Module 30: Special Locations -- Face
1. Learning Objectives
After completing this module, the learner should be able to:
- Explain why facial skin produces unique dermoscopic patterns that differ from the rest of the body, including the role of attenuated rete ridges, follicular openings, and chronic photodamage.
- Define and recognize the pseudonetwork (annular pattern) on the face and differentiate it from true pigment network seen on non-facial sites.
- Identify the two predominant pigment distribution patterns on the face -- the annular pattern and the reticular (fingerprint) pattern -- and list lesions associated with each.
- Describe the facial melanoma progression model (Schiffner model) and its four stages, from gray dots/granules through annular-granular pattern, angulated lines/rhomboidal structures, to obliterated follicles.
- List and apply the dermoscopic features of lentigo maligna (LM) that distinguish it from its simulators, including gray follicular openings, circle within a circle (isobar sign), asymmetric pigmented follicular openings, and dark structureless areas.
- Differentiate the key melanoma simulators on the face -- pigmented actinic keratosis (AK), lichen planus-like keratosis (LPLK), and pigmented basal cell carcinoma (BCC) -- from lentigo maligna using dermoscopic criteria.
- Recognize the dermoscopic features of common nonmelanocytic facial lesions, including BCC (arborizing vessels, blue-gray ovoid nests), SCC (dotted/glomerular vessels), and sebaceous hyperplasia (crown vessels, yellow-white lobular structures).
- Apply the "seven non-melanoma features" rule and the general management algorithm for pigmented facial lesions to guide clinical decision-making.
2. Prerequisites
- Module 01: Introduction and Principles of Dermoscopy -- understanding of polarized vs. nonpolarized dermoscopy, fundamental colors, and the concept of dermoscopic structures is essential (white shiny structures in facial melanoma are visible only under polarized light).
- Module 02: Histopathologic Correlations of Dermoscopic Structures -- understanding of how rete ridge attenuation, follicular anatomy, and dermal melanin produce specific dermoscopic appearances, including the pseudonetwork concept.
- Module 03: Pattern Analysis -- familiarity with global and local dermoscopic features, symmetry assessment, and the multicomponent pattern is required to evaluate the complex overlapping criteria seen on the face.
3. Key Concepts
3.1 Why Facial Skin Is Different
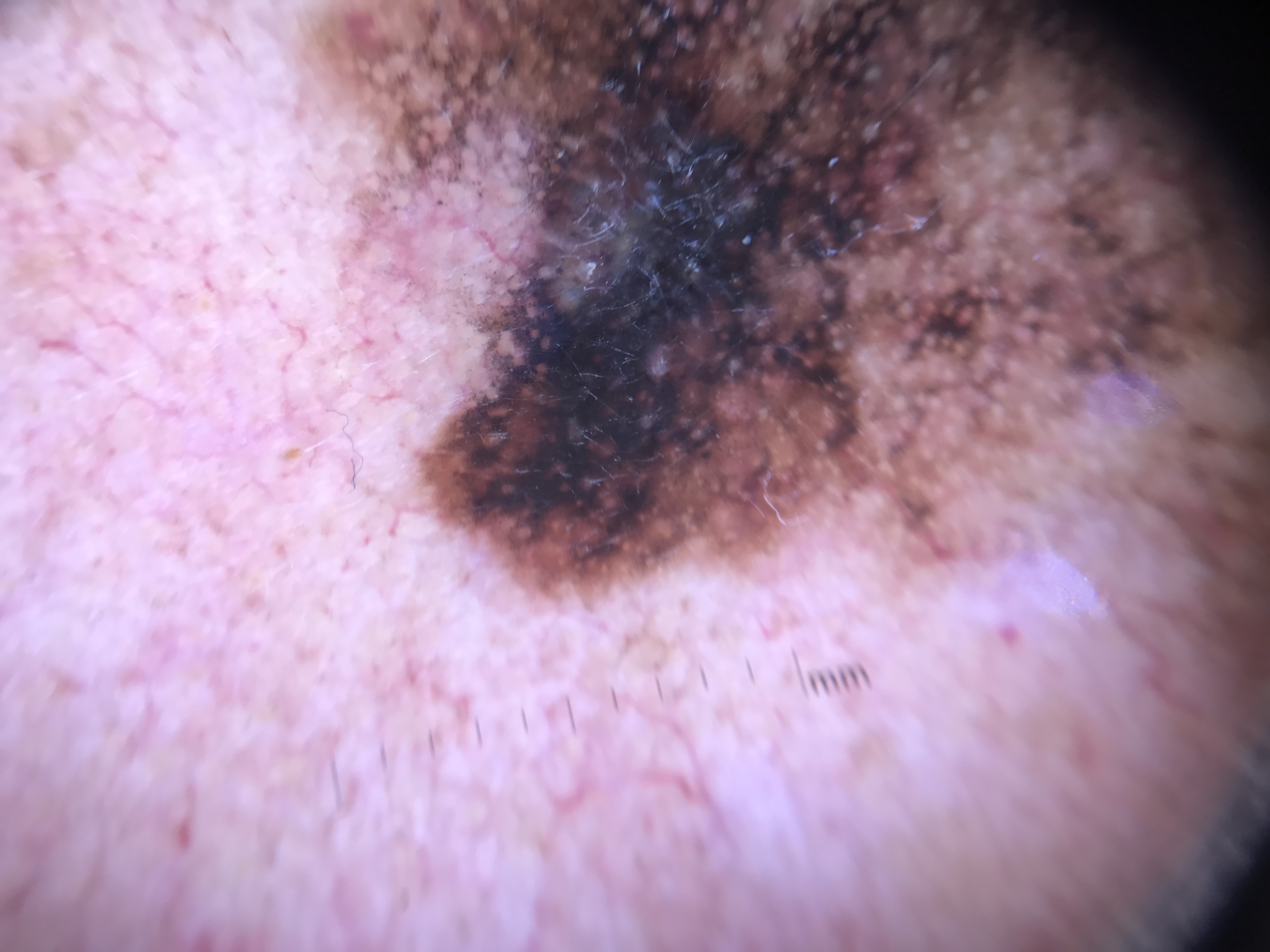
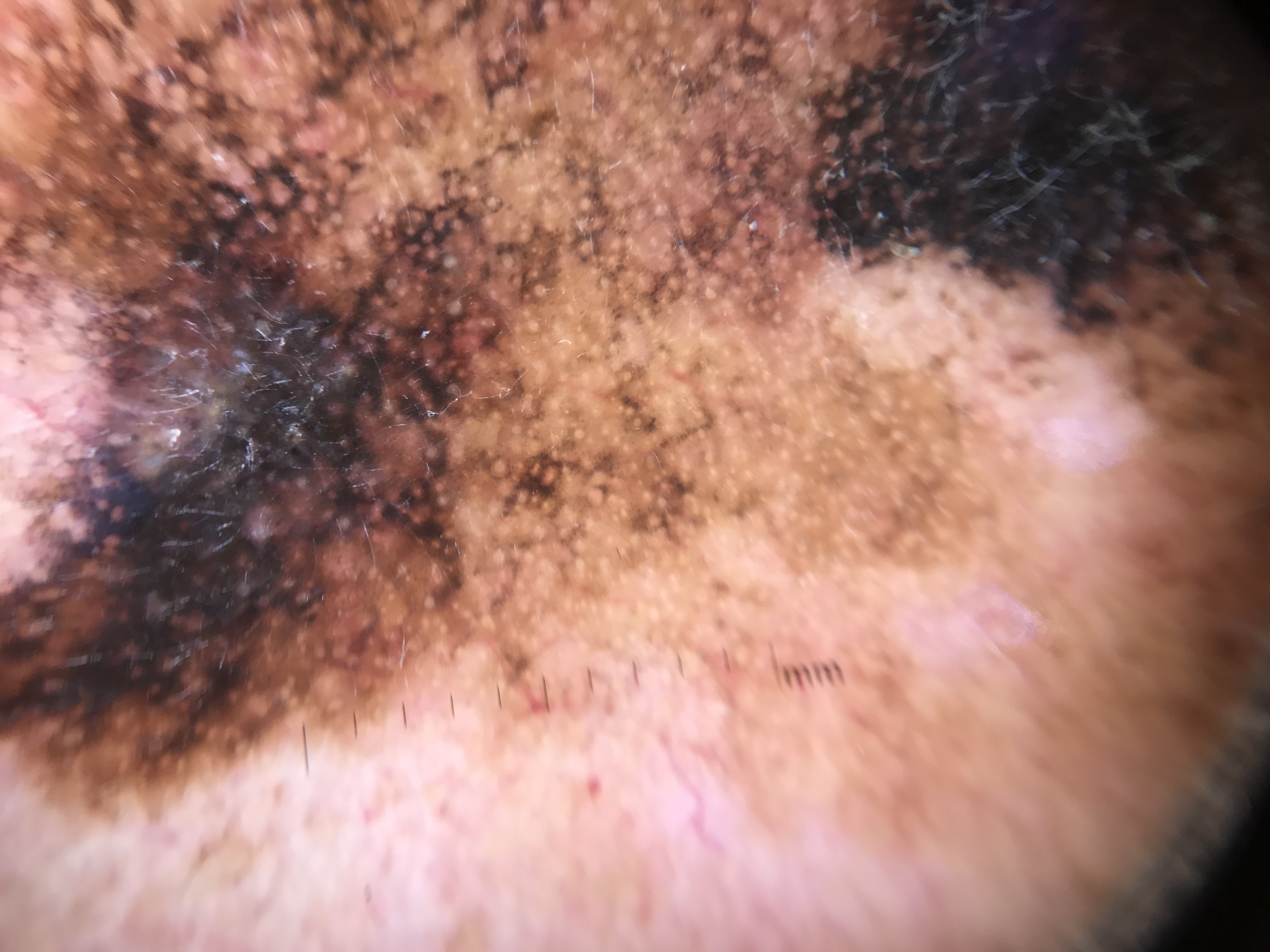
Facial dermoscopy is challenging because the same lesion types produce markedly different dermoscopic patterns on the face compared with other body sites. Two anatomical factors account for this:
