Module 37: Digital Monitoring --- Short-Term and Long-Term
Dermoscopy Education Series Chapter 13: Digital Monitoring: Short- and Long-Term (Kittler & Menzies)
1. Learning Objectives
Upon completion of this module, the learner will be able to:
- Explain the rationale for digital dermoscopic monitoring in patients with equivocal melanocytic lesions and in high-risk populations.
- Define sequential digital dermoscopy imaging (SDDI) and describe its workflow, including image capture, storage, and side-by-side comparison.
- Distinguish between short-term monitoring (approximately 3-month interval) and long-term monitoring (6--12-month interval) with respect to protocols, change criteria, and clinical indications.
- Classify morphologic changes as significant or nonsignificant according to the established criteria for both short-term and long-term monitoring intervals.
- Identify lesion types appropriate for digital monitoring versus those that require immediate excision without monitoring.
- Describe the natural history of melanocytic nevi as revealed by digital dermoscopy, including patterns of symmetric enlargement, peripheral globules, senescence, and involution.
- Discuss the role and limitations of artificial intelligence and automated change detection in digital dermoscopy surveillance.
- Apply patient selection criteria for short-term and long-term monitoring programs based on individual melanoma risk profiles.
2. Prerequisites
| Prerequisite | Topic |
|---|---|
| Modules 01--07 | Foundational dermoscopy principles, pattern analysis, algorithmic approaches (two-step, chaos and clues, TADA) |
| Modules 21--28 | Melanocytic lesion differentiation, melanoma recognition, diagnostic sensitivity and specificity |
Learners should be comfortable with dermoscopic structures (network, globules, dots, streaks, blotches, regression structures, blue-white veil, vascular patterns) and the distinction between melanoma-specific and nevus-associated features before proceeding.
3. Key Concepts
| Concept | Definition |
|---|---|
| Surveillance dermoscopy | Systematic, repeated dermoscopic evaluation of melanocytic lesions over defined time intervals to detect early malignant change |
| Sequential digital dermoscopy imaging (SDDI) | A second-level diagnostic tool involving repeated digital dermoscopic imaging of an equivocal lesion at defined time points, with side-by-side comparison on a monitor |
| Total body photography (TBP) | Standardized photographic documentation of the entire skin surface at baseline, used to detect new or changed lesions at subsequent examinations |
| Short-term monitoring | SDDI protocol with a follow-up interval of approximately 2.5--4.5 months (usually 3 months), where ANY morphologic change triggers excision |
| Long-term monitoring | SDDI protocol with follow-up intervals of 6--12 months, where only SPECIFIC substantial changes trigger excision |
| Change detection | Identification of morphologic alterations in a lesion between time points, either by human comparison or automated/AI-assisted analysis |
| Featureless melanoma | Melanoma lacking classic dermoscopic melanoma-specific structures, identifiable only by morphologic change on sequential imaging |
| Involution | The natural process of pigment loss and regression in a senescent nevus, representing the final stage of the nevus life cycle (distinct from regression in melanoma) |
4. Core Content
4.1 Rationale for Digital Monitoring
The diagnosis of the majority of melanocytic skin lesions can be made with certainty using dermoscopy. However, diagnostic accuracy is not 100%. When a melanocytic lesion is doubtful for melanoma---whether clinically or dermoscopically---the standard approach is excision to rule out malignancy. This strategy is adequate for most clinical situations, but it becomes impractical in two common scenarios:
- Patients with multiple (sometimes hundreds of) doubtful melanocytic lesions -- Excising all equivocal lesions is neither feasible nor appropriate.
- Nevi with banal dermoscopic appearance presenting with a history of change -- Excision is not usually necessary, but both patient and physician benefit from knowing the actual biological dynamics of the lesion.
Digital imaging technology has made it easy to store, retrieve, and compare dermoscopic images of melanocytic lesions over time. Dermoscopic images provide a detailed view of subsurface structures that cannot be identified by conventional photographic close-ups. Monitoring changes within these subsurface structures via digital dermoscopy:
- Improves diagnostic sensitivity for early melanoma by identifying incipient changes over time.
- Reduces unnecessary biopsies of biologically indolent (senescent, non-changing) benign lesions.
It is generally agreed that patients with multiple nevi need regular skin examinations, including self-examination and physician-performed full-body examinations. Photographic close-ups and digital dermoscopic images are powerful adjuncts to this surveillance process.
4.2 Sequential Digital Dermoscopy Imaging (SDDI)
4.2.1 Concept and Workflow
SDDI is defined as a second-level diagnostic tool that involves:
- Baseline capture -- A digital dermoscopic image of the equivocal lesion is acquired under standardized conditions.
- Interval -- A defined waiting period (short-term: approximately 3 months; long-term: 6--12 months).
- Follow-up capture -- A repeat digital dermoscopic image is acquired under the same conditions.
- Side-by-side comparison -- Both images are displayed on a monitor and compared for morphologic changes.
- Clinical decision -- Based on the presence, type, and significance of any detected changes, a management decision is reached (continued monitoring versus excision).
SDDI improves diagnostic accuracy for melanoma:
- Specificity improved: Reduces unnecessary skin biopsies of benign lesions by up to 75%.
- Sensitivity improved: Identifies "featureless" melanomas based on change alone, which would otherwise be missed.
These observations in multiple clinical trials have led to the recommendation for routine use of SDDI by national clinical guidelines. SDDI is frequently used during surveillance of high-risk patients in conjunction with dermoscopy and total body photography.
4.2.2 Which Lesions to Monitor
Appropriate for SDDI:
- Melanocytic lesions that are flat or slightly raised
- Lesions that do not display features of melanoma but are otherwise considered doubtful (e.g., because of a recent history of change)
- Mildly atypical melanocytic lesions
NOT appropriate for SDDI (excise instead):
- Lesions that are raised or nodular -- these must be excised rather than monitored
- Lesions with clear dermoscopic features of melanoma (melanoma-specific structures present)
Critical principle: Digital dermoscopic follow-up is restricted to flat or slightly raised melanocytic lesions that are only mildly atypical.
