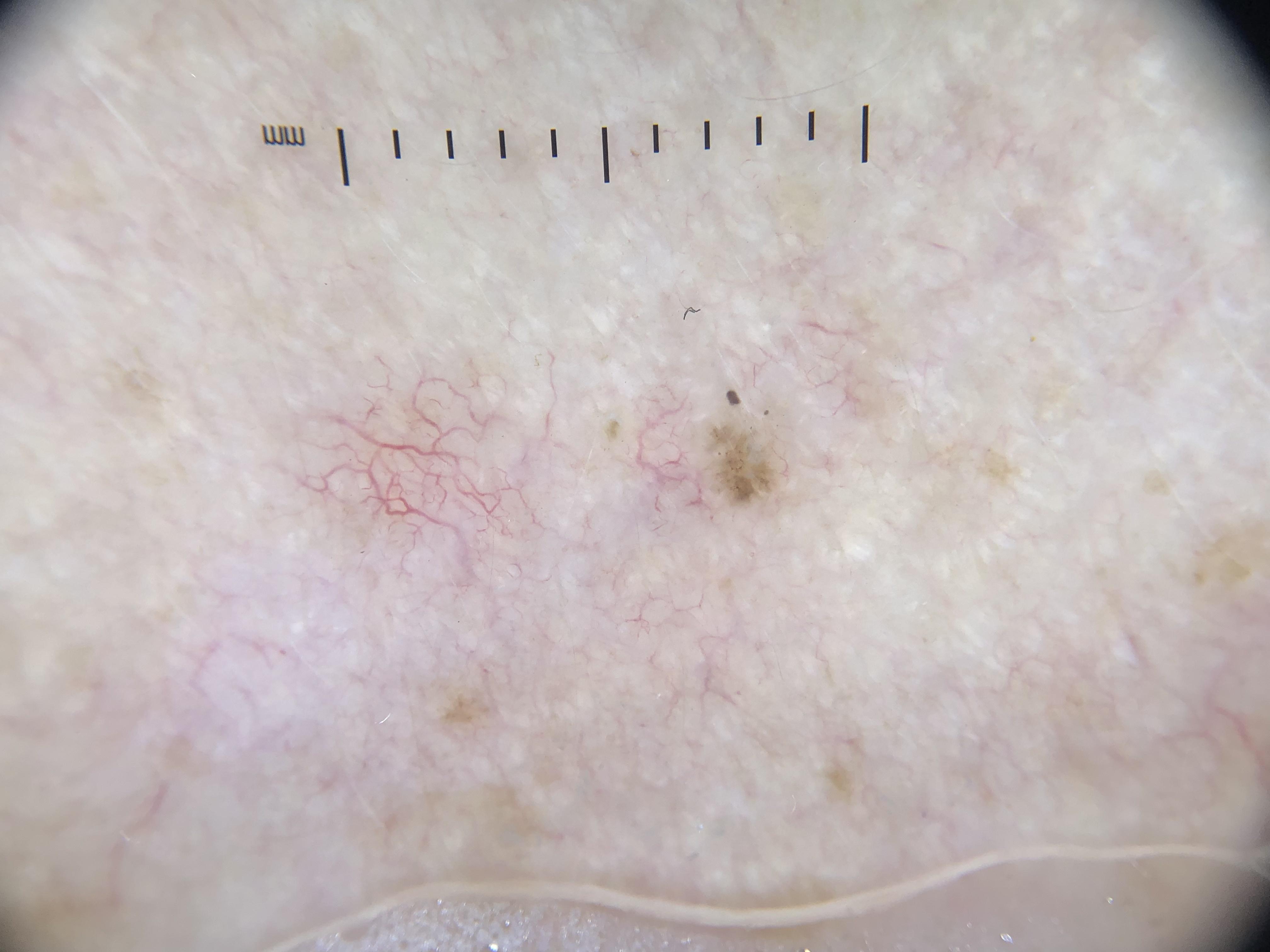
Module 29: Collision Tumors and Exceptions to Rules -- False Positives and False Negatives
Source: Dermoscopy Educational Course Authors: Andrea Combalia, Xavier Fusta, Alicia Barreiro, and Cristina Carrera
1. Learning Objectives
After completing this module, the learner should be able to:
- Define collision tumors and explain why they pose a unique diagnostic challenge in dermoscopy, including the role of anchoring bias and search satisfaction in diagnostic error.
- Identify the common collision tumor combinations (nevus + SK, melanoma + SK, BCC + SK, melanoma + nevus) and describe their typical dermoscopic presentations as bicomponent or multicomponent patterns.
- Distinguish false positive scenarios (benign lesions mimicking malignancy) involving seborrheic keratosis, hemangiomas, dermatofibromas, blue nevi, and acquired/congenital nevi.
- Recognize false negative scenarios (malignancies mimicking benign lesions) including SK-like melanoma, hemangioma-like melanoma, featureless melanoma, and pyogenic granuloma-like melanoma.
- Explain how specific dermoscopic structures normally associated with one diagnosis can appear in another (e.g., globules in clonal SK, milia-like cysts in melanoma, arborizing vessels in melanoma metastasis).
- Differentiate BCC features that mimic melanoma (globules, leaf-like areas, shiny white structures, homogeneous blue pigmentation) from their melanocytic counterparts, and vice versa.
- Apply the concept of nonaccurate skin cancer diagnoses -- understanding when a diagnostic miscall (e.g., BCC called as melanoma) still leads to correct management but impacts diagnostic accuracy.
- Integrate clinical context (patient history, lesion evolution, sun damage, patient age) with dermoscopic findings to override algorithmic decisions when collision tumors or diagnostic exceptions are suspected.
