Module 01: Introduction and Principles of Dermoscopy
1. Learning Objectives
After completing this module, the learner should be able to:
- Define dermoscopy and explain how it differs from unaided (naked-eye) clinical examination and simple magnification.
- Describe the optical principles underlying nonpolarized dermoscopy (NPD), including the role of the refractive index mismatch at the skin--air interface and the function of the liquid interface.
- Describe the optical principles underlying polarized dermoscopy (PD), including the role of cross-polarization, scattering events, and optical rotation.
- Compare and contrast the structures, colors, and clinical scenarios best visualized with NPD versus PD, and explain the complementary nature of both modalities.
- Explain the concept of birefringence and its relevance to shiny white structures visible under polarized dermoscopy.
- Identify the types of dermoscopic equipment available (nonpolarized, polarized, hybrid dermatoscopes, smartphone attachments, dedicated camera lenses, and total body digital systems) and state their respective advantages.
- Summarize the clinical evidence supporting dermoscopy's role in improving diagnostic accuracy, confidence, and the benign-to-malignant biopsy ratio.
- Outline best practices for immersion fluid selection, minimizing air bubbles, and reducing nosocomial contamination during dermoscopic examination.
2. Prerequisites
None. This is the first module in the course sequence. No prior dermoscopy knowledge is assumed. Learners should have a basic understanding of skin anatomy (epidermis, dermis, stratum corneum, dermal-epidermal junction) and clinical dermatology terminology.
3. Key Concepts
3.1 Dermoscopy -- Definition
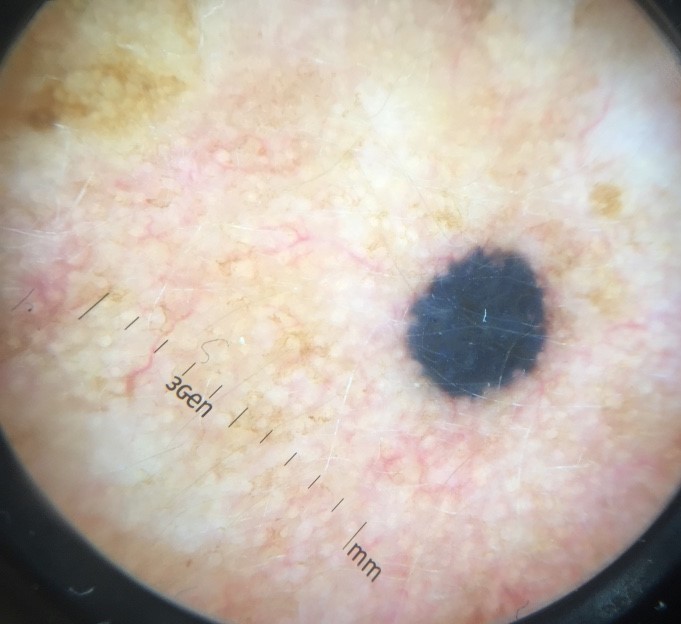
Dermoscopy (also called dermatoscopy or epiluminescence microscopy) is a noninvasive, in vivo diagnostic technique that uses a handheld microscope -- the dermatoscope -- equipped with a magnification lens (typically 10x) and a light source (typically LEDs) to examine subsurface morphologic structures of the skin. It permits visualization from the stratum corneum through to the superficial dermis, revealing colors and structures that are invisible to the naked eye.
3.2 Dermatoscope
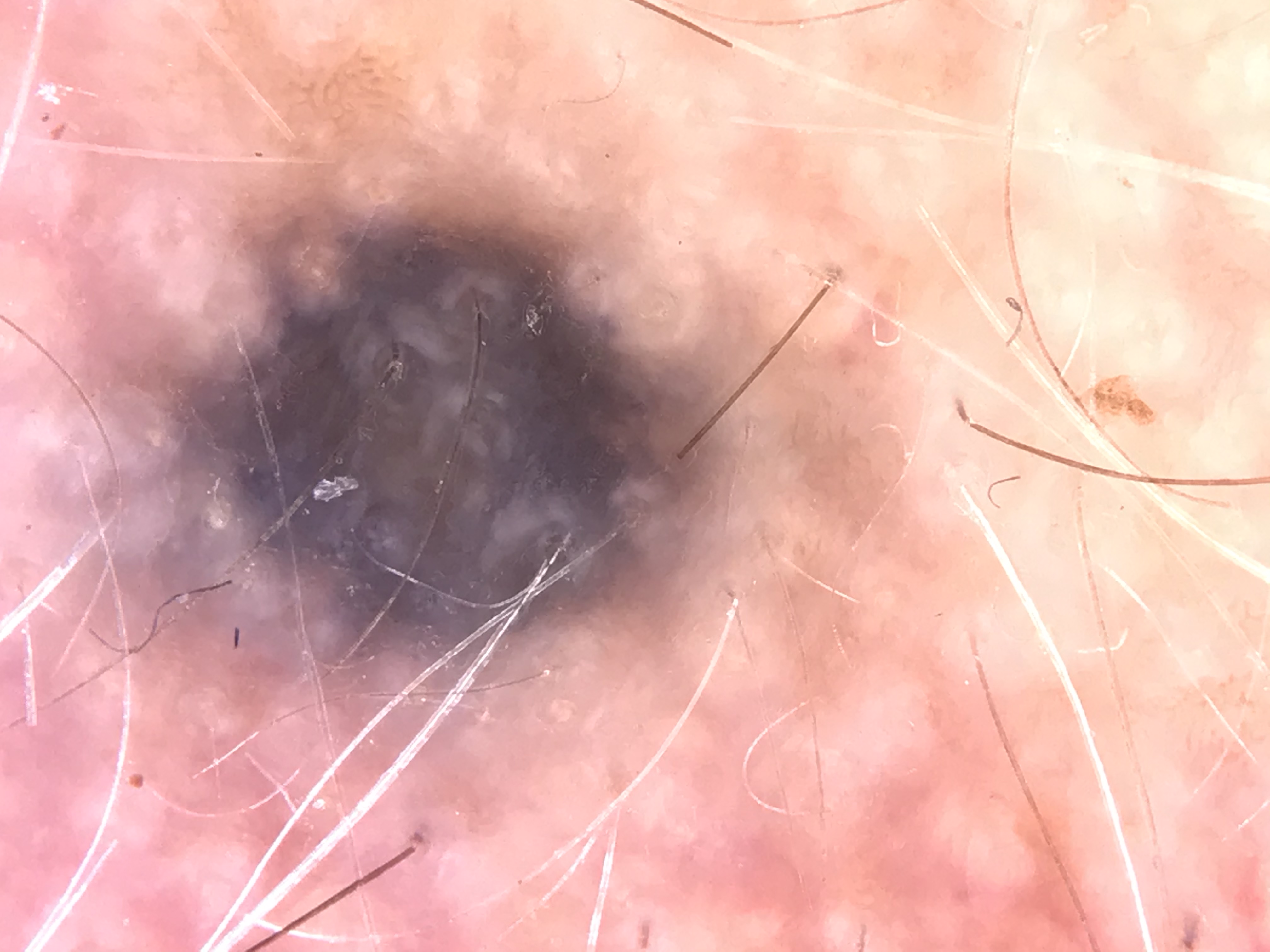
A handheld instrument consisting of:
- A magnification lens (usually 10x)
- A light source (light-emitting diodes, LEDs)
- Optionally, a glass contact plate (for nonpolarized devices)
- Optionally, polarizing filters (for polarized or hybrid devices)
3.3 Stratum Corneum and Light Interaction
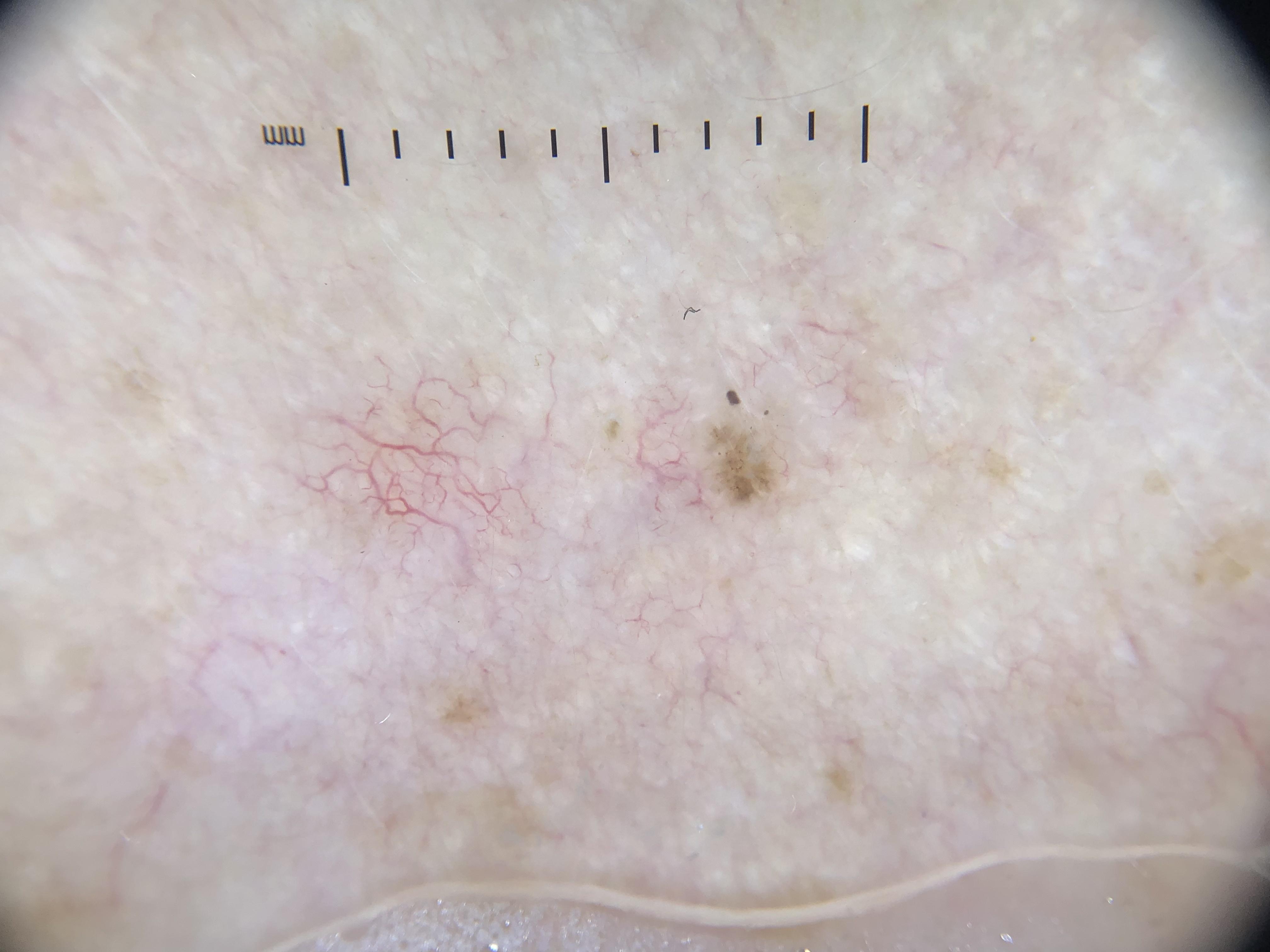
The stratum corneum has a higher refractive index than air. When light strikes the skin, much of it is reflected off the surface (surface glare). This backscattered light overwhelms the retina and prevents visualization of deeper structures. Dermoscopy addresses this problem through either a liquid interface (NPD) or cross-polarization (PD).