4.2.3 Image Capture Standardization
Effective SDDI depends on standardized, reproducible image acquisition:
- Same dermoscopic device and magnification at baseline and follow-up
- Consistent contact medium (if contact dermoscopy is used)
- Consistent lighting conditions
- Anatomic orientation markers to ensure the same area is captured
- Digital storage with patient identification and lesion location metadata
- Software capable of side-by-side display of baseline and follow-up images
Check Your Understanding
What is the primary goal of digital dermoscopic monitoring (sequential digital dermoscopy)?
The primary goal is to detect melanoma at the earliest possible stage by identifying subtle changes in dermoscopic morphology over time that would not be apparent on a single examination. By comparing standardized dermoscopic images taken at baseline and follow-up, even minimal changes in structure, color, or symmetry can be detected.
Key Takeaways
- Short-term digital dermoscopy (3-month follow-up) is used for equivocal melanocytic lesions; any morphologic change at short-term review is an indication for excision.
- The rationale for short-term monitoring is that benign nevi are stable over 3 months while melanomas show detectable changes in structure, color, or pattern.
- Short-term monitoring is NOT appropriate for lesions with features already suspicious for melanoma (blue-white veil, irregular vessels, regression) or for nodular lesions.
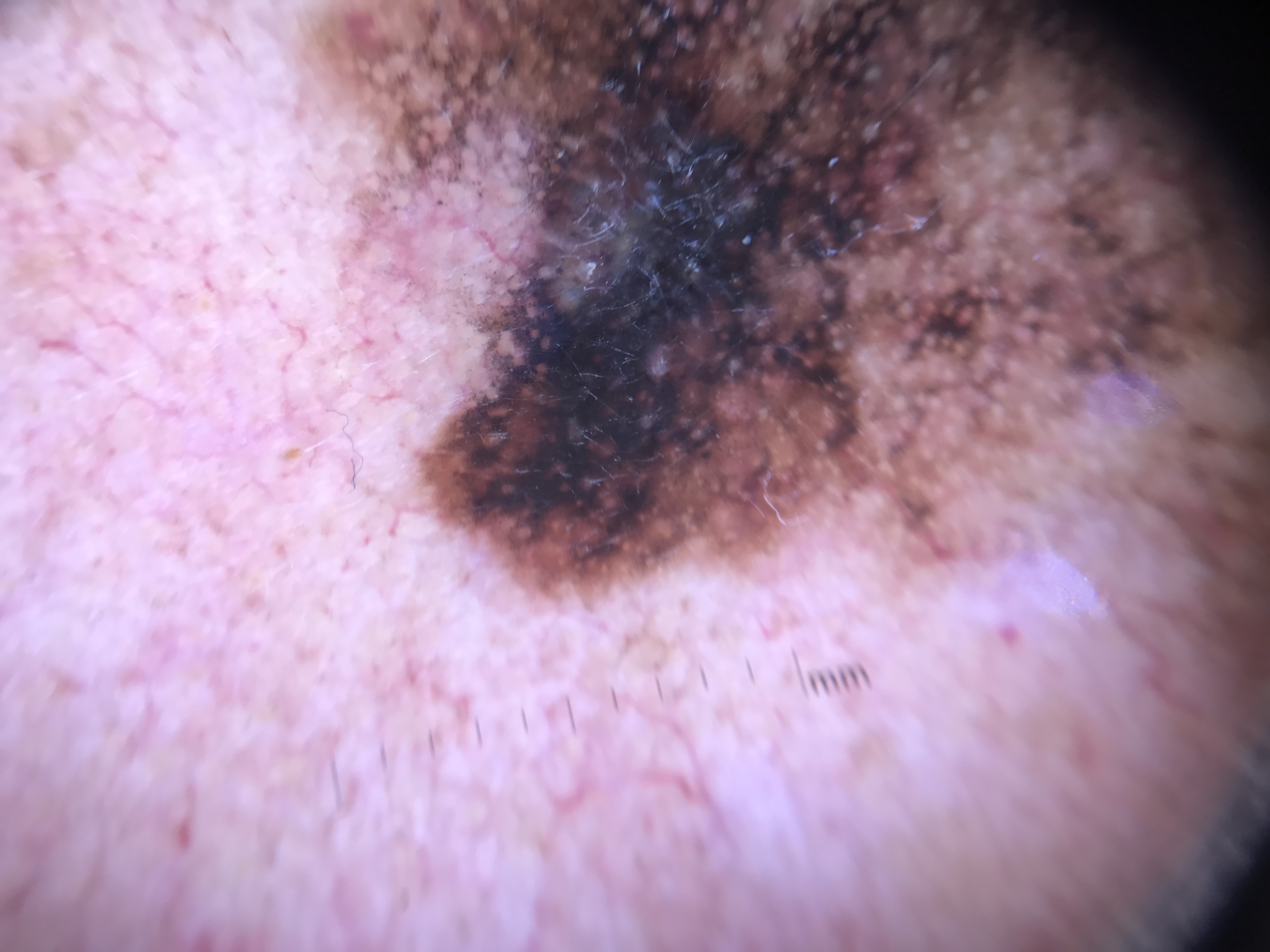
Clinical Scenario
A 38-year-old man with a personal history of melanoma and more than 100 nevi is enrolled in a digital dermoscopy monitoring program. At his 3-month short-term follow-up, comparison of sequential dermoscopic images reveals that one 6 mm truncal lesion has developed new peripheral brown globules asymmetrically distributed on one side, a subtle color shift from light brown to darker brown focally, and loss of the previously regular reticular pattern in one quadrant. All other monitored lesions are unchanged.
What is the significance of these changes at short-term review, and what is the appropriate management?
Excision recommended -- morphologic change at short-term follow-up
The fundamental principle of short-term digital dermoscopy monitoring (typically 3-month intervals) is that any morphologic change detected at short-term review is an indication for excision. Benign melanocytic nevi are biologically stable over a 3-month period, while early melanomas show detectable changes in structure, color, or pattern. In this case, the asymmetric development of peripheral globules, focal darkening, and loss of regularity are all suspicious changes. Symmetric peripheral globules in young patients can be a sign of benign growth, but asymmetric globule distribution is concerning. This approach allows detection of featureless melanomas that lack classic melanoma-specific structures at any single time point but reveal themselves through change over time.
