Module 31: Special Locations -- Palms and Soles (Volar Surface)
1. Learning Objectives
After completing this module, the learner should be able to:
- Describe the unique microanatomy of volar (glabrous) skin, including the relationship between sulci (furrows), cristae (ridges), crista limitans, crista intermedia, and eccrine ducts, and explain how this anatomy produces the parallel pigment patterns characteristic of acral lesions.
- Differentiate furrows from ridges on dermoscopy using at least three reliable criteria (width, eccrine duct openings, and the ink test).
- Identify and classify the six recognized benign dermoscopic patterns of volar melanocytic lesions: parallel furrow pattern (and its four subtypes), lattice-like pattern, fibrillar pattern, globular pattern, reticular pattern, and homogeneous pattern, as well as the peas-in-a-pod variant and the nontypical (nondescript) pattern.
- Recognize the parallel ridge pattern (PRP) as the hallmark dermoscopic finding of acrolentiginous melanoma (ALM) and explain the histopathologic basis for preferential pigment deposition on ridges in melanoma versus furrows in nevi.
- Apply the BRAAFF checklist to score volar melanocytic lesions and determine which lesions require biopsy.
- Distinguish subcorneal hemorrhage from melanoma on volar skin by recognizing key dermoscopic features such as pebbles on the ridges, abrupt peripheral cutoff, cracks in dried blood, and reddish-rust coloration.
- Identify the dermoscopic features of benign vascular lesions on volar skin, including the double red-dotted parallel ridge pattern, and differentiate them from amelanotic ALM.
- Explain the clinical significance of the Wallace line and the transition pattern seen in melanocytic lesions that cross the junction of glabrous and nonglabrous skin.
2. Prerequisites
- Module 01: Introduction and Principles of Dermoscopy -- understanding of polarized versus nonpolarized dermoscopy, the Tyndall effect, and basic color-to-depth correlations.
- Module 02: Histopathologic Correlations of Dermoscopic Structures -- understanding of how dermal and epidermal structures produce dermoscopic patterns, including the concept of rete ridges.
- Module 03: Pattern Analysis -- familiarity with the principle of global pattern recognition, the distinction between reticular, globular, homogeneous, and structureless patterns, and assessment of symmetry and color distribution.
3. Key Concepts
3.1 Dermatoglyphics and the Origin of Parallel Patterns
Volar skin (palms and soles) possesses a unique microanatomy that produces the individualized dermatoglyphic patterns (fingerprints and footprints) we all carry. This same microanatomy is directly responsible for the characteristic parallel pigment line patterns observed under dermoscopy in melanocytic lesions on these surfaces. Understanding the underlying anatomy is the key to correctly interpreting volar lesion dermoscopy.
3.2 Sulci and Cristae: The Two Parallel Structures
The surface of volar skin consists of alternating:
- Sulci (furrows / sulcus superficialis): The narrow grooves of the dermatoglyphics, approximately 0.2 mm in width.
- Cristae (ridges / crista superficialis): The broader elevated lines, approximately 0.5 mm in width. The eccrine sweat ducts open on the surface of the ridges.
Beneath the surface, two types of rete ridges create these structures:
- Crista limitans: The rete ridge associated with the furrow. Benign melanocytes preferentially localize here.
- Crista intermedia: The rete ridge associated with the ridge. The eccrine duct traverses through this structure. Melanoma cells tend to cluster here during early growth phases.
3.3 The Fundamental Principle of Acral Dermoscopy
The single most important concept in volar dermoscopy is this: In nevi, pigment is preferentially deposited in the furrows; in melanoma, pigment is preferentially deposited on the ridges. This principle underlies all acral dermoscopic pattern analysis and algorithm construction.
3.4 The Wallace Line
The Wallace line is the demarcation boundary separating glabrous (non-hair-bearing) volar skin from nonglabrous (hair-bearing) skin on the hands and feet. Lesions below the Wallace line display parallel line patterns characteristic of volar skin. Lesions above the Wallace line display conventional dermoscopic criteria of nonglabrous skin (e.g., reticular pattern). Melanocytic lesions that straddle the Wallace line frequently display a multicomponent transition pattern combining features of both skin types, which can appear atypical.
4. Core Content
4.1 Anatomy of Volar Skin
A detailed understanding of the histologic microanatomy of volar skin underpins dermoscopic interpretation:
4.1.1 The Tyndall Effect in Volar Skin
In nonglabrous skin, eumelanin pigment located in the upper dermis appears brown, and eumelanin in the lower dermis appears bluish. This is due to the Tyndall effect: melanin appears black when superficial, brown when slightly deeper, and blue when deep within the skin. On volar skin, the stratum corneum is significantly thickened compared with nonglabrous skin. This thickened corneal layer shifts the apparent depth at which pigment sits, which explains why most compound nevi appear brown on nonvolar skin but have a characteristic bluish hue when located on the palms and soles.
4.1.2 Furrows, Ridges, and Their Underlying Rete Ridges
- Furrows (sulcus superficialis) and ridges (crista superficialis) are created by two types of rete ridges:
- The crista limitans corresponds to the furrow.
- The crista intermedia corresponds to the ridge.
- The eccrine duct traverses through the crista intermedia and opens on the surface of the ridge.
- In nevi, melanocytes preferentially localize around the crista limitans and transfer melanin pigment to keratinocytes associated with the furrow. This produces the parallel furrow pattern.
- In early melanoma, melanoma cells tend to cluster around the crista intermedia (where melanocytic stem cells reside near the sweat glands). This produces the parallel ridge pattern.
4.1.3 Differentiating Ridges from Furrows
While differentiating furrows from ridges is usually straightforward, it can occasionally be challenging. Three reliable clues help:
- Width: Ridges are wider (~0.5 mm) than furrows (~0.2 mm).
- Eccrine duct openings: Visible as small white dots evenly distributed along the center of the ridge on dermoscopy.