3.4 Refractive Index Matching
When a liquid with a refractive index close to that of skin is placed between the dermatoscope glass plate and the skin surface, the normal skin--air interface is replaced by a skin--liquid--glass interface. This reduces surface reflection and glare, making the stratum corneum more translucent and allowing visualization of subsurface structures.
3.5 Cross-Polarization
A system using two polarizing filters oriented perpendicular (orthogonal) to each other. The "source" filter produces unidirectional (polarized) light. Only light that has undergone sufficient scattering events to rotate its polarization by 90 degrees can pass through the "detector" filter. This selectively blocks surface-reflected light and allows deeper structures to be visualized.
3.6 Birefringence
The property of certain biological structures (most notably collagen) to rotate the plane of polarized light in an orientation-dependent manner. Birefringent structures appear as bright white under polarized dermoscopy. This is the optical basis for shiny white structures (shiny white lines, shiny white blotches and strands, and rosettes).
3.7 Key Terminology Reference
| Term | Definition |
|---|---|
| NPD | Nonpolarized dermoscopy -- requires contact with skin and liquid interface |
| PD | Polarized dermoscopy -- uses cross-polarization; does not mandate contact or liquid |
| Hybrid dermatoscope | Device allowing toggle between PD and NPD modes |
| Immersion fluid | Liquid (water, mineral oil, alcohol, gel) placed between scope and skin in NPD |
| Surface glare | Light reflected from stratum corneum that obscures deeper structures |
| DEJ | Dermal-epidermal junction |
| Shiny white structures | Collective term for short shiny white lines, blotches/strands, and rosettes visible only under PD |
| Blink sign | The "lighting up" of milia-like cysts when toggling between NPD and PD on a hybrid dermatoscope |
4. Core Content
4.1 The Rationale for Dermoscopy
4.1.1 Beyond Naked-Eye Examination
Unaided visual inspection of the skin -- with or without a simple magnifying lens -- only permits appreciation of gross morphologic features: size, symmetry, shape, color, contour, and surface topography. These features are limited to what can be observed on the surface layer (stratum corneum). Dermoscopy is unique in allowing clinicians to see subsurface primary morphology of cutaneous lesions, from the stratum corneum down to the level of the superficial dermis. This additional layer of information is what gives dermoscopy its diagnostic power.
4.1.2 Clinical Evidence Supporting Dermoscopy
The evidence base for dermoscopy is substantial:
- Improved diagnostic accuracy: Dermoscopy improves diagnostic accuracy for both pigmented and nonpigmented skin lesions in the hands of experienced users (Bafounta et al., 2001; Kittler et al., 2002; Vestergaard et al., 2008).
- Increased diagnostic confidence: Clinicians using dermoscopy report greater confidence in their clinical diagnoses compared with naked-eye examination alone (Benvenuto-Andrade et al., 2006).
- Improved benign-to-malignant biopsy ratio: The dermatoscope helps clinicians detect early skin cancers while simultaneously minimizing the unnecessary removal of benign lesions (Carli et al., 2003, 2004).
- Cost-effectiveness: The dermatoscope has been shown to be a cost-effective tool in clinical practice (Noor et al., 2009).
- Primary care applicability: Dermoscopy improves the accuracy of primary care physicians in triaging lesions suggestive of skin cancer (Argenziano et al., 2006).
- Guideline endorsement: Various skin cancer screening guidelines now recommend dermoscopy as a standard technique for the early detection of skin cancer, including clinical practice guidelines from Australian Cancer Network and others (Watts et al., 2015; Dinnes et al., 2018).
4.1.3 Who Uses Dermoscopy
While dermoscopy was initially adopted primarily by dermatologists specializing in pigmented lesion evaluation, dermatoscopes are now found in the hands of:
- General dermatologists
- Primary care physicians
- Physician extenders (nurse practitioners, physician assistants)
4.1.4 Applications of Dermoscopy
Dermoscopy has evolved to become indispensable in the evaluation of:
- Pigmented skin lesions
- Nonpigmented skin lesions
- Rashes and inflammatory dermatoses
- Nail disorders
- Hair disorders
4.1.5 Historical Landmark
In the 1970s, Rona MacKie was one of the first clinicians to recognize the advantages of dermoscopy for the preoperative evaluation of equivocal pigmented skin lesions (MacKie, 1971, 1972). Since then, significant progress has been made in defining benign and malignant dermoscopic structures and patterns.
4.2 Mastering Dermoscopy
The literature emphasizes that mastery of dermoscopy requires:
- Formal training -- structured dermoscopy courses taught by experts.
- Bedside mentorship -- learning at the patient's bedside with a dermoscopy mentor.
- Daily practice -- using dermoscopy in the evaluation of as many lesions as possible, on as many patients as possible, on a daily basis.
- Image review -- viewing dermoscopy images freely available at sites such as the International Dermoscopy Society, Dermoscopedia.org, and the International Skin Imaging Collaboration (ISIC).
- Case discussion -- acquiring images of interesting cases and discussing them with colleagues.
Mastery permits the dermoscopist not only to understand the diagnostic significance of what they see through the lens, but also to gain insights into the histopathology and biology of lesions.
Key Takeaways
- Dermoscopy visualizes subsurface structures from the stratum corneum to the superficial dermis that are invisible to the naked eye.
- Dermoscopy improves diagnostic accuracy, increases confidence, and reduces the benign-to-malignant biopsy ratio across multiple evidence-based studies.