4.3 Total Body Photography (TBP)
4.3.1 Concept and Setup
Total body photography provides standardized photographic documentation of the patient's entire skin surface. TBP serves as a macroscopic baseline for comparison at subsequent surveillance visits, enabling detection of:
- New lesions that were not present at baseline
- Changed lesions whose macroscopic appearance has evolved
TBP is typically acquired in a standardized set of poses (usually 15--25 views) with consistent lighting, camera settings, and positioning. It is most frequently used in conjunction with dermoscopy and SDDI for surveillance of high-risk patients.
4.3.2 Comparative Approach
At each follow-up visit:
- The patient's current skin is compared against the TBP baseline images.
- Any new or visibly changed lesion identified on clinical comparison is then examined with dermoscopy.
- Equivocal new or changed lesions are enrolled into SDDI protocols or excised based on clinical judgment.
4.3.3 Macro vs Dermoscopic Imaging
| Feature | Total Body Photography (Macro) | Digital Dermoscopy (SDDI) |
|---|---|---|
| Resolution | Clinical-level (surface) | Subsurface structural detail |
| Purpose | Detect new and overtly changed lesions | Detect subtle morphologic change in individual lesions |
| Scope | Entire body surface | Individual lesion(s) of concern |
| Change detection | New lesion appearance, gross size/color change | Structural/architectural changes invisible to the naked eye |
| Limitation | Cannot detect subtle subsurface changes | Cannot survey the entire body; requires pre-selection of lesions |
Two melanomas in the Kittler et al. study did not enlarge but showed changes only in their dermoscopic structures. These tumors probably would have been missed or detected much later if followed only by conventional clinical photography---demonstrating the superiority of dermoscopic monitoring for detecting subtle change.
4.4 Short-Term Monitoring (3-Month Follow-Up)
4.4.1 Protocol
- Baseline (Time 0): Capture standardized digital dermoscopic image of the equivocal melanocytic lesion.
- Follow-up (approximately 3 months): Capture a repeat image under the same conditions.
- Side-by-side comparison: Display both images on a monitor and evaluate for ANY morphologic change.
- Decision: If ANY change is detected (other than nonsignificant changes listed below), the lesion must be excised.
The optimal short-term monitoring interval is 2.5--4.5 months (median 3 months).
4.4.2 Criteria for Significant Change
In short-term monitoring, any morphologic change other than the following nonsignificant changes is considered significant and mandates excision:
Nonsignificant changes (short-term):
- Overall solar-induced pigment changes (generalized darkening or lightening)
- Increase or decrease in the number of milia-like cysts
Significant changes (short-term):
- Any change other than the above nonsignificant changes
- Any focal increase in size
- Any internal architectural change
- Any change in color, shape, or structure
Key principle: No specific type of morphologic change can distinguish melanoma from nevi when lesions are monitored over this short duration; therefore, ANY change during the 3-month period leads to excision.
4.4.3 Which Lesions Are Appropriate for Short-Term Monitoring
- Flat or slightly raised melanocytic lesions
- Dermoscopically mildly atypical or equivocal lesions
- Lesions lacking melanoma-specific structures but clinically suspicious (e.g., patient reports recent change)
- Dermoscopically "banal" lesions with a history of change
4.4.4 Which Lesions Should NOT Be Monitored (Excise Instead)
- Raised or nodular lesions -- Not appropriate for SDDI; must be excised
- Lesions with clear dermoscopic features of melanoma
- Lesions with any melanoma-specific structures already identified
4.4.5 Sensitivity and Specificity of Short-Term Monitoring
Evidence from clinical trials (Menzies et al. and subsequent larger series):
| Parameter | Value |
|---|---|
| Lesions unchanged at 3 months | ~81% |
| Lesions showing morphologic change | ~19% |
| Changed lesions that were melanoma | ~11% of changed lesions (~2% of total) |
| Melanomas detected that were in situ | 5 of 7 (71%) |
| Invasive melanomas | 2 of 7, Breslow thickness 0.25 mm and 0.28 mm |
| Melanomas lacking classic features | Nearly two-thirds (up to one-third in some series) |
| Sensitivity for non-lentigo-maligna melanoma | ~94% at 2.5--4.5 months |
| Sensitivity for lentigo maligna | ~75% at 2.5--4.5 months |
| Benign lesions remaining unchanged at 2.5--4.5 months | Majority |
| Reduction in unnecessary biopsies | Up to 75% |
| Featureless melanomas detected via SDDI | Up to one-third of all melanomas discovered |
Special consideration -- Lentigo maligna:
- Only 75% of lentigo maligna will show change within the standard 3-month interval.
- For 25% of cases, changes develop more gradually.
- When lentigo maligna is in the differential diagnosis, a second monitored interval between 6 and 12 months following the baseline image is recommended.
4.4.6 Outcome Significance
- None of the melanomas detected by short-term monitoring developed any classic clinical or dermoscopic features of melanoma.
- These melanomas were identifiable only by morphologic change recognizable on comparative analysis.
- Short-term monitoring enables detection of incipient (featureless) melanomas while decreasing unnecessary excision of clinically suspicious benign lesions.
Check Your Understanding
What types of changes during digital monitoring warrant biopsy?
Changes warranting biopsy include: new or enlarging focal structures (asymmetric new dots, globules, streaks, or regression structures), development of new colors, evolution from an organized to a disorganized pattern, and any change in a previously stable melanocytic lesion in adults. Global symmetric enlargement alone in young patients may be benign, but focal changes are always concerning.
4.5 Long-Term Monitoring
4.5.1 Protocol
- Baseline: Capture digital dermoscopic images of all doubtful melanocytic lesions in the high-risk patient.
- Follow-up interval: 6--12 months (may extend to years for ongoing surveillance).
- Side-by-side comparison: Compare images at each follow-up visit.
- Decision: Excise lesions showing specific substantial changes (see criteria below).
Long-term SDDI is tailored for patients with multiple doubtful melanocytic skin lesions who are under lifelong regular surveillance.