- The ink test: Apply a felt-tip marker to the skin surface, then wipe off excess ink with an alcohol swab. The ink highlights the ridges and eccrine duct openings, making it straightforward to determine whether the lesion's pigment is on the ridges or in the furrows.
4.1.4 Additional Anatomic Features
- Absence of follicular openings: Volar skin is glabrous (non-hair-bearing), so follicular openings are absent.
- The Wallace line: Lesions below this line show parallel patterns; those above show conventional dermoscopic criteria. Lesions at the junction display a transition pattern with features of both glabrous and nonglabrous skin.
4.2 Dermoscopy of Melanocytic Lesions
flowchart TD
A[Volar Melanocytic<br/>Lesion] --> B{Pigment on Furrows<br/>or Ridges?}
B -->|Furrows| C{Pattern Type?}
B -->|Ridges| D[Parallel Ridge Pattern<br/>-- Suspect Melanoma]
B -->|Both / Diffuse| E{Lesion > 7 mm?}
C -->|Parallel furrow| F[Benign -- Most<br/>Common Nevus Pattern]
C -->|Lattice-like| G[Benign -- Typically<br/>Arch of Foot]
C -->|Fibrillar| H{Type A or B?}
C -->|Globular| I[Benign -- Likely<br/>Congenital Nevus]
C -->|Homogeneous| J[Benign -- Monitor<br/>if > 7 mm]
C -->|Nontypical| K[Evaluate with<br/>BRAAFF Algorithm]
H -->|Type A: Uniform| L[Benign -- Weight-<br/>Bearing Sole]
H -->|Type B: Variable<br/>color/thickness| M[Suspicious --<br/>Consider Biopsy]
D --> N[Apply BRAAFF<br/>Score >= 1: Biopsy]
E -->|Yes| N
E -->|No| K
There is a pervasive myth in medicine that all melanocytic lesions on palms and soles should be excised. This myth may persist because volar nevi are relatively uncommon and because the clinical morphologic features of nevi and early melanoma overlap significantly, making naked-eye differentiation difficult. However, with dermoscopy, it has become relatively straightforward to identify nevi and melanoma based on the preferential localization of pigment in the furrows (nevi) versus the ridges (melanoma).
Occasionally, pigment may be distributed diffusely across both the ridges and furrows without preferential localization, resulting in homogeneous pigmented areas. Such a pattern should raise concern for melanoma, particularly in lesions greater than 7 mm.
Check Your Understanding
What is the most important dermoscopic feature distinguishing benign acral nevi from acral melanoma?
The most important distinguishing feature is the parallel pattern: benign acral nevi show the parallel furrow pattern (pigment follows the sulci/furrows), while acral melanoma shows the parallel ridge pattern (pigment follows the ridges/cristae). This distinction has high sensitivity and specificity for melanoma on acral skin.
Key Takeaways
- The parallel furrow pattern (pigment along dermatoglyphic furrows) is the most common benign acral dermoscopic pattern, corresponding to melanocytes in the crista limitans rete ridges.
- Multiple benign variants exist: classic parallel furrow, lattice-like (furrow lines connected across ridges), and fibrillar (oblique lines from shearing forces).
- The crista dotted pattern (dots on ridges) is a benign variant predominantly seen in children and on the lateral aspects of fingers and toes.
4.3 Benign Dermoscopic Patterns
An important principle to bear in mind before classifying patterns is context: history, skin type, age, and location all factor into the final management decision. Miyazaki et al. demonstrated that the distribution of the three most common benign dermoscopic patterns is not random:
- Lattice-like pattern: Located mainly on the arch of the foot.
- Fibrillar pattern: Located on the weight-bearing parts of the foot.
- Parallel furrow pattern: Located between the arch and weight-bearing portion.
Until further evidence establishes whether patterns located in "atypical" anatomic positions retain the same benign significance, lesions displaying a benign-appearing pattern in the "wrong" location should be managed with caution.
4.3.1 Parallel Furrow Pattern
Description: Linear pigmentation predominantly localized to the furrows. This is the most common benign pattern on volar skin.
Histologic correlate: Melanocytes preferentially located around the crista limitans with melanin columns arranged vertically in the epidermis and stratum corneum.
Four subtypes (variants):
| Subtype | Description |
|---|---|
| Single line | A single continuous line of pigment within the furrow |
| Double line | Two parallel lines of pigment flanking the furrow |
| Single dotted line | A single row of dots within the furrow |
| Double dotted line | Two parallel rows of dots along both sides of the furrow |
Typical locations: Commonly seen on palms or on the sole between the arch and the weight-bearing portion.
Diagnostic clue: The nonpigmented ridges are wider than the pigmented furrows, and white dots (eccrine duct openings) are visible on the ridges.
4.3.2 Lattice-Like Pattern
Description: Similar to the parallel furrow pattern but with the addition of parallel pigment bands that cross over the ridges from one furrow to the next, resembling the rungs of a ladder.
Typical location: The arch area of the sole. This is the most common pattern of nevi found on the arch. It can also be seen on the palms.
4.3.3 Fibrillar Pattern
Description: Multiple thin parallel lines oriented obliquely (tangentially) to the dermatoglyphics, appearing to cross both the furrows and the ridges.
Mechanism: Persistent horizontal pressure applied to the stratum corneum causes it to grow in a slanted direction (in the direction of lateral pressure). As linearly oriented melanin-laden epidermal cells in the stratum granulosum move into the stratum corneum, they travel in an oblique direction, converting a parallel furrow or ridge pattern into a fibrillar pattern.
Typical location: Weight-bearing parts of the sole. The fibrillar pattern is not normally seen on the palms because persistent weight-bearing forces do not occur there.
Critical distinction -- Type A (benign) versus Type B (suspicious):
| Feature | Type A (Benign) | Type B (Suspicious) |
|---|---|---|
| Line thickness | Thin, uniform | Variable, often thicker |
| Color | Light brown, minimal variation | Variable; gray hues (uncommon in nevi) |
| Distribution | Organized, regular | Disorganized |
| Location | Weight-bearing plantar skin | Any location |
Important clinical rule: ANY fibrillar pattern on the palms (regardless of appearance) should raise suspicion for ALM, because constant frictional pressure on the palms does not normally occur.