- Mastery requires the combination of formal training, bedside mentorship, daily practice, image review, and case discussion.
4.3 Optical Principles of Nonpolarized Dermoscopy (NPD)
4.3.1 The Problem: Surface Glare
The refractive index of the stratum corneum is higher than that of air. When ambient or instrument light strikes the skin surface, the refractive index mismatch causes most incident light to be reflected back from the stratum corneum. This backscattered surface glare overwhelms the retina and prevents visualization of light reflected from the deeper layers of the skin (the epidermis below the stratum corneum and the dermis). As a result, without dermoscopy, clinical examination (even with a simple magnifying lens) only reveals morphologic features manifest on the skin surface.
4.3.2 The Solution: Liquid Interface and Contact
The first handheld dermatoscopes introduced into clinical practice used a nonpolarized light source. Modern NPD devices contain:
- LEDs for illumination
- A 10x magnification lens
- A glass contact plate
NPD requires:
- Direct contact of the dermatoscope's glass plate with the skin.
- A liquid interface (immersion liquid) between the glass plate and the skin, ideally with a refractive index equal to that of skin.
This setup replaces the normal skin--air interface with a skin--liquid--glass interface. Because the refractive indices within this new interface are more closely matched, surface light reflection is decreased. Glare is minimized, making the stratum corneum appear more translucent. The result: the observer can see deeper structures in the skin.
4.3.3 What NPD Visualizes
With NPD, most of the light reaching the observer's eye comes from the more superficial, minimally scattered light -- structures at the level of the epidermis and the dermal-epidermal junction (DEJ). Some light penetrates deeper and is absorbed and reflected back after multiple scattering events, but this deeper light contributes only a small fraction to the NPD image.
Structures best visualized by NPD therefore include:
- Milia-like cysts
- Comedo-like openings
- Blue-white veil (due to orthokeratosis overlying dermal melanin)
- Granularity / peppering
- Surface features in general
4.3.4 Air Bubble Management
When utilizing NPD, it is imperative to eliminate air pockets (air bubbles) between the dermatoscope's glass plate, the liquid, and the skin. Air pockets create a skin--air interface that will preclude visualization of structures below the stratum corneum.
4.3.5 Immersion Fluids
Several immersion liquids can be used for NPD:
| Fluid | Notes |
|---|---|
| Water | Basic option; readily available |
| Mineral oil | Traditional choice; provides good optical coupling |
| 70% alcohol | Reported as the best immersion liquid in one study (Gewirtzman et al., 2003) -- yielded fewer air bubbles and provided clearer images; added benefit of reducing bacterial contamination (more hygienic) |
| Ultrasound gel | Superior for nail apparatus examination (gel viscosity prevents it from rolling off the convex nail surface) |
| Antibacterial gel | Also superior for nail examination; similar viscosity advantage |
Best practices for gel use: Air bubbles are commonly trapped in gel and can be distracting. To minimize bubbles:
- Store gel bottles upside down
- Avoid shaking the bottle
- Squeeze out a small amount of gel before use to discard any remnant dried gel
Hygienic considerations: The dermatoscope can be a potential source of nosocomial infection (Stauffer et al., 2001). Using 70% alcohol as an immersion fluid has the added benefit of reducing bacterial contamination (Kelly & Purcell, 2006).
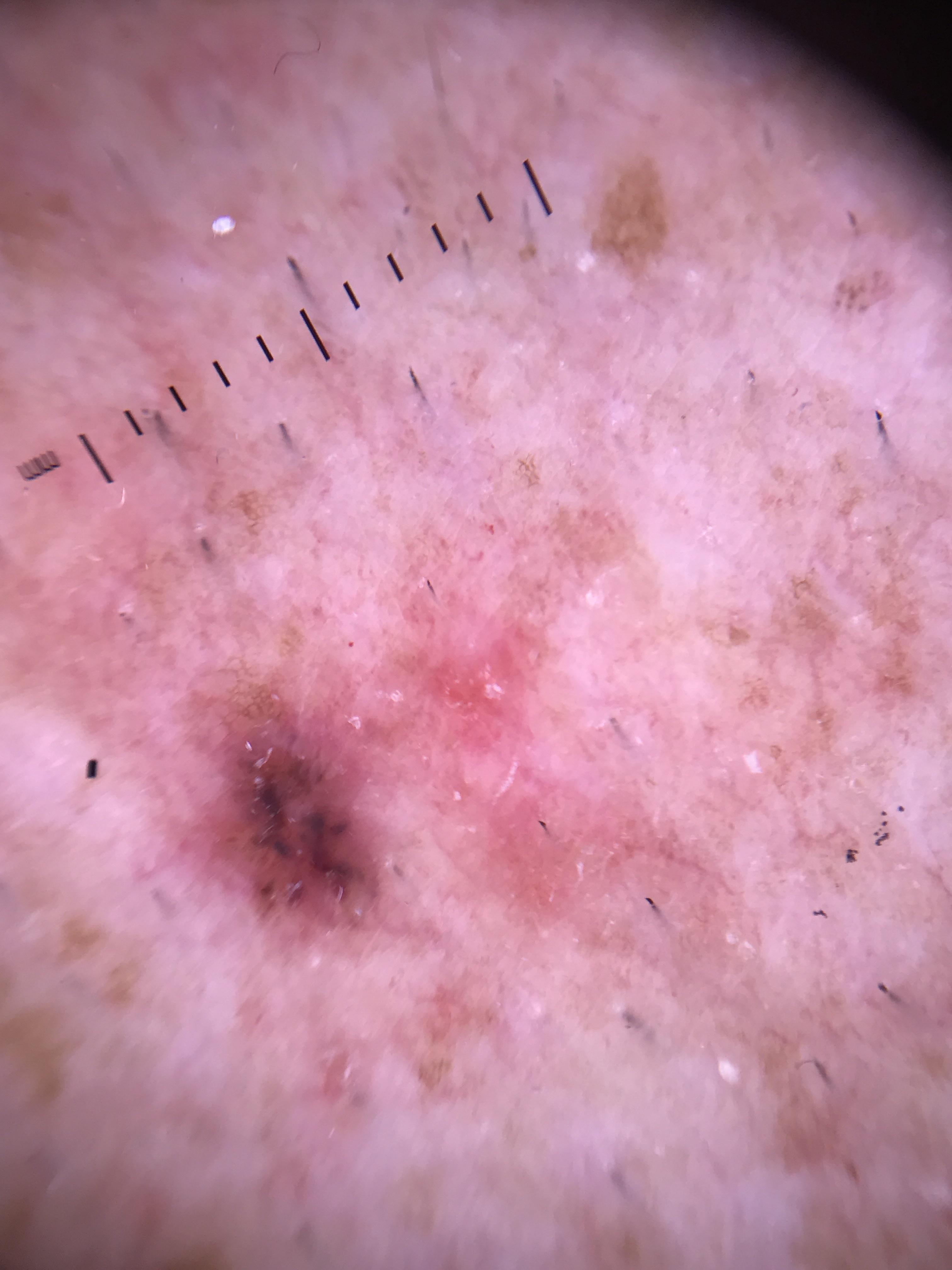
Clinical Scenario
A 55-year-old woman presents with a well-demarcated brown papule on the left forearm. You examine the lesion with a nonpolarized dermatoscope using mineral oil and observe multiple small white-yellow globules (milia-like cysts) and dark plugs (comedo-like openings) scattered across the surface. No vascular structures or shiny white lines are identified.