4.5.2 Change Detection Criteria
In contrast to short-term monitoring, long-term monitoring uses specific change criteria to determine which lesions require excision:
Significant changes (long-term) -- mandate excision:
- Asymmetric enlargement (change in size AND shape)
- Focal changes in pigmentation or structure
- Regression features
- Change in color (other than overall lightening or darkening)
- Appearance of melanoma-specific structures
- Appearance of new structures or new colors
Nonsignificant changes (long-term) -- do NOT mandate excision:
- Darker or lighter overall appearance
- Change in number or distribution of brown globules
- Decrease in number of black dots
- Disappearance of inflammatory reaction
- Disappearance of small foci of pigment network within the central portion of the lesion and replacement by diffuse brown pigmentation
Caveat: Although disappearance of network foci and replacement with diffuse brown pigmentation is classified as nonsignificant, this change can also be seen in slow-growing melanomas and warrants heightened vigilance.
4.5.3 Evidence from the Kittler et al. Cohort
| Parameter | Value |
|---|---|
| Patients | 202 (with multiple melanocytic nevi) |
| Lesions monitored | 1,862 |
| Median follow-up | 1 year |
| Stable or nonsignificant change | 96% |
| Substantial changes | 75 lesions (4%) |
| Melanomas among changed lesions | 8 |
| Melanomas in situ | 5 of 8 |
| Breslow thickness of invasive melanomas | All < 0.75 mm |
| Patients unaware of change | 6 of 8 melanoma patients |
Key findings:
- Even in patients with multiple nevi, the vast majority (96%) of lesions will not show substantial changes -- patients can be reassured.
- 6 of 8 patients with melanoma were unaware that the lesion had changed, confirming that patients have difficulty detecting subtle changes.
- Two melanomas did not enlarge but showed changes only in their dermoscopic structures -- demonstrating the superiority of dermoscopic monitoring over clinical photography alone.
4.5.4 Evolution Patterns in Nevi (Benign vs Malignant Change)
Changes observed by SDDI are more pronounced with longer follow-up intervals, for both nevi and melanomas. However, the pattern of change differs:
| Feature | Melanomas | Nevi |
|---|---|---|
| Growth pattern | Asymmetric enlargement (change in size AND shape) -- more frequent | Symmetric enlargement (change in size but NOT shape) -- more frequent |
| Structural changes | Appearance of new structures -- more frequent | Structural changes less common |
| Color changes | Appearance of new colors -- more frequent | Color changes less common |
| Interpretation | Changes strongly suggest malignancy when asymmetric | Symmetric growth with peripheral globules is consistent with benign radial growth |
The interpretation of follow-up images strongly depends on the length of the observation period, with longer follow-up intervals increasing the chances of detecting new melanomas.
Key Takeaways
- Long-term sequential dermoscopy (6-12 month intervals) is the standard for monitoring patients with multiple atypical nevi and high melanoma risk.
- The ugly duckling sign (a nevus that is morphologically distinct from the patient's other nevi) is a powerful clinical complement to dermoscopic monitoring and should be assessed at every visit.
- Total body photography combined with sequential dermoscopy is the most effective surveillance strategy for high-risk patients, allowing detection of both changing and new lesions.
Clinical Scenario
A 42-year-old woman with a family history of melanoma undergoes her annual total body photography comparison visit. Comparison of current clinical images against her baseline TBP reveals a new 4 mm pigmented lesion on her upper back that was not present 12 months ago. Dermoscopy of this new lesion shows a small structureless brown area without any classic melanoma-specific features. All previously documented nevi are stable on both clinical and dermoscopic comparison.
How should this new lesion be managed, and what is the rationale?
Excision or short-term monitoring of the new lesion
In high-risk patients undergoing total body photography surveillance, the detection of a new lesion that was not present at baseline is itself a significant finding that warrants careful evaluation. Even though this lesion lacks classic melanoma-specific structures on a single dermoscopic examination, de novo melanomas (those arising without a precursor nevus) can initially appear dermoscopically bland or featureless. Studies have shown that TBP-aided surveillance detects melanomas that are thinner on average than those found without TBP, precisely because new and changed lesions are identified early. The appropriate management is either direct excision (given the patient's risk profile and the lesion's novelty) or enrollment into short-term digital dermoscopy monitoring (3-month follow-up) to detect early morphologic change. In patients over age 40, new melanocytic lesions are uncommon and merit a lower threshold for biopsy.
4.6 The Natural History of Melanocytic Nevi Revealed by Digital Dermoscopy
Digital monitoring has provided unique insight into the biological lifecycle of melanocytic nevi:
4.6.1 Symmetric Enlargement with Peripheral Brown Globules
- Melanocytic nevi typically show symmetrical enlargement without structural changes.
- The dermoscopic sign of a peripheral rim of brown globules is highly characteristic of symmetrically enlarging nevi in youth.
- This pattern can also be found in eruptive nevi in immunocompromised patients (e.g., post-renal transplantation).
- As long as these lesions manifest:
- A single row of peripheral brown globules
- Develop in younger individuals
- Do NOT display any melanoma-specific structures (atypical network, negative network, atypical streaks, shiny white lines, atypical dots and globules, irregular blotch, blue-white veil, regression structures, atypical vessels, peripheral brown structureless areas)
- Then there is no need for excision. These nevi represent benign nevi growing in a radial (horizontal) plane.
4.6.2 Histopathologic Correlation
- Histopathology and confocal microscopy have confirmed that peripheral globules correspond to junctional nevomelanocytic nests at the tips of rete ridges in Clark-type nevi.
- The globules are relatively small, homogeneous, and brown, with the same color as the rest of the nevus.
- The central portion of the nevus typically has a reticular or homogeneous pattern.
4.6.3 Peripheral Globules and Age
- The pattern of peripheral rim of globules is common in youth.
- Prevalence declines rapidly after the third decade of life.
- The pattern is not observed at all after the sixth decade.
- Management algorithm: Age-appropriate expectation -- peripheral globules in a young person are normal; in older individuals, this pattern warrants greater concern.
4.6.4 Tiered Globules and Starburst Pattern
- Nevi with multiple rows of peripheral globules (tiered globules) are classified as having a starburst pattern.
- The starburst pattern is usually associated with Spitz/Reed nevus (see Chapter 7e).
- Both peripheral globular and starburst patterns are signs of active radial growth.
- When the radial growth phase ends and the nevus enters senescence, the peripheral globules, streaks, or tiered globules are no longer visible.
- The senescent nevus typically manifests a reticular or homogeneous pattern.
4.6.5 Asymmetric Enlargement
- Although most growing nevi enlarge symmetrically, some show asymmetrical enlargement.