Oblique-view dermoscopy: A diagnostic technique that can help unmask the underlying pattern (furrow or ridge) hidden by the fibrillar artifact. Viewing the lesion at an oblique angle, or applying downward and horizontal pressure opposite to the normal frictional forces, can transiently convert the fibrillar pattern back into a parallel pattern, revealing whether the pigment originates from the furrows or the ridges.
4.3.4 Globular Pattern
Description: Globules (corresponding to nests of nevomelanocytes of varying sizes) not associated with a parallel pattern. These lesions are presumed to represent congenital nevi.
4.3.5 Reticular Pattern
Description: A well-defined pigment network not associated with the skin markings. This is a nontypical pattern for volar skin but can be seen on the arch of the foot, where nevi usually display a lattice-like pattern.
4.3.6 Homogeneous Pattern
Description: Uniformly distributed pigment involving both the furrows and ridges, devoid of any other dermoscopic structures. Some nevi with a parallel furrow pattern transform over time into a homogeneous pattern. Digital dermoscopy follow-up has shown that some homogeneous-patterned nevi eventually fade away via transepidermal elimination of melanocytes.
Caution: Homogeneous diffuse pigmentation with variable shades of brown in lesions larger than 7-10 mm should raise concern for melanoma.
4.3.7 Peas-in-a-Pod Pattern
Description: A variant of the parallel furrow pattern consisting of parallel furrow lines (in any of the four subtypes) in combination with dots/globules located adjacent to or in the center of the ridges. Sometimes the globules on the ridges are visible but the furrow pigment is not.
Association: Congenital nevi on volar skin.
Additional congenital nevus feature: The "crista dotted pattern" (dots on the ridges) is also commonly seen in congenital nevi.
4.3.8 Nontypical (Nondescript) Pattern
Description: A pattern that cannot be classified into any of the recognized benign patterns and also does not display melanoma-specific patterns. This is an intermediate category.
Management: These lesions require careful evaluation. Context (age, size, location, history) becomes particularly important. The decision to biopsy or monitor depends on additional features such as:
- Maximum diameter (>7 mm is suspicious)
- Asymmetry of color or structure
- Presence of more than two colors
- Blue-white structures, vessels, dots, streaks, or abrupt edges
- Patient age and clinical history

Clinical Scenario
A 58-year-old woman presents with a slowly expanding pigmented macule on her left sole present for 2 years. Dermoscopy reveals diffuse pigmentation following the sulci (furrows) with a lattice-like connection between adjacent furrow lines and uniform brown coloration throughout. No ridge pigmentation is identified.
What is the most likely dermoscopic pattern, and does this lesion require excision?
Lattice-like pattern (benign variant of parallel furrow pattern)
The lattice-like pattern is a recognized benign variant of the parallel furrow pattern in which pigment lines along the sulci are connected by thin bridging lines crossing the ridges, creating a lattice or grid appearance. The key reassuring features are: pigment is confined to the furrows (not the ridges), the pattern is symmetric and regular, and coloration is uniform. This pattern does not require excision but should be documented with dermoscopic photography for baseline comparison, particularly given its location on the weight-bearing sole where the lattice-like pattern is most commonly found.
4.4 Malignant Dermoscopic Patterns on Volar Skin
The malignant dermoscopic patterns on volar skin are extensively covered in Chapter 8d. The key patterns are summarized here.
4.4.1 Parallel Ridge Pattern (PRP)
The hallmark of acrolentiginous melanoma. Linear pigmentation located predominantly on the ridges.
- Specificity: 99%
- Sensitivity: 86%
- Positive predictive value: 84%
Characteristics in melanoma in situ: Typically displays only tan-to-brown lines without other colors or visible structures.
Characteristics in invasive melanoma: Pigmentation on the ridges will rarely be the only feature; additional features such as multiple colors, irregular dots/globules, and streaks are usually present.
Exceptions -- Benign conditions displaying PRP:
- Ethnic pigmentation in darker-skinned patients
- Peutz-Jeghers syndrome
- Laugier-Hunziker syndrome
- Chemotherapy-induced volar pigmentation
- Exogenous dye
- Subcorneal hemorrhage (blood)
- Congenital nevi (occasionally)
4.4.2 Diffuse Pigmentation with Variable Shades of Brown
The second most common pattern in ALM. Structureless diffuse pigmentation involving both ridges and furrows, displaying various shades of brown.
4.4.3 Serrated Pattern
Projections (similar to streaks) at the edge of the tumor, occasionally encountered in ALM.
4.4.4 Atypical Fibrillar Pattern (Type B)
Fibrillar lines with increased variability in color (including gray) and thickness, distributed in a disorganized manner. On the palms, any fibrillar pattern should be considered atypical. On the soles, only the irregular (type B) fibrillar pattern is considered suspicious.
4.4.5 Milky-Red Pattern
Homogeneous reddish/whitish coloring, mainly seen in thicker melanomas with a vascularized nodular component.
4.4.6 Multicomponent Pattern
Multiple patterns present focally within the lesion, including:
- Focal parallel ridge pattern (often at the periphery)
- Structureless diffuse pigmented areas with multiple colors (brown, red, blue-white, black)
- Irregular dots and globules
- Streaks (serrated edge)
- Irregular blotches
- Blue-white veil
- Regression structures
- Atypical vessels
- Abrupt cutoff of pigment at the periphery
4.4.7 ALM with Focal Benign Patterns
Melanoma on volar skin may display patterns associated with nevi (parallel furrow, lattice-like) focally, but the rest of the lesion will display malignant patterns. Malignant patterns trump benign patterns. The entire lesion surface must be searched for malignant features before concluding a lesion is benign.
