Solar<br/>Lentigo Features]
B -->|Level 4: Other| F[Angioma, Angiokeratoma,<br/>Lymphangioma, etc.]
B -->|Not Recognized| G{Step 2: Organized<br/>or Disorganized?}
C --> H[Benign -- Manage<br/>Accordingly]
D --> H
E --> H
F --> H
G -->|Disorganized| I{Step 2a: Which<br/>Malignancy?}
G -->|Organized| J{Step 2b: Any<br/>Warning Features?}
I -->|BCC features| K[Manage as BCC]
I -->|SCC features| L[Manage as SCC]
I -->|Melanoma features| M[Manage as<br/>Melanoma]
I -->|Other/Mimicker| N[Biopsy or Monitor]
J -->|Starburst, Negative network,<br/>Vessels, Ulceration,<br/>Blue-black, Gray, White| O[Biopsy<br/>Recommended]
J -->|None present| P[Monitor with<br/>Digital Dermoscopy]
Text version of algorithm
STEP 1: Can you make a specific benign diagnosis?
|
+---> Level 1: Acquired/Small Congenital Nevus?
| |
| +---> Network patterns: diffuse reticular, patchy reticular
| | peripheral network + central hypo/hyperpigmentation
| +---> Globular patterns: globular, cobblestone, peripheral
| | network + central globules, reticular + peripheral globules
| +---> Streak: starburst pattern
| +---> Homogeneous: blue, brown, tan/pink
| |
| +-- YES --> BENIGN (manage accordingly, consider contextual clues)
|
+---> Level 2: IDN or Dermatofibroma?
| |
| +---> IDN: dome-shaped (face) or sessile (torso), comma vessels
| | brown halo, globules, preserved skin markings
| +---> DF: firm papule, dimples on lateral pressure, peripheral
| | network, central white scar, ring-like globules
| |
| +-- YES --> BENIGN
|
+---> Level 3: Seborrheic Keratosis or Solar Lentigo?
| |
| +---> SK/SL: sharp borders, gyri/sulci, fingerprints, milia-like
| | cysts, comedo-like openings, hairpin vessels + white halo
| | moth-eaten borders (lentigo)
| |
| +-- YES --> BENIGN (watch for LPLK mimicking melanoma)
|
+---> Level 4: Other Benign Lesion?
| |
| +---> Angioma: red-maroon-blue lacunae with stroma
| +---> Angiokeratoma: multi-colored lacunae + thrombosis
| +---> Lymphangioma: clear/yellowish lacunae, hypopyon sign
| +---> Sebaceous hyperplasia: popcorn globules + crown vessels
| +---> Clear cell acanthoma: string of pearls vascular pattern
| |
| +-- YES --> BENIGN
|
+-- NO to all levels -->
|
STEP 2: Is the pattern ORGANIZED or DISORGANIZED?
|
+---------------------------------------+----------------------------------+
| | |
v v |
STEP 2a: DISORGANIZED STEP 2b: ORGANIZED |
(Asymmetric / Chaotic) (Symmetric / Orderly) |
| | |
+---> BCC features? +---> ANY of the following? |
| (leaf-like, spoke wheel, | - Starburst pattern |
| blue-gray ovoid nests, | - Negative network |
| arborizing vessels, | - Vessels |
| ulceration, MAY globules, | - Ulceration |
| shiny white blotches) | - Blue-black color |
| --> Manage as BCC | - Gray color |
| | - Shiny white color |
+---> SCC features? | |
| (adherent scale, glomerular +-- YES --> BIOPSY |
| vessels, white/brown circles, | |
| rosettes, brown dots) +-- NO --> MONITOR |
| --> Manage as SCC | (digital dermoscopy, |
| | confocal microscopy, |
+---> Melanoma features? | other technologies) |
| (atypical network, angulated | |
| lines, streaks, negative +----------------------------------+
| network, shiny white lines
| atypical blotch, atypical
| dots/globules, blue-white
| veil, regression, peripheral
| tan structureless, atypical
| vessels)
| --> Manage as melanoma
|
+---> Other malignancy?
| (Merkel cell, sebaceous CA
| porocarcinoma)
| --> BIOPSY
|
+---> Benign mimicker?
(dysplastic nevi, spitzoid
nevi, BAPomas)
--> BIOPSY or MONITOR
6. Clinical Pearls
The outlier rule: Always compare a lesion to the patient's other nevi. An outlier nevus -- one that does not conform to the patient's "signature nevus pattern" -- should always raise the index of suspicion for melanoma, regardless of how benign its individual features may appear.
Age is the single most powerful contextual modifier: A starburst pattern in a child is almost certainly a Reed's nevus; the same pattern in an older adult carries a substantially higher pretest probability for melanoma. Apply this principle across all Level 1 patterns.
The wobble sign has two applications: (a) IDN wobbles on dermoscopy while BCC tends not to wobble; (b) SK slides en bloc while melanoma wobbles. This simple maneuver can resolve two of the most common diagnostic dilemmas.
Tape-stripping is a diagnostic tool: Central hyperpigmentation (blotch) in network nevi is often a melanin lamella in the stratum corneum. Tape-stripping removes it and reveals the underlying typical network, confirming the benign nature.
Gray on the face = think lentigo maligna: Any time gray color is seen in a lesion on facial skin, lentigo maligna should be in the differential diagnosis regardless of other features.