What is your diagnosis and key dermoscopic findings?
Seborrheic keratosis
The combination of milia-like cysts and comedo-like openings is the hallmark dermoscopic pattern of seborrheic keratosis. These are superficial epidermal structures best visualized under NPD because NPD preferentially images the stratum corneum and upper epidermis. This case illustrates why NPD achieves higher diagnostic accuracy for seborrheic keratosis (75% vs 59% with PD in the Wang et al. study).
Check Your Understanding
What problem does the liquid interface in nonpolarized dermoscopy solve?
The liquid interface replaces the skin-air boundary with a skin-liquid-glass interface, reducing surface glare caused by the refractive index mismatch between the stratum corneum and air. This makes the stratum corneum more translucent, allowing visualization of subsurface structures.
4.4 Optical Principles of Polarized Dermoscopy (PD)
4.4.1 Introduction and History
Polarized dermoscopy devices were introduced into clinical practice around the year 2000. They rely on fundamentally different optical principles than NPD.
4.4.2 The Cross-Polarization System
PD devices use two polarizers to achieve cross-polarization:
"Source" polarized filter: The light emitted from the dermatoscope first passes through this filter, producing polarized, unidirectional light that illuminates the skin.
"Detector" cross-polarized filter: Oriented perpendicular (orthogonal) to the source filter. Reflected light from the skin must pass through this filter to be visualized by the observer's eye.
The key principle: For light to pass through the detector filter (which is orthogonal to the source filter), the light must undergo a 90-degree rotation in its direction of polarization. Such rotation depends on the light wave undergoing sufficient scattering events through collisions with tissue structures.
4.4.3 Why Surface Glare Is Eliminated
- Light reflected from the stratum corneum or superficial epidermis does not undergo sufficient scattering events to cause the 90-degree optical rotation required to pass through the detector filter. Therefore, this light is blocked.
- Light penetrating to deeper levels -- the DEJ and superficial dermis -- undergoes sufficient scattering events to achieve randomization of polarization and can pass through the detector filter.
On average, polarized light must traverse a distance of between 0.06 and 0.1 mm of skin before sufficient polarized light changes its angle of polarization.
4.4.4 What PD Visualizes
Because PD captures backscattered light from deeper skin layers:
- DEJ and dermal structures (e.g., blood vessels) are visualized with enhanced clarity.
- Superficial structures (e.g., comedo-like openings in seborrheic keratosis) are poorly visualized.
4.4.5 Contact and Fluid Not Required
Since surface glare is blocked by cross-polarization, PD:
- Does not mandate the use of a liquid interface
- Does not require direct contact with the skin
These features may enable faster scanning of lesions compared with NPD. However, PD typically requires stronger LED lighting to compensate for photons blocked by cross-polarization.
Safety note: During examination of the face, it is recommended to ask the patient to close their eyes to avoid looking directly into the strong light source.
Expert tip: Despite PD not mandating contact and fluid, the authors' clinical experience indicates that some dermatoscopes provide higher-quality visualization of dermoscopic structures and colors when PD is used with immersion fluid (e.g., 70% alcohol) and direct skin contact.
Clinical Scenario
A 38-year-old man presents with a pink, slightly raised lesion on the upper back that has been slowly growing for 6 months. Examination with a nonpolarized dermatoscope shows a structureless pink area with no discernible pattern. When you switch to polarized dermoscopy, you now observe dotted vessels arranged irregularly, a subtle vascular blush, and short shiny white lines crossing the lesion.
What is your diagnosis and key dermoscopic findings?
Amelanotic melanoma (suspected)
This case demonstrates the critical importance of polarized dermoscopy for nonpigmented lesions. The dotted vessels, vascular blush, and shiny white lines were invisible under NPD due to contact pressure compressing vessels and the inability of NPD to detect birefringent structures. PD revealed these features because it visualizes deeper dermal structures without requiring contact pressure, and shiny white lines are exclusively visible under cross-polarized light. This is why PD achieves higher diagnostic accuracy for melanoma (34% vs 23% for NPD). Biopsy is warranted.