4.4.8 Size Matters
Most acquired nevi on volar skin are under 7 mm in greatest diameter. Acquired melanocytic lesions on volar skin greater than 7 mm should raise suspicion for melanoma, independently of the dermoscopic pattern.
Check Your Understanding
What variants of the parallel furrow pattern exist, and are they all considered benign?
Variants include the lattice-like pattern (cross-hatched lines in the sulci), the fibrillar pattern (fine oblique parallel lines), and the crista dotted pattern (dots on the ridges with lines in the furrows). All variants are considered benign. The lattice-like pattern is the second most common benign acral pattern after the classic parallel furrow pattern.
4.5 Subcorneal Hemorrhage
Trauma-induced subcorneal blood often presents with a parallel ridge pattern, mimicking melanoma. Understanding the mechanism and distinguishing features is critical.
4.5.1 Mechanism
Blood within the skin tracks along the path of least resistance, which happens to be adjacent to the eccrine duct. Since the eccrine duct opens on the ridge, blood sequesters on the ridges. Initially, blood appears as globular structures ("pebbles on the ridges"). These focal blood spots fuse, resulting in the formation of a parallel ridge pattern.
4.5.2 Color
Depending on the oxidative state of hemoglobin, the pigment may be reddish, bluish, purple, black, brownish, or rust-colored.
4.5.3 Distinguishing Features from Melanoma
| Feature | Subcorneal Hemorrhage | Melanoma |
|---|---|---|
| Peripheral pigment | Ends abruptly at the edge | Tends to fade toward the periphery |
| Cracks | Present (dried blood cracks visible on dermoscopy) | Absent |
| Color | Reddish, rust, or purple hues | Brown to black, may include blue-white |
| Scraping test | Paring down the stratum corneum with a scalpel removes the blood, confirming the diagnosis | Pigment cannot be removed |
| History | Often identifiable trauma | No trauma history, or de novo lesion |
| Morphology | "Pebbles on the ridges" (globular blood spots on ridges) | Linear continuous pigmentation on ridges |
Key Takeaways
- The parallel ridge pattern (pigment on dermatoglyphic ridges) has the highest sensitivity and specificity for acral melanoma of any single dermoscopic criterion.
- Eccrine duct openings (white dots on ridges visible under magnification) help determine whether pigment is on ridges (malignant) or in furrows (benign).
- Any acral lesion showing parallel ridge pattern should be biopsied regardless of size or clinical appearance, as early acral melanoma is often clinically subtle.
4.6 Benign Vascular Lesions on Volar Skin
Angiomas, nevus flammeus, and hemangiomas on volar skin display two recurrent dermoscopic patterns:
- Red dots/globules arranged linearly along each side of the ridge with sparing of the eccrine openings. This produces the double red-dotted parallel ridge pattern, which results from clusters of vessels in the papillary dermis located on both sides of the crista intermedia.
- Regular lacunae situated on the ridges with sparing of the furrows. Red-to-maroon lacunae are diagnostic of angiomas/hemangiomas.
4.6.1 Differentiating Benign Vascular Lesions from Amelanotic ALM
Both benign vascular lesions and amelanotic ALM display red dots (vessels) on the ridges. The key distinction:
- Benign vascular lesions: Red dots/globules are oriented in regular, parallel lines on either side of the ridge (double red-dotted parallel ridge pattern).
- Amelanotic ALM: Vessels are distributed randomly along the ridges, without the regular double-line arrangement.
Check Your Understanding
How should pigmented lesions on the non-glabrous (hairy) portions of the feet and hands be evaluated?
Non-glabrous acral skin (dorsal hands and feet, lateral digits) lacks dermatoglyphics and should be evaluated using standard dermoscopic criteria rather than acral-specific patterns. The parallel ridge/furrow distinction does not apply to these areas. Standard features like pigment network, globules, and streaks should be assessed as on any other body site.
4.7 Lesions with Multiple Benign Patterns
It is not uncommon to encounter nevi on volar skin that manifest more than one benign pattern (e.g., double line furrow pattern on one side and double dotted line furrow pattern on another). Lesions manifesting more than one of the classic benign patterns are classified as benign in the acral diagnostic algorithm. These combination patterns do not indicate malignancy as long as all component patterns are recognized benign variants.
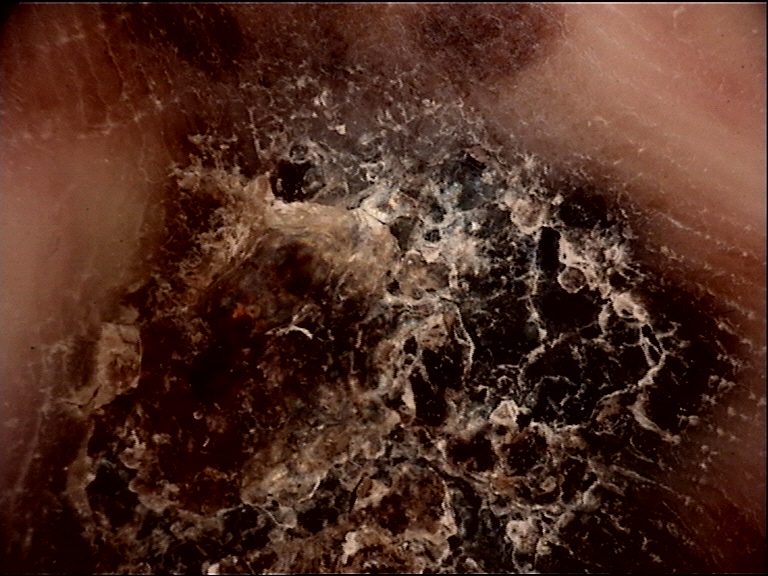
Clinical Scenario
A 62-year-old man presents with a 9 mm pigmented lesion on his right great toe pad that has darkened over the past 6 months. Dermoscopy shows diffuse brown-to-black pigmentation predominantly located on the ridges (sulcus-free areas) with irregular dots and a focal area of blue-white veil. The parallel ridge pattern is clearly identified.