2. Prerequisites
- Module 08: Dermatofibroma -- dermoscopic patterns, variants, and melanoma mimicry
- Module 09: Basal Cell Carcinoma -- BCC-specific criteria (arborizing vessels, blue-gray ovoid nests, leaf-like areas)
- Module 12: Solar Lentigines, Seborrheic Keratoses, and LPLK -- SK criteria (milia-like cysts, comedo-like openings, fissures/ridges)
- Module 13: Vascular Lesions -- hemangioma, angiokeratoma, and pyogenic granuloma dermoscopic features
- Module 15: Congenital Melanocytic Nevi -- congenital nevus patterns and malignant transformation
- Module 16: Acquired Melanocytic Nevi -- acquired nevus patterns and atypical mole syndrome
- Module 18: Blue Nevi and Variants -- homogeneous blue pattern and differential from melanoma
- Module 19: Spitz and Reed Nevi -- spitzoid patterns and melanoma mimicry
- Module 21: Superficial Spreading Melanoma -- atypical network, regression structures, multicomponent pattern
- Module 22: Nodular Melanoma -- blue-black pattern, atypical vessels, rapid growth
- Module 25: Other Melanoma Subtypes -- nevoid, desmoplastic, spitzoid melanoma
- Module 26: Amelanotic and Hypomelanotic Melanoma -- polymorphous vessels, milky-red areas
- Module 27: Differentiation -- Pattern Analysis and Melanoma-Specific Criteria
- Module 28: Improving Sensitivity and Specificity in Melanoma Diagnosis
3. Key Concepts
Collision Tumors
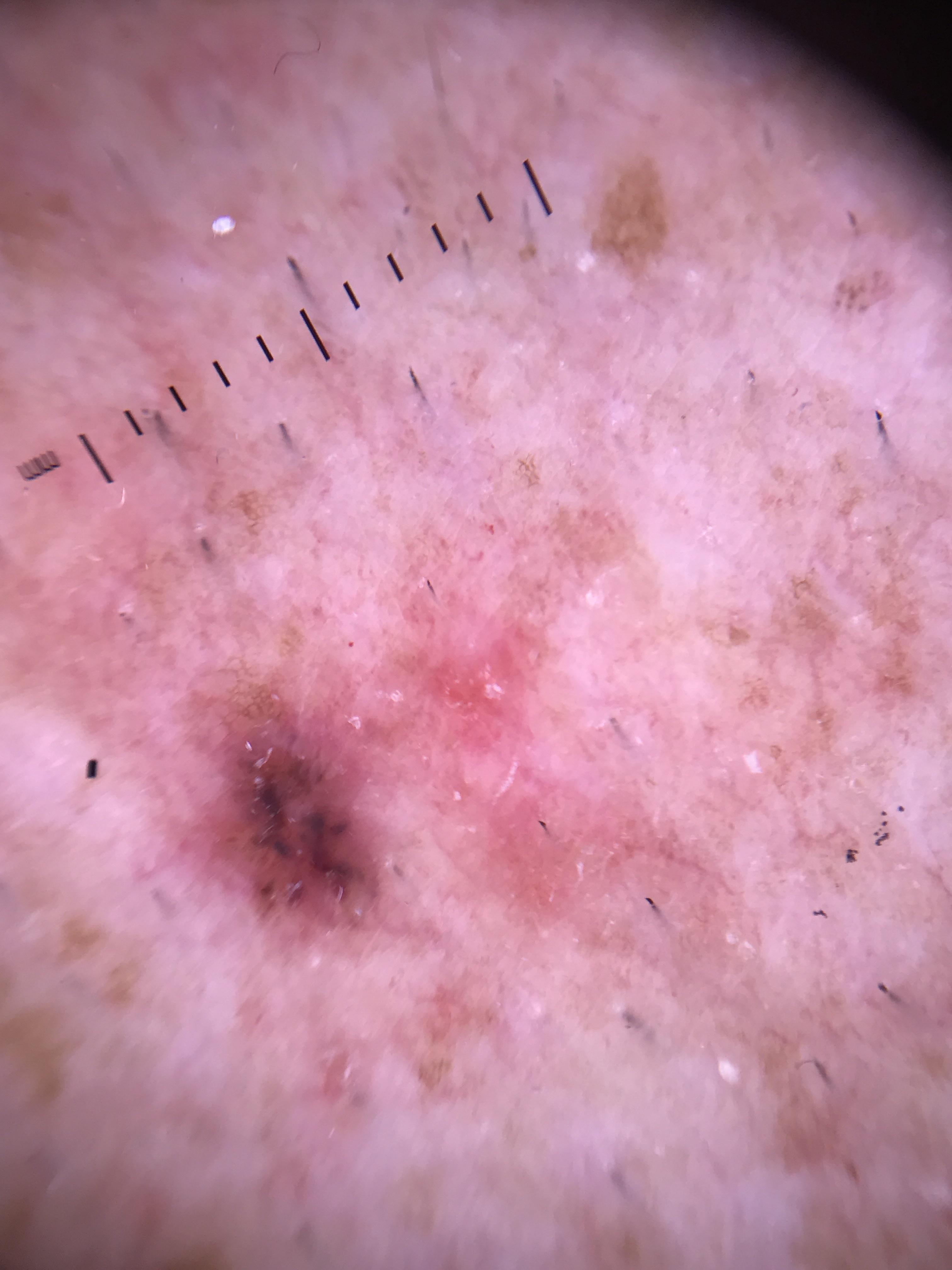
A collision tumor consists of either two different neoplasms that are so close to each other that they clinically appear as a single lesion, or the development of one tumor within and intermingled with another. On dermoscopy, the hallmark is a bicomponent or multicomponent pattern -- two or more distinct sets of dermoscopic criteria recognizable within a single lesion. Collision tumors are frequent, particularly on sun-damaged skin, and seborrheic keratosis is almost always one of the two components.
False Positives
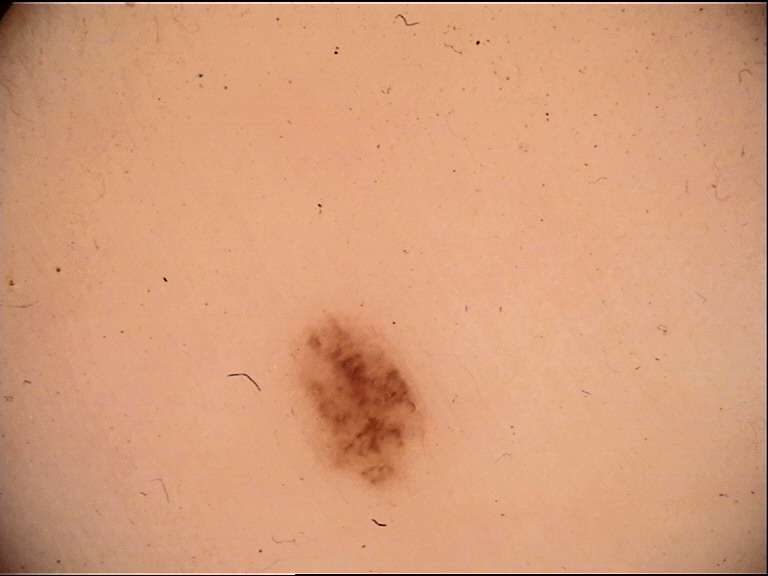
A false positive in dermoscopy refers to a benign lesion that simulates malignancy, leading to unnecessary excision. While this negatively impacts the clinician's benign-to-malignant biopsy ratio, the impact on the individual patient is usually minimal (the lesion is still removed and found to be benign). Examples include irritated SK mimicking amelanotic melanoma, dermatofibromas mimicking melanoma, and hemangiomas mimicking nodular melanoma.
False Negatives
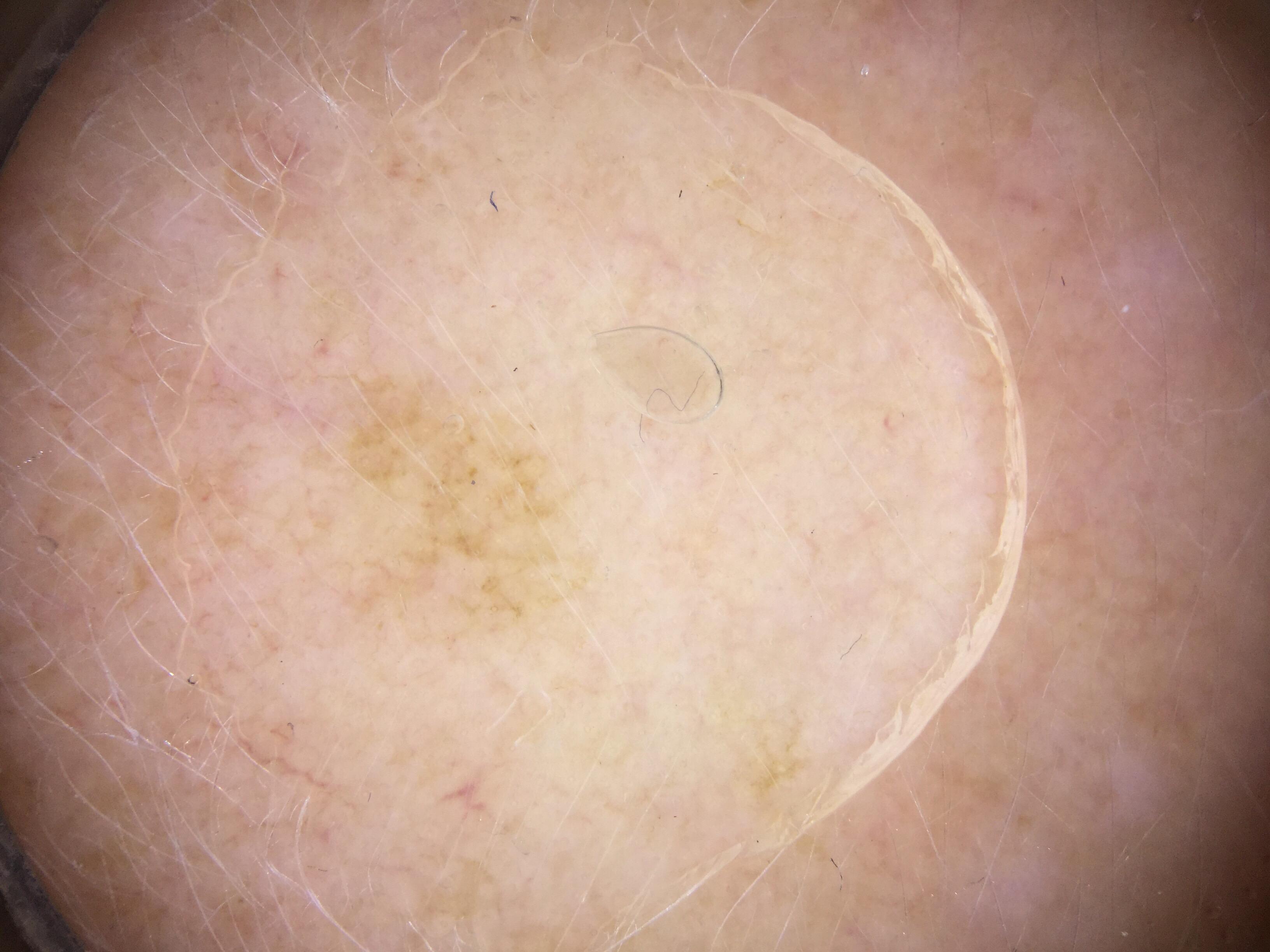
A false negative refers to a malignancy that simulates a benign lesion, potentially leading to delayed diagnosis. This is the more dangerous scenario. While delayed diagnosis of a BCC may not lead to significant negative consequences, a delay in diagnosing melanoma can be catastrophic. Difficult-to-diagnose melanomas include nodular, nevoid, desmoplastic, spitzoid, amelanotic, and lentiginous melanomas on sun-damaged skin.