Check Your Understanding
How does cross-polarization in PD eliminate surface glare without requiring a liquid interface?
PD uses two perpendicular polarizing filters. Surface-reflected light maintains its original polarization and is blocked by the orthogonal detector filter. Only light that has undergone sufficient scattering events at deeper levels (0.06-0.1 mm) to rotate its polarization by 90 degrees passes through.
4.5 Hybrid Dermatoscopes
More recently, hybrid dermatoscopes have been developed that allow the user to toggle between PD and NPD. Important usage requirements:
- Hybrid dermatoscopes should be applied using direct skin contact with a liquid interface.
- If no liquid interface is used, the user will see dermoscopic structures only in the polarized mode.
- In the nonpolarized mode without a liquid interface, no dermoscopic structures will be discernible -- the observer will simply see a magnified clinical (not dermoscopic) image of the lesion surface.
4.6 Polarized vs. Nonpolarized Dermoscopy -- Detailed Comparison
4.6.1 Overall Similarity
For most pigmented and nonpigmented skin lesions, PD and NPD offer overall similar images. However, important differences exist that affect diagnostic accuracy and confidence.
4.6.2 Structures Better Seen with NPD
| Structure | Explanation |
|---|---|
| Comedo-like openings | Epidermal location; NPD preferentially images superficial layers |
| Milia-like cysts | Epidermal location; more conspicuous under NPD |
| Blue-white veil (due to orthokeratosis) | Whitish veil is due to orthokeratosis overlying dermal melanin; most conspicuous when viewed with a device that preferentially images superficial layers |
| Gray-blue granularity (peppering) | Due to free melanin in dermis or melanophages in superficial dermis; slightly more conspicuous with NPD (though this varies depending on skin thickness and melanin location -- e.g., peppering in superficial papillary dermis within thin sun-damaged facial skin is more conspicuous with NPD) |
4.6.3 Structures Better Seen with PD
| Structure | Explanation |
|---|---|
| Blood vessels | Dermal structures; PD enhances DEJ and dermal visualization. Also, NPD contact pressure can compress small vessels |
| Vascular blush (pink veil due to vasodilation) | Enhanced visualization of red/pink colors with PD; no compression effect |
| Shiny white structures (collectively) | Visible only under PD -- completely disappear under NPD; due to birefringence of collagen and other structures |
| Melanin pigment (color depth) | PD displays melanin with varying and darker shades of brown and blue compared with NPD |
4.6.4 Color Differences
The PD system displays melanin pigment with varying and darker shades of brown and blue compared with NPD. Red and pink colors are also more prominent under PD (+++ vs +).
Summary table (adapted):
| Color or Structure | NPD | PD |
|---|---|---|
| Melanin | + | ++ |
| Red/pink | + | +++ |
| Blue-white veil (orthokeratosis over melanin) | +++ | + |
| Gray-blue hue (dermal regression) | +++ | ++ |
| Granularity | +++ | ++ |
| White shiny lines and strands | - (not visible) | +++ |
| Blood vessels | + | +++ |
| Milia-like cysts | +++ | +/- |
Key Takeaways
- NPD best visualizes superficial structures (milia-like cysts, comedo-like openings, blue-white veil) via refractive index matching with a liquid interface.
- PD best visualizes dermal structures (blood vessels, vascular blush) and is the only modality that reveals shiny white structures via birefringence.
- PD maximizes sensitivity for melanoma detection while NPD maximizes specificity for benign lesion identification.
- Using both modalities together on a hybrid dermatoscope provides the highest overall diagnostic accuracy.
4.6.5 The Role of Pressure
Some differences between PD and NPD images are not purely optical but also reflect the mechanical effects of contact pressure:
- NPD requires a liquid interface and contact, so the dermatoscope is pressed against the skin. This pressure can compress small blood vessels, making them difficult to visualize. As little as 18 mmHg of pressure is sufficient to blanch the blood volume within a lesion.
- PD does not require direct contact, so blood vessels and pink color are more evident.
- When gel (rather than alcohol) is used as the fluid interface during NPD, the operator can apply less pressure, which greatly enhances the ability to visualize blood vessels.
4.6.6 Shiny White Structures in Detail
Under PD, a category of structures known collectively as shiny white structures may be observed. These include:
- Short shiny white lines (previously called crystalline structures) -- correspond to altered stromal collagen. Due to the birefringence of collagen, their visibility depends on the orientation of collagen fibers relative to the polarizing filter. This explains why:
- Shiny white lines under PD display only two orthogonal orientations.
- Rotating the dermatoscope on its axis while viewing causes some shiny white lines to disappear while a new set appears, with all lines maintaining their orthogonal orientation (angular dependence).
Shiny white blotches and strands -- seen in basal cell carcinomas (BCC), likely due to a combination of mucin and the BCC matrix (not collagen).
Rosettes -- a shiny white structure composed of four perpendicular white dots, corresponding histopathologically to either keratin-filled adnexal openings or concentric perifollicular fibrosis (Haspeslagh et al., 2016).
All shiny white structures completely disappear when viewed with NPD. This is not due to selective visualization of anatomic depth but due to the unique optical properties of polarized light -- specifically birefringence.
4.6.7 Diagnostic Impact: Study Data
The Wang et al. (2008) study demonstrated statistically significant differences between NPD and PD:
- Seborrheic keratosis diagnostic accuracy: NPD 75% vs PD 59% (P < 0.0001). NPD was superior because milia-like cysts and comedo-like openings are visible under NPD, making the correct diagnosis easier.
- Melanoma diagnostic accuracy: PD 34% vs NPD 23% (P = 0.0008). PD was superior because amelanotic or structureless melanomas may only be identifiable by dotted or polymorphous blood vessels, vascular blush, and/or white shiny lines -- features readily appreciated with PD but difficult or impossible to visualize with NPD.