What is the significance of the parallel ridge pattern, and what is the appropriate management?
Acrolentiginous melanoma (parallel ridge pattern)
The parallel ridge pattern (PRP) -- pigmentation located on the ridges of volar skin -- is the dermoscopic hallmark of acrolentiginous melanoma, with a specificity of 99% and sensitivity of 86%. In this case, the PRP is accompanied by additional concerning features: irregular dots/globules and blue-white veil, which indicate an invasive component. Immediate excisional biopsy is mandatory. The additional features beyond simple ridge pigmentation suggest progression beyond melanoma in situ. While benign conditions such as subcorneal hemorrhage or ethnic pigmentation can occasionally produce ridge pigmentation, the combination of PRP with multicomponent features in this clinical context is highly suspicious for ALM.
4.8 The BRAAFF Algorithm for Volar Lesions
The BRAAFF checklist (Lallas et al., 2015) provides a structured scoring system for evaluating volar melanocytic lesions.
4.8.1 Scoring Criteria
Positive criteria (anywhere within the lesion):
| Letter | Criterion | Score |
|---|---|---|
| B | Irregular Blotch | +1 |
| R | Parallel Ridge pattern | +3 |
| A | Asymmetry of structures | +1 |
| A | Asymmetry of colors | +1 |
Negative criteria (anywhere within the lesion):
| Letter | Criterion | Score |
|---|---|---|
| F | Parallel Furrow pattern | -1 |
| F | Fibrillar pattern | -1 |
4.8.2 Interpretation
A total score of 1 or more indicates the lesion should be considered suspicious for acral melanoma and warrants biopsy or referral.
4.8.3 Application Notes
- The parallel ridge pattern carries the highest positive weight (+3), reflecting its strong association with ALM.
- The presence of a parallel furrow pattern or fibrillar pattern provides negative (protective) scores, reflecting their benign associations.
- Context (age, size, location) should still be considered alongside the BRAAFF score.
Key Takeaways
- Subcorneal hemorrhage (blood in the stratum corneum) on acral skin shows red-brown globules that track distally with skin turnover and can be confirmed by dermoscopic follow-up at 2-4 weeks.
- Ethnic/racial melanosis on the soles shows regular parallel furrow pattern bilaterally and does not require biopsy but should be documented for baseline monitoring.
- Pressure-related changes on the soles can distort dermatoglyphic patterns and create pseudoridges; examining the lesion without pressure and comparing with the contralateral foot helps clarify the pattern.
4.9 The 3-Step Acral Algorithm
The comprehensive algorithm for evaluating volar melanocytic lesions follows a stepwise approach:
Step 1 -- Identify the pattern:
- Determine whether the lesion displays a recognizable benign pattern (parallel furrow, lattice-like, typical fibrillar, globular, reticular, homogeneous) or a malignant pattern (parallel ridge, diffuse irregular pigmentation, multicomponent).
Step 2 -- Classify and act:
- Classic benign pattern(s) present: Classify as benign. Multiple benign patterns within one lesion are still benign.
- Classic malignant pattern present: Biopsy/excise. Remember that malignant patterns trump focal benign patterns.
- Nontypical pattern (no classic benign or malignant pattern): Proceed to Step 3.
Step 3 -- Evaluate nontypical lesions by context:
- Lesion diameter greater than 7 mm: Consider biopsy regardless of pattern.
- Lesion diameter 7 mm or less: Evaluate for asymmetry, more than two colors, blue-white structures, vessels, dots, streaks, or abrupt edges. Consider clinical context (age, location, history). If suspicious features are present, biopsy. If absent, consider digital dermoscopy monitoring.
4.10 Acral Melanocytic Nevi: Patterns by Age and Site
The distribution and morphology of acral nevi vary with patient age and anatomic location on the foot:
| Factor | Pattern Association |
|---|---|
| Congenital nevi | Peas-in-a-pod pattern, crista dotted pattern, globular pattern |
| Acquired nevi (typical) | Parallel furrow pattern, lattice-like pattern |
| Arch of foot | Lattice-like pattern most common; reticular pattern occasionally |
| Weight-bearing sole | Fibrillar pattern (type A) most common |
| Between arch and weight-bearing | Parallel furrow pattern most common |
| Palms | Parallel furrow variants; lattice-like |
4.11 Pressure-Related Artifacts
Weight-bearing forces and frictional pressure significantly influence the appearance of acral lesions:
- The fibrillar pattern is itself a pressure artifact: lateral shearing forces on the stratum corneum cause melanin columns to grow obliquely, converting an underlying parallel (furrow or ridge) pattern into a fibrillar pattern.
- Oblique-view dermoscopy can reverse this effect, revealing the true underlying pattern.
- Contact dermoscopy with counter-pressure: Applying downward and horizontal pressure opposite to normal frictional forces can transiently convert the fibrillar pattern back into a parallel pattern.
- "PlayStation purpura" and "black heel" represent pressure-induced subcorneal hemorrhage that mimics the parallel ridge pattern.
4.12 Differential Diagnosis of Pigmented Acral Lesions
Several nonmelanocytic conditions can mimic melanocytic lesions on volar skin:
Subcorneal Hemorrhage (Hematoma)
- Discussed in detail in Section 4.5.
- Key clue: "Pebbles on the ridges," abrupt peripheral cutoff, rust/purple color, cracks, positive scraping test.
Viral Wart (Verruca)
- Dermoscopy: Frog-spawn pattern (thrombosed capillaries appearing as red-black dots within a papillomatous surface), interrupted dermatoglyphics.
- Disruption of normal sulci/cristae pattern distinguishes warts from melanocytic lesions.
Corn/Callus
- Dermoscopy: Homogeneous yellowish structureless area, preservation of dermatoglyphics (unlike warts), absence of melanin pigmentation.
- Central translucent core in corns.