- Attenuated rete ridges: Facial skin has inherently flattened rete ridges, and this flattening is compounded by a lifetime of solar exposure causing epidermal thinning. Because the rete ridge pattern is the structural basis of the true pigment network, its absence on the face means that melanocytic lesions do not produce a classic pigment network. Instead, pigment is deposited around adnexal structures (follicles and eccrine glands), creating a pseudonetwork.
- Abundant follicular openings and adnexal structures: The high density of hair follicles and sebaceous glands on the face means that these openings dominate the dermoscopic landscape, producing ring-like or annular patterns around hypopigmented circles that correspond to follicular ostia.
3.2 The Pseudonetwork (Annular Pattern)

The pseudonetwork is the defining dermoscopic feature of facial skin. Unlike the true pigment network (which results from melanin along rete ridges), the pseudonetwork arises because pigment is deposited around follicular openings and eccrine gland ostia, creating a honeycomb-like pattern of small circles surrounded by pigment. Key characteristics:
- Small hypopigmented circles (follicular openings) surrounded by varying amounts of pigment.
- In benign lesions, the circles tend to be uniform in size and shape, with even pigment distribution and relative symmetry.
- In malignant lesions, the circles are of different sizes and shapes, the pigment shows multiple colors, and the pattern is asymmetrical.
3.3 The Two Predominant Facial Patterns

Pigmented lesions on the face manifest one of two predominant patterns:
- Annular pattern: Small circles (follicular openings) surrounded by varying amounts of pigment. Seen in Clark nevi, solar lentigines, early SK, LPLK, pigmented AK, and melanoma in situ.
- Reticular pattern (also called "fingerprinting"): Fine, thin hyperpigmented lines that are short, curved, or interrupted. Most commonly seen in solar lentigines and sometimes in melanoma.
3.4 The Critical Diagnostic Challenge

The most important role of facial dermoscopy is the early diagnosis of melanoma in situ (lentigo maligna) on sun-damaged skin. This diagnosis is made difficult because multiple lesion types -- solar lentigo, SK, LPLK, pigmented AK, and pigmented BCC -- can all mimic melanoma on the face. Mastering the features that distinguish melanoma from its simulators is the central objective of this module.
4. Core Content
4.1 Nonmelanocytic Facial Lesions

The dermoscopic criteria for nonmelanocytic lesions on the face are generally the same as those for nonfacial lesions. The following are the most common nonmelanocytic facial lesions and their key features.
4.1.1 Basal Cell Carcinoma (BCC) on the Face
BCC is the most common skin cancer on the face. Its dermoscopic features on the face mirror those seen elsewhere:
- Absence of a pigmented network -- a critical negative criterion.
- Leaf-like structures (pigmented BCC).
- Multiple nonaggregated blue-gray dots or blue globular structures (pigmented BCC).
- Large blue to blue-gray ovoid nests (pigmented BCC).
- Spoke wheel-like areas or concentric structures (pigmented BCC).