Nonaccurate Diagnoses

A nonaccurate diagnosis occurs when a skin cancer is correctly identified as malignant but the specific type is miscalled (e.g., BCC diagnosed as melanoma, or vice versa). This lowers diagnostic accuracy but has no impact on management -- the biopsy is performed regardless, and the cancer is diagnosed histopathologically.
Anchoring Bias and Search Satisfaction
Two cognitive errors are central to misdiagnosis of collision tumors:
- Anchoring bias: The clinician anchors the diagnosis on the most conspicuous features first identified (e.g., comedo openings in an SK) and bases the entire diagnosis on these features.
- Search satisfaction: Once the anchoring diagnosis is made, the clinician stops searching for additional features (e.g., a focus of malignancy within the SK), leaving portions of the lesion unevaluated.
Why Dermoscopy Matters
While dermoscopy has significantly improved differentiation between benign and malignant lesions, awareness of its limitations is essential. A combined clinical and dermoscopic approach, supplemented by total body photography and digital dermoscopic monitoring, is necessary to minimize both false positive and false negative diagnoses.
4. Core Content
4.1 Introduction: The Limits of Dermoscopy
Dermoscopy has improved the ability to differentiate benign from malignant lesions, but false positive and false negative cases still occur. These scenarios result in two distinct clinical consequences:
- Unnecessary excisions of benign lesions (false positives)
- Delayed detection of malignant tumors (false negatives)
Three categories of lesions are particularly prone to misdiagnosis:
- Collision tumors: Lesions with features of two or more entities
- Featureless lesions: Malignancies lacking evident dermoscopic features
- Exception lesions: Lesions displaying structures normally associated with a different diagnosis
Awareness of exceptions to the established rules in dermoscopy is essential to improve diagnostic accuracy. Before discussing specific pitfalls, two important principles must be underscored:
- Diagnostic accuracy and management decisions may not be coupled. A BCC misdiagnosed as melanoma still gets biopsied -- the management is correct even though the diagnosis is wrong.
- The consequences of error are asymmetric. False positives (benign mimicking malignant) result in unnecessary biopsies with minimal patient harm. False negatives (malignant mimicking benign) may result in delayed diagnosis of melanoma, with potentially serious consequences.
4.2 Collision Tumors: Definition, Prevalence, and Key Principles
Definition
Collision tumors include either:
- Two different entities so close to each other that they clinically appear as one lesion
- One tumor developing within and intermingled with another
Prevalence and Demographics
- Collision tumors are frequent in clinical practice
- Most commonly found on sun-damaged skin
- SK is almost always involved as one of the two components
- Collisions between SK and melanocytic lesions are found more commonly in younger patients
- Collisions between SK and BCC are found in persons older than 60 years
Dermoscopic Recognition
The dermoscopic evaluation improves identification of both components. During routine examination, clinicians must keep in mind that collision tumors:
- Can be diagnosed easily if suspected -- the key is maintaining awareness
- Present with two or more distinct sets of dermoscopic criteria within one lesion (the bicomponent pattern)
- Rare cases can be challenging when independent dermoscopic criteria are unrecognizable or the features are intermingled
Cognitive Pitfalls in Collision Tumor Diagnosis
The major cognitive errors that lead to misdiagnosis of collision tumors are:
- Anchoring bias: Diagnosis is anchored on the most conspicuous features first identified
- Search satisfaction: The search for features stops once a confident diagnosis is reached
Clinical Example: A lesion with morphologic features consistent with SK. Nonpolarized dermoscopy reveals comedo openings, confirming SK. Search satisfaction occurs when the clinician anchors on the comedo openings and stops searching. With polarized dermoscopy, a focal area reveals shiny white lines -- a feature associated with malignancy. Histopathology proved this to be a BCC of Pinkus arising within a SK.
Check Your Understanding
What is a collision tumor, and how does it appear on dermoscopy?
A collision tumor consists of two or more distinct neoplasms that are contiguous or overlapping but maintain separate histologic identities. On dermoscopy, collision tumors characteristically show two or more distinct dermoscopic patterns within the same lesion, with a relatively sharp demarcation between the different components.
Key Takeaways
- Collision tumors contain two or more distinct neoplasms that have grown together, each maintaining its own dermoscopic features in separate zones of the lesion.
- The most common collision is SK plus melanocytic nevus; recognizing the distinct patterns in different areas prevents misdiagnosis of the combined pattern as melanoma.
- A multicomponent dermoscopic pattern is the hallmark of collision tumors, but the same pattern can indicate melanoma; careful zone-by-zone analysis is essential.
Clinical Scenario
A 73-year-old woman presents with a 14 mm pigmented lesion on her upper back. Dermoscopy reveals two distinct zones: the left half shows comedo-like openings, milia-like cysts, and fissures/ridges (cerebriform pattern), while the right half shows an atypical pigment network with focal blue-white veil and irregular brown-black globules.
What is the diagnosis, and what cognitive error could lead to mismanagement?
Collision Tumor: Seborrheic Keratosis + Melanoma
This lesion demonstrates a bicomponent pattern -- classic SK features in one zone and melanoma-specific features in another. The cognitive error to avoid is anchoring bias: recognizing the SK features first and stopping the examination (search satisfaction error) without evaluating the entire lesion. The melanoma component shows atypical network, blue-white veil, and irregular globules -- all melanoma-specific structures requiring excisional biopsy. Zone-by-zone analysis of the entire lesion is essential when a multicomponent pattern is present.
4.3 Common Collision Tumor Combinations
4.3.1 Nevus + Seborrheic Keratosis
- One of the most common collision combinations in younger patients
- Dermoscopic appearance: One portion of the lesion displays melanocytic features (pigment network, globules), while another portion displays SK features (cerebriform pattern, fissures and ridges, comedo-like openings)
- The upper part shows a heavily pigmented lesion with atypical pigmented network suggesting a melanocytic lesion; the other part shows a cerebriform pattern with fissures and ridges, suggesting SK. Excision confirmed collision between melanocytic nevus and SK.