Tinea Nigra
- Dermoscopy: Superficial wispy light brown pigmentation with a spiculated or nondescript pattern that does not follow the furrow-ridge architecture of melanocytic lesions. No parallel furrow or parallel ridge pattern.
- Pigment can be removed with scraping (superficial fungal infection in the stratum corneum).
Drug-Induced (Chemotherapy) Pigmentation
- Dermoscopy: Can display a parallel ridge pattern or diffuse homogeneous pigmentation.
- Clinical context: bilateral involvement, temporal correlation with drug initiation, multiple digits affected.
- Commonly associated with hydroxyurea, cyclophosphamide, doxorubicin, and other chemotherapeutic agents.
Ethnic/Racial Pigmentation
- In darker-skinned individuals, physiologic pigmentation can display a parallel ridge pattern.
- Clinical context: bilateral, symmetric, multiple locations, stable over time.
Laugier-Hunziker Syndrome / Peutz-Jeghers Syndrome
- Can display parallel ridge pattern.
- Clinically: multiple small brownish macules on multiple fingers and/or lips; systemic features in Peutz-Jeghers (GI polyps).
Key Takeaways
- The acral algorithm begins with identifying dermatoglyphic patterns: furrow pattern = benign, ridge pattern = biopsy, irregular/non-pattern = further evaluation.
- Multi-component pattern on acral skin (combining ridge pigment, irregular diffuse pigmentation, and regression) strongly suggests melanoma and warrants complete excision.
- Serial acral dermoscopy is appropriate for benign-pattern lesions but inappropriate for lesions with any ridge pigmentation, irregular diffuse pigmentation, or multi-component features.
5. Acral Pattern Reference Table
| Pattern | Location of Pigment | Significance | Key Features |
|---|---|---|---|
| Parallel furrow | Sulci (furrows) | Benign | Most common benign pattern; 4 subtypes (single line, double line, single dotted, double dotted); white dots (eccrine ducts) on ridges |
| Lattice-like | Sulci + cross-bridges over ridges | Benign | Ladder-rung appearance; most common on arch of foot |
| Fibrillar (Type A) | Oblique lines crossing sulci and cristae | Benign (plantar only) | Thin, uniform, light brown lines; organized; weight-bearing sole only |
| Fibrillar (Type B) | Oblique lines crossing sulci and cristae | Suspicious | Thick, variable color (gray), disorganized; any fibrillar on palms is suspicious |
| Globular | Nests not aligned with dermatoglyphics | Benign | Cobblestone appearance; presumed congenital nevi |
| Reticular | Network not aligned with skin markings | Benign | Seen on arch of foot; nontypical for volar skin |
| Homogeneous | Diffuse across both sulci and cristae | Benign (if <7 mm, uniform) | Uniform light brown; may represent involuting nevi |
| Peas-in-a-pod | Sulci + globules on ridges | Benign | Variant of parallel furrow; associated with congenital nevi |
| Nontypical/nondescript | Variable, unclassifiable | Intermediate | Requires contextual evaluation (age, size, BRAAFF) |
| Parallel ridge pattern | Cristae (ridges) | Malignant (melanoma hallmark) | Eccrine duct openings (white dots) within pigmented bands; 99% specificity for ALM |
| Diffuse irregular pigmentation | Both sulci and cristae | Malignant | Variable shades of brown; >7 mm concerning |
| Multicomponent | Mixed focal patterns | Malignant | Multiple colors, irregular structures, abrupt edges, focal ridge pattern at periphery |
| Subcorneal hemorrhage | Cristae (ridges) | Benign mimic | Pebbles on ridges; reddish/rust/purple; cracks; abrupt cutoff; positive scraping test |
6. Acral Lesion Differential Diagnosis Table
| Condition | Dermoscopic Clues | Key Differentiators |
|---|---|---|
| Acral melanocytic nevus | Parallel furrow, lattice-like, typical fibrillar, globular, peas-in-a-pod | Pigment in furrows; <7 mm; symmetric; benign pattern |
| Acrolentiginous melanoma (in situ) | Parallel ridge pattern (tan-brown lines on ridges) | Eccrine dots within pigmented ridges; unilateral; often >7 mm |
| Acrolentiginous melanoma (invasive) | Multicomponent, diffuse irregular pigmentation, atypical vessels, blue-white veil | Multiple colors; irregular dots/globules; regression; streaks |
| Amelanotic ALM | Random red dots on ridges; atypical vessels (corkscrew); remnants of pigment | Random vessel distribution (not regular double-line pattern) |
| Subcorneal hemorrhage | Parallel ridge pattern; pebbles on ridges; cracks | Abrupt peripheral cutoff; rust/purple color; positive scraping test; history of trauma |
| Benign vascular lesion (angioma/nevus flammeus) | Double red-dotted parallel ridge pattern; regular lacunae on ridges | Regular parallel red dot lines on both sides of ridge; sparing of eccrine openings |
| Viral wart (verruca) | Frog-spawn pattern; thrombosed capillaries; interrupted dermatoglyphics | Disrupted sulci/cristae; papillomatous surface |
| Corn/callus | Homogeneous yellowish structureless area; preserved dermatoglyphics | No melanin pigmentation; central translucent core in corns |
| Tinea nigra | Superficial wispy brown spiculated pigmentation | Does not follow furrow/ridge architecture; removable by scraping |
| Drug-induced pigmentation | Parallel ridge or diffuse homogeneous pattern | Bilateral; multiple digits; temporal correlation with drug use |
| Ethnic/racial pigmentation | May display parallel ridge pattern | Bilateral; symmetric; stable; multiple locations |
| Laugier-Hunziker / Peutz-Jeghers | Parallel ridge pattern | Multiple macules on multiple fingers/lips; systemic features in PJ |
| Congenital nevus (acral) | Peas-in-a-pod; crista dotted; globular; occasionally ridge pattern | Present from birth or early childhood; stable |
7. Clinical Pearls
Furrow versus ridge identification is foundational. Before interpreting any volar lesion, first identify which lines are the furrows and which are the ridges. Use the three clues: width (ridges are wider), eccrine duct openings (white dots on ridges), and the ink test when uncertain.