- Arborizing (serpentine or serpentine branched) telangiectasias -- the hallmark vascular pattern of BCC. These vessels are bright red, thick-walled, and sharply in focus.
- Ulceration.
- Pink-white to white shiny areas.
Face-specific note on pigmented BCC: Dark blue BCCs on the face can at times be indistinguishable from thick melanomas. Focal areas within the BCC may reveal characteristic structures (ovoid nests, arborizing vessels, leaf-like areas), making the diagnosis easier. A critical rule: the presence of a pigment network or pseudonetwork (corresponding to ostial openings surrounded by pigment) precludes the diagnosis of pigmented BCC. To diagnose pigmented BCC, at least one of four criteria must be present: spoke wheel-like areas, large gray-blue ovoid nests, arborizing telangiectasias, or leaf-like structures.
4.1.2 Squamous Cell Carcinoma (SCC) on the Face
- Dotted or glomerular vessels -- the key vascular finding.
- Scaling -- frequently associated with SCC, often making it difficult to visualize underlying dermoscopic structures. Removal of surface scale before dermoscopy may reveal additional features.
4.1.3 Sebaceous Hyperplasia
Sebaceous hyperplasia is extremely common on the face and has a distinctive dermoscopic appearance:
- Yellow to yellow-white lobular structures resembling popcorn -- sometimes referred to as the "cumulus sign" due to the lobular, cloud-like appearance.
- Linear winding or serpentine vessels at the periphery of the lesion that radiate toward the center but do not cross the center of the lesion. These vessels are known as "wreath vessels" or "crown vessels" -- a pathognomonic finding.
4.2 Solar Lentigines and Seborrheic Keratoses on the Face
4.2.1 Solar Lentigines
Solar lentigines are among the most common pigmented lesions on the face and have the following dermoscopic features:
- Annular pattern with areas of light brown and dark brown.
- Reticular pattern with fingerprinting and fine interrupted lines.
- Sharp borders.
- Moth-eaten borders -- irregularly scalloped edges where pigment fades or drops out at the periphery.
4.2.2 Seborrheic Keratosis (SK) on the Face
Early SK on the face may show the features of a solar lentigo plus:
- Fine interrupted lines that are often thicker than those seen in solar lentigines.
- Bulbous projections and ridge formation (fat finger-like structures or gyri).
- A few milia-like cysts and/or comedo-like openings.
Mature SK on the face has the same features as on other body sites:
- Sharply demarcated borders.
- Milia-like cysts.
- Comedo-like openings (crypts).
- Fissures (sulci).
- Ridges (gyri) -- together with fissures, these create a cerebriform pattern.
- Hairpin vessels with a white halo.
Check Your Understanding
Why do facial skin lesions require a different dermoscopic approach than lesions on the trunk?
Facial skin has unique anatomy: a flat dermal-epidermal junction (rete ridges are effaced), prominent hair follicles, and sun-damaged background. This means the standard pigment network is absent. Instead, facial lesions display a 'pseudonetwork' -- a pattern of pigment interrupted by follicular openings. Specific facial dermoscopy criteria are needed.
Key Takeaways
- The face lacks a true pigment network due to the flattened DEJ; instead, a pseudonetwork of brown structureless areas interrupted by follicular openings is the normal background.
- All pigmented facial lesions share the pseudonetwork background, making it essential to identify lesion-specific features superimposed on this common pattern.
- The key diagnostic challenge on the face is distinguishing solar lentigo, pigmented AK, lentigo maligna, and flat SK, all of which share the pseudonetwork pattern.
4.3 Facial Melanocytic Nevi
- Flat pigmented lesions (Clark nevi, junctional type) on the face are characterized by an annular pattern -- pigment surrounds the follicular openings in a uniform, symmetrical manner.
- Raised nevi with a prominent dermal component (congenital nevi, compound Clark nevi) take on the same dermoscopic features as similar nevi on other body sites. For example, a dermal nevus with a globular pattern will appear the same on the torso as on the face.

Clinical Scenario
A 78-year-old woman presents with a slowly enlarging brown macule on her left cheek. Among her many facial solar lentigines, this 12 mm lesion stands out as an outlier: it is larger and darker. Dermoscopy reveals asymmetric pigmented follicular openings, gray dots arranged in an annular-granular pattern around follicles, and focal angulated lines forming rhomboidal structures in one area.
What is the diagnosis, and what stage of the Schiffner progression model does this represent?
Lentigo Maligna (Facial Melanoma in Situ)
The combination of asymmetric pigmented follicular openings, annular-granular gray dots, and angulated lines/rhomboidal structures indicates at least Stage 2-3 in the Schiffner facial melanoma progression model. The lesion qualifies as an outlier among her other facial lentigines. Solar lentigines show moth-eaten borders and fingerprinting but NOT gray perifollicular dots or asymmetric follicular openings. The gray color is the most sensitive dermoscopic feature for LM. Biopsy is mandatory.
4.4 Facial Melanoma
4.4.1 Clinical Context
Facial melanomas (predominantly lentigo maligna and lentigo maligna melanoma) are typically found in the elderly in areas with photodamage. The diagnosis is challenging because many other lesions -- pigmented AK, LPLK, and occasionally pigmented BCC -- can simulate melanoma.
4.4.2 The Facial Melanoma Progression Model (Schiffner Model)
A four-stage progression model describes the evolving dermoscopic appearance of melanoma in situ on sun-damaged facial skin:
Stage 1 -- Gray Dots and Granules (Earliest Manifestation)
- The earliest dermoscopic sign of lentigo maligna is slate-gray dots and granules.
- These represent either free melanin or melanin within macrophages (melanophages) in the upper dermis.
- As gray dots accumulate around follicles, the annular-granular pattern forms.
- Short angulated lines (zig-zag pattern) may also appear at this stage.
Stage 2 -- Angulated Lines and Rhomboidal Structures
- Short angulated lines coalesce to form polygonal structures such as rhomboids.
- Perifollicular invasion becomes apparent, with pigment accumulating asymmetrically around follicles.
Stage 3 -- Asymmetric Pigmented Follicular Openings (APFOs)
- As melanoma cells within follicles multiply, asymmetric pigmented follicular openings develop, often with a grayish hue.
- Circle within a circle (isobar sign) can be seen as melanoma cells proliferate along the dermo-epidermal junction within and around follicles.
- Homogeneous dark areas begin to appear, but follicular openings are still preserved (visible).
Stage 4 -- Obliterated Follicular Openings
- Polygonal (rhomboid) structures become thickened.
- Follicular openings are obliterated as the melanoma advances to become invasive.