4.3.2 Melanoma + Seborrheic Keratosis
- Among the most dangerous collision combinations because the SK component may mask the melanoma
- Anchoring bias on SK features (comedo openings, milia-like cysts) may cause the clinician to overlook melanoma-specific features
- Key: Any melanocytic features (atypical network, streaks, blue-whitish veil, irregular globules) within what appears to be an SK should prompt concern
4.3.3 BCC + Seborrheic Keratosis
- Common in patients older than 60 years on sun-damaged skin
- The central part shows an erythematous area with blue-gray ovoid nests and fine in-focus vessels (BCC features), while the periphery shows milia-like cysts, fissures, ridges, and cerebriform pattern (SK features). Excision confirmed collision between BCC and SK.
- The BCC of Pinkus variant may arise within an SK
4.3.4 Melanoma + Nevus
- Melanoma arising within a pre-existing nevus (congenital or acquired)
- The melanoma component may show asymmetric or atypical features arising focally within an otherwise benign-appearing nevus pattern
- Key: Appearance of melanoma-specific structures in a pre-existing nevus -- atypical network, focal negative network, crystalline structures, streaks, irregular blotches, blue-white veil, or regression structures -- should lead to excision
4.3.5 Other Reported Collision Combinations
- BCC + melanocytic nevus
- SCC + SK
- Multiple different benign tumors (e.g., SK + solar lentigo)
- Rare combinations of different malignant tumors
4.4 False Positives: Benign Tumors That Simulate Cancer
Benign lesions mimicking malignancy will be included in the differential diagnosis of melanoma and other pigmented tumors (melanocytic or nonmelanocytic).
4.4.1 Seborrheic Keratosis Mimicking Malignancy
Standard dermoscopic criteria for SK include milia-like cysts, comedo-like openings (pseudofollicular openings), fissures and ridges (cerebriform pattern), light brown fingerprint-like structures, and hairpin vessels. Although the majority of SK can be diagnosed with confidence, a subset of difficult lesions can resemble skin cancer.
Specific SK Variants Mimicking Malignancy:
- Melanoacanthoma
- A rare variant of SK
- Histopathology: deeply pigmented benign proliferation of melanocytes and keratinocytes within a SK
- Can produce intense pigmentation mimicking melanoma
- Inflamed or Irritated SK
- May exhibit irregular and asymmetric vascularization
- Raises differential diagnosis of amelanotic melanoma and SCC
- The inflammatory changes alter the typical SK appearance
- Lichen Planus-Like Keratosis (LPLK)
- A regressing epidermal neoplasm, most frequently a SK or actinic keratosis
- Granularity (peppering) and regression-like features can mimic regressing melanoma
- SK with Melanocytic-Like Structures
a. SK with pigment network-like structures:
- This network-like structure is usually thinner with larger holes and abrupt ending compared with the true pigmented network of melanocytic lesions
- Ink spot lentigo (reticular SK): characterized by a prominent black network with a three-dimensional quality; lines can be thick or thin and end abruptly at the edge of the lesion
b. SK with globule-like structures:
- Clonal SK: a rare variant presenting with nests of basaloid cells resembling globular structures seen in melanocytic lesions
- On dermoscopy: light brown to dark brown/blue globules
- Histopathologic correlate: nests of pigmented basaloid cells within an acanthotic epidermis -- these resemble melanocyte nests and project as globules on dermoscopy, potentially leading to incorrect diagnosis of a melanocytic neoplasm
4.4.2 Hemangiomas Mimicking Malignancy
- Cherry angiomas and angiokeratomas: On occasion, vascular lesions can mimic melanoma, particularly when there are deep or thrombosed vessels that produce dark coloration
- Targetoid hemosiderotic hemangiomas: The hemosiderin-related pigmentation can produce brown-black areas resembling melanoma
4.4.3 Dermatofibroma Mimicking Melanoma
Although dermatofibromas have a high positive predictive value when diagnosed with dermoscopy, some DFs may mimic melanoma. Difficult-to-diagnose DFs may present with additional structures such as shiny white lines and atypical vessels, which are also seen in melanoma.
Key Differentiating Features:
| Feature | Dermatofibroma | Melanoma |
|---|---|---|
| Structure distribution | Shiny white lines and atypical vessels located towards center and over scar-like area | Disorganized pattern with random distribution of structures |
| Scar-like area | Not associated with other regression structures | Often reveals granularity associated with scar-like areas |
| Overall pattern | Organized, predictable structure distribution | More chaotic, disorganized pattern |
Specific DF Variants Mimicking Melanoma:
- Atypical dermatofibromas: May reveal atypical network, atypical scar-like area, negative network, and homogeneous pigmentation, making differentiation from melanoma difficult
- Hemosiderotic and aneurysmal dermatofibromas: Can reveal diffuse or localized homogeneous blue, blue-gray, blue-yellow, or blue-red pigmentation (correlates with siderophages containing hemosiderin and hemosiderin deposition in the dermis)
Additional Clues for Dermatofibroma:
- Palpation: DFs reveal a positive "dimple sign" (central depression when pressed along the margin)
- Peripheral network: Fine, light brown, often associated with ring-like globules located toward the center of the lesion, between the delicate network and the central scar-like area
4.4.4 Adnexal Tumors Mimicking Malignancy
Adnexal tumors can produce dermoscopic features that overlap with melanocytic or other malignant lesions.
4.4.5 Melanocytic Nevi Mimicking Malignancy
- Blue nevus
- Prototypical pattern: homogeneous blue
- On occasion, this homogeneous blue pigmentation can also be seen in nodular melanoma, dermal melanoma, and cutaneous metastasis of melanoma
- Clues to melanoma or metastasis: history of recent changes and/or a previous invasive melanoma; presence of differing shades of blue, pink, crystalline structures, and atypical vessels
- Acquired and congenital nevi
- Early superficial spreading melanomas sometimes lack melanoma-specific structures (featureless melanomas)
- Patients with atypical mole syndrome should be followed with digital monitoring to detect early melanomas without increasing unnecessary excisions
- Warning signs in a congenital nevus: appearance of atypical network, focal negative network, crystalline structures, streaks, irregular blotches, blue-white veil, or regression structures
Check Your Understanding
What are the most common combinations seen in collision tumors?
The most common combinations include nevus + seborrheic keratosis, nevus + BCC, seborrheic keratosis + BCC, melanoma + nevus, and melanoma + seborrheic keratosis. The combination of a melanocytic and non-melanocytic component is the most clinically significant because it can mask malignancy.
Clinical Scenario
A 65-year-old man presents with a 10 mm dark brown papule on his trunk. Dermoscopy shows a cerebriform surface with comedo-like openings and fissures resembling an SK, but focal areas of blue-black pigment are present at the base, along with a few irregular brown globules and loss of the typical "stuck-on" sharp demarcation at one border.
What is the concern, and what dermoscopic clues suggest this is not simply an SK?
Verrucous (SK-Like) Melanoma -- A False Negative Trap
The blue-black pigment at the base (blue-black sign), irregular globules, and loss of the sharp border are features inconsistent with a pure SK. Approximately 50% of verrucous melanomas are initially misdiagnosed as SK. The blue-black sign within an apparent SK should always prompt biopsy. The fissures and comedo-like openings can exist in melanoma (crypts and structures are not exclusive to SK). This case illustrates why every portion of a lesion must be evaluated, and why anchoring on SK-like features without completing the examination is dangerous.
4.5 False Negatives: Skin Cancers That Simulate Benign Lesions
False negatives represent the more dangerous category of diagnostic error because malignant lesions are left undiagnosed, potentially leading to delayed treatment. Difficult-to-diagnose melanomas include nodular, nevoid, desmoplastic, spitzoid, amelanotic, and lentiginous melanomas on sun-damaged skin.