Pigment in furrows = benign; pigment on ridges = suspect. This is the single most important rule in acral dermoscopy. The parallel ridge pattern has 99% specificity for melanoma.
Any fibrillar pattern on the palms is suspicious. Because persistent weight-bearing forces do not normally act on palms, the fibrillar pattern should not be seen on palms under normal circumstances. Consider this atypical regardless of the pattern's regularity.
Size matters on acral skin. Acquired melanocytic lesions >7 mm in greatest diameter on volar skin should raise suspicion for melanoma regardless of the dermoscopic pattern.
Subcorneal hemorrhage is the most common benign mimic of the parallel ridge pattern. Look for pebbles on the ridges, abrupt peripheral cutoff, cracks, and reddish-rust coloration. When in doubt, pare down the stratum corneum to confirm.
The scraping test is diagnostic for subcorneal hemorrhage. Carefully scraping the corneal layer with a scalpel removes the blood, confirming the diagnosis. This technique does not work for melanin.
Oblique-view dermoscopy can unmask a fibrillar pattern. Viewing a fibrillar lesion at an oblique angle or applying counter-pressure can reveal whether the underlying pattern is a furrow pattern (benign) or a ridge pattern (malignant).
Malignant patterns trump benign patterns. ALM may display focal areas with benign patterns (parallel furrow, lattice-like). Always search the entire lesion for malignant features before concluding benignity.
The transition pattern at the Wallace line is expected, not alarming. Lesions straddling the glabrous/nonglabrous junction naturally display two different pattern types. Recognize this as a normal anatomic transition rather than a sign of multicomponent malignancy.
Congenital nevi on volar skin have distinctive patterns. The peas-in-a-pod pattern (parallel furrow lines + globules on ridges) and the crista dotted pattern are characteristic of congenital nevi. These should not be confused with malignant ridge pigmentation.
Multiple benign patterns in one lesion remain benign. A nevus showing different benign pattern variants in different areas (e.g., parallel furrow on one side, fibrillar on another) is still classified as benign per the acral algorithm.
Context prevents errors with the parallel ridge pattern. Before diagnosing melanoma based on PRP, consider Laugier-Hunziker syndrome (macules on multiple fingers and lips), Peutz-Jeghers syndrome, ethnic pigmentation (bilateral, symmetric), chemotherapy-induced pigmentation (drug history), and subcorneal hemorrhage (trauma history).
Amelanotic ALM versus benign vascular lesions. Both show red dots on ridges. In benign vascular lesions, the dots form a regular double-line pattern flanking each ridge. In amelanotic ALM, the vascular pattern is random and disorganized.
Clinical Vignettes
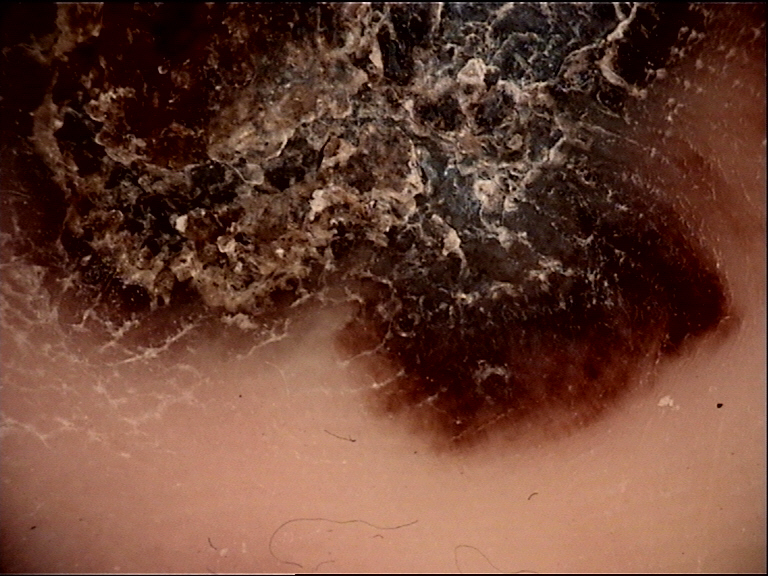
Clinical Scenario A 50-year-old woman presents with a 6 mm pigmented macule on the arch of the right sole. Dermoscopy reveals parallel lines of pigment in the furrows with cross-bridging bands resembling rungs of a ladder. White dots (eccrine duct openings) are on the unpigmented ridges. The pattern is symmetric.
What is the most likely diagnosis?
Diagnosis: Acral melanocytic nevus -- lattice-like pattern.
Pigment is in the furrows, not on the ridges (Clinical Pearl 2: furrows = benign). The lattice-like pattern is a benign variant of the parallel furrow pattern. BRAAFF scores -1 (parallel Furrow: -1). Multiple benign patterns in one lesion remain benign (Clinical Pearl 11 above).
Clinical Scenario A 63-year-old man presents with a 9 mm pigmented macule on the sole that has been darkening. Dermoscopy reveals brown-black bands on the ridges with eccrine duct openings within the pigmented bands. Variable width and color intensity. An irregular dark blotch is present focally.
What is the most likely diagnosis?
Diagnosis: Acrolentiginous melanoma -- parallel ridge pattern.
Pigment on the ridges defines the PRP (99% specificity). BRAAFF: Blotch +1, Ridge +3 = +4 (above threshold of 1). Malignant patterns trump benign patterns (Clinical Pearl 8 above). The PRP alone exceeds the biopsy threshold (Clinical Pearl 7 in Module 24: Acrolentiginous Melanoma). Biopsy is mandatory.