4.6.8 Complementary Nature and the Blink Sign
PD and NPD provide complementary and additive information:
- PD provides maximum sensitivity for detecting cutaneous malignancy.
- NPD provides maximum specificity by correctly identifying lesions such as seborrheic keratosis.
- Using both modalities may provide the clinician with the highest diagnostic accuracy.
Hybrid dermatoscopes make this practical by allowing toggling between PD and NPD:
- Structures at all depths can be visualized: NPD for stratum corneum to DEJ; PD for DEJ, superficial dermis, and birefringent structures.
- The "blink sign" (Braun et al., 2011): Toggling back and forth on hybrid dermoscopes "lights up" the milia-like cysts in seborrheic keratosis, creating a highly informative visual cue.
- For melanoma or dermatofibroma, toggling highlights shiny white lines, which can be diagnostically informative.
Clinical Scenario
A 72-year-old woman presents for a full-body skin examination. You are using a hybrid dermatoscope with ultrasound gel on a nail lesion. When you toggle between NPD and PD modes on a brown plaque on the adjacent dorsal hand, you notice small white-yellow globules that seem to "light up" and become more conspicuous in NPD mode, then fade when switching to PD mode.
What is your diagnosis and key dermoscopic findings?
Seborrheic keratosis (blink sign)
The "blink sign" describes the phenomenon where milia-like cysts in seborrheic keratosis appear to light up when toggling between PD and NPD on a hybrid dermatoscope. Milia-like cysts are superficial epidermal keratin-filled structures that are much more conspicuous under NPD than PD. The alternating visibility creates a characteristic blinking effect that is highly informative for diagnosing seborrheic keratosis. This case also illustrates the value of hybrid dermatoscopes in clinical practice.
Check Your Understanding
Name two structures better seen with NPD and two better seen with PD.
NPD excels at visualizing milia-like cysts and comedo-like openings (superficial epidermal structures). PD excels at visualizing blood vessels and shiny white structures (dermal and birefringent structures).
4.7 Capturing Dermoscopic Images
4.7.1 Methods of Image Capture
| Method | Description |
|---|---|
| Handheld dermatoscope + camera adapter | Adapters couple the dermatoscope to a digital camera |
| Dedicated dermoscopic camera lenses | Less cumbersome than handheld units with adapters; generally produce sharper, clearer images |
| Smartphone dermoscopic lenses | Dermoscopic lenses that attach directly to smartphones; image quality is on a par with more traditional methods |
| Integrated computer systems | Dermoscopic imaging device linked directly to a computer; simplifies image acquisition, storage, organization, retrieval, and viewing |
| Total body digital systems | Afford acquisition of dermoscopic images, serial dermoscopy, and linking of dermoscopic images to clinical lesion images |
4.7.2 Image Storage and Management
- Most images captured today are digitally acquired.
- Images can be stored in the cloud or on hard drives.
- Easy retrieval of relevant images may pose a challenge; multiple image database programs are available to facilitate organization and retrieval.
- Many integrated systems include computer-based analytical algorithms to assist clinicians in managing skin lesions.
Key Takeaways
- Shiny white structures (lines, blotches, strands, rosettes) are exclusively visible under PD and completely disappear under NPD due to birefringence.
- As little as 18 mmHg of contact pressure can blanch blood vessels; use gel or noncontact PD when vascular assessment is critical.
- The blink sign (toggling PD/NPD on a hybrid dermatoscope) lights up milia-like cysts in seborrheic keratosis and is a highly informative diagnostic cue.
5. Dermoscopic Equipment Summary
5.1 Equipment Types
| Equipment Type | Light Source | Contact Required | Liquid Interface | Key Advantage |
|---|---|---|---|---|
| Nonpolarized dermatoscope (NPD) | LEDs (nonpolarized) | Yes | Yes (mandatory) | Best for superficial epidermal structures (milia-like cysts, comedo-like openings); maximum specificity |
| Polarized dermatoscope (PD) | LEDs (cross-polarized) | No (optional) | No (optional) | Best for dermal structures, blood vessels, shiny white structures; maximum sensitivity for malignancy; faster scanning |
| Hybrid dermatoscope | LEDs (toggleable PD/NPD) | Yes (recommended) | Yes (recommended) | Combines both modalities; enables blink sign; highest overall diagnostic accuracy |
| Smartphone dermoscopic lens | Phone LED + lens attachment | Varies | Varies | Portable; quality comparable to traditional methods; affordable |
| Dedicated dermoscopic camera | Built-in | Varies | Varies | Sharper/clearer images than handheld + adapter combinations |
| Integrated computer system | Built-in | Varies | Varies | Streamlined workflow: image acquisition, storage, organization, retrieval, computer-assisted analysis |
| Total body digital system | Built-in | Varies | Varies | Serial dermoscopy; links dermoscopic to clinical images; total body photography integration |
5.2 Magnification
Standard dermatoscopes provide 10x magnification. This is sufficient to visualize subsurface structures from the stratum corneum through the superficial dermis.
5.3 Immersion Fluid Selection Guide
| Clinical Scenario | Recommended Fluid | Rationale |
|---|---|---|
| General skin examination | 70% alcohol | Fewest air bubbles, clearest images, hygienic (reduces bacterial contamination) |
| Nail apparatus examination | Ultrasound gel or antibacterial gel | Viscosity prevents fluid from rolling off convex nail surface |
| Minimizing blood vessel compression | Ultrasound gel | Allows lower pressure application during NPD |
| Rapid scanning of multiple lesions | None (PD mode) | PD does not require liquid; allows fastest workflow |
6. Clinical Pearls
Start with both modes: When using a hybrid dermatoscope, examine each lesion with both NPD and PD. NPD maximizes specificity (correctly identifying benign lesions), while PD maximizes sensitivity (detecting malignancy). Together, they provide the highest diagnostic accuracy.