4.5.1 Seborrheic Keratosis-Like Melanoma
Melanomas that simulate SK are dermoscopically challenging. However, critical melanoma features can still be identified if the clinician resists anchoring bias:
Features that allow correct diagnosis despite SK-like appearance:
- Blue and black colors (blue-black sign)
- Pigment network
- Pseudopods or streaks
- Blue-white veil
These features, despite the presence of other SK features (comedo openings, milia-like cysts), should lead to correct identification of the melanoma component.
A hyperkeratotic and pigmented lesion on the face of an 80-year-old male, clinically resembling SK. Dermoscopy revealed obliteration of the facial pseudonetwork, central keratin, and comedo-like openings. Despite the keratinizing surface, the presence of the blue-black sign led to ruling out a benign diagnosis. Pathology confirmed invasive cutaneous melanoma (Breslow depth 0.8 mm).
Critical Warning: Some skin cancers, including melanoma, can reveal milia-like cysts and comedo-like openings. These structures should be ignored during the evaluation of lesions that are considered melanocytic, or until the entire lesion has been completely evaluated. Structures that are easily recognized may produce diagnostic errors such as anchoring bias, where the decision-making process is interrupted once the familiar structure is identified, leaving the rest of the lesion without evaluation.
4.5.2 Hemangioma-Like Melanoma
Rarely, melanomas (primary or metastatic) can clinically and dermoscopically resemble vascular lesions such as hemangiomas and angiokeratomas.
Dermoscopic Features of Hemangioma-Like Melanoma:
- Red to purple ill-defined lacunar-like structures
- Usually in combination with atypical vessels
- Milky-red areas
Differentiating True Vascular Lesions from Melanoma:
| Feature | Cherry Angioma / Angiokeratoma | Hemangioma-Like Melanoma |
|---|---|---|
| Lacunae | Red, dark red, red-blue, or blue-black; well-defined | Red to purple; ill-defined lacunar-like structures |
| Septae | Well-defined septae separating lacunae | Absent or poorly defined |
| Vessels within lacunae | Absent or uniform | Atypical vessels within or around lacunae |
| Milky-red areas | Absent | Present |
| Shiny white structures | Absent | May be present |
Clinical Warning: Clinicians must suspect malignancy in any case of a fast-growing hemangioma-like tumor with atypical vessels within the lacunae, or lacunae-like areas with shiny white and milky-red areas.
A lesion clinically suggestive of capillary hemangioma. Dermoscopy showed ill-defined lacunar-like structures, milky-red areas, and importantly, vessels within the lacunae. The patient had a history of invasive cutaneous melanoma, and this lesion appeared 20 cm from the scar. Biopsy confirmed melanoma metastasis.
4.5.3 Pyogenic Granuloma-Like Melanoma
Despite their characteristic dermoscopic presentation, pyogenic granulomas should always be histopathologically confirmed. Rare amelanotic nodular melanomas and melanoma metastases may have morphology resembling pyogenic granulomas.
4.5.4 Featureless Melanoma
Some cutaneous melanomas may lack any evident dermoscopic features (featureless lesions) to aid in diagnosis. A combined clinical and dermoscopic approach is required for detection:
- Total body photography and digital dermoscopic monitoring have proven to be powerful means for identifying featureless melanomas based on observed changes over time
- Digital monitoring is especially important for patients with the atypical mole syndrome, where early superficial spreading melanomas may not show melanoma-specific structures
4.5.5 Other Difficult-to-Diagnose Melanomas
The following melanoma subtypes are particularly prone to false negative diagnosis:
- Nodular melanoma: May present with a blue-black homogeneous pattern or be amelanotic
- Nevoid melanoma: Closely mimics benign melanocytic nevi
- Desmoplastic melanoma: Often amelanotic, scar-like appearance
- Spitzoid melanoma: Mimics Spitz nevus
- Amelanotic melanoma: Lacks pigmented features; depends on vascular pattern recognition
- Lentiginous melanoma on sun-damaged skin: Facial melanoma with subtle features easily mistaken for benign pigmented changes
Key Takeaways
- Clonal expansion within a single tumor (e.g., melanocytic clones within a SK) can create dermoscopic patterns that mimic collision tumors or melanoma.
- When dermoscopic features from two different lesion types are clearly separated into distinct zones with a sharp border, collision tumor is favored over melanoma.
- Melanoma arising within a nevus (nevus-associated melanoma) is a specific type of collision that shows benign nevus features in one area and melanoma features in another.
4.6 Nonaccurate Skin Cancer Diagnoses: Dermoscopic Diagnoses That Prove Incorrect
Accuracy is established when the dermoscopic diagnosis is shown to be correct. On occasion, skin cancers will be miscalled (e.g., BCC miscalled as melanoma), resulting in lower diagnostic accuracy. However, this miscalling has no impact on the management decision to perform a biopsy, and the skin cancer will be diagnosed.
4.6.1 Basal Cell Carcinoma Mimicking Melanoma (and Vice Versa)
BCC may reveal features that mimic structures seen in melanomas, and vice versa:
Globules:
- In BCC: usually demonstrate a blue-gray color and are not aggregated
- BCCs lack other melanocytic features such as network, aggregated globules, or streaks
- Can simulate globules seen in melanocytic lesions
Leaf-Like Areas vs. Streaks:
- Leaf-like areas (BCC): broader lines that radiate towards the tumor and converge at multiple different focal points, usually at the periphery; each central point is the center of a few lines, resulting in a leaf-like configuration
- Streaks (melanocytic): thinner, centrifugal, and in-focus lines that radiate away from the tumor mass towards normal skin
Shiny White Structures:
- In BCC: appear as blotches and strands, usually more disorganized
- In melanoma: tend to be short lines orthogonally oriented (shiny white lines or crystalline structures)
Homogeneous Blue Pigmentation:
- BCC can present with a large blue ovoid nest occupying almost the entire lesion, simulating a homogeneous blue pattern
- BCC may additionally reveal shiny white blotches and strands, in-focus brown dots, or blue-gray nonaggregated globules
Arborizing Vessels:
- Commonly observed in BCC
- Can also be seen in some melanocytic lesions, including thick melanomas and cutaneous melanoma metastases
4.6.2 Squamous Cell Carcinoma Mimicking Melanoma
Pigmented and nonpigmented SCC can simulate melanoma when specific features are present:
Structureless Lesions:
- Following the two-step algorithm, structureless lesions will be considered melanocytic by default
- These structureless lesions are either monitored using digital dermoscopy (short-term digital monitoring), imaged using confocal microscopy, or biopsied
Brown Dots or Globules in SCC:
- Pigmented SCC can present with focal brown dots or globules that are linearly arranged, often towards the periphery of the lesion
Polymorphous Vessels:
- The clue for any malignant tumor, including melanoma and SCC
- Clinical appearance with keratin in the context of a cancerization field favors SCC
- Any nonspecific tumor with atypical vessels should undergo skin biopsy to rule out malignant skin tumor (angiosarcoma, Merkel cell carcinoma, metastasis, lymphoma)
Check Your Understanding
Why are collision tumors a diagnostic pitfall in dermoscopy, and how should they be managed?
Collision tumors are pitfalls because one component may mask or distract from the other. For example, recognizable seborrheic keratosis features in one portion may cause the clinician to dismiss the entire lesion as benign, missing an adjacent melanoma component. Any lesion with two distinct patterns should be carefully evaluated for malignant features in each component independently. Biopsy should include all components.