- Biopsy is generally recommended for asymmetrically enlarging nevi to rule out melanoma.
4.6.6 Involution
- Loss of pigmentation may occur in a melanocytic nevus, resulting in partial to complete disappearance.
- Although involution can occur in youth, it is more common in adults and elderly individuals.
- Involution represents the last step in the natural evolution of a melanocytic nevus.
- Involution is NOT the same as regression: Regression is an active inflammatory process seen in lesions with a halo reaction or dermoscopic regression structures.
4.6.7 Melanoma Arising in a Congenital Nevus
- Digital monitoring can detect melanoma arising within a congenital nevus -- an important but uncommon observation demonstrating the value of longitudinal surveillance.
Check Your Understanding
What are the recommended monitoring intervals, and for which patients is digital monitoring most appropriate?
Standard monitoring intervals are 3 months for the first follow-up (short-term) and then every 6-12 months for long-term surveillance. Digital monitoring is most appropriate for patients with multiple atypical nevi (atypical mole syndrome), personal or family history of melanoma, and patients with lesions that are dermoscopically equivocal but not clearly warranting immediate biopsy.
4.7 Digital Tools and Technologies
4.7.1 Imaging Devices and Software
Digital dermoscopy platforms typically comprise:
- Dermoscope with digital capture capability (contact or non-contact polarized dermoscopy attached to a digital camera or smartphone adapter)
- Dedicated software for image storage, retrieval, patient/lesion indexing, and side-by-side comparison
- Total body photography stations -- multi-camera arrays or standardized single-camera setups for whole-body imaging
- Integrated platforms combining TBP with dermoscopic imaging in a single workflow
Key software requirements:
- Patient and lesion database with body-map annotation
- Side-by-side baseline vs. follow-up display
- Standardized image metadata (capture date, device, magnification, body site)
- DICOM or equivalent medical imaging compliance
4.7.2 Automated Change Detection
- Software-based change detection algorithms compare sequential dermoscopic images and flag lesions that have changed beyond a threshold.
- Automated systems can reduce the burden on clinicians when monitoring large numbers of lesions across many patients.
- Human error in change detection (failure to identify or incorrectly dismissing change as nonsignificant) is a known source of lost sensitivity -- it is anticipated that artificial intelligence applications detecting change will remove such human errors.
4.7.3 Computer-Aided Diagnosis
- Computer-aided diagnosis (CAD) systems analyze dermoscopic images for features suggestive of malignancy.
- CAD can augment clinical decision-making but is not a replacement for expert dermoscopic assessment.
- Current CAD systems show variable performance depending on the training dataset, the model architecture, and the clinical population.
4.8 AI and Dermoscopy
4.8.1 Machine Learning Applications
- Deep learning models (convolutional neural networks) have been applied to dermoscopic image classification, achieving performance comparable to or exceeding that of dermatologists in some study settings.
- AI can be applied to both single-image classification (malignant vs. benign) and sequential change detection (identifying meaningful change between baseline and follow-up images).
4.8.2 Current State and Limitations
- AI tools are trained on curated datasets and may not generalize well across different skin types, dermoscopic devices, or clinical populations.
- False-positive and false-negative rates remain a concern, especially for featureless melanomas and slow-growing melanomas.
- Regulatory approval and clinical validation in prospective settings are still evolving.
- AI should be viewed as a decision-support tool, not an autonomous diagnostic system.
4.8.3 AI-Assisted Triage
- It is anticipated that AI applications capable of detecting change in sequential dermoscopic images will reduce the human errors inherent in manual comparison.
- AI-assisted triage could flag lesions with the highest probability of change for priority clinician review.
- This is particularly relevant for high-volume clinics monitoring hundreds of lesions per patient.
Key Takeaways
- Meaningful dermoscopic changes include new structures (dots, globules, streaks), color shifts (new gray or blue), architectural disruption (loss of symmetry), and regression.
- Symmetric enlargement alone in a nevus may represent physiologic growth (especially in young patients) and should be interpreted in context rather than automatically prompting excision.
- Artificial intelligence and computer-assisted dermoscopy are increasingly used for change detection, offering objective measurement of growth, color shift, and structural evolution.
4.9 Patient Selection for Monitoring
4.9.1 Risk Stratification
SDDI is most valuable for patients at elevated melanoma risk, including:
- Patients with multiple (dysplastic/atypical) nevi (atypical mole syndrome)
- Patients with a personal history of melanoma
- Patients with a family history of melanoma
- Patients with fair skin and high cumulative UV exposure
- Immunocompromised patients with eruptive nevi
4.9.2 High-Risk Patient Protocols
For individuals at extreme high risk:
- Combination approach: TBP + dermoscopy + SDDI used together during surveillance
- Long-term SDDI is recommended for routine surveillance
- Short-term SDDI is applied to individual suspicious lesions identified during surveillance visits
- Follow-up intervals: Typically every 6--12 months for long-term monitoring, with interim 3-month short-term monitoring for newly suspicious lesions
National guidelines recommend the routine use of SDDI for high-risk patient surveillance.