- Dark structureless areas obscure the follicular openings.
- White scar-like areas may be present, representing regression.
4.4.3 Dermoscopic Features of Facial Melanoma
Global features:
- Asymmetry (of structure and/or color).
- Multiple colors (brown, gray, blue, black, white).
Local features:
- Gray follicular openings -- follicular ostia surrounded by a gray hue rather than the normal tan/brown.
- Irregular gray/brown pigmentation between follicles (perifollicular hyperpigmentation).
- Circle within a circle (isobar sign) -- concentric rings of pigment around follicular openings; when present, highly suggestive of lentigo maligna.
- Slate-gray to blue-gray dots/granules -- the single most sensitive dermoscopic feature for lentigo maligna, though it lacks specificity (also seen in pigmented AK and LPLK).
- Angulated lines and rhomboidal structures -- polygonal lines formed by coalescing angulated lines.
- Dark structureless areas obscuring the follicular openings -- indicates advanced disease with dermal invasion.
- Blue-white veil -- indicates deep melanin and/or dermal fibrosis; suggests invasive melanoma.
- White shiny structures (visible only with polarized light) -- orthogonal shiny white lines (chrysalis structures).
Pattern variants:
- Facial melanoma may present with annular patterns, reticular patterns, or nonspecific patterns.
4.4.4 Amelanotic Melanoma on the Face
Amelanotic melanomas on the face have the same dermoscopic features as amelanotic melanomas on other body sites (e.g., atypical vascular patterns, milky-red areas, regression structures). The reader is referred to the relevant chapters on amelanotic tumors.
Check Your Understanding
What dermoscopic features distinguish benign facial lentigo from lentigo maligna?
Benign facial lentigo shows a uniform moth-eaten border, fingerprint-like structures, and homogeneous light brown pseudonetwork without follicular involvement. Lentigo maligna shows asymmetric pigmented follicular openings, annular-granular pattern (gray dots around follicles), rhomboidal structures, and progressive obliteration of follicles by pigment.
Key Takeaways
- Lentigo maligna shows gray perifollicular dots, asymmetric pigmented follicular openings, and rhomboidal structures that progress to follicular obliteration with advancement.
- Pigmented AK on the face shows a strawberry pattern with yellowish keratotic follicular plugs, scale, and preserved follicular architecture, distinguishing it from LM.
- Solar lentigo shows moth-eaten borders, fingerprinting, and sharply demarcated structureless brown areas without the gray perifollicular features of LM.
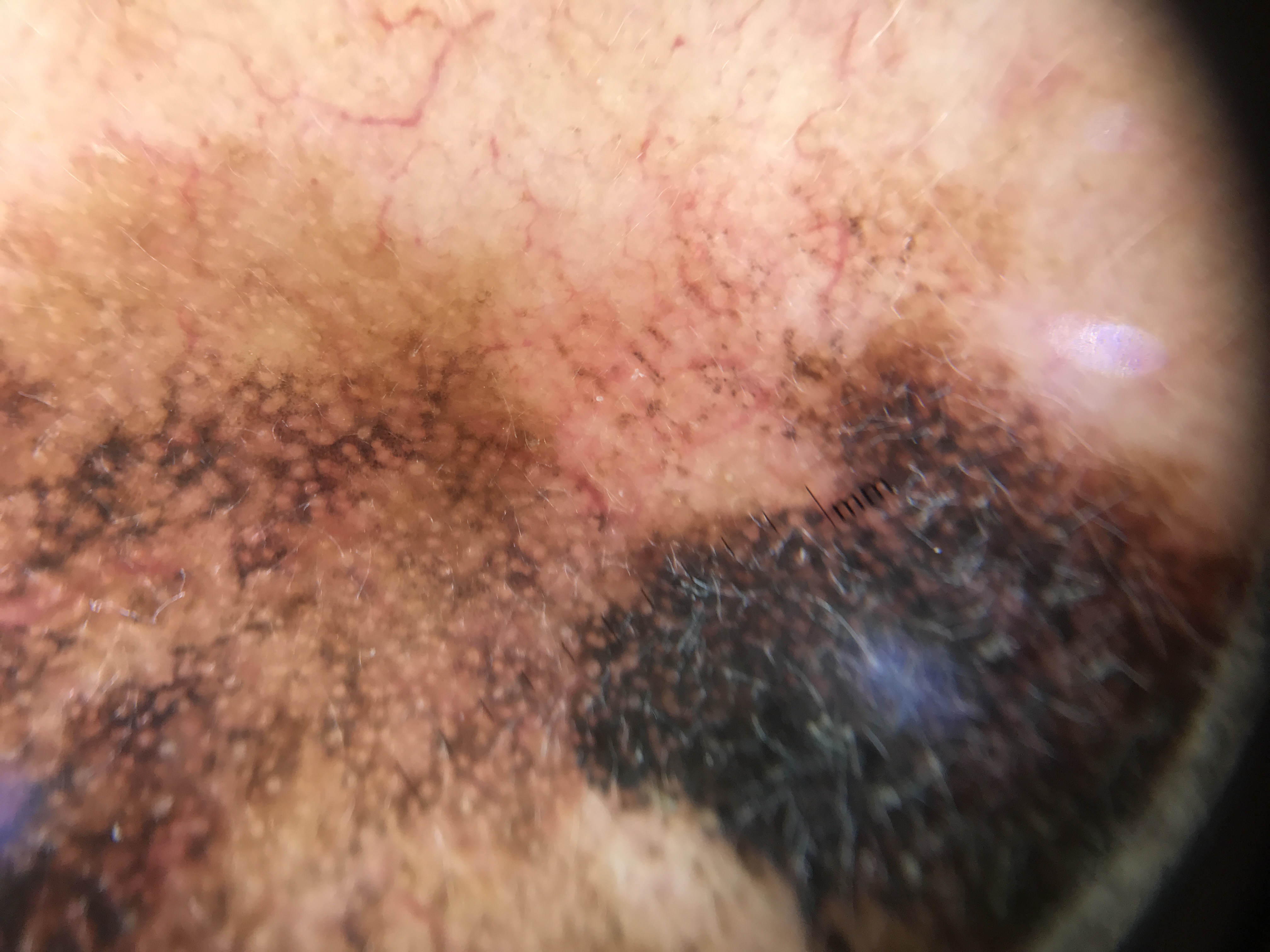
Clinical Scenario
A 70-year-old man presents with a 6 mm pigmented papule on the bridge of his nose. Dermoscopy reveals arborizing bright red vessels in sharp focus, blue-gray ovoid nests, and a few leaf-like structures. There is no pigment network, no gray perifollicular dots, and no follicular obliteration.