4.7 Atypical Presentations and Diagnostic Pitfalls
The Anchoring Bias Problem
The most important pitfall in collision tumor and exception diagnosis is the tendency to:
- Identify the most conspicuous feature first
- Anchor the diagnosis on that feature
- Stop searching (search satisfaction)
- Miss additional features that might change the diagnosis
Structures Crossing Diagnostic Boundaries
Dermoscopic structures have strong associations with specific diagnoses. However, occasionally lesions display structures normally associated with a different diagnosis:
| Structure | Expected Diagnosis | Can Also Be Seen In |
|---|---|---|
| Milia-like cysts | SK | Melanoma, SCC, other malignancies |
| Comedo-like openings | SK | Melanoma, BCC |
| Globules | Melanocytic lesions | Clonal SK (basaloid nests), BCC (blue-gray) |
| Pigment network | Melanocytic lesions | SK (thinner, larger holes, abrupt ending) |
| Arborizing vessels | BCC | Thick melanoma, melanoma metastasis |
| Homogeneous blue | Blue nevus | Nodular melanoma, BCC, metastatic melanoma |
| Lacunae | Hemangioma | Amelanotic melanoma |
When Histopathology Explains the Mimicry
Understanding the histopathologic correlates of misleading structures reveals the cause of misdiagnosis:
- Clonal SK: Nests of pigmented basaloid cells within acanthotic epidermis produce globules on dermoscopy, mimicking melanocyte nests
- Hemosiderotic DF: Siderophages containing hemosiderin and hemosiderin deposition in the dermis produce blue-gray pigmentation mimicking melanoma
- SK with network: Basal layer hyperpigmentation in ridged acanthotic epidermis produces a network-like structure
Key Takeaways
- Any collision lesion containing a component that shows features suspicious for malignancy (atypical network, blue-white veil, irregular vessels) should be completely excised.
- Partial biopsy of a collision tumor risks sampling only the benign component and missing an adjacent malignancy; excisional biopsy is preferred.
- Serial dermoscopy is not appropriate for monitoring collision tumors with suspicious components because the malignant component may be obscured by the benign component.
4.8 When to Override Algorithmic Decisions
The following scenarios should prompt the clinician to override an algorithmic "benign" classification:
- Any lesion with a mixed pattern that includes both benign and malignant features -- biopsy to rule out collision tumor
- Any hemangioma-like lesion that is fast-growing, has atypical vessels within lacunae, or has milky-red areas
- Any pyogenic granuloma -- should always be histopathologically confirmed
- Any SK with blue-black sign, pigment network, pseudopods, streaks, or blue-white veil
- Any homogeneous blue lesion in a patient with history of invasive melanoma (rule out metastasis)
- Any featureless lesion that is new, changing, or in a patient with atypical mole syndrome
- Any lesion where search satisfaction may have occurred -- the clinician should deliberately continue the evaluation beyond the first recognized pattern
- Congenital nevi with new melanoma-specific features -- atypical network, negative network, crystalline structures, streaks, irregular blotches, blue-white veil, or regression structures
4.9 The Role of Clinical Context
Clinical context is indispensable when dermoscopic features are ambiguous:
- Patient age: SK + melanocytic nevus collisions are more common in younger patients; SK + BCC collisions in those older than 60
- Sun-damaged skin: Collision tumors are most frequently found on sun-damaged skin
- Previous melanoma history: A new lesion with homogeneous blue pigmentation or vascular features near a prior melanoma scar should raise suspicion for metastasis
- Lesion evolution: History of recent changes in a blue nevus, or rapid growth of a hemangioma-like lesion, should prompt biopsy
- Anatomic location: Facial location increases risk of lentiginous melanoma on sun-damaged skin being missed
- Digital monitoring: Total body photography and digital dermoscopy are powerful tools for detecting featureless melanomas and early changes in atypical nevi
Key Takeaways
- The differential for collision tumors includes melanoma (multicomponent pattern), combined nevi (different nevus types), and irritated SK with inflammatory changes.
- A key diagnostic clue for collision tumor is the presence of an abrupt transition between two morphologically distinct zones, each with internally consistent features.
- In clinical practice, most suspected collision tumors are excised because the dermoscopic complexity makes confident benign diagnosis difficult.
5. Collision Tumor Types Reference Table
| Collision Combination | Typical Patient Profile | Dermoscopic Appearance | Key Diagnostic Features |
|---|---|---|---|
| Nevus + SK | Younger patients | Bicomponent: melanocytic area (network, globules) adjacent to SK area (cerebriform, comedo openings, fissures/ridges) | Two distinct well-defined zones with recognizable criteria |
| Melanoma + SK | Variable; can occur at any age | SK features in one area (comedo openings, milia-like cysts) with melanoma features in another (atypical network, blue-white veil, blue-black sign, streaks) | Blue-black sign and melanoma-specific structures despite SK features |
| BCC + SK | Older patients (>60 years), sun-damaged skin | BCC area (blue-gray ovoid nests, fine in-focus vessels, arborizing vessels) adjacent to SK area (milia-like cysts, fissures/ridges, cerebriform pattern) | Erythematous focus with BCC structures within or adjacent to SK |
| BCC of Pinkus + SK | Older patients, sun-damaged skin | SK features (comedo openings) with focal shiny white lines (BCC component visible on polarized dermoscopy) | Shiny white lines on polarized dermoscopy within an apparent SK |
| Melanoma + Nevus | Variable; congenital or acquired nevus background | Focal asymmetric features (atypical network, negative network, crystalline structures, streaks, blotches, blue-white veil, regression) arising within an otherwise benign nevus pattern | New or asymmetric melanoma-specific features within pre-existing nevus |
| SK + SK | Older patients, sun-damaged skin | Two SKs in close proximity appearing as one lesion | Both components display SK criteria |
6. False Positive / False Negative Pitfalls Table
Table 6A: False Positives -- Benign Lesions Mimicking Malignancy
| Benign Lesion | Mimicked Malignancy | Misleading Features | Differentiating Clues |
|---|---|---|---|
| Melanoacanthoma (SK variant) | Melanoma | Deeply pigmented, proliferation of melanocytes and keratinocytes | SK architecture present; comedo openings, milia-like cysts still visible |
| Inflamed/Irritated SK | Amelanotic melanoma, SCC | Irregular and asymmetric vascularization | History of irritation; SK features remain identifiable |
| LPLK (lichen planus-like keratosis) | Regressing melanoma | Granularity, regression-like features | Clinical history of regressing SK or AK; no melanoma-specific structures |
| SK with pigment network | Melanocytic neoplasm | Network-like structure | Network is thinner, larger holes, abrupt ending vs. true melanocytic network |
| Ink spot lentigo (reticular SK) | Melanoma | Prominent black network, 3D quality | Lines end abruptly at edge; no melanoma-specific features |
| Clonal SK | Melanocytic neoplasm | Light brown to dark brown/blue globules | Globules represent basaloid nests, not melanocyte nests; SK architecture present |
| Cherry angioma / Angiokeratoma | Melanoma | Deep or thrombosed vessels producing dark coloration | Well-defined lacunae, well-defined septae; no milky-red areas |
| Targetoid hemosiderotic hemangioma | Melanoma | Brown-black hemosiderin pigmentation | Vascular architecture, clinical context |
| Dermatofibroma | Melanoma | Shiny white lines, atypical vessels (especially atypical and hemosiderotic variants) | Central location of structures, positive dimple sign, fine peripheral network, ring-like globules |
| Atypical DF | Melanoma | Atypical network, negative network, homogeneous pigmentation | Positive dimple sign, extremity location, firm papule |
| Hemosiderotic/Aneurysmal DF | Melanoma | Blue, blue-gray, blue-yellow, blue-red homogeneous pigmentation | Peripheral delicate network, dimple sign, hemosiderin-related color |