The 18 mmHg threshold: As little as 18 mmHg of pressure can blanch blood vessels within a lesion. When vascular structures are important for diagnosis (e.g., suspected BCC, amelanotic melanoma), minimize contact pressure. Gel interfaces allow lower pressure than alcohol during NPD.
The blink sign for seborrheic keratosis: Toggling between PD and NPD on a hybrid dermatoscope causes milia-like cysts in seborrheic keratoses to "light up," creating a highly useful diagnostic sign.
Alcohol is the best general-purpose immersion fluid: A 70% alcohol solution provides the fewest air bubbles, the clearest images, and the added benefit of reducing nosocomial contamination.
Gel for nails, not alcohol: For nail examination, ultrasound or antibacterial gel is superior because its viscosity keeps it in place on the convex nail surface. Store gel bottles upside down, avoid shaking, and squeeze out a small amount before use to discard dried gel.
Close the patient's eyes on facial exam with PD: PD typically requires stronger LEDs to compensate for cross-polarization photon loss. Ask patients to close their eyes during facial examination to avoid discomfort from the bright light.
Shiny white structures are PD-exclusive: Short shiny white lines, shiny white blotches/strands, and rosettes are completely invisible under NPD. If you are examining a lesion only with NPD, you will miss these diagnostically important structures entirely.
Angular dependence of shiny white lines: When viewing shiny white lines under PD, try rotating the dermatoscope on its axis. Due to the birefringent properties of collagen, some lines will disappear and new lines will appear, always maintaining orthogonal orientations. This phenomenon confirms the collagenous nature of the structure.
PD with contact and fluid can be superior: Although PD does not require contact or liquid, many experienced dermoscopists find that using PD with immersion fluid and direct contact provides higher-quality visualization of structures and colors.
Amelanotic melanoma detection: Some amelanotic or structureless melanomas are identifiable only by dotted or polymorphous blood vessels, vascular blush, and/or white shiny lines. These structures are readily appreciated with PD and may be impossible to visualize with NPD. Always include PD in the evaluation of clinically suspicious pink or flesh-colored lesions.
Daily practice is essential: The literature strongly recommends using dermoscopy on as many lesions as possible, on as many patients as possible, every day. Supplementing clinical practice with image review from resources such as the International Dermoscopy Society, Dermoscopedia.org, and the ISIC database accelerates learning and knowledge retention.
8. Cross-References
| Topic | Chapter | Pages |
|---|---|---|
| Introduction and rationale for dermoscopy | Chapter 1 | pp. 12--13 |
| Principles of nonpolarized dermoscopy | Chapter 2 | pp. 14--15 |
| Principles of polarized dermoscopy | Chapter 2 | pp. 15--16 |
| Polarized vs. nonpolarized dermoscopy comparison | Chapter 2 | pp. 16--17 |
| Shiny white structures (birefringence) | Chapter 2 | pp. 16--17 |
| Wang et al. study (PD vs NPD diagnostic accuracy) | Chapter 2 | p. 17 |
| Capturing dermoscopic images and equipment | Chapter 2 | pp. 18--19 |
| Histopathologic correlations of dermoscopic structures | Chapter 3 | pp. 20--52 |
| Pattern analysis | Chapter 4a | pp. 53--60 |
Key Illustrations:
- Schematic of light interaction with skin without dermoscopy (surface glare)
- Physician using contact NPD
- Schematic of light interaction during contact NPD with liquid interface
- Schematic of light interaction during polarized dermoscopy (cross-polarization)
- Physician using noncontact PD
- Melanoma (0.9 mm thickness) -- NPD vs PD comparison showing blue-white veil (NPD) and shiny white lines (PD)
- Seborrheic keratosis -- NPD vs PD (milia-like cysts visible only with NPD)
- Basal cell carcinoma -- arborizing vessels better seen with PD
- Melanoma (0.3 mm thickness) -- vascular blush better seen with PD
- Melanoma (1.65 mm thickness) -- three images comparing NPD with alcohol, NPD with gel, and noncontact PD
- Combined blue nevus -- NPD vs PD color differences
- Superficial BCC -- NPD vs PD (contact and noncontact)
- Dermatofibroma -- shiny white lines visible only with PD
- Dermatofibroma -- PD contact vs noncontact (vascular compression effects)
- Blue nevus -- NPD vs PD (homogeneous blue steel pattern)
9. Related Modules
Module 02: Histopathologic Correlations of Dermoscopic Structures (
module_02_histopathologic_correlations.md) -- Builds directly on the principles introduced in this module by explaining the histopathologic basis (what you see under the microscope) for the colors and structures observed through the dermatoscope. Understanding why structures appear as they do in dermoscopy requires knowledge of where melanin, collagen, blood vessels, and other chromophores are located in the skin.Module 03: Pattern Analysis Revised (
module_03_pattern_analysis.md) -- Introduces the systematic approach to interpreting dermoscopic images using defined structural elements (lines, dots, clods, circles, pseudopods, structureless areas), patterns, and colors. This module applies the foundational optical principles learned here to develop a structured diagnostic framework, including the Chaos and Clues short algorithm.
This module is part of the Dermoscopy Educational Course. For the complete course outline and suggested study paths, see COURSE_OUTLINE.md.
Image Sources & Citations
- DERM12345 (Skin Lesion Dataset with 40 Subclasses): DERM12345: A Large-scale Skin Lesion Image Dataset with 40 Subclasses. Figshare. 2023. License: CC-BY-4.0.
- HIBA Dermoscopy Dataset: HIBA Dermoscopy Dataset. Hospital Italiano de Buenos Aires. License: CC-BY-4.0.