What is the diagnosis, and what rules out melanoma on the face?
Pigmented Basal Cell Carcinoma
The sharply focused arborizing vessels, blue-gray ovoid nests, and leaf-like structures are BCC-specific criteria. The absence of a pigment network is a critical negative criterion supporting BCC over a melanocytic lesion. Facial melanoma (LM) would show gray perifollicular dots, asymmetric follicular openings, and angulated lines -- none of which are present. BCC vessels are bright red and sharply in focus, whereas the arborizing vessels sometimes seen in facial Miescher nevi are dull red and out of focus. Biopsy confirms the diagnosis.
4.5 Simulators of Facial Melanoma
The most common facial melanoma simulators include pigmented AK, LPLK, and pigmented BCC.
4.5.1 Pigmented Actinic Keratosis
Pigmented AKs are collision tumors of solar lentigines and AKs. They often share dermoscopic features with melanoma, including asymmetrical pigmented follicular openings, polygonal lines, and gray dots/granules. The helpful clues that favor a diagnosis of pigmented AK over lentigo maligna include:
- Fine scale (clinically palpable rough surface).
- Moth-eaten borders.
- Annular pattern (pseudonetwork with uniform follicular openings).
- Red pseudonetwork (erythema filling the spaces between follicles).
- White circles / white evident follicles -- follicular openings that appear prominently white.
- Rosettes (under polarized light) -- four-dot cloverleaf pattern.
- Inner gray halo -- a gray ring surrounding the follicular opening, inside the perifollicular pigment. Present in 94.1% of pigmented AKs vs. only 23.8% of lentigo maligna (Nascimento et al.). This is one of the most useful differentiating features.
- Scales and red color -- among the most significant findings favoring pigmented AK.
When a clear diagnosis of pigmented AK cannot be made dermoscopically, histopathologic examination should be obtained.
4.5.2 Lichen Planus-Like Keratosis (LPLK) on the Face
LPLK is thought to represent a pre-existing epidermal lesion (usually a solar lentigo or SK) undergoing regression and involution. Two general dermoscopic patterns have been described:
Diffuse granular pattern:
- Brownish-gray, reddish-brown, bluish-gray, or whitish-gray granules distributed throughout the lesion.
Localized granular pattern:
- Granules seen in juxtaposition with dermoscopic features of solar lentigines and SK (fingerprint lines, milia-like cysts, comedo-like openings).
Key differentiating feature -- granule size:
- The granules in LPLK tend to be larger/coarser compared with the blue-gray fine dots seen in melanomas.
- However, multiple blue-gray dots have been found in 45% of invasive melanomas with a specificity of 91% for invasive melanoma.
- If the lesion does not manifest other structures confirming LPLK (such as fingerprint-like lines, milia-like cysts, or comedo-like openings), the diagnosis should be considered uncertain, and biopsy should be contemplated.
- A retrospective study found that coarse granules (not fine peppering) demonstrated a statistically significant association with the diagnosis of LPLK.
4.5.3 Pigmented Basal Cell Carcinoma on the Face
See Section 4.1.1 for full BCC features. Additional points for the differential with melanoma:
- The presence of a pigment network or pseudonetwork precludes pigmented BCC.
- At least one of four criteria must be present to diagnose pigmented BCC: spoke wheel-like areas, large gray-blue ovoid nests, arborizing telangiectasias, or leaf-like structures.
- The clinical importance: the decision to biopsy does not change even if BCC is incorrectly diagnosed as melanoma or vice versa under dermoscopy, because both are malignant and require intervention.
4.6 Circle Within a Circle (Isobar Sign)
The circle within a circle (also called the isobar sign) is a specific dermoscopic finding in which concentric rings of pigment are visible around a follicular opening:
- It results from melanoma cells proliferating along the dermo-epidermal junction within and around the follicular structures.
- It is not commonly seen in lesions overall, but when present, it is highly suggestive of lentigo maligna.
- Reflectance confocal microscopy and en face histopathology have confirmed the correlation between this dermoscopic finding and the pattern of follicular melanocyte proliferation (Navarrete-Dechent et al.).
Check Your Understanding
What is the 'circle within a circle' pattern seen on facial dermoscopy?
The circle-within-a-circle pattern (also called the isobar pattern or target-like pattern) refers to concentric pigmented rings around follicular openings, seen in both lentigo maligna and pigmented actinic keratosis. In lentigo maligna, these circles tend to be asymmetric and gray-brown, whereas in actinic keratosis they are more yellow-brown (follicular plugging).
4.7 The Facial Lesion Management Algorithm
The general rule for evaluating a pigmented facial lesion is to systematically exclude melanoma simulators. The following algorithm is based on the "seven non-melanoma features" approach (Tschandl et al.):
Step 1: Look for features that rule OUT melanoma (non-melanoma features):
| Feature | Associated Diagnosis |
|---|---|
| Scale (fine, palpable) | Actinic keratosis |
| White evident follicles | Actinic keratosis |
| Erythema / red color | Actinic keratosis |
| Reticular or curved lines (fingerprinting) | Solar lentigo |
| Structureless brown color | Solar lentigo |
| Sharp demarcation with or without moth-eaten border | Solar lentigo |
| Classic SK criteria (milia-like cysts, comedo-like openings, fissures/ridges) | Seborrheic keratosis |
Step 2: If none of the above non-melanoma features is the predominant feature, suspect melanoma, especially if any of the following are present:
- Gray color (most sensitive single feature for LM).
- Granularity around follicles (annular-granular pattern).
- Asymmetric pigmented follicular openings.
- Circle within a circle (isobar sign).
- Angulated lines / rhomboidal structures.
- Dark blotches / structureless dark areas.
Step 3: If any portion of the lesion manifests features suggestive of melanoma, even if only focally present, the lesion should be considered a possible melanoma and biopsy should be performed.
Key Takeaways
- Follicular openings provide the most important diagnostic information on the face: preserved with yellow plugs (AK), asymmetrically pigmented (LM), or obliterated (advanced LM).
- Flat facial SK shows sharp demarcation, comedo-like openings, and milia-like cysts superimposed on the pseudonetwork, features not seen in LM or AK.
- When dermoscopy is inconclusive for facial pigmented lesions, reflectance confocal microscopy provides additional cellular-level information that can guide biopsy decisions.