| Blue nevus | Nodular melanoma, melanoma metastasis | Homogeneous blue pigmentation | Stable lesion, no history of change; absence of differing shades, pink, crystalline structures, atypical vessels |
| Acquired/Congenital nevi | Early melanoma | Features may overlap with featureless melanoma | Digital monitoring recommended; melanoma-specific structures absent |
| Adnexal tumors | Various malignancies | Variable, may overlap with malignant features | Clinical context, histopathologic correlation |
Table 6B: False Negatives -- Malignancies Mimicking Benign Lesions
| Malignancy | Mimicked Benign Lesion | Misleading Features | Clues to Correct Diagnosis |
|---|---|---|---|
| SK-like melanoma | Seborrheic keratosis | Comedo-like openings, milia-like cysts, keratinizing surface | Blue-black sign, pigment network, pseudopods/streaks, blue-white veil (evaluate the ENTIRE lesion) |
| Hemangioma-like melanoma | Hemangioma / Angiokeratoma | Red-purple lacunar-like structures | Ill-defined lacunae, atypical vessels within lacunae, milky-red areas, shiny white structures |
| Pyogenic granuloma-like melanoma | Pyogenic granuloma | Nodular, vascular, rapidly growing | Always biopsy pyogenic granulomas; history of melanoma should raise suspicion |
| Featureless melanoma | Normal skin / Atypical nevus | Lack of any dermoscopic features | Digital monitoring, total body photography, detection of change over time |
| Nodular melanoma | Blue nevus / Hemangioma | Homogeneous pattern, amelanotic | Rapid growth, atypical vessels, ulceration, differing shades, clinical concern |
| Nevoid melanoma | Melanocytic nevus | Nevus-like symmetrical pattern | Subtle asymmetry, clinical change, patient age discordance |
| Desmoplastic melanoma | Scar / Dermatofibroma | Amelanotic, scar-like | Clinical history, location on sun-damaged skin |
| Spitzoid melanoma | Spitz nevus | Starburst or globular pattern | Patient age, asymmetry, clinical evolution |
| Amelanotic melanoma | Dermatofibroma / Inflammatory lesion | No pigmented features | Polymorphous vessels, milky-red areas, shiny white structures |
| Lentiginous melanoma on sun-damaged skin | Solar lentigo / Flat SK | Subtle pigmented changes on face | Asymmetric follicular openings, annular-granular structures, rhomboidal structures |
Table 6C: Nonaccurate Diagnoses -- Skin Cancers Miscalled as Different Cancer Types
| Actual Diagnosis | Miscalled As | Overlapping Features | Impact on Management |
|---|---|---|---|
| BCC | Melanoma | Blue-gray globules, homogeneous blue, shiny white structures | None -- biopsy performed regardless |
| Melanoma | BCC | Arborizing-like vessels in thick melanoma, shiny white blotches | None -- biopsy performed regardless |
| BCC | SCC | Overlap in nonspecific lesions | Minimal -- biopsy performed |
| Pigmented SCC | Melanoma | Brown dots/globules, structureless pigmentation | None -- biopsy performed |
| Melanoma metastasis | Hemangioma | Vascular-appearing structures | Significant if dismissed as benign -- biopsy required |
7. Clinical Pearls
Complete the evaluation -- always. The single most important principle when examining any lesion is to evaluate it in its entirety. Never stop at the first recognized pattern. Anchoring bias and search satisfaction are the primary causes of missed malignancies in collision tumors.
The blue-black sign is your lifeline in SK-like melanomas. The presence of blue and black colors (blue-black sign), pigment network, pseudopods or streaks, and/or blue-white veil allows correct diagnosis of most difficult melanoma cases despite the presence of SK features.
Milia-like cysts and comedo-like openings do not exclude melanoma. Some skin cancers, including melanoma, can reveal these structures. They should be ignored during the evaluation of lesions considered melanocytic, or until the entire lesion has been completely evaluated.
Use both polarized and nonpolarized dermoscopy for collision tumors. The case of BCC of Pinkus arising in SK illustrates that shiny white lines -- visible only with polarized dermoscopy -- can reveal a malignant component hidden within an apparently benign lesion.
Patient age and sun damage predict collision type. SK + melanocytic nevus collisions occur in younger patients; SK + BCC collisions in patients older than 60. On sun-damaged skin, always consider the possibility of a second pathology.
Hemangioma-like lesions with atypical vessels demand biopsy. Any fast-growing hemangioma-like tumor with atypical vessels within lacunae, or lacunae-like areas with shiny white and milky-red areas, should be biopsied to exclude melanoma.
Always biopsy pyogenic granulomas. Despite their characteristic dermoscopic presentation, histopathologic confirmation is mandatory. Rare amelanotic nodular melanomas and melanoma metastases can closely resemble pyogenic granulomas.
Know the differences between BCC and melanoma mimicry. BCC globules are blue-gray and nonaggregated; BCC leaf-like areas radiate toward the tumor (broader, convergent) versus melanocytic streaks that radiate away (thinner, centrifugal); BCC shiny white structures are more disorganized versus melanoma's orthogonally oriented short lines.
A homogeneous blue lesion in a patient with melanoma history is metastasis until proven otherwise. Do not anchor on blue nevus -- check for differing shades, pink areas, crystalline structures, and atypical vessels.
Digital monitoring is essential for featureless melanomas. Total body photography and digital dermoscopic monitoring are the most powerful tools for detecting melanomas that lack any dermoscopic features, based on observed changes over time.
Nonaccurate diagnosis is not always harmful. A BCC miscalled as melanoma will lower diagnostic accuracy but not affect management (biopsy is performed regardless). Do not let the quest for a specific diagnosis prevent appropriate management.
When in doubt, biopsy. For any lesion where collision tumor, false negative, or diagnostic exception is suspected, the appropriate management is histopathologic evaluation. The cost of an unnecessary biopsy is far less than the cost of a missed melanoma.
Clinical Vignettes
Clinical Scenario A 72-year-old man presents with a 15 mm lesion on his sun-damaged forehead. Nonpolarized dermoscopy reveals comedo-like openings and a cerebriform surface consistent with SK. On closer inspection with polarized dermoscopy, one area at the edge shows a subtle gray pseudonetwork with asymmetric perifollicular gray dots not explained by the SK pattern.
What is the most likely diagnosis?
Diagnosis: Collision tumor -- seborrheic keratosis with adjacent lentigo maligna.
This illustrates "satisfaction of search" -- finding one diagnosis and stopping. SK features can coexist with or mask melanoma. Clinical Pearl 3: milia-like cysts and comedo-like openings do not exclude melanoma. Always evaluate the ENTIRE lesion (Clinical Pearl 1).
Clinical Scenario A 65-year-old woman presents with an 8 mm lesion on the left leg. Dermoscopy reveals two distinct zones: the right half shows irregular pigment network with atypical dots, while the left half shows blue-gray ovoid nests, spoke wheel areas, and arborizing vessels. A clear demarcation line separates the two zones.
What is the most likely diagnosis?
Diagnosis: Collision tumor -- melanocytic lesion colliding with basal cell carcinoma.
Two distinct dermoscopic halves represent two neoplasms. Clinical Pearl 8: BCC globules are blue-gray and nonaggregated; BCC structures converge toward the tumor while melanocytic streaks radiate centrifugally. Biopsy must be sufficiently large to sample both components (Clinical Pearl 12).
Clinical Scenario A 58-year-old man with melanoma history presents with a new 5 mm blue-purple papule on the right upper arm that he assumes is a cherry angioma. Dermoscopy reveals a homogeneous blue area with a subtle pinkish zone containing small irregular vessels at one edge. No lacunae or fibrous septae are seen.
What is the most likely diagnosis?
Diagnosis: Must rule out melanoma metastasis.
Clinical Pearl 9: a homogeneous blue lesion in a patient with melanoma history is metastasis until proven otherwise. The absence of lacunae argues against angioma. Irregular vessels at one edge are not consistent with benign blue nevus. Excisional biopsy is mandatory.