"Y"-shaped vessels in IDN vs. extensive arborization in BCC: When evaluating a raised facial papule with arborizing vessels, count the branching points. A single branching point creating a "Y" shape favors IDN; multiple levels of branching (true arborization) favors BCC.
The hypopyon sign in lacunar lesions: Gravity-dependent settling of blood creating two-toned lacunae is pathognomonic for lymphangioma and distinguishes it from hemangioma.
Crown vessels that do not cross the midline: This pattern is shared by sebaceous hyperplasia and molluscum contagiosum -- clinical context (age, location, number of lesions) completes the differentiation.
Negative network is not one entity: Two morphologically distinct subtypes exist -- brown curvilinear globular structures on a lighter background (type 1) and reticular depigmentation/HPLA lines (type 2). Both can be seen in melanoma, but type 2 is also seen in Fibroepithelioma of Pinkus.
Regression structures: location and pattern matter: In involuting SK/lentigo, peppering starts at the edge and moves centripetally, with coarse clumped granules. In melanoma, peppering tends to be finer and may expand centrifugally from the center.
The Step 2b safety net: An organized lesion lacking ALL warning features (starburst, negative network, vessels, ulceration, blue-black, gray, white) is NOT necessarily benign -- it requires monitoring. Featureless or feature-poor melanomas exist and are diagnosed only by detecting change over time.
8. Cross-References
| Topic | Chapter | Pages |
|---|---|---|
| Top-Down 2-Step Algorithm (this chapter) | 4b | 50-60 |
| Pattern Analysis Revised (Chaos and Clues) | 4a | - |
| Prediction without Pigment | 4c | - |
| BCC dermoscopic features | 6b | - |
| SCC spectrum | 6d | - |
| SK and solar lentigo | 6e | - |
| Vascular lesions (angioma, angiokeratoma, lymphangioma) | 6g | - |
| Adnexal tumors (sebaceous hyperplasia, clear cell acanthoma) | 6h | - |
| Acquired and small congenital nevi | 7a, 7b, 7d, 7e | - |
| Intradermal nevi | 7c | - |
| Dermatofibroma | 6a | - |
| Melanoma-specific structures | 8 | - |
| Nodular, nevoid, desmoplastic, spitzoid, amelanotic melanoma | 8b, 8e, 8f | - |
| Acral (volar) lesions | 8d, 11b | - |
| Face | 11a | - |
| Nails | 11d | - |
| Mucosal surfaces | 11c | - |
Key References from the Chapter
- Jaimes N, Marghoob AA. Triage amalgamated dermoscopic algorithm. J Am Acad Dermatol. 2020 Feb.
- Marghoob AA, Braun R. Proposal for a revised 2-step algorithm for the classification of lesions of the skin using dermoscopy. Arch Dermatol. 2010;146(4):426-8.
- Rogers T, Marino M, Dusza SW, Bajaj S, Marchetti MA, Marghoob A. Triage amalgamated dermoscopic algorithm (TADA) for skin cancer screening. Dermatol Pract Concept. 2017;7(2):39-46.
9. Related Modules
| Module | Relationship |
|---|---|
| Module 01: Introduction and Principles of Dermoscopy | Prerequisite -- equipment, polarized vs. nonpolarized |
| Module 02: Histopathologic Correlations | Prerequisite -- structural correlates |
| Module 03: Pattern Analysis Revised | Prerequisite -- basic elements, Chaos and Clues |
| Module 05: Prediction without Pigment | Companion -- decision algorithm for nonpigmented lesions (Chapter 4c) |
| Module 06: Chaos and Clues Triage Algorithm | Companion -- alternative triage framework |
| Module 07: TADA and Other Triage Algorithms | Companion -- TADA shares concepts with the top-down approach |
| Module 08: Dermatofibroma | Deepens Level 2 (DF recognition) |
| Module 09: Basal Cell Carcinoma | Deepens Step 2a (BCC features) |
| Module 11: SCC Spectrum | Deepens Step 2a (SCC/KA/AK features) |
| Module 12: SK, Solar Lentigo, and LPLK | Deepens Level 3 |
| Module 13: Vascular Lesions | Deepens Level 4 (angioma, angiokeratoma, lymphangioma) |
| Module 14: Adnexal Neoplasms | Deepens Level 4 (sebaceous hyperplasia, clear cell acanthoma) |
| Module 15: Congenital Melanocytic Nevi | Deepens Level 1 (globular/cobblestone patterns) |
| Module 16: Acquired Melanocytic Nevi | Deepens Level 1 (network patterns, outlier concept) |
| Module 17: Intradermal Nevus | Deepens Level 2 (IDN recognition) |
| Module 18: Blue Nevi and Variants | Deepens Level 1 (homogeneous blue pattern) |
| Module 19: Spitz and Reed Nevi | Deepens Level 1 (starburst pattern) |
| Module 21: Superficial Spreading Melanoma | Deepens Step 2a (melanoma-specific structures) |
Module 04 -- Top-Down 2-Step Pattern Analysis Algorithm Part of the Dermoscopy Educational Course. Authors of source material: Ashfaq A. Marghoob, Natalia Jaimes, Ralph P. Braun
Image Sources & Citations
- DERM12345 (Skin Lesion Dataset with 40 Subclasses): DERM12345: A Large-scale Skin Lesion Image Dataset with 40 Subclasses. Figshare. 2023. License: CC-BY-4.0.
- HIBA Dermoscopy Dataset: HIBA Dermoscopy Dataset. Hospital Italiano de Buenos Aires. License: CC-BY-4.0.