5. Facial Dermoscopy Pattern Reference Table
| Dermoscopic Pattern / Feature | Description | Lesion Association(s) |
|---|---|---|
| Annular pattern (pseudonetwork) | Small hypopigmented circles (follicular openings) surrounded by pigment | Clark nevus, solar lentigo, early SK, LPLK, pigmented AK, melanoma in situ |
| Reticular pattern (fingerprinting) | Fine, thin, short, curved, or interrupted hyperpigmented lines | Solar lentigo, melanoma (less common) |
| Annular-granular pattern | Annular pattern with gray dots/granules around follicles | Lentigo maligna (high suspicion), pigmented AK, LPLK |
| Angulated lines / zig-zag pattern | Short lines at angles to each other | Lentigo maligna (early) |
| Rhomboidal structures | Polygonal shapes formed by coalescing angulated lines | Lentigo maligna (progressive) |
| Asymmetric pigmented follicular openings (APFOs) | Follicles with uneven pigment distribution and grayish hue | Lentigo maligna; also pigmented AK (tan/brown in lentigines) |
| Circle within a circle (isobar sign) | Concentric rings of pigment around follicular openings | Lentigo maligna (highly suggestive when present) |
| Obliterated follicular openings | Follicular openings no longer visible, obscured by dark pigment | Advanced lentigo maligna / lentigo maligna melanoma |
| Gray follicular openings | Follicles surrounded by gray rather than tan/brown pigment | Lentigo maligna |
| Slate-gray to blue-gray dots/granules | Fine granular pigment | Lentigo maligna (most sensitive), pigmented AK, LPLK |
| Coarse granules | Larger granular structures (brownish-gray, bluish-gray, whitish-gray) | LPLK (statistically associated) |
| Inner gray halo | Gray ring within the follicular opening, inside perifollicular pigment | Pigmented AK (94.1%), less common in LM (23.8%) |
| Moth-eaten borders | Irregularly scalloped, fading peripheral pigment | Solar lentigo, pigmented AK |
| Fingerprint-like lines | Fine parallel curved lines resembling fingerprints | Solar lentigo, LPLK |
| Milia-like cysts | White-yellow round structures | SK, LPLK |
| Comedo-like openings (crypts) | Dark round/oval keratin-filled openings | SK, LPLK |
| Fissures and ridges (sulci and gyri) | Brain-like surface pattern | Mature SK (cerebriform pattern) |
| Arborizing telangiectasias | Bright red, sharply focused, thick branching vessels | BCC |
| Blue-gray ovoid nests | Large blue to blue-gray oval aggregates | Pigmented BCC |
| Leaf-like structures | Brown to gray-blue bulbous extensions | Pigmented BCC |
| Spoke wheel-like areas | Radial projections around a central axis | Pigmented BCC |
| Dotted / glomerular vessels | Tiny red dots or coiled vessels | SCC |
| Crown vessels (wreath vessels) | Peripheral serpentine vessels radiating toward but not crossing center | Sebaceous hyperplasia |
| Yellow-white lobular structures | Popcorn-like yellow-white aggregates | Sebaceous hyperplasia |
| Rosettes | Four-dot cloverleaf pattern (polarized light only) | AK, sun-damaged skin |
| White shiny structures | Orthogonal bright white lines (polarized light only) | Melanoma, BCC |
| Blue-white veil | Irregular blue-white overlay | Melanoma (invasive), pigmented BCC |
| White scar-like areas | Structureless white zones | Melanoma regression |
6. Facial Lesion Differential Diagnosis Table
Lentigo Maligna vs. Solar Lentigo vs. Pigmented AK vs. Flat SK
| Feature | Lentigo Maligna (LM) | Solar Lentigo (SL) | Pigmented AK | Flat/Early SK |
|---|---|---|---|---|
| Predominant color | Gray, blue-gray, dark brown, black (multiple colors) | Light brown to dark brown (1-2 colors) | Brown with gray areas and red | Brown, tan |
| Gray color | Present (most sensitive feature) | Absent | May be present (inner gray halo) | Absent |
| Symmetry | Asymmetric (structure and color) | Relatively symmetric | Variable | Symmetric |
| Follicular openings | Asymmetric, gray-hued; may show circle within a circle; eventually obliterated | Uniform, tan/brown | White/evident follicles; inner gray halo (94%) | Uniform, may have keratin plugs |
| Annular-granular pattern | Present (fine gray granules around follicles) | Absent | May be present | Absent |
| Angulated lines / rhomboids | Present (progressive feature) | Absent | May have polygonal lines | Absent |
| Fingerprinting / reticular lines | Less common; if present, irregular | Common; fine, regular | Fingerprinting may be present (from lentigo component) | Thicker lines, interrupted |
| Borders | Irregular, ill-defined | Sharp or moth-eaten | Moth-eaten | Sharp |
| Scale | Absent (smooth surface) | Absent | Present (fine, palpable) | May be present |
| Red pseudonetwork / erythema | Uncommon | Absent | Present | Absent |
| Rosettes | Uncommon | Absent | May be present (polarized light) | Absent |
| Milia-like cysts | Absent | Absent | Absent | May be present (few) |
| Comedo-like openings | Absent | Absent | Absent | May be present (few) |
| Ridges / gyri | Absent | Absent | Absent | May be present (bulbous projections) |
| Blue-white veil | May be present (invasive LMM) | Absent | Absent | Absent |
| White shiny structures | May be present (polarized) | Absent | Absent | Absent |
| Dark structureless areas | Present (advanced) | Absent | Absent | Absent |
| Surface texture (clinical) | Smooth | Smooth | Rough, sandpaper-like | Slightly rough or waxy |
| Management | Biopsy mandatory | Observation or treatment | Biopsy if melanoma cannot be excluded | Observation or treatment |
7. Clinical Pearls
Gray is the alarm color on the face. The presence of gray color is the single most sensitive dermoscopic feature for lentigo maligna. Any gray pigmentation on a facial lesion should raise suspicion and prompt careful evaluation for melanoma criteria.
Evaluate the ENTIRE lesion. If any portion of a facial pigmented lesion manifests features suggestive of melanoma, even if only focally present, the lesion should be considered a possible melanoma. Do not be reassured by benign-appearing areas elsewhere in the same lesion.
The pseudonetwork is not a true pigment network. The annular pattern on the face is produced by pigment deposited around follicular openings, not by melanin along rete ridges. This fundamental distinction explains why facial lesions show different dermoscopic patterns than the same lesion types on the trunk or extremities.
Use the exclusion approach. When confronted with a pigmented facial macule, systematically look for features of non-melanoma diagnoses (scale, white follicles, erythema, sharp borders, fingerprinting, milia-like cysts). Only when these are absent as predominant features should melanoma be suspected.