4.9.3 When to Stop Monitoring and Excise
Excision should replace monitoring when:
- Short-term monitoring: ANY change (other than nonsignificant changes) is detected at the 3-month follow-up
- Long-term monitoring: Specific substantial changes are detected (asymmetric enlargement, focal structural change, new structures, new colors, regression features)
- The lesion becomes raised or nodular at any point during monitoring
- The lesion develops melanoma-specific structures at any point
- The patient is noncompliant with follow-up -- if the patient does not return for scheduled follow-up, the safety net of monitoring is lost, and excision of equivocal lesions should be considered
- Clinical judgment identifies features suggesting rapid growth or malignant transformation
4.9.4 Digital Monitoring Decision Algorithm
The following flowchart summarizes the clinical decision pathway for digital dermoscopic monitoring:
flowchart TD
A[Equivocal melanocytic lesion identified] --> B{Raised or nodular?}
B -->|Yes| C[Excise immediately]
B -->|No| D{Melanoma-specific structures present?}
D -->|Yes| C
D -->|No| E{Multiple equivocal lesions?}
E -->|No| F[Short-term SDDI: 3-month follow-up]
E -->|Yes| G[Enroll in long-term SDDI program]
F --> H{ANY morphologic change at 3 months?}
H -->|No change| I{Lentigo maligna in differential?}
I -->|Yes| J[Extend to 6-12 month follow-up]
I -->|No| K[Reassure and discharge or continue surveillance]
H -->|Change detected| L[Excise for histopathology]
G --> M{Significant change at 6-12 months?}
M -->|Asymmetric enlargement / focal change / new structures| L
M -->|Nonsignificant change only| N[Continue long-term monitoring]
J --> M
Text version of the digital monitoring decision algorithm
- Evaluate equivocal melanocytic lesion
- If raised/nodular OR melanoma-specific structures → Excise immediately
- If flat/slightly raised without melanoma features:
- Single equivocal lesion → Short-term SDDI (3-month follow-up)
- Multiple equivocal lesions → Long-term SDDI (6-12 month program)
- Short-term (3 months): ANY change → excise; no change + lentigo maligna differential → extend to 6-12 months; no change + no LM concern → reassure
- Long-term (6-12 months): Significant changes (asymmetric enlargement, focal structural change, new structures/colors, regression) → excise; nonsignificant changes → continue monitoring
4.10 The Risks and Benefits of Follow-Up
Benefits:
- Improves the detection rate for melanoma
- Reduces the excision rate of benign lesions
- Enables detection of featureless melanomas that would otherwise be missed
- Reduces the benign-to-malignant biopsy ratio
- Provides reassurance for patient and physician when lesions remain stable
Risks:
- Patient noncompliance: The utility of sequential imaging critically depends on patient compliance with follow-up. If the patient does not return, the loss of sensitivity may prove problematic.
- Missed change: Sensitivity is lost when the melanoma is not detected because the change was not identified or was erroneously considered insignificant.
- Slow-growing melanoma: Some melanomas, particularly lentigo maligna, change gradually and may not be detected within the standard 3-month short-term interval (only 75% of lentigo maligna change within 3 months).
- Delay in diagnosis: Although some delay occurs inherently with monitoring, studies have shown that a delay in diagnosis during monitoring does not necessarily equate to a worse prognosis, as melanomas detected through monitoring tend to be thin (< 0.75 mm Breslow thickness).
4.11 Evidence-Based Recommendations
SDDI reduces the benign-to-malignant biopsy ratio and reduces the number of benign lesions excised while improving diagnostic sensitivity for melanoma by identifying dermoscopically featureless melanoma.
Digital dermoscopic follow-up is restricted to flat or slightly raised melanocytic lesions that are only mildly atypical. Raised or nodular lesions must be excised.
Any morphologic change at 3 months from baseline (short-term monitoring) requires excision. Over 90% of melanomas (non-lentigo-maligna type) and approximately 15% of nevi will display change within 3 months. Between 10% and 30% of changed lesions will prove to be melanoma, and up to one-third of these melanomas will not reveal any melanoma-specific structures.
About 75% of lentigo maligna will change within 3 months. In 25% of cases, changes develop more gradually, and a longer follow-up interval (6--12 months) is necessary.
Changes are more pronounced during long-term follow-up for both nevi and melanomas.
When follow-up is 6 months or longer, any lesion with an increase in size (more frequently asymmetric), appearance of new structures, or appearance of new colors requires excision to rule out melanoma.
Long-term SDDI is recommended for routine surveillance of high-risk patients, ideally in combination with TBP and clinical dermoscopy.
Key Takeaways
- A standardized imaging protocol (consistent lighting, positioning, magnification, and device) is essential for reliable comparison of sequential dermoscopic images.
- Patient selection for monitoring should be risk-stratified: high-risk patients (dysplastic nevus syndrome, personal/family melanoma history) receive more intensive surveillance.
- Digital dermoscopy does not replace clinical judgment; it is a tool that augments the clinician's ability to detect subtle changes that may not be apparent on individual examination.
5. Digital Monitoring Decision Flowchart
flowchart TD
A[Equivocal melanocytic<br/>lesion identified] --> B{Raised or<br/>nodular?}
B -- Yes --> C[Excise immediately<br/>Do NOT monitor]
B -- No --> D{Melanoma-specific<br/>structures?}
D -- Yes --> C
D -- No --> E[Flat or slightly raised<br/>mildly atypical lesion]
E --> F{Single suspicious<br/>lesion or high-risk<br/>patient surveillance?}
F -- Single lesion --> G[Short-term SDDI<br/>3-month follow-up]
F -- High-risk surveillance --> H[Long-term SDDI<br/>6-12 month follow-up]
G --> I{Any morphologic<br/>change at 3 months?}
I -- No change --> J[Lesion stable:<br/>reassure or continue<br/>monitoring]
I -- Nonsignificant only<br/>solar pigment / milia --> J
I -- Any other change --> K[Excise the lesion]
H --> L{Change detected<br/>at 6-12 months?}
L -- No change or<br/>nonsignificant only --> M[Continue long-term<br/>monitoring]
L -- Asymmetric enlargement /<br/>new structures / new colors /<br/>regression features --> K
J --> N{Lentigo maligna<br/>in differential?}
N -- Yes --> O[Extend follow-up<br/>to 6-12 months]
N -- No --> P[Routine follow-up<br/>or discharge]
O --> L
6. Monitoring Protocol Comparison Table
| Parameter | Short-Term Monitoring | Long-Term Monitoring |
|---|---|---|
| Follow-up interval | 2.5--4.5 months (usually 3 months) | 6--12 months (ongoing) |
| Target population | Any patient with a mildly suspicious flat/slightly raised lesion | High-risk patients with multiple doubtful nevi under lifelong surveillance |
| Lesion selection | Individual equivocal flat or slightly raised melanocytic lesions | Multiple doubtful melanocytic lesions across the body |