Clinical Scenario
A 74-year-old man presents with a raised lesion on his sun-damaged forehead. Nonpolarized dermoscopy reveals comedo-like openings and a cerebriform pattern consistent with seborrheic keratosis. You are about to move on, but then switch to polarized dermoscopy and notice shiny white lines and focal blue-gray ovoid nests in one portion of the lesion not visible under nonpolarized light.
What is your diagnosis?
Collision tumor: seborrheic keratosis with basal cell carcinoma
This case illustrates two critical principles. First, search satisfaction (stopping after recognizing SK features) is the primary cognitive error in collision tumors -- always evaluate the ENTIRE lesion. Second, polarized and nonpolarized dermoscopy provide complementary information: shiny white lines are visible only under polarized light and revealed the hidden BCC component. On sun-damaged skin in older patients, always consider the possibility of a second pathology within a seborrheic keratosis.
Clinical Scenario
A 67-year-old woman presents with a pigmented lesion on her left lower leg. Dermoscopy reveals milia-like cysts and fissures in one half consistent with SK, but the other half shows an atypical pigment network, blue-white veil, and irregular streaks with blue-black coloration. She says the lesion has been present for years but one side has recently darkened.
What is your diagnosis?
Collision tumor: seborrheic keratosis with melanoma
The blue-black sign (simultaneous presence of blue and black areas) is the lifeline in SK-like melanomas. Milia-like cysts and comedo-like openings do NOT exclude melanoma -- they should be ignored during evaluation of melanocytic features. The atypical pigment network, blue-white veil, and irregular streaks in one half of the lesion are classic melanoma-specific structures. The key lesson is that SK features in one portion of a lesion must never prevent thorough evaluation of the remainder. Anchoring bias on the SK component is the most dangerous cognitive error here.
Clinical Scenario
A 52-year-old man with a history of melanoma (excised 4 years ago) presents with a new 6 mm blue-purple papule on his trunk that resembles a hemangioma. Dermoscopy shows red-purple lacunae-like areas, but within the lacunae you notice atypical vessels, shiny white areas, and a focal milky-red zone that lacks the typical homogeneous red of a true lacuna.
What is your diagnosis?
Melanoma metastasis mimicking hemangioma
A homogeneous blue lesion in a patient with melanoma history is metastasis until proven otherwise. Hemangioma-like lesions with atypical vessels within lacunae, or lacunae-like areas with shiny white and milky-red areas, demand biopsy to exclude melanoma. Melanoma metastases can closely resemble vascular lesions. The patient's history of prior melanoma is paramount clinical context -- do not anchor on the hemangioma-like appearance. Always biopsy pyogenic granuloma-like and hemangioma-like lesions when the clinical history includes melanoma.
9. Cross-References
| Topic | Page(s) | Figures / Tables |
|---|---|---|
| Chapter 10: Collision Tumors and Exceptions to Rules (full chapter) | pp. 237--242 | --10.9 |
| Introduction and cognitive errors (anchoring bias, search satisfaction) | pp. 237--238 | |
| False positives overview | p. 238 | |
| Seborrheic keratosis mimicking malignancy | pp. 238--239 | -- |
| Melanoacanthoma | p. 238 | See Chapter 6e |
| Inflamed/irritated SK | p. 238 | See Chapter 6e |
| LPLK | p. 238 | See Chapter 6e |
| SK with pigment network-like structures | pp. 238--239 | See Chapter 8e |
| Clonal SK with globule-like structures | p. 239 | See Chapter 6e |
| Hemangiomas mimicking malignancy | p. 239 | See Chapter 6g |
| Dermatofibroma mimicking melanoma | p. 239 | |
| Atypical and hemosiderotic dermatofibromas | p. 239 | See Chapter 6a |
| Blue nevus and melanocytic nevi as false positives | p. 239 | See Chapters 7a, 7d |
| Collision tumors section | p. 239 | |
| SK-like melanoma (false negative) | pp. 239--240 | |
| Hemangioma-like melanoma | p. 240 | see Chapter 6g |
| Pyogenic granuloma-like melanoma | p. 240 | See Chapter 6g |
| BCC mimicking melanoma and vice versa | pp. 240--241 | See Chapters 6b, 8b, 8f |
| SCC mimicking melanoma | pp. 241--242 | See Chapter 6d |
| Featureless melanoma and digital monitoring | p. 237 | See Chapter 13 |
| Difficult-to-diagnose melanomas (nodular, nevoid, desmoplastic, spitzoid, amelanotic, lentiginous) | p. 237 | See Chapters 8c, 8e, 8f |
| References | p. 242 | References 1--10 |
10. Related Modules
| Module | Relevance |
|---|---|
| Module 08: Dermatofibroma | Key false positive entity -- atypical and hemosiderotic variants mimicking melanoma; dimple sign, peripheral network, and ring-like globules as differentiating features |
| Module 09: Basal Cell Carcinoma | BCC features (globules, leaf-like areas, shiny white structures, arborizing vessels, homogeneous blue) that mimic melanoma and vice versa; BCC + SK collision tumors |
| Module 11: SCC Spectrum | Pigmented and nonpigmented SCC mimicking melanoma through structureless appearance, linearly arranged brown dots/globules, and polymorphous vessels |
| Module 12: Solar Lentigines, Seborrheic Keratoses, and LPLK | SK criteria (comedo openings, milia-like cysts, fissures/ridges); SK variants that mimic melanoma (melanoacanthoma, inflamed SK, clonal SK, ink spot lentigo); LPLK as false positive |
| Module 13: Vascular Lesions | Hemangiomas and angiokeratomas as false positives; hemangioma-like melanoma and pyogenic granuloma-like melanoma as false negatives |
| Module 15: Congenital Melanocytic Nevi | Melanoma arising within congenital nevi; warning signs for malignant transformation |
| Module 16: Acquired Melanocytic Nevi | Atypical mole syndrome and the need for digital monitoring; featureless melanomas arising in nevi |
| Module 18: Blue Nevi and Variants | Homogeneous blue pattern differential -- blue nevus vs. nodular melanoma vs. melanoma metastasis |
| Module 19: Spitz and Reed Nevi | Spitzoid melanoma as a false negative; overlap with atypical spitzoid lesions |
| Module 21: Superficial Spreading Melanoma | Melanoma-specific structures (atypical network, streaks, blue-white veil, regression) that may appear focally in collision tumors |
| Module 22: Nodular Melanoma | Nodular melanoma as false negative (mimics blue nevus, hemangioma); amelanotic nodular melanoma mimicking pyogenic granuloma |
| Module 25: Other Melanoma Subtypes | Nevoid, desmoplastic, and spitzoid melanomas -- specific false negative melanoma subtypes discussed in this chapter |
| Module 26: Amelanotic and Hypomelanotic Melanoma | Amelanotic melanoma as a false negative; polymorphous vessels and milky-red areas as diagnostic clues |
| Module 27: Differentiation -- Pattern Analysis and Melanoma-Specific Criteria | Algorithmic approaches to melanoma diagnosis and their limitations when confronted with collision tumors |
| Module 28: Improving Sensitivity and Specificity | Strategies to minimize false negatives, including comparative approach, ugly duckling sign, and digital monitoring |
| Module 37: Digital Monitoring | Total body photography and digital dermoscopy for detecting featureless melanomas through change over time |
Module 29 is part of Part V: Melanoma in the Dermoscopy Educational Course.
Image Sources & Citations
- HIBA Dermoscopy Dataset: HIBA Dermoscopy Dataset. Hospital Italiano de Buenos Aires. License: CC-BY-4.0.
- DERM12345 (Skin Lesion Dataset with 40 Subclasses): DERM12345: A Large-scale Skin Lesion Image Dataset with 40 Subclasses. Figshare. 2023. License: CC-BY-4.0.
- PROVe-AI Dermoscopy Dataset: PROVe-AI: Prospective Validation of AI in Dermatology dataset. License: CC0-1.0.