The inner gray halo distinguishes pigmented AK from LM. The inner gray halo (a gray ring within the follicular opening) is present in approximately 94% of pigmented AKs but only 24% of lentigo maligna -- making it one of the most reliable differentiating features.
Coarse vs. fine granules distinguish LPLK from melanoma. LPLK tends to have larger, coarser granules, whereas melanoma shows fine blue-gray dots. If no additional confirming features of LPLK are present (fingerprint lines, milia-like cysts), biopsy is warranted.
Circle within a circle is rare but highly specific. The isobar sign is not commonly seen in facial lesions, but when present it is strongly suggestive of lentigo maligna and should prompt biopsy.
Obliterated follicles indicate advanced disease. In the Schiffner progression model, follicular openings that are no longer visible (obscured by dark structureless pigment) indicate that the melanoma has progressed beyond the in situ stage. This finding demands urgent biopsy.
Sebaceous hyperplasia has pathognomonic features. Crown vessels (peripheral serpentine vessels that radiate toward but do not cross the center) combined with yellow-white lobular structures make the dermoscopic diagnosis of sebaceous hyperplasia straightforward.
Pigmented BCC and melanoma share blue-white veil. Both can show blue-white veil and blue structures. The key differentiator is that pigmented BCC should NOT have a pigment network or pseudonetwork. Look for at least one of the four BCC-specific criteria (spoke wheel areas, ovoid nests, arborizing vessels, leaf-like structures) to confirm BCC.
Scale favors AK; smoothness favors LM. The tactile quality of the lesion surface is an important clinical adjunct: AK is rough and gritty, while lentigo maligna is smooth to palpation. Always correlate dermoscopic findings with clinical context.
Polarized light reveals additional clues. White shiny structures (chrysalis-like structures) are visible only under polarized dermoscopy and can be present in facial melanomas. Rosettes, visible only under polarized light, are associated with AK and sun-damaged skin.
Clinical Vignettes
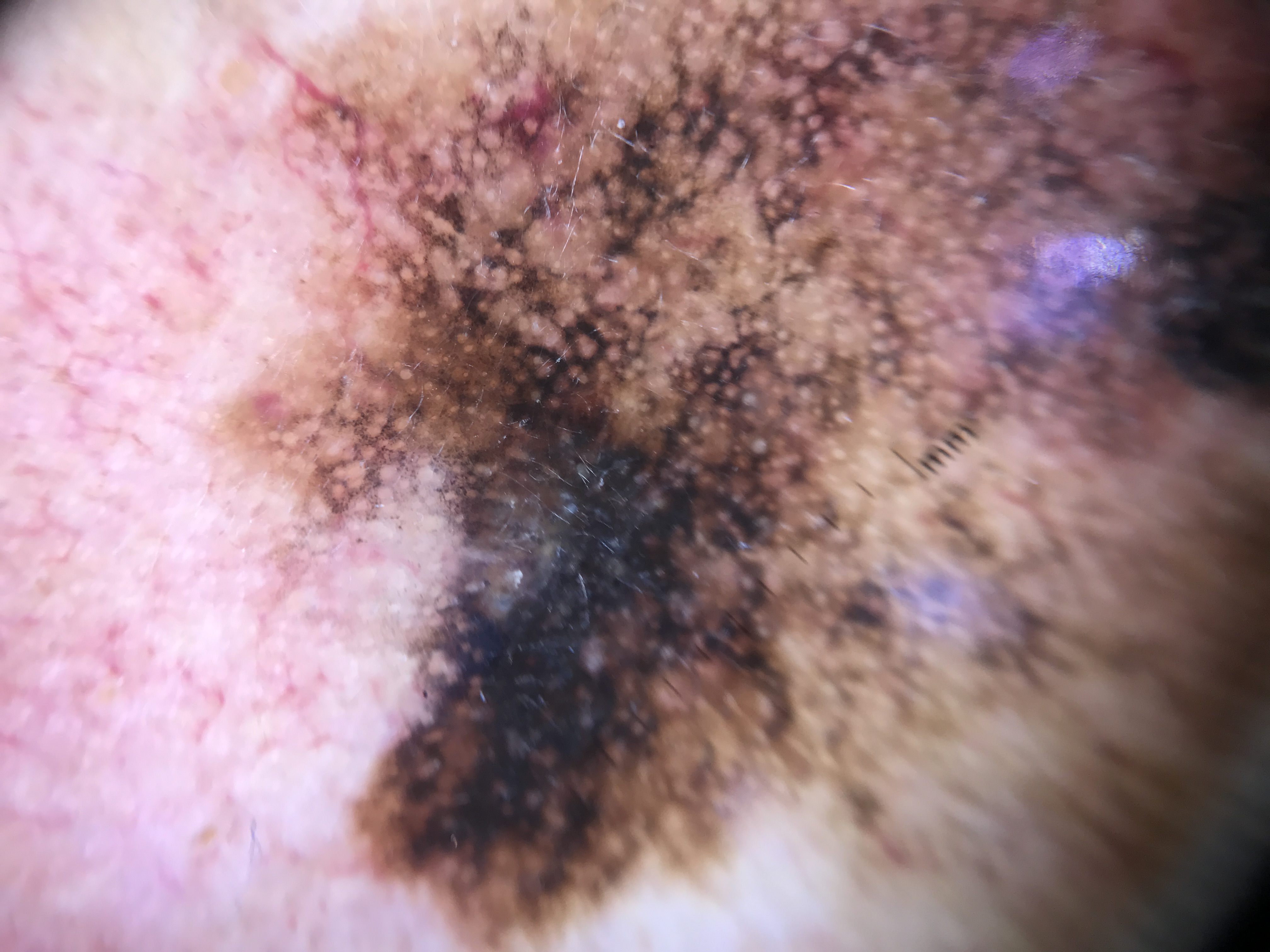
Clinical Scenario A 70-year-old woman presents with a 12 mm brown macule on the left cheek. Dermoscopy reveals small follicular openings surrounded by pigment with gray dots and granules clustered asymmetrically around the follicles. The surface is smooth on palpation.
What is the most likely diagnosis?
Diagnosis: Lentigo maligna.
Gray is the alarm color on the face (Clinical Pearl 1). The asymmetric perifollicular gray pigmentation distinguishes LM from solar lentigo (symmetric, tan-brown). Clinical Pearl 11: smooth texture favors LM over AK. Biopsy is mandatory.
Clinical Scenario A 68-year-old man presents with a 5 mm yellowish papule on the nose with a central depression. Dermoscopy reveals polylobular yellowish-white structures around a central umbilication. Crown vessels radiate toward the center but do not cross the midline.