| Change criteria for excision | ANY change (other than nonsignificant) | SPECIFIC substantial changes (asymmetric enlargement, focal structural/color change, regression features, melanoma-specific structures) |
| Nonsignificant changes | Overall solar-induced pigment change; change in milia-like cyst number | Overall lightening/darkening; globule number/distribution changes; black dot decrease; loss of inflammation; focal network loss replaced by diffuse brown pigmentation |
| Sensitivity for melanoma | ~94% (non-lentigo-maligna); ~75% (lentigo maligna) | Increases with longer follow-up intervals |
| Specificity | High (81% of lesions unchanged; up to 75% reduction in unnecessary biopsies) | Very high (96% of lesions stable or showing only nonsignificant change) |
| Melanoma detection characteristics | Thin melanomas (most in situ); up to one-third featureless | Thin melanomas (all < 0.75 mm); melanomas show asymmetric growth, new structures, new colors |
| Lentigo maligna consideration | If lentigo maligna is in the differential, extend to 6--12 months | Standard protocol |
| Combined use | Often combined with TBP in high-risk patients | Routinely combined with TBP and dermoscopy |
7. Change Detection Criteria Table
Based on Kittler & Menzies
| Change Type | Short-Term (3 months) | Long-Term (6--12 months) |
|---|---|---|
| Asymmetric enlargement | Significant | Significant |
| Focal increase in size | Significant | Significant |
| Internal architectural change | Significant | Significant |
| Focal changes in pigmentation or structure | Significant | Significant |
| Change in color (focal) | Significant | Significant |
| Appearance of new structures | Significant | Significant |
| Appearance of new colors | Significant | Significant |
| Regression features | Significant | Significant |
| Melanoma-specific structures | Significant | Significant |
| Overall darkening or lightening (solar-induced) | Nonsignificant | Nonsignificant |
| Change in milia-like cyst number | Nonsignificant | N/A (not listed) |
| Change in brown globule number/distribution | Significant | Nonsignificant |
| Decrease in black dot number | Significant | Nonsignificant |
| Disappearance of inflammatory reaction | Significant | Nonsignificant |
| Central network loss replaced by diffuse brown pigmentation | Significant | Nonsignificant (but see caveat*) |
*Caveat: Central network loss replaced by diffuse brown pigmentation, while classified as nonsignificant in long-term monitoring, CAN also be seen in slow-growing melanomas and warrants close attention.
8. Patient Selection Guide
| Patient Profile | Recommended Monitoring Strategy | Rationale |
|---|---|---|
| Single mildly suspicious flat lesion | Short-term SDDI (3 months) | Detect featureless melanoma; avoid unnecessary excision if stable |
| Flat lesion with history of change, banal dermoscopy | Short-term SDDI (3 months) | History of change alone warrants monitoring; most will prove benign |
| Multiple atypical nevi (atypical mole syndrome) | Long-term SDDI (6--12 months) + TBP | Lifelong surveillance; cannot excise all lesions; detect new melanomas |
| Personal history of melanoma | Long-term SDDI + TBP | Elevated lifetime risk; comprehensive surveillance |
| Family history of melanoma, fair skin | Long-term SDDI + TBP | Risk-appropriate surveillance strategy |
| Equivocal lesion, lentigo maligna in differential | Short-term SDDI initially; if no change at 3 months, extend to 6--12 months | Only 75% of lentigo maligna change at 3 months |
| Raised or nodular suspicious lesion | Excise immediately -- do NOT monitor | Monitoring is inappropriate for raised/nodular lesions |
| Lesion with melanoma-specific structures | Excise immediately -- do NOT monitor | Melanoma-specific features mandate biopsy, not monitoring |
| Immunocompromised patient with eruptive nevi | Long-term SDDI + TBP | Peripheral globule pattern may be seen; context-dependent assessment |
| Noncompliant patient | Consider excision over monitoring | If patient will not return for follow-up, sensitivity of monitoring is lost |
| Peripheral rim of globules in patient < 30 years | Observation without excision (unless melanoma-specific structures) | Expected pattern of benign radial growth in youth |
| Peripheral rim of globules in patient > 60 years | Heightened concern; consider biopsy | Pattern not expected after the sixth decade |
9. Clinical Pearls
The power of "nothing changed": In short-term monitoring, 81% of monitored lesions remain unchanged, and in long-term monitoring, 96% remain stable or show only nonsignificant changes. Stability is the most common and most reassuring finding.
Featureless melanomas are real: Up to one-third of melanomas discovered by SDDI lack any classic dermoscopic melanoma-specific structures. Without digital monitoring, these melanomas would be missed. This is the single most compelling argument for SDDI.
Short-term rule is absolute: In short-term monitoring (approximately 3 months), ANY change other than overall solar pigment shifts or milia-like cyst changes mandates excision. There is no "wait and see" -- excise the lesion.
Long-term monitoring discriminates: Unlike the "any change = excise" rule of short-term monitoring, long-term monitoring requires interpretation. Asymmetric enlargement, new structures, new colors, and regression features trigger excision, while symmetric darkening/lightening and globule redistribution generally do not.
Asymmetry is the red flag in long-term monitoring: Melanomas more frequently grow asymmetrically (change in size AND shape), whereas nevi more frequently grow symmetrically (change in size but NOT shape).
Lentigo maligna is the exception: Only 75% of lentigo maligna will show change within 3 months. When lentigo maligna is in the differential, extend the follow-up to 6--12 months before concluding the lesion is stable.
Never monitor nodular lesions: Raised or nodular lesions are categorically inappropriate for SDDI. Excise them.
Patients cannot self-detect subtle change: Six of eight melanoma patients in the Kittler et al. study were unaware that their lesion had changed. This underscores the value of instrument-assisted (digital dermoscopy) surveillance over patient self-monitoring alone.
Involution is NOT regression: Loss of pigmentation in a nevus (involution) is a normal biological endpoint. Do not confuse it with regression, which is an active inflammatory process associated with dermoscopic regression structures and may indicate malignancy.
Peripheral globules in youth are normal: A single row of peripheral brown globules in a nevus in a young person represents normal radial growth. These nevi do not need excision as long as they lack melanoma-specific structures. However, this pattern after age 60 should not be dismissed.
Compliance is a prerequisite for safety: The entire safety model of digital monitoring depends on the patient returning for follow-up. If compliance is uncertain, excision of equivocal lesions is the safer strategy.
Thin melanomas dominate: All melanomas detected through digital monitoring in the landmark studies were thin (in situ or < 0.75 mm Breslow thickness), supporting the concept that digital monitoring captures melanoma at an early, curable stage.