Clinical Scenario A 42-year-old runner presents with a 4 mm brown macule on the ball of the left foot. Dermoscopy reveals fine filamentous lines oriented obliquely to dermatoglyphics, gray in some areas with variable thickness. Oblique-view dermoscopy reveals underlying pigment on the ridges.
What is the most likely diagnosis?
Diagnosis: Suspicious for ALM -- irregular fibrillar pattern masking a parallel ridge pattern.
Gray fibrillar lines are always atypical (Clinical Pearl 4 in Module 24: Acrolentiginous Melanoma). Oblique-view dermoscopy unmasked the underlying PRP (Clinical Pearl 7 above). Despite the small size, gray color and underlying PRP warrant biopsy.
Clinical Scenario
A 58-year-old man presents with a 4 mm pigmented macule on the arch of his left foot. Dermoscopy reveals parallel lines of pigment confined to the sulci (furrows), with white dots (eccrine duct openings) visible on the unpigmented ridges between the pigmented lines. The pigment is uniformly brown with regular spacing.
What is your diagnosis?
Acral melanocytic nevus with parallel furrow pattern
Pigment in the furrows equals benign; pigment on the ridges equals suspect. This lesion shows the parallel furrow pattern -- pigment deposited along the sulci (furrows) -- which is the most common benign pattern on acral skin. The eccrine duct openings (white dots) are located on the ridges, confirming that the pigment is in the furrows, not on the ridges. The uniform brown color and regular spacing are additional reassuring features. Observation is appropriate.
Clinical Scenario
A 42-year-old woman presents with a dark spot on the ball of her right foot that appeared after a long-distance run. Dermoscopy reveals reddish-black globules with smooth margins ("pebbles") distributed along the ridges, with an abrupt peripheral cutoff. The surrounding skin shows preserved dermatoglyphics. The color is rust-red rather than brown.
What is your diagnosis?
Subcorneal hemorrhage (traumatic "black heel" equivalent)
Subcorneal hemorrhage is the most common benign mimic of the parallel ridge pattern. The key distinguishing features are: pebble-like globules on the ridges (rather than continuous linear pigmentation), reddish-rust coloration (rather than brown), abrupt peripheral cutoff, and history of mechanical trauma. The scraping test is diagnostic -- carefully scraping the stratum corneum with a scalpel removes the blood (but does not work for melanin). A rust-colored parallel ridge pattern developing after sports is hemorrhage until proven otherwise.
Clinical Scenario
A 69-year-old woman presents with an 11 mm pigmented macule on her right sole near the heel. Dermoscopy reveals broad brown-black bands along the ridges (parallel ridge pattern) in the center, but at the periphery, there are areas showing a lattice-like pattern with cross-bridging lines. The lesion is irregularly shaped with heterogeneous color.
What is your diagnosis?
Acrolentiginous melanoma
Malignant patterns trump benign patterns. Although the periphery shows a lattice-like pattern (a benign variant), the central parallel ridge pattern is sufficient to classify this lesion as suspicious. ALM may focally display benign patterns, and the entire lesion must be searched for malignant features before concluding benignity. The lesion exceeds the 7 mm safety threshold, and the heterogeneous color adds further concern. The BRAAFF algorithm scores +3 for the parallel ridge pattern alone, exceeding the biopsy threshold. Excisional biopsy is mandatory.
9. Cross-References
| Topic | Chapter Reference | Page(s) |
|---|---|---|
| Anatomy of volar skin (detailed) | Chapter 11b | 253-254 |
| Benign dermoscopic patterns on volar skin | Chapter 11b | 254-258 |
| Malignant patterns on volar skin (comprehensive) | Chapter 8d | 196-201 |
| Parallel ridge pattern (specificity, sensitivity) | Chapter 8d | 196 |
| Diffuse pigmentation with variable brown shades | Chapter 8d | 196 |
| Atypical fibrillar pattern | Chapter 8d | 197 |
| Milky-red pattern | Chapter 8d | 197 |
| Multicomponent pattern | Chapter 8d | 197 |
| BRAAFF algorithm | Chapter 8d | 201 |
| Acral algorithm for volar lesions | Chapter 8d | 201 |
| Subcorneal hemorrhage | Chapter 11b | 259 |
| Benign vascular lesions on volar skin | Chapter 11b | 259-262 |
| Ink test for furrow/ridge identification | Chapter 11b | 254 |
| Wallace line and transition pattern | Chapter 11b | 253-254 |
| Schematic of all acral patterns | Chapter 11b | 256 |
| Nontypical lesion evaluation criteria | Chapter 8d | 197 |
10. Related Modules
| Module | Relevance to This Module |
|---|---|
| Module 24: Acrolentiginous Melanoma | Deep-dive companion covering malignant acral dermoscopic patterns, ALM subtypes (pigmented and amelanotic), staging features, and the full BRAAFF algorithm in clinical context |
| Module 01: Introduction and Principles | Foundational concepts including the Tyndall effect, which explains color shifts on thickened volar skin |
| Module 02: Histopathologic Correlations | Understanding of rete ridges, crista limitans, crista intermedia, and how melanocyte localization produces dermoscopic patterns |
| Module 03: Pattern Analysis | Core pattern recognition skills applicable to the global assessment of volar lesion symmetry, colors, and structures |
| Module 07: TADA and Other Algorithms | The BRAAFF algorithm is one of several specialized algorithms; understanding the general algorithmic approach aids acral lesion evaluation |
| Module 13: Vascular Lesions | Benign vascular lesions on volar skin (angiomas, hemangiomas) and the double red-dotted parallel ridge pattern |
| Module 15: Congenital Nevi | Congenital nevi on volar skin display distinctive patterns (peas-in-a-pod, crista dotted) covered here and in the congenital nevi module |
Module 31 -- Version 1.0 Part of the Dermoscopy Educational Course.
Image Sources & Citations
- DERM12345 (Skin Lesion Dataset with 40 Subclasses): DERM12345: A Large-scale Skin Lesion Image Dataset with 40 Subclasses. Figshare. 2023. License: CC-BY-4.0.