What is the most likely diagnosis?
Diagnosis: Sebaceous hyperplasia.
Clinical Pearl 9: crown vessels that approach but do not cross the center, combined with yellow-white lobular structures, are pathognomonic. In BCC, arborizing vessels traverse the entire lesion -- this vessel behavior difference is the key differentiator.
Clinical Scenario A 75-year-old man presents with a 7 mm pearly papule on the left alar crease. Dermoscopy reveals bright red, sharply focused arborizing vessels, a small blue-gray ovoid nest, and a leaf-like area. No pigment network or pseudonetwork is visible.
What is the most likely diagnosis?
Diagnosis: Pigmented basal cell carcinoma.
Clinical Pearl 10: pigmented BCC should NOT have a pigment network or pseudonetwork. The BCC-specific criteria (arborizing vessels, ovoid nest, leaf-like areas) confirm the diagnosis. Bright red, sharply focused arborizing vessels distinguish BCC from the dull red, out-of-focus arborizing vessels of dermal nevi.
Clinical Scenario
A 70-year-old woman presents with a slowly enlarging pigmented macule on her left cheek. Dermoscopy reveals multiple follicular openings with asymmetric gray pigment halos, fine gray dots and granules distributed around the follicles (annular-granular pattern), and one area where follicular openings are still visible. No scale, erythema, or fingerprint-like structures are identified. The surface is smooth to palpation.
What is your diagnosis?
Lentigo maligna
Gray is the alarm color on the face. The annular-granular pattern (gray dots and granules around follicular openings) combined with asymmetric perifollicular pigment halos is characteristic of lentigo maligna. The smooth surface texture favors LM over actinic keratosis (which is rough and gritty). The exclusion approach supports this diagnosis: the absence of scale (AK), fingerprinting (solar lentigo), milia-like cysts (SK), and erythema (BCC) leaves LM as the primary consideration. Biopsy is mandatory.
Clinical Scenario
A 65-year-old man presents with a tan macule on his nose. Dermoscopy reveals a brown pseudonetwork with symmetric tan perifollicular openings, an inner gray halo visible within multiple follicular openings, and a rough, sandpaper-like surface texture. No angulated lines or asymmetric features are seen.
What is your diagnosis?
Pigmented actinic keratosis (PAK)
The inner gray halo (a gray ring within the follicular opening) is present in approximately 94% of pigmented AKs but only 24% of lentigo maligna, making it one of the most reliable differentiating features. The rough surface texture (sandpaper quality) further supports AK over LM, which is characteristically smooth. The symmetric perifollicular openings and absence of angulated lines argue against melanoma. Treatment or monitoring is appropriate, but if any doubt persists, biopsy is warranted.
Clinical Scenario
An 80-year-old man presents with multiple yellowish papules on his forehead. Dermoscopy of one lesion reveals peripheral serpentine vessels that radiate toward but do not cross the center (crown vessels), combined with yellow-white lobular structures centrally. No pigment network, gray color, or blue structures are identified.
What is your diagnosis?
Sebaceous hyperplasia
Crown vessels (peripheral serpentine vessels radiating toward but not crossing the center) combined with yellow-white lobular structures are pathognomonic for sebaceous hyperplasia. This dermoscopic pattern is straightforward and virtually diagnostic. The absence of any pigmented structures, gray color, or blue-white veil excludes melanocytic and melanoma-related diagnoses. Multiple lesions on the forehead in an elderly man are consistent with the typical clinical presentation.
9. Cross-References
- Facial skin showing characteristic flattening of rete ridges (histologic correlation of the pseudonetwork).
- Annular pattern examples in solar lentigo, Clark nevus, SK, LPLK, and melanoma in situ.
- Reticular pattern in solar lentigines and melanoma.
- BCC on the face (blue-gray ovoid nests, arborizing vessels, pink-white shiny areas).
- SCC on the face (dotted and glomerular vessels with scale).
- Sebaceous hyperplasia (yellow-white lobular structures and crown vessels).
- Solar lentigines (annular and reticular patterns, moth-eaten borders).
- Mature SK on the face (cerebriform pattern with ridges and fissures).
- Clark nevi junctional type with annular pattern.
- Combined melanocytic nevi with globular homogeneous pattern.
- Schiffner facial melanoma progression model (four stages).
- Progression model stages 1-4 with clinical and dermoscopic images.
- Lentigo maligna melanoma with asymmetry and multiple colors.
- Gray-brown follicular openings in lentigo maligna.
- Irregular perifollicular hyperpigmentation in lentigo maligna.
- Circle within a circle (isobar sign) in lentigo maligna.
- Slate-gray dots/granules, rhomboid structures, and dark structureless areas in lentigo maligna.
- Blue-white veil and white shiny structures in melanoma.
- Facial melanoma patterns (annular, reticular, nonspecific).
- Pigmented AK with fingerprinting, gray dots/granules, and fine scale.
- LPLK with diffuse granular pattern and localized granular pattern.
- Pigmented BCC with blue-white veil, blue ovoid nests, and arborizing vessels.
- Chapter 14: Management algorithm for facial lesions.
10. Related Modules
- Module 01: Introduction and Principles of Dermoscopy -- foundational concepts including polarized vs. nonpolarized dermoscopy, white shiny structures (visible only with polarized light), and rosettes.
- Module 03: Pattern Analysis -- global and local features, multicomponent pattern analysis, and symmetry assessment used for facial lesion evaluation.
- Module 09: Basal Cell Carcinoma -- detailed coverage of BCC dermoscopic features (arborizing vessels, ovoid nests, leaf-like structures, spoke wheel areas) applicable to facial BCC.
- Module 10: Actinic Keratosis -- comprehensive treatment of AK dermoscopy including the strawberry pattern, follicular plugs with halo, rosettes, and the AK grading system; critical background for understanding pigmented AK on the face.
- Module 12: Seborrheic Keratosis and Solar Lentigo -- detailed dermoscopic features of SK (milia-like cysts, comedo-like openings, fissures/ridges) and solar lentigo (fingerprinting, moth-eaten borders) that serve as the comparator lesions for facial melanoma simulators.
- Module 23: Lentigo Maligna -- extended coverage of lentigo maligna dermoscopy, progression models, and management considerations that complement the facial-specific approach presented in this module.
Image Sources & Citations
- DERM12345 (Skin Lesion Dataset with 40 Subclasses): DERM12345: A Large-scale Skin Lesion Image Dataset with 40 Subclasses. Figshare. 2023. License: CC-BY-4.0.