Clinical Vignettes
Clinical Scenario A 42-year-old woman with a flat, 4 mm melanocytic lesion on her forearm presents for short-term monitoring. At baseline, dermoscopy shows a symmetric reticular pattern without melanoma-specific structures. At the 3-month follow-up, the lesion shows focal darkening in one quadrant and a slight increase in size (approximately 10%). No classic melanoma-specific structures have appeared.
What is the appropriate management?
Management: Excision -- any change at 3 months mandates excision.
Clinical Pearl 3: in short-term monitoring, the rule is absolute. ANY change other than overall solar pigment shifts or milia-like cyst changes mandates excision. There is no "wait and see." The focal darkening and asymmetric size increase constitute morphologic change. Clinical Pearl 2: up to one-third of melanomas discovered by SDDI lack classic dermoscopic features -- without digital monitoring, these would be missed. This is the single most compelling argument for the monitoring protocol, but its safety depends on immediate action when change is detected (Clinical Pearl 11: compliance is a prerequisite for safety).
Clinical Scenario A 55-year-old man with over 80 nevi and melanoma family history undergoes annual long-term surveillance with TBP and SDDI. Comparison of current images with those from 2 years ago reveals one 6 mm lesion on the back has shown symmetric enlargement with uniform darkening. The pattern changed from reticular to reticular-globular with symmetric peripheral globules. No asymmetric features, new colors, or regression structures are present.
What is the appropriate management?
Management: Continue monitoring -- this represents benign nevus evolution.
Clinical Pearl 4: unlike the "any change = excise" rule of short-term monitoring, long-term monitoring requires interpretation. Symmetric enlargement with uniform changes (darkening, globule redistribution) generally does not trigger excision -- these are patterns of benign nevus evolution. The key discriminators for excision in long-term monitoring are asymmetric enlargement, new structures, new colors, and regression features. However, Clinical Pearl 10: peripheral globules are normal in young adults but become rare after the fourth decade. In a 55-year-old, symmetric peripheral globules warrant heightened attention, and the lesion should be monitored at shorter intervals (6 months rather than annually).
Clinical Scenario A 65-year-old woman with a history of melanoma has been monitored with TBP and SDDI. A flat, 5 mm lesion on her right thigh has been stable for 4 years on sequential imaging. At this visit, comparison images show no change in size, structure, or color. However, she reports feeling that the lesion "has changed" and she is concerned.
What is the appropriate management?
Management: Document the patient's concern, perform careful dermoscopy, but the objective stability over 4 years is highly reassuring.
Clinical Pearl 1: "nothing changed" is the most common and most reassuring finding in digital monitoring. The 4-year objective stability documented by TBP and SDDI provides strong evidence against malignancy. Clinical Pearl 8: patients cannot reliably self-detect subtle change (six of eight melanoma patients in the Kittler study were unaware their lesion had changed), but the converse is also true -- subjective concern does not always correlate with objective change. The appropriate response is to take the patient's concern seriously, perform detailed dermoscopy, and compare meticulously with previous images. If no objective change is identified, continue monitoring at the regular interval. Clinical Pearl 9: involution (loss of pigmentation) is a normal biological endpoint and should not be confused with regression, which is an active inflammatory process. Document the patient's concern in the clinical record.
Clinical Scenario
A 70-year-old woman presents with a slowly enlarging pigmented macule on her cheek. Short-term digital monitoring at 3 months shows no definitive change. However, her dermatologist suspects lentigo maligna based on gray perifollicular dots. She asks whether the lack of change at 3 months excludes melanoma.
What is your diagnosis?
Lentigo maligna cannot be excluded -- extend monitoring to 6-12 months or biopsy
Lentigo maligna is the exception to standard short-term monitoring timelines. Only 75% of lentigo maligna will show change within 3 months. When LM is in the differential diagnosis, the follow-up period must be extended to 6-12 months before concluding that the lesion is stable. Alternatively, given the clinical suspicion and the presence of gray perifollicular dots (a feature suspicious for LM), biopsy is a reasonable and potentially preferable option. The decision between extended monitoring and biopsy depends on the clinical certainty, lesion size, and patient factors.
11. Cross-References
| Topic | Reference |
|---|---|
| Sequential digital dermoscopy imaging (SDDI) | Chapter 13, pp. 309--310 |
| Short-term monitoring protocol and results | Chapter 13, pp. 309--310 (Menzies et al. study) |
| Long-term monitoring protocol and results | Chapter 13, pp. 310--311 (Kittler et al. study) |
| Classification of changes table | |
| Natural history of melanocytic nevi | Chapter 13, pp. 311--313 |
| Peripheral rim of globules and age | Chapter 13; Zalaudek et al., 2011 |
| Starburst pattern and Spitz/Reed nevus | Chapter 7e (Spitz nevus) |
| Nevus involution vs regression | Chapter 13, pp. 312--313 |
| Melanoma arising in congenital nevus | Chapter 13 |
| Risks and benefits of follow-up | Chapter 13, pp. 313--314 |
| Key points summary | Chapter 13, p. 314 |
| Slow-growing melanomas | Chapter 13 |
12. Related Modules
| Module | Relevance |
|---|---|
| Module 01: Introduction and Principles | Foundation for understanding dermoscopic image acquisition and interpretation |
| Module 03: Pattern Analysis | Core pattern recognition skills required for change detection |
| Module 04: Two-Step Algorithm | First-level triage (melanocytic vs non-melanocytic) before monitoring decisions |
| Module 05: Prediction Without Pigment | Relevant to featureless melanoma detection |
| Module 06: Chaos and Clues | Complementary diagnostic approach for equivocal lesions |
| Module 07: TADA and Other Algorithms | Alternative algorithmic frameworks applicable during monitoring assessments |
| Module 15: Congenital Nevi | Context for melanoma arising in congenital nevi |
| Modules 21--27: Melanocytic Lesion Differentiation | Essential background on melanoma-specific structures and nevus patterns |
| Module 28: Sensitivity and Specificity | Direct application of diagnostic performance metrics to monitoring protocols; understanding benign-to-malignant biopsy ratios |
Part of the Dermoscopy Educational Course.
Image Sources & Citations
- DERM12345 (Skin Lesion Dataset with 40 Subclasses): DERM12345: A Large-scale Skin Lesion Image Dataset with 40 Subclasses. Figshare. 2023. License: CC-BY